Abstract
B cells can promote liver fibrosis, but the mechanism of B cell infiltration and therapy against culprit B cells are lacking. We postulated that the disruption of cholangiocyte-B-cell crosstalk could attenuate liver fibrosis by blocking the CXCL12-CXCR4 axis via a cyclooxygenase-2-independent effect of celecoxib. In wild-type mice subjected to thioacetamide, celecoxib ameliorated lymphocytic infiltration and liver fibrosis. By single-cell RNA sequencing and flow cytometry, CXCR4 was established as a marker for profibrotic and liver-homing phenotype of B cells. Celecoxib reduced liver-homing B cells without suppressing CXCR4. Cholangiocytes expressed CXCL12, attracting B cells to fibrotic areas in human and mouse. The proliferation and CXCL12 expression of cholangiocytes were suppressed by celecoxib. In CXCL12-deficient mice, liver fibrosis was also attenuated with less B-cell infiltration. In the intrahepatic biliary epithelial cell line HIBEpiC, bulk RNA sequencing indicated that both celecoxib and 2,5-dimethyl-celecoxib (an analog of celecoxib that does not show a COX-2-dependent effect) regulated the TGF-β signaling pathway and cell cycle. Moreover, celecoxib and 2,5-dimethyl-celecoxib decreased the proliferation, and expression of collagen I and CXCL12 in HIBEpiC cells stimulated by TGF-β or EGF. Taken together, liver fibrosis can be ameliorated by disrupting cholangiocyte-B cell crosstalk by blocking the CXCL12-CXCR4 axis with a COX-2-independent effect of celecoxib.
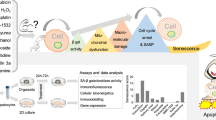
Graphical abstract








Similar content being viewed by others
Data availability
The raw data of single-cell RNA sequencing and RNA sequencing have been deposited in the NCBI Gene Expression Omnibus (GSE221481, GSE220643). All the data are available from the corresponding author Jinhang Gao (Gao.jinhang@scu.edu.cn) upon reasonable request.
Abbreviations
- BM:
-
Bone marrow
- CCL2:
-
C–C motif chemokine ligand 2
- CCK8:
-
Cell Counting Kit 8
- CXCL12:
-
C-X-C Motif Chemokine Ligand 12
- CXCR4:
-
C-X-C Motif Chemokine Receptor 4
- COX-2:
-
Cyclooxygenase-2
- DAPI:
-
4′,6-Diamidino-2-phenylindole
- DEGs:
-
Differentially expressed genes
- DMEM:
-
Dulbecco’s modified eagle medium
- DMSO:
-
Dimethyl sulfoxide
- EGF:
-
Epidermal growth factor
- ELISA:
-
Enzyme-linked immunosorbent assay
- FACS:
-
Fluorescence-activated cell sorting
- FISH:
-
Fluorescence in situ hybridization
- GO:
-
Gene ontology
- H&E:
-
Hematoxylin and eosin
- IF:
-
Immunofluorescence
- KEGG:
-
Kyoto encyclopedia of genes and genomes
- PB:
-
Portal venous blood
- RNA-seq:
-
RNA-sequencing
- scRNA-seq:
-
Single-cell RNA-sequencing
- SSC:
-
Saline sodium citrate
- TAA:
-
Thioacetamide
- TGF-β:
-
Transforming growth factor-β
- WB:
-
Western blot
References
Gines P, Krag A, Abraldes JG, Sola E, Fabrellas N, Kamath PS (2021) Liver cirrhosis. Lancet 398:1359–1376. https://doi.org/10.1016/S0140-6736(21)01374-X
Moon AM, Singal AG, Tapper EB (2020) Contemporary Epidemiology of Chronic Liver Disease and Cirrhosis. Clin Gastroenterol Hepatol 18:2650–2666. https://doi.org/10.1016/j.cgh.2019.07.060
Kisseleva TD (2021) Brenner Molecular and cellular mechanisms of liver fibrosis and its regression. Nat Rev Gastroenterol Hepatol 18:151–166. https://doi.org/10.1038/s41575-020-00372-7
