Abstract
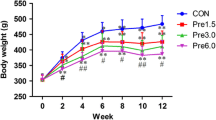
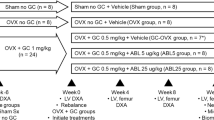
Glucocorticoid induced osteoporosis has been associated with high doses and it has been partially attributed to decreased absorption and to increased calcium excretion. The present study examined the effect of low but effective doses of methylprednisolone (MP) on calcium balance and on skeleton in rats. Total duration of the experiment 29 days. Thirty-one male Wistar rats (MP group) were injected with 4mg/kg body weight MP sc at the 1st, 11th and 20th day of the experiment and 28 rats (C group) were used as matched controls. The 1st, 11th and 20th day of the experiment rats were placed in individual metabolic cages for three days. Food and water consumption were measured at the 2nd and 3rd days after each injection; urine and faeces were collected at the same days for calcium estimation. Calcium intake and excretion after each injection was significantly lower in the MP group as compared to controls. A statistically significant positive correlation between calcium consumption and calcium excretion was found in both groups resulting in a negative final balance. Rats were killed the 29th day. Adrenal weight was statistically significant lower in MP group (p<0.001). Morphometric properties were evaluated for the right femur. No significant difference was found between the two groups. Mineral and calcium content was slightly increased in the MP group. According to these results, it seems that methylprednisolone while effective on HPA axis did not have any effect on calcium absorption and on bone calcium deposition in rats.
Similar content being viewed by others
References
Cushing H. The basophil adenomas of the pituitary body and their clinical manifestations (pituitary basophilism). Bull. Johns Hopkins 50: 137, 1932.
Goulding A., Gold E. Effects of dietary sodium chloride loading on parathyroid function, 1,25-dihydroxyvitamin D, calcium balance and bone metabolism in female rats during chronic prednisolone administration. Endocrinology 119: 2148, 1986.
Hahn T.J., Halstead L.R., Baran D.T. Effects of short term glucocorticoid administration on intestinal calcium absorption and circulating vitamin D metabolite concentrations in man. J. Clin. Endocrinol. Metab. 52: 111, 1981.
Kimberg D.V., Baerg R.D., Gesshon E., Gradusius R.T. Effect of cortisone treatment on the active transport of calcium by the small intestine. J. Clin. Invest. 50: 1309, 1971.
Morris H.A., Need A.G., O’Loughlin P.D. Malabsorption of calcium in corticosteroid -induced osteoporosis. Calcif. Tissue Int. 46: 305, 1990.
Need A.G., Hartley T.F., Philcox J.C., Nordin B.E.C. Calcium metabolism and osteoporosis in corticosteroid-treated postmenopausal women. Aust. NZ. J. Med. 16: 341, 1986.
Nielsen H.K., Thomsen K., Eriksen E.F., Charles P., Storm T., Moseklide L. The effects of high dose glucocorticoid administration on serum bone gamma carboxyglutamic acid-containing protein, serum alkaline phosphatase and vitamin D metabolites in normal subject. Bone Miner 4: 105, 1988.
Suzuki Y., Ichikawa Y., Saito E., Homme M. Importance of increased urinary calcium excretion in the development of secondary hyperparathyroidism of patients under glucocorticoid therapy. Metabolism 32: 151, 1983.
Chyun Y.S., Kream B.E., Raisz L.G. Cortisol decreases bone formation by inhibiting periostal cell proliferation. Endocrinology 114: 477, 1984.
Haussler M.R., Manolagas S.C., Deftos L.J. Glucocorticoid receptor in clonal osteosarcoma cell lines: A novel system for investigating bone active hormones. Biochem. Biophys Res. Commun. 94: 373, 1980.
Hughes-Fulfold M., Appel R., Kumegawa M., Schmidt J. Effect of sex on proliferating osteoblasts. Inhibition of prostaglandin E2 synthesis, DNA synthesis and alterations in actin cytoskeleton. Exp. Cell Res. 203: 150, 1992.
Wong G.L Basal activities and hormone responsiveness of osteoclast-like and osteoblast-like bone cells are regulated by glucocorticoids. J. Biol. Chem. 254: 6337, 1979.
Adinoff A.D., Hollister J.R. Steroid induced fractures and bone loss in patients with asthma. N. Engl. J. Med. 309: 265, 1983.
Dempster D.W., Arlott M.A., Meunier P.J. Mean wall thickness and formation periods of trabecular bone packets in corticosteroid-induced osteoporosis. Calcif. Tissue Int. 35: 410, 1983.
Greenberger P.A., Hendrix R.W., Patterson R., Chmill J.S. Bone studies in patients on prolonged systemic corticosteroid therapy for asthma. Clin. Allergy 12: 363, 1982.
Lo Cascio V., Bonucci E., Imbimbo B., Ballanti P., Adami S., Milani S., Tartarotti D., Delia Rocca C. Bone loss in response to long term glucocorticoid therapy. Bone Miner. 8: 39, 1990.
Gordan G.S, Eisenberg E. The effect of oestrogens, androgens and corticoids on skeletal kinetics in man. Proc. Roy. Soc. Med. 56: 1027, 1963.
Deuxchaisnes C.N., Devogelaer J.P., Esselinckx W., Bouchez B., Depresseux G., Rombouts-Lindemans C., Huaux J.P. The effect of low dosage glucocorticoids on bone mass in rheumatoid arthritis: a cross sectional and a longitudinal study using single photon absorptiometry. Adv. Exp. Med. Biol. 171: 210, 1984.
Lukert B.P., Raisz L.G. Glucocorticoid-induced osteoporosis:pathogenesis and management. Ann. Intern. Med. 112: 352, 1990.
Moulding A., Gold E. Effects of chronic prednisolone treatment on bone resorption and bone composition in intact and ovariectomized rats receiving β-estradiol. Endocrinology 122: 482, 1988.
Quarles L.D. Prednisone-induced osteopenia in beagles, variable effects by differential suppression of bone formation. Am. J.Physiol. 263: E136, 1992.
Gluck O.S., Murphy W.A., Hahn T.J., Hahn B. Bone loss in adults receiving alternate glucocorticoid therapy. A comparison with daily therapy. Arthritis Rheum. 24: 892, 1981.
Ruegsegger P., Medici T.C., Anliker M. Corticosteroid induced bone loss. A longitudinal study of alternate day therapy in patients with bronchial asthma using quantitative computed tomography. Eur. J. Clin. Pharmacol. 25: 615, 1983.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Voulgaris, A., Liapi, C. & Papadopoulos, J. Effect of low-dose methylprednisolone on calcium balance and bone composition in rats. J Endocrinol Invest 20, 659–663 (1997). https://doi.org/10.1007/BF03348027
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03348027