Abstract
Introduction
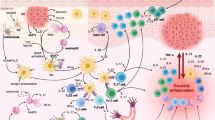
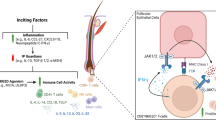
Psoriasis cellular hallmarks, such as the imbalance between Th1/Th17 and Th2 cytokines and the dysregulated expression of vascular endothelial growth factor (VEGF), inducible nitric oxide synthase, (iNOS) and indoleamine 2,3-dioxygenase (IDO), are all detectable in mesenchymal stem cells (MSCs) suggesting that psoriasis originates at mesenchymal level. Aim of the study: In this scenario, MSCs may become the new therapeutic target and interest in the effects of traditionally used drugs, such as Apremilast, on MSCs has greatly increased.
Materials and Methods
MSCs from control subjects (C-MSCs) and from psoriatic patients before (PsO MSCs T0) and after in vivo treatment with Apremilast (PsO-MSCs T12) were isolated and characterized; subsequently, the effects of Apremilast on VEGF, iNOS and IDO expression were evaluated by immunocytochemistry (ICC). The expression of VEGF, iNOS and IDO was also detected in skin sections by immunohistochemistry (IHC).
Results
The results indicate that in vivo administration of Apremilast is able to drive the altered profile of PsO-MSCs towards a more physiological pattern. In skin sections, the role of Apremilast is evident in reducing VEGF, iNOS and IDO expression.
Conclusion
Apremilast treatment influences the expression of VEGF, iNOS and IDO not only by keratinocytes but also by MSCs, restoring their intrinsic profile and their natural anti-inflammatory action, and decreasing the auto-inflammatory process that underpins the development of psoriasis.



Similar content being viewed by others
References
Quaglino P, Bergallo M, Ponti R, et al. Th1, Th2, Th17 and regulatory T cell pattern in psoriatic patients: modulation of cytokines and gene targets induced by etanercept treatment and correlation with clinical response. Dermatology. 2011;223:57–67.
Davidovici BB, Sattar N, Prinz J, et al. Psoriasis and systemic inflammatory diseases: potential mechanistic links between skin disease and co-morbid conditions. J Invest Dermatol. 2010;130:1785–2196.
Llamas-Velasco M, Bonay P, José Concha-Garzón M, et al. Immune cells from patients with psoriasis are defective in inducing indoleamine 2,3-dioxygenaseexpression in response to inflammatory. Br J Dermatol. 2017;176:695–704.
Sheipouri D, Grant R, Bustamante S, et al. Characterisation of the kynurenine pathway in skin-derived fibroblasts and keratinocytes. J Cell Biochem. 2015;116:903–22.
Asp L, Johansson AS, Mann A, et al. Effects of pro-inflammatory cytokines on expression of kynurenine pathway enzymes in human dermal fibroblasts. J Inflamm. 2011;8:25.
Campanati A, Orciani M, Sorgentoni G, et al. Indirect co-cultures of healthy mesenchymal stem cells restore the physiological phenotypical profile of psoriatic mesenchymal stem cells. Clin Exp Immunol. 2018a;193:234–40.
Campanati A, Orcian M, Consales V, et al. Characterization and profiling of immunomodulatory genes in resident mesenchymal stem cells reflect the Th1-Th17/Th2 imbalance of psoriasis. Arch Dermatol Res. 2014;306:915–20.
Orciani M, Campanati A, Salvolini E, et al. The mesenchymal stem cell profile in psoriasis. Br J Dermatol. 2011;165:585–92.
Campanati A, Orciani M, Lazzarini R, et al. TNF-α inhibitors reduce the pathological Th(1)-Th(17)/Th(2) imbalance in cutaneous mesenchymal stem cells of psoriasis patients. Exp Dermatol. 2017;26:319–24.
Campanati A, Orciani M, Gorbi S, et al. Effect of biologic therapies targeting tumour necrosis factor-α on cutaneous mesenchymal stem cells in psoriasis. Br J Dermatol. 2012;167:68–76.
Schett G, Sloan VS, Stevens RM, et al. Apremilast: a novel PDE4 inhibitor in the treatment of autoimmune and inflammatory diseases. Ther Adv Musculoskelet Dis. 2010;2:271–8.
Gottlieb AB, Strober B, Krueger JG, et al. An open-label, single-arm pilot study in patients with severe plaque-type psoriasis treated with an oral anti-inflammatory agent, apremilast. Curr Med Res Opin. 2008;24:1529–38.