Trivedi P, Wang S, Friedman SL (2021) The power of plasticity-metabolic regulation of hepatic stellate cells. Cell Metab 33:242–257. https://doi.org/10.1016/j.cmet.2020.10.026
Parola MM, Pinzani. (2019) Liver fibrosis: Pathophysiology, pathogenetic targets and clinical issues. Mol Aspects Med 65:37–55. https://doi.org/10.1016/j.mam.2018.09.002
Sutti SE, Albano. (2020) Adaptive immunity: an emerging player in the progression of NAFLD. Nat Rev Gastroenterol Hepatol 17:81–92. https://doi.org/10.1038/s41575-019-0210-2
Faggioli F, Palagano E, Di Tommaso L, Donadon M, Marrella V, Recordati C, Mantero S, Villa A, Vezzoni P, Cassani B (2018) B lymphocytes limit senescence-driven fibrosis resolution and favor hepatocarcinogenesis in mouse liver injury. Hepatology 67:1970–1985. https://doi.org/10.1002/hep.29636
Barrow F, Khan S, Fredrickson G, Wang H, Dietsche K, Parthiban P, Robert S, Kaiser T, Winer S, Herman A, Adeyi O, Mouzaki M, Khoruts A, Hogquist KA, Staley C, Winer DA, Revelo XS (2021) Microbiota-driven activation of intrahepatic B cells aggravates NASH through innate and adaptive signaling. Hepatology 74:704–722. https://doi.org/10.1002/hep.31755
Zhang F, Jiang WW, Li X, Qiu XY, Wu Z, Chi YJ, Cong X, Liu YL (2016) Role of intrahepatic B cells in non-alcoholic fatty liver disease by secreting pro-inflammatory cytokines and regulating intrahepatic T cells. J Dig Dis 17:464–474. https://doi.org/10.1111/1751-2980.12362
Thapa M, Chinnadurai R, Velazquez VM, Tedesco D, Elrod E, Han JH, Sharma P, Ibegbu C, Gewirtz A, Anania F, Pulendran B, Suthar MS, Grakoui A (2015) Liver fibrosis occurs through dysregulation of MyD88-dependent innate B-cell activity. Hepatology 61:2067–2079. https://doi.org/10.1002/hep.27761
Novobrantseva TI, Majeau GR, Amatucci A, Kogan S, Brenner I, Casola S, Shlomchik MJ, Koteliansky V, Hochman PS, Ibraghimov A (2005) Attenuated liver fibrosis in the absence of B cells. J Clin Invest 115:3072–3082. https://doi.org/10.1172/JCI24798
Patel AM, Liu YS, Davies SP, Brown RM, Kelly DA, Scheel-Toellner D, Reynolds GM, Stamataki Z (2021) The Role of B Cells in Adult and Paediatric Liver Injury. Front Immunol 12:729143. https://doi.org/10.3389/fimmu.2021.729143
Britton C, Poznansky MC, Reeves P (2021) Polyfunctionality of the CXCR4/CXCL12 axis in health and disease: implications for therapeutic interventions in cancer and immune-mediated diseases. FASEB J 35:e21260. https://doi.org/10.1096/fj.202001273R
Chen Z, Liu S, He C, Sun J, Wang L, Chen H, Zhang F (2021) CXCL12-CXCR4-mediated chemotaxis supports accumulation of mucosal-associated invariant T cells into the liver of patients with PBC. Front Immunol 12:578548. https://doi.org/10.3389/fimmu.2021.578548
Chalin A, Lefevre B, Devisme C, Barget N, Amiot L, Samson M (2019) Circulating levels of CXCL11 and CXCL12 are biomarkers of cirrhosis in patients with chronic hepatitis C infection. Cytokine 117:72–78. https://doi.org/10.1016/j.cyto.2019.02.006
Chow LN, Schreiner P, Ng BY, Lo B, Hughes MR, Scott RW, Gusti V, Lecour S, Simonson E, Manisali I, Barta I, McNagny KM, Crawford J, Webb M, Underhill TM (2016) Impact of a CXCL12/CXCR4 antagonist in bleomycin (BLM) induced pulmonary fibrosis and carbon tetrachloride (CCl4) induced hepatic fibrosis in mice. PLoS ONE 11:e0151765. https://doi.org/10.1371/journal.pone.0151765
