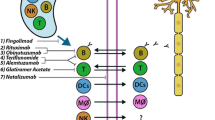
Summary
Copolymer-1 is a mixture of synthetic random polypeptides composed of 4 amino acids. In a variety of animal species, including primates, it suppresses experimental allergic encephalomyelitis, an approximate model of multiple sclerosis. In vitro experiments using murine and human T cell lines demonstrate that copolymer-1 inhibits the binding of some myelin proteins to the major histocompatibility complex.
Although reactive antibodies to copolymer-1 were observed in most patients receiving the drug in a trial, available evidence suggests that these antibodies do not neutralise the clinical effectiveness of copolymer-1.
In monkeys, subcutaneous copolymer-1 is quickly absorbed with a time to maximum plasma concentration of 2 to 4 hours. Therapeutic doses of subcutaneous copolymer-1 are unlikely to produce detectable plasma concentrations in patients because of rapid metabolism to smaller peptide fragments.
Compared with placebo (n = 126), subcutaneous copolymer-1 20mg once daily (n = 125) for up to 2.5 years significantly reduced the annual relapse rate by 30% and slowed the progression of disability in patients with relapsing-remitting multiple sclerosis. Copolymer-1 was more beneficial to patients with little initial accumulated neurological disability than more severely affected patients. In a smaller trial, also involving patients with relapsing-remitting multiple sclerosis, copolymer-1 20mg once daily (n = 25) caused a 76% reduction in the annual relapse rate compared with placebo (n = 23). However, in patients with secondary progressive multiple sclerosis, subcutaneous copolymer-1 15mg twice daily (n =51) for 2 years was not shown to be effective in slowing disease progression in comparison to placebo (n = 55).
In clinical trials, injection site reactions were the most common adverse effects associated with copolymer-1 treatment, with 90 and 59% of copolymer-1 (n = 125) and placebo (n = 126) recipients reporting ≥1 reaction from an average of about 730 injections in 1 trial. A transient benign systemic reaction characterised by flushing, chest tightness, dyspnoea, palpitations or anxiety occurred more frequently with copolymer-1 than placebo. Nine to 15% of patients receiving copolymer-1 20mg once daily reported this reaction at least once, compared with 0 to 3% of placebo recipients.
Overall, copolymer-1 causes few serious adverse effects and appears to be effective in slowing the relapse rate and progression of disability of patients with relapsing-remitting multiple sclerosis. However, it has not been shown to be effective for the treatment of the secondary progressive form of the disease. Copolymer-1 can thus be considered a significant addition to the limited armoury of drugs for the treatment of patients with multiple sclerosis.
Similar content being viewed by others
References
Becker CC, Gidal BE, Fleming JO. Immunotherapy in multiple sclerosis, part 1. Am J Health System Pharm 1995 Sep 15; 52: 1985–2000
Anderson DW, Ellenburg JH, Leventhal CM, et al. Revised estimate of the prevalence of multiple sclerosis in the United States. Ann Neurol 1992; 31(3): 333–6
Lublin FD, Reingold SC, National Multiple Sclerosis Society (USA) Advisory Committee on Trials of New Agents in Multiple Sclerosis. Defining the clinical course of multiple sclerosis. Results of an international survey. Neurology 1996; 46: 907–11
Goodkin DE, Hertsgaard D, Rudick RA. Exacerbation rates and adherence to disease type in a prospectively followed-up population with multiple sclerosis. Arch Neurol 1989; 46: 1107–12
