Abstract
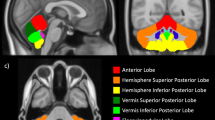
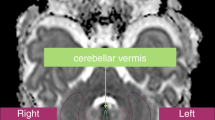
Unilateral atrophy of a cerebellar hemisphere occurring as a sequela of ischemic or destructive injury of the contralateral cerebral hemisphere is uncommon in children. We reviewed our experience with this phenomenon and found an unexpected association with extreme prematurity and a complicated perinatal course with a poor subsequent neurologic outcome. We retrospectively identified eight children, aged 8 months to 13 years, in whom cerebellar atrophy associated with cerebral injury was diagnosed on MR or CT, and reviewed their past medical history, neurologic findings, and neu-roimaging studies. Seven patients were born extremely premature, EGA 25–28 weeks, and had severe perinatal intracranial hemorrhage. Neurologic problems include severe developmental delay in seven, spastic paresis in six, and seizures in five. Neuroimaging showed severe unilateral holohemispheric atrophy in four, bilateral asymmetric holohemispheric atrophy in two, and left temporoparietal atrophy in one. Cerebellar atrophy was unilateral in five and bilateral but asymmetric in two. Gliosis of the atrophic cerebellum occurred in one patient. Sequential neuroimaging in one patient showed evolution of crossed cerebellar atrophy at 8 months of age. The final patient, a term infant, had an idiopathic perinatal left cerebral infarct. In our experience, crossed cerebellar atrophy was an uncommon manifestation of extreme prematurity complicated by severe intracranial hemorrhage and/or ischemic necrosis of white matter. The cerebellar atrophy is most often a secondary degenerative phenomenon rather than a result of direct cerebellar injury.
Similar content being viewed by others
References
Bouchareb M, Moulin T, Cattin F, et al (1988) Wallerian degeneration of the descending tracts: CT and MRI features of the brain stem. J Neuroradiol 15: 238–252
Hanyu H, Ayrai H, Katsunuma H, Fujita R, Tomori C (1991) Crossed cerebellar glucose metabolism in supratentorial tumors. Nippon Ronen Igakkai Zasshi 228:160–165
Lenzi GL, Frackowiak RSJ, Jones T (1982) Cerebral oxygen metabolism and blood flow in human cerebral ischemic infarction. J Cereb Blood Flow Metab 2: 321–335
Patronas NJ, di Chiro G, Smith BH, et al (1984) Depressed cerebellar glucose metabolism in supratentorial tumors. Brain Res 291: 93–101
Tien R, Ashdown B (1992) Crossed cerebellar diaschisis and crossed cerebellar atrophy: correlation or MR findings, clinical symptoms and supratentorial diseases in 26 patients. AJR 158: 1155–1159
Sasaki K, Oka H, Matsuda Y (1977) Electrophysiological studies of the projections from the parietal association area to the cerebellar cortex. Exp Brain Res 23: 91–102
Kushner JM, Alavi A, Reivich M, Dann R, Burke A, Robinson G (1984) Contralateral cerebellar hypometabolism following cerebral insult. Ann Neurol 15: 425–434
Eckard D, Purdy, Bonte F (1992) Crossed cerebellar diaschisis and loss of consciousness during temporary balloon occlusion of the internal carotid artery. AJNR 13: 55–57
Brunberg J, Frey K, Horton J, Kuhl D (1992) Crossed cerebellar diaschisis: occurrence and resolution demonstrated with PET during carotid temporary balloon occlusion. AJNR 13: 58–61
Baron JC, Bousse MG, Comar D, Castaigne P (1980) “Crossed cerebellar diaschisis” in human supratentorial infarction (abstract). Ann Neurol 8:128
Chung D (1985) Retrograde crossed cerebellar atrophy. Brain 108: 881–889
Flodmark O, Roland E, Hill A, Whitfield M (1987) Periventricular leukomalacia: radiologic diagnosis. Radiology 162: 119–124
Barkovich AJ, Truwit C (1989) Brain damage from perinatal asphyxia: correlation of MR findings with gestational age. AJNR 11:1087–1096
Guzzetta F, Shackelford G, Volpe JS, Perlman J, Volpe J (1986) Periventricular intraparenchymal echodensities in the premature newborn: critical determinant of neurologic outcome. Pediatrics 78: 995–1006
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rollins, N.K., Wen, T.S. & Dominguez, R. Crossed cerebellar atrophy in children: a neurologic sequela of extreme prematurity. Pediatr Radiol 25 (Suppl 1), S20–S25 (1995). https://doi.org/10.1007/BF03545574
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03545574