Saiman Y, Jiao J, Fiel MI, Friedman SL, Aloman C, Bansal MB (2015) Inhibition of the CXCL12/CXCR4 chemokine axis with AMD3100, a CXCR4 small molecule inhibitor, worsens murine hepatic injury. Hepatol Res 45:794–803. https://doi.org/10.1111/hepr.12411
Tsuchiya A, Imai M, Kamimura H, Takamura M, Yamagiwa S, Sugiyama T, Nomoto M, Heike T, Nagasawa T, Nakahata T, Aoyagi Y (2012) Increased susceptibility to severe chronic liver damage in CXCR4 conditional knock-out mice. Dig Dis Sci 57:2892–2900. https://doi.org/10.1007/s10620-012-2239-8
Terada R, Yamamoto K, Hakoda T, Shimada N, Okano N, Baba N, Ninomiya Y, Gershwin ME, Shiratori Y (2003) Stromal cell-derived factor-1 from biliary epithelial cells recruits CXCR4-positive cells: implications for inflammatory liver diseases. Lab Invest 83:665–672. https://doi.org/10.1097/01.lab.0000067498.89585.06
Wald O, Pappo O, Safadi R, Dagan-Berger M, Beider K, Wald H, Franitza S, Weiss I, Avniel S, Boaz P, Hanna J, Zamir G, Eid A, Mandelboim O, Spengler U, Galun E, Peled A (2004) Involvement of the CXCL12/CXCR4 pathway in the advanced liver disease that is associated with hepatitis C virus or hepatitis B virus. Eur J Immunol 34:1164–1174. https://doi.org/10.1002/eji.200324441
Lei Y, Liu Z, Han Q, Kang W, Zhang L, Lou S (2010) G-CSF enhanced SDF-1 gradient between bone marrow and liver associated with mobilization of peripheral blood CD34+ cells in rats with acute liver failure. Dig Dis Sci 55:285–291. https://doi.org/10.1007/s10620-009-0757-9
Liu Y, Yang X, Jing Y, Zhang S, Zong C, Jiang J, Sun K, Li R, Gao L, Zhao X, Wu D, Shi Y, Han Z, Wei L (2015) Contribution and mobilization of mesenchymal stem cells in a mouse model of carbon tetrachloride-induced liver fibrosis. Sci Rep 5:17762. https://doi.org/10.1038/srep17762
Zhang L, Tai Y, Zhao C, Ma X, Tang S, Tong H, Tang C, Gao J (2021) Inhibition of cyclooxygenase-2 enhanced intestinal epithelial homeostasis via suppressing beta-catenin signalling pathway in experimental liver fibrosis. J Cell Mol Med 25:7993–8005. https://doi.org/10.1111/jcmm.16730
Tang S, Huang Z, Jiang J, Gao J, Zhao C, Tai Y, Ma X, Zhang L, Ye Y, Gan C, Su W, Jia X, Liu R, Wu H, Tang C (2021) Celecoxib ameliorates liver cirrhosis via reducing inflammation and oxidative stress along spleen-liver axis in rats. Life Sci 272:119203. https://doi.org/10.1016/j.lfs.2021.119203
Tai Y, Zhao C, Zhang L, Tang S, Jia X, Tong H, Liu R, Tang C, Gao J (2021) Celecoxib reduces hepatic vascular resistance in portal hypertension by amelioration of endothelial oxidative stress. J Cell Mol Med 25:10389–10402. https://doi.org/10.1111/jcmm.16968
Gao JH, Wen SL, Tong H, Wang CH, Yang WJ, Tang SH, Yan ZP, Tai Y, Ye C, Liu R, Huang ZY, Tang YM, Yang JH, Tang CW (2016) Inhibition of cyclooxygenase-2 alleviates liver cirrhosis via improvement of the dysfunctional gut-liver axis in rats. Am J Physiol Gastrointest Liver Physiol 310:G962–G972. https://doi.org/10.1152/ajpgi.00428.2015
Gao JH, Wen SL, Feng S, Yang WJ, Lu YY, Tong H, Liu R, Tang SH, Huang ZY, Tang YM, Yang JH, Xie HQ, Tang CW (2016) Celecoxib and octreotide synergistically ameliorate portal hypertension via inhibition of angiogenesis in cirrhotic rats. Angiogenesis 19:501–511. https://doi.org/10.1007/s10456-016-9522-9