McDonald WI, Miller DH, Thompson AJ. Are magnetic resonance findings predictive of clinical outcome in therapeutic trials in multiple sclerosis? The dilemma of interferon-β. Ann Neurol 1994; 36(1): 14–7
Mushlin AI, Detsky AS, Phelps CE, et al. The accuracy of magnetic resonance imaging in patients with suspected multiple sclerosis. JAMA 1993 Jun 23/30; 269(24): 3146–51
Sinnige LGF, Teeuwissen E, Hew JM, et al. Correlation between magnetic resonance imaging and clinical parameters in multiple sclerosis. Acta Neurol Scand 1995; 91: 188–91
Rieumont MJ, Deluca SA. Neuroimaging evaluation in multiple sclerosis. Am Fam Phys 1993; 48(2): 273–6
Ebers GC. Treatment of multiple sclerosis. Lancet 1994 Jan 29; 343: 275–9
Miller DH, Thompson AJ, Morrissey SP, et al. High dose steroids in acute relapses of multiple sclerosis: MRI evidence for a possible mechanism of therapeutic effect. J Neurol Neuro-surg Psychiatry 1992; 55: 450–3
Kinkel RP, Goodkin DE. Immunotherapy for multiple sclerosis. A review of the clinical experience. Clin Immunother 1994 Feb; 1: 117–34
van Oosten BW, Truyen L, Barkhof F, et al. Multiple sclerosis therapy: a practical guide. Drugs 1995 Feb; 49: 200–12
Martin R, McFarland HF. Immunological aspects of experimental allergic encephalomyelitis and multiple sclerosis. Crit Rev Clin Lab Sci 1995; 32(2): 121–82
Traugott E, Lebon P. Multiple sclerosis: involvement of interferons in lesion pathogenesis. Ann Neurol 1988; 24: 243–51
Vartdal F. HLA associations in multiple sclerosis: implications for immunopathogenesis. Res Immunol 1989; 140: 192–6
Marrosu MG, Muntoni F, Murru MR, et al. Sardinian multiple sclerosis is associated with HLA-DR4: a serologic and molecular analysis. Neurology 1988; 38: 1749–53
Jersild C, Fog T, Hansen GS, et al. Histocompatibility determinants in multiple sclerosis, with special reference to clinical course. Lancet 1973 Dec 1; II: 1221–5
Chofflon M, Weiner HL, Morimoto C, et al. Loss of functional suppression is linked to decrease in circulating suppressor inducer (CD4+ 2H4+) T cells in multiple sclerosis. Ann Neurol 1988; 24: 185–91
Reinherz EL, Weiner HL, Hauser SL, et al. Loss of suppressor T cells in active multiple sclerosis: analysis with monoclonal antibodies. N Engl J Med 1980 Jul 17; 303(3): 125–9
Traugott U, Reinherz EL, Raine CS. Multiple sclerosis: distribution of T cells, T cell subsets and la-positive macrophages in lesions of different ages. J Neuroimmunol 1983; 4: 201–21
Antel JP, Arnason BGW, Medof ME. Suppressor cell function in multiple sclerosis: correlation with clinical disease activity. Ann Neurol 1979; 5: 338–42
Hafler DA, Weiner HL. MS: a CNS and systemic autoimmune disease. Immunol Today 1989; 10(3): 104–7
Hauser SL, Dawson DM, Lehrich JR, et al. Intensive immunosuppression in progressive multiple sclerosis: a randomized, three-arm study of high-dose intravenous cyclophosphamide, plasma exchange, and ACTH. N Engl J Med 1983 Jan 27; 308(4): 173–80
Panitch HS, Hirsch RL, Haley AS, et al. Exacerbations of multiple sclerosis in patients treated with gamma interferon. Lancet 1987 Apr 18; 8538: 893–5
Compston A. Future prospects for the management of multiple sclerosis. Ann Neurol 1994; 36 Suppl.: S146–150
Johnson KP, Brooks BR, Cohen JA, et al. Copolymer 1 reduces relapse rate and improves disability in relapsing-remitting multiple sclerosis: results of a phase III multicenter, double-blind, placebo-controlled trial. Neurology 1995 Jul; 45: 1268–76
Teitelbaum D, Meshorer A, Hirshfeld T, et al. Suppression of experimental allergic encephalomyelitis by a synthetic polypeptide. Eur J Immunol 1971; 1: 242–8