Pincelli C, Schafer PH, French LE, Augustin M, Krueger JG. Mechanisms underlying the clinical effects of apremilast for psoriasis. J Drugs Dermatol. 2018;17(8):835–40.
Campanati A, Orciani M, Sorgentoni G, et al. Pathogenetic characteristics of mesenchymal stem cells in hidradenitis suppurativa. JAMA Dermatol. 2018b;154:1184–90.
Orciani M, Campanati A, Caffarini M, et al. T helper (Th)1, Th17 and Th2 imbalance in mesenchymal stem cells of adult patients with atopic dermatitis: at the origin of the problem. Br J Dermatol. 2017;176:1569–76.
Dominici M, Le Blanc K, Mueller I, et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 2006;8:315–7.
Campanati A, Orciani M, Ganzetti G, et al. The effect of etanercept on vascular endothelial growth factor production by cutaneous mesenchymal stem cells from patients with psoriasis. J Int Med Res. 2016;44:6–9.
Schafer PH, Parton A, Gandhi AK, et al. Apremilast, a cAMP phosphodiesterase-4 inhibitor, demonstrates anti-inflammatory activity in vitro and in a model of psoriasis. Br J Pharmacol. 2010;159:842–55.
Heidenreich R, Röcken M, Ghoreschi K. Angiogenesis drives psoriasis pathogenesis. Int J Exp Pathol. 2009;90:232–48.
Marina ME, Roman II, Constantin A-M, Mihu CM, Tătaru AD. VEGF involvement in psoriasis. Clujul Med. 2015;88:247–52.
Simonetti O, Lucarini G, Campanati A, et al. VEGF, survivin and NOS overexpression in psoriatic skin: critical role of nitric oxide synthases. J Dermatol Sci. 2009;54:205–8.
Cals-Grierson MM, Ormerod AD. Nitric oxide function in the skin. Nitric Oxide. 2004;10:179–93.
Kroll J, Waltenberger J. VEGF-A induces expression of eNOS and iNOS in endothelial cells via VEGF receptor-2 (KDR). Biochem Biophys Res Commun. 1998;252:743–6.
Merighi S, Gessi S, Varani K, et al. Hydrogen sulfide modulates the release of nitric oxide and VEGF in human keratinocytes. Pharmacol Res. 2012;66:428–36.
Ito M, Ogawa K, Takeuchi K, et al. Gene expression of enzymes for tryptophan degradation pathway is upregulated in the skin lesions of patients with atopic dermatitis or psoriasis. J Dermatol Sci. 2004;36:157–64.
Criado G, Simelyte E, Inglis JJ, et al. Indoleamine 2,3 dioxygenase-mediated tryptophan catabolism regulates accumulation of Th1/ Th17 cells in the joint in collagen-induced arthritis. Arthritis Rheum. 2009;60:1342–51.
Mancuso R, Hernis A, Agostini S, et al. Indoleamine 2,3 dioxygenase (IDO) expression and activity in relapsing-remitting multiple sclerosis. PLoS ONE. 2015;10:e0130715.
Trabanelli S. Indoleamine 2,3-dioxygenase in psoriasis: a defective mechanism. Br J Dermatol. 2017;176:570–2.
Ribatti D, Nico B, Crivellato E. The role of pericytes in angiogenesis. Int J Dev Biol. 2011;55:261–8.
Covas DT, Panepucci RA, Fonte AM, et al. Mesenchymal stem cells, fibroblasts and pericytes: different functional states of the same cell? Blood. 2005;106:4310.
Stapor PC, Sweat RS, Dashti DC, et al. Pericyte dynamics during angiogenesis: new insights from new identities. J Vasc Res. 2014;51:163–74.
Shin TH, Kim HS, Choi SW, et al. Mesenchymal stem cell therapy for inflammatory skin diseases: clinical potential and mode of action. Int J Mol Sci. 2017;18(2):244.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
All procedures were performed in accordance with the ethical standards of the institutional research committee (Università Politecnica delle Marche Ethical Commitee (Protocol 2016 0360 OR) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Responsible Editor: J. Di Battista.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Campanati, A., Caffarini, M., Diotallevi, F. et al. The efficacy of in vivo administration of Apremilast on mesenchymal stem cells derived from psoriatic patients. Inflamm. Res. 70, 79–87 (2021). https://doi.org/10.1007/s00011-020-01412-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-020-01412-3