Al-Rashed F, Calay D, Lang M, Thornton CC, Bauer A, Kiprianos A, Haskard DO, Seneviratne A, Boyle JJ, Schonthal AH, Wheeler-Jones CP, Mason JC (2018) Celecoxib exerts protective effects in the vascular endothelium via COX-2-independent activation of AMPK-CREB-Nrf2 signalling. Sci Rep 8:6271. https://doi.org/10.1038/s41598-018-24548-z
Xu XT, Hu WT, Zhou JY, Tu Y (2017) Celecoxib enhances the radiosensitivity of HCT116 cells in a COX-2 independent manner by up-regulating BCCIP. Am J Transl Res 9:1088–1100
Tamura D, Saito T, Murata K, Kawashima M, Asano R (2015) Celecoxib exerts antitumor effects in canine mammary tumor cells via COX2independent mechanisms. Int J Oncol 46:1393–1404. https://doi.org/10.3892/ijo.2015.2820
Gallouet AS, Travert M, Bresson-Bepoldin L, Guilloton F, Pangault C, Caulet-Maugendre S, Lamy T, Tarte K, Guillaudeux T (2014) COX-2-independent effects of celecoxib sensitize lymphoma B cells to TRAIL-mediated apoptosis. Clin Cancer Res 20:2663–2673. https://doi.org/10.1158/1078-0432.CCR-13-2305
Lan T, Tai Y, Zhao C, Xiao Y, Yang Z, Zhang L, Gan C, Dai W, Tong H, Tang C, Huang Z, Gao J (2023) Atypical cholangiocytes derived from hepatocyte-cholangiocyte transdifferentiation mediated by COX-2: a kind of misguided liver regeneration. Inflamm Regen 43:37. https://doi.org/10.1186/s41232-023-00284-4
Mederacke I, Dapito DH, Affo S, Uchinami H, Schwabe RF (2015) High-yield and high-purity isolation of hepatic stellate cells from normal and fibrotic mouse livers. Nat Protoc 10:305–315. https://doi.org/10.1038/nprot.2015.017
Sobolewski CN, Legrand. (2021) Celecoxib Analogues for Cancer Treatment: An Update on OSU-03012 and 2,5-Dimethyl-Celecoxib. Biomolecules. https://doi.org/10.3390/biom11071049
Fuster D, Garcia-Calvo X, Farre O, Zuluaga P, Bolao F, Leis A, Hernandez-Rubio A, Rivas I, Muga R (2021) Markers of monocyte activation, inflammation, and microbial translocation are associated with liver fibrosis in alcohol use disorder. J Clin Med 10:3496. https://doi.org/10.3390/jcm10163496
Chen X, Liu X, Duan S, Tang R, Zhou S, Ye R, Yang Y, Wang J, Yao S, He N (2020) Plasma Inflammatory Biomarkers Associated with Advanced Liver Fibrosis in HIV-HCV-Coinfected Individuals. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph17249474
Tobon GJ, Izquierdo JH, Canas CA (2013) B lymphocytes: development, tolerance, and their role in autoimmunity-focus on systemic lupus erythematosus. Autoimmune Dis 2013:827254. https://doi.org/10.1155/2013/827254
Hendrickx AX, Bossuyt. (2001) Quantification of the leukocyte common antigen (CD45) in mature B-cell malignancies. Cytometry 46:336–339. https://doi.org/10.1002/cyto.10032
Kajikhina K, Tsuneto M, Melchers F (2016) B-lymphopoiesis in fetal liver, guided by chemokines. Adv Immunol 132:71–89. https://doi.org/10.1016/bs.ai.2016.07.002
Liepelt AF, Tacke. (2016) Stromal cell-derived factor-1 (SDF-1) as a target in liver diseases. Am J Physiol Gastrointest Liver Physiol 311:G203–G209. https://doi.org/10.1152/ajpgi.00193.2016
Pino MS, Milella M, Gelibter A, Sperduti I, De Marco S, Nuzzo C, Bria E, Carpanese L, Ruggeri EM, Carlini P, Cognetti F (2009) Capecitabine and celecoxib as second-line treatment of advanced pancreatic and biliary tract cancers. Oncology 76:254–261. https://doi.org/10.1159/000205388