Arnon R. The development of Cop 1 (Copaxone®), an innovative drug for the treatment of multiple sclerosis: personal reflections. Immunol Lett 1996; 50: 1–15
Arnon R, Teitelbaum D, Sela M. Suppression of experimental allergic encephalomyelitis by COP1 — relevance to multiple sclerosis. Isr J Med Sci 1989 Dec; 25: 686–9
Ben-Nun A, Mendel I, Bakimer R, et al. The autoimmune reactivity to myelin oligodendrocyte glycoprotein (MOG) in multiple sclerosis is potentially pathogenic: effect of copolymer 1 on MOG-induced disease. J Neurology 1996; 243 Suppl. 1: S14–22
Bernard CCA, Kerlero de Rosbo N. Multiple sclerosis: an autoimmune disease of multifactorial etiology. Curr Opin Immunol 1992; 4: 760–5
Arnon R, Teitelbaum D. Immunomodulation of experimental allergic encephalomyelitis. Isr J Med Sci 1993; 29(2–3): 175–81
Kerlero de Rosbo N, Milo R, Lees MB, et al. Reactivity to myelin antigens in multiple sclerosis. Peripheral blood lymphocytes respond predominantly to myelin oligodendrocyte glycoprotein. J Clin Invest 1993; 92: 2602–8
Lisak RP, Zweiman B, Blanchard N, et al. Effect of treatment with Copolymer 1 (Cop-1) on the in vivo and in vitro manifestations of experimental allergic encephalomyelitis (EAE). J Neurol Sci 1983 Dec; 62: 281–93
Wisniewski HM, Keith AB. Chronic relapsing experimental allergic encephalomyelitis: an experimental model of multiple sclerosis. Ann Neurol 1977; 1(2): 144–8
Teitelbaum D, Webb C, Meshorer A, et al. Suppression by several polypeptides of experimental allergic encephalomyelitis induced in guinea pigs and rabbits with bovine and human basic encephalitogen. Eur J Immunol 1973; 3: 273–9
Teitelbaum D, Fridkis-Hareli M, Arnon R, et al. Copolymer-1 inhibits chronic relapsing experimental allergic encephalomyelitis induced by proteolipid protein (PLP) peptides in mice and interferes with PLP-specific T cell responses. J Neuroimmunol 1996; 64: 209–17
Webb C, Teitelbaum D, Arnon R, et al. In vivo and in vitro immunological cross-reactions between basic encephalotigen and synthetic basic polypeptides capable of suppressing experimental allergic encephalomyelitis. Eur J Immunol 1973; 3: 279–86
Teitelbaum D, Aharoni R, Sela M, et al. Cross-reactions and specificities of monoclonal antibodies against myelin basic protein and against the synthetic copolymer 1. Proc Natl Acad Sci USA 1991 Nov 1; 88: 9528–32
Guéry J-C, Adorini L. Selective immunosuppression of class II-restricted T cells by MHC class II-binding peptides. Crit Rev Immunol 1993; 13: 195–206
Lando Z, Teitelbaum D, Arnon R. Effect of cyclophosphamide on suppressor cell activity in mice unresponsive to EAE. J Immunol 1979 Nov; 123: 2156–60
Lando Z, Teitelbaum D, Arnon R. The immunological response in mice unresponsive to experimental allergic encephalomyelitis. J Immunol 1981; 126: 1526–8
Lando Z, Dori Y, Teitelbaum D, et al. Unresponsiveness to experimental allergic encephalomyelitis in mice: replacement of suppressor cells by a soluble factor. J Immunol 1981; 127: 1915–9
Aharoni R, Teitelbaum D, Arnon R. T suppressor hybridomas and interleukin-2-dependent lines induced by copolymer 1 or by spinal cord homogenate down-regulate experimental allergic encephalomyelitis. Eur J Immunol 1993 Jan; 23: 17–25
Arnon R, Sela M, Teitelbaum D. New insights into the mechanism of action of copolymer 1 in experimental allergic encephalomyelitis and multiple sclerosis. J Neurology 1996; 243 Suppl. 1: S8–13
Fridkis-Hareli M, Teitelbaum D, Gurevich E, et al. Direct binding of myelin basic protein and synthetic copolymer 1 to class II major histocompatibility complex molecules on living antigen-presenting cells — specificity and promiscuity. Proc Natl Acad Sci USA 1994 May 24; 91: 4872–6
Teitelbaum D, Milo R, Arnon R, et al. Synthetic copolymer 1 inhibits human T-cell lines specific for myelin basic protein. Proc Natl Acad Sci USA 1992 Jan 1; 89: 137–41
Teitelbaum D, Aharoni R, Arnon R, et al. Specific inhibition of the T-cell response to myelin basic protein by the synthetic copolymer Cop 1. Proc Natl Acad Sci USA 1988 Dec; 85: 9724–8
Racke MK, Martin R, McFarland H, et al. Copolymer-1-induced inhibition of antigen-specific T cell activation: interference with antigen presentation. J Neuroimmunol 1992 Mar; 37: 75–84
Fridkis-Hareli M, Teitelbaum D, Arnon R, et al. Synthetic copolymer 1 and myelin basic protein do not require processing prior to binding to class II major histocompatibility complex molecules on living antigen-presenting cells. Cell Immunol 1995 Jul; 163: 229–36
Milo R, Panitch H. Additive effects of copolymer-1 and interferon β-1b on the immune response to myelin basic protein. J Neuroimmunol 1995; 61: 185–93
Govaerts A, Gony J, Martin-Mondière C, et al. HLA and multiple sclerosis: population and families study. Tissue Antigens 1985; 25: 187–99
Johnson KP, U.S. Phase III Copolymer 1 Study Group. Antibodies to copolymer-1 do not interfere with its clinical effect [abstract]. Ann Neurol 1995 Dec; 38: 973
Kott E, Radnay Y, Yochay Y. COP I increases suppressor cell number in multiple sclerosis [abstract]. J Neurology 1995; 242 Suppl. 2: S37–38
Burns J, Krasner J, Guerrero F. Human cellular response to copolymer 1 and myelin basic protein. Neurology 1986; 36: 92–4
Burns J, Littlefield K. Failure of copolymer I to inhibit the human T-cell response to myelin basic protein. Neurology 1991 Aug; 41: 1317–9
Baumhefner RW, Tourtellotte WW, Syndulko K, et al. Copolymer 1 as therapy for multiple sclerosis: the cons. Neurology 1988 Jul; 38 (7 Suppl. 2): 69–72
Lobel E, Riven-Krietman R, Amselem A, et al. Copolymer-1. Drugs Future 1996 Feb; 21(2): 131–4
Johnson KP. A review of the clinical efficacy profile of copolymer 1: new U.S. phase III trial data. J Neurology 1996; 243 Suppl. 1: S3–7
Bornstein MB, Miller A, Slagle S, et al. A pilot trial of Cop 1 in exacerbating-remitting multiple sclerosis. N Engl J Med 1987 Aug 13; 317: 408–14
Bornstein MB, Miller A, Slagle S, et al. A placebo-controlled, double-blind, randomized, two-center, pilot trial of Cop 1 in chronic progressive multiple sclerosis. Neurology 1991 Apr; 41: 533–9
Abramsky O, Teitelbaum D, Arnon R. Effect of a synthetic polypeptide (COP 1) on patients with multiple sclerosis and with acute disseminated encephalomyelitis. Preliminary report. J Neurol Sci 1977 Apr; 31: 433–8
Kurtzke JF. A proposal for a uniform minimal record of disability in multiple sclerosis. Acta Neurol Scand 1981; 87 Suppl. 1: 110–29
Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 1983; 33: 1444–52
Johnson KP, The U.S. Phase III Copolymer 1 Study Group. Copolymer 1: multicenter multiple sclerosis trial extension shows improved effects on relapse rate and disability [abstract]. Ann Neurol 1995 Dec; 38: 971
Johnson KP, The Copolymer 1 Multiple Sclerosis Study Group. Extended report of the positive multicenter phase III trial of copolymer 1 for the treatment of relapsing remitting multiple sclerosis [abstract]. Neurology 1996 Feb; 46(2) Suppl.: A406
Cohen JA, Grossman RI, Udupa JK, et al. Assessment of the efficacy of copolymer-1 in the treatment of multiple sclerosis by quantitative MRI [abstract]. Neurology 1995 Apr; 45 Suppl. 4: A418
Mancardi GL, Sardanelli F, Parodi RC, et al. The activity of copolymer-1 on gadolinium enhanced MRI lesions in relapsing remitting multiple sclerosis [abstract no. P277]. J Neurology 1996; 243(6) Suppl. 2: S13