Wojcik M, Ramadori P, Blaschke M, Sultan S, Khan S, Malik IA, Naz N, Martius G, Ramadori G, Schultze FC (2012) Immunodetection of cyclooxygenase-2 (COX-2) is restricted to tissue macrophages in normal rat liver and to recruited mononuclear phagocytes in liver injury and cholangiocarcinoma. Histochem Cell Biol 137:217–233. https://doi.org/10.1007/s00418-011-0889-9
Acknowledgements
The authors thank Ms. Huifang Li, Mengli Zhu, and Yan Wang (Research Core Facility of West China Hospital, State Key Laboratory of Biotherapy, West China Hospital, Sichuan University) for technical assistance in flow cytometry. We thank Dr. Shisheng Wang (West China Hospital, Sichuan University) and Dr. Chengpin Shen (Omicsolution Co., Ltd) for advice about data analysis and free access to their 'Wu Kong' platform (https://www.omicsolution.com/wkomics/main/). A free online platform (http://www.bioinformatics.com.cn) was also utilized for data analysis and visualization.
Funding
This work was supported by the National Natural Science Fund of China (82200687, 82170623, 82170625, 82322011, 82241054, 82000613, and 82000574), the National Key R&D Program of China (2017YFA0205404), the Sichuan Science and Technology Program (24NSFSC0232, 21ZDYF1667, 2020YJ0084, 2021YFS0147, and 2022NSFSC0819), and the 135 projects for disciplines of excellence of West China Hospital, Sichuan University (ZYGD18004). The funding sources had no involvement in performing the study, writing of the report, or the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
LZ: study concept and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, obtained funding. CZ: acquisition of data, analysis and interpretation of data, drafting of the manuscript. WD: acquisition of data, analysis and interpretation of data, administrative, technical, or material support. HT: analysis and interpretation of data, administrative, technical, or material support, critical revision of the manuscript for important intellectual content, obtained funding. WY: analysis and interpretation of data, administrative, technical, or material support, obtained funding. ZH: administrative, technical, or material support, critical revision of the manuscript for important intellectual content, obtained funding. CT: study concept and design, critical revision of the manuscript for important intellectual content, study supervision, obtained funding. JG: study concept and design, critical revision of the manuscript for important intellectual content, study supervision, obtained funding. All authors have approved the final article.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
All animals received human care and study protocols complied with the guidelines of and were approved by Animal Use and Care Committee of West China Hospital, Sichuan University (No. 2021741A). The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki as reflected in a priori approval by the the Ethical Committee of West China Hospital (No. 2022989).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, L., Zhao, C., Dai, W. et al. Disruption of cholangiocyte-B cell crosstalk by blocking the CXCL12-CXCR4 axis alleviates liver fibrosis. Cell. Mol. Life Sci. 80, 379 (2023). https://doi.org/10.1007/s00018-023-05032-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-023-05032-y