Poser CM, Paty DW, Scheinberg L, et al. New diagnostic criteria for multiple sclerosis: guidelines for research protocols. Ann Neurol 1983; 13(3): 227–31
Goodkin DE, Ransohoff RM, Rudick RA. Experimental therapies for multiple sclerosis: current status. Cleve Clin J Med 1992 Jan–Feb; 59: 63–74
Carter JL. Disease modifying therapies for multiple sclerosis. CNS Drugs 1995 Feb; 3: 99–114
Becker CC, Gidal BE, Fleming JO. Immunotherapy in multiple sclerosis, part 2. Am J Health System Pharm 1995 Oct 1; 52: 2105–20
Product news: Betaserons® approved for MS. Inpharma 1993 Jul 31; 898: 27
Market news: Update on interferon beta-1b license for multiple sclerosis in the UK. Pharm J 1995 Aug 1; 255: 202
The IFNB Multiple Sclerosis Study Group and the University of British Columbia MS/MRI Analysis Group. Interferon beta-1b in the treatment of multiple sclerosis: final outcome of the randomized controlled trial. Neurology 1995; 45: 1277–85
Jacobs LD, Cookfair DL, Rudick RA, et al. Intramuscular interferon beta-1a for disease progression in relapsing multiple sclerosis. Ann Neurol 1996; 39: 285–94
Noseworthy JH, Ebers GC, Vandervoort MK, et al. The impact of blinding on the results of a randomized, placebo-controlled multiple sclerosis clinical trial. Neurology 1994 Jan; 44: 16–20
Ellison GW, Myers LW, Leake BD, et al. Design strategies in multiple sclerosis clinical trials. Ann Neurol 1994; 36 Suppl.: S108–112
McDonald E. Disease-modifying therapies for multiple sclerosis. Curr Ther 1995 Oct; 36: 47–53
The IFNB Multiple Sclerosis Study Group. Interferon beta-1b is effective in relapsing-remitting multiple sclerosis. I. Clinical results of a multicenter, randomized, double-blind, placebo-controlled trial. Neurology 1993; 43: 655–61
Wolinsky JS. Copolymer 1: a most reasonable alternative therapy for early relapsing-remitting multiple sclerosis with mild disability. Neurology 1995 Jul; 45: 1245–7
First approval for Avonex — in the US. Scrip 1996 May 24; 2131: 19
Teva Copaxone price estimated at $7,000–$10,000 per year per patient, the company tells Lehman Bros, meeting. FDC Rep Pink Sheet 1996 May 20
Walley T, Barton S. A purchase perspective of managing new drugs: interferon beta as a case study. BMJ 1995; 311: 796
Gunderson G-H. The impact of new pharmaceutical agents on the cost of neurologic care. Neurology 1995; 45: 569–72
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: R. Arnon, Department of Chemical Immunology, The Weizmann Institute of Science, Rehovot, Israel; D. Buljevac, Department of Neurology, University Hospital Dijkzigt Rotterdam, Rotterdam, The Netherlands; A. Coles, Department of Neurology, Addenbrooke’s Hospital, Cambridge, England; L. Durelli, Clinica Neurologica, Università di Torino, Turin, Italy; A. Goonetilleke, Department of Neurology, Middlesbrough General Hospital, Middlesbrough, England; J.W. Hadden, Department of Internal Medicine, University of South Florida, Tampa, Florida, USA; H.P. Hartung, Neurologische Universitätsklinik, Julius-Maximilians-Universität, Würzburg, Germany; E. McDonald, Multiple Sclerosis Society of Victoria, Toorak, Victoria, Australia; P.K. Newman, Department of Neurology, Middlesbrough General Hospital, Middlesbrough, England; H. Panitch, Department of Neurology, University of Maryland Hospital, Baltimore, Maryland, USA; C.H. Polman, Department of Neurology, Free University Hospital, Amsterdam, The Netherlands.
Rights and permissions
About this article
Cite this article
Lea, A.P., Goa, K.L. Copolymer-1. Clin. Immunother. 6, 319–331 (1996). https://doi.org/10.1007/BF03259096
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03259096