Abstract
Background: Myopathic complaints are common in the general population and are more frequent with increasing age. When myopathic symptoms arise in a patient treated with a HMG-CoA reductase inhibitor (statin), it is always a question of whether the symptoms are due to statin-induced myopathy (SIM) or not (non-SIM). Diagnosis of SIM is not as straightforward as previously thought, because the most commonly used biomarker, serum creatine kinase, shows low specificity and selectivity, except in serious cases of rhabdomyolysis. There is a definite need for a novel biomarker for SIM.
Objective: Based on a previous study reporting an altered metabolic profile with increased systemic exposure to the suspected muscle-toxic metabolite atorvastatin lactone in patients with SIM compared with healthy controls, this study aimed to explore the use of atorvastatin metabolite measurements to diagnose muscular complaints during statin treatment as being either SIM or non-SIM.
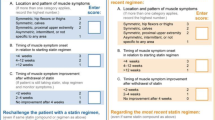
Patients, Setting, and Study Design: Fifty-three patients with self-reported myopathic symptoms during atorvastatin treatment were recruited from our outpatient clinic. The symptoms were clinically evaluated as being SIM or non-SIM, on the basis of atorvastatin re-challenge testing. Atorvastatin and its metabolites were measured at steady state in all patients and compared with the clinical evaluation to see if this could predict the outcome and hence be suitable as a diagnostic tool for SIM.
Main Outcome Measure: This was an exploratory study to investigate the proportion of patients correctly diagnosed by different metabolite cut-off ratios.
Results: With a cut-off ratio set at 1.1 for the atorvastatin lactone to atorvastatin acid ratio, 15 of 28 SIM patients (sensitivity of 54%) and 20 of 24 non-SIM patients (specificity of 83%) were correctly diagnosed. This corresponds to a positive predictive value of 79% and a negative predictive value of 61% (p = 0.006).
Conclusion: The present study confirms an altered metabolic pattern of atorvastatin in patients with SIM and substantiates a central role of the lactone forms of statins in future investigations of statin myotoxicity. The atorvastatin lactone to acid ratio seems to be a valuable supportive diagnostic tool with high specificity and moderate sensitivity, adding to ordinary clinical evaluations when diagnosing SIM.
Trial registration number (clinicaltrials.gov): NCT00414531




Similar content being viewed by others
References
Abourjaily HM, Alsheikh-Ali AA, Karas RH. Comparison of the frequency of adverse events in patients treated with atorvastatin or simvastatin. Am J Cardiol 2003; 91(8): 999–1002
Omar MA, Wilson JP. FDA adverse event reports on statin-associated rhabdomyolysis. Ann Pharmacother 2002; 36(2): 288–95
Graham DJ, Staffa JA, Shatin D, et al. Incidence of hospitalized rhabdomyolysis in patients treated with lipid-lowering drugs. JAMA 2004; 292(21): 2585–90
Arora R, Liebo M, Maldonado F. Statin-induced myopathy: the two faces of Janus. J Cardiovasc Pharmacol Ther 2006; 11(2): 105–12
Phillips PS, Haas RH, Bannykh S, et al. Statin-associated myopathy with normal creatine kinase levels. Ann Intern Med 2002; 137(7): 581–5
Thompson PD, Clarkson P, Karas RH. Statin-associated myopathy. JAMA 2003; 289(13): 1681–90
Joy TR, Hegele RA. Narrative review: statin-related myopathy. Ann Intern Med 2009; 150(12): 858–68
Chatzizisis YS, Koskinas KC, Misirli G, et al. Risk factors and drug interactions predisposing to statin-induced myopathy: implications for risk assessment, prevention and treatment. Drug Saf 2010; 33(3): 171–87
Schachter M. Chemical, pharmacokinetic and pharmacodynamic properties of statins: an update. Fundam Clin Pharmacol 2005; 19(1): 117–25
Jacobsen W, Kuhn B, Soldner A, et al. Lactonization is the critical first step in the disposition of the 3-hydroxy-3-methylglutaryl-CoA reductase inhibitor atorvastatin. Drug Metab Dispos 2000; 28(11): 1369–78
Prueksaritanont T, Subramanian R, Fang X, et al. Glucuronidation of statins in animals and humans: a novel mechanism of statin lactonization. Drug Metab Dispos 2002; 30(5): 505–12
Kearney AS, Crawford LF, Mehta SC, et al. The interconversion kinetics, equilibrium, and solubilities of the lactone and hydroxyacid forms of the HMG-CoA reductase inhibitor, CI-981. Pharm Res 1993; 10(10): 1461–5
Williams D, Feely J. Pharmacokinetic-pharmacodynamic drug interactions with HMG-CoA reductase inhibitors. Clin Pharmacokinet 2002; 41(5): 343–70
Riedmaier S, Klein K, Hofmann U, et al. UDP-glucuronosyltransferase (UGT) polymorphisms affect atorvastatin lactonization in vitro and in vivo. Clin Pharmacol Ther 2009; 87(1): 65–73
Lennernäs H. Clinical pharmacokinetics of atorvastatin. Clin Pharmacokinet 2003; 42(13): 1141–60
Skottheim IB, Gedde-Dahl A, Hejazifar S, et al. Statin induced myotoxicity: the lactone forms are more potent than the acid forms in human skeletal muscle cells in vitro. Eur J Pharm Sci 2008; 33(4-5): 317–25
Hermann M, Bogsrud MP, Molden E, et al. Exposure of atorvastatin is unchanged but lactone and acid metabolites are increased several-fold in patients with atorvastatin-induced myopathy. Clin Pharmacol Ther 2006; 79(6): 532–9
Hermann M, Christensen H, Reubsaet JLE. Determination of atorvastatin and metabolites in human plasma with solid-phase extraction followed by LC-tandem MS. Anal Bioanal Chem 2005; 382(5): 1242–9
Skottheim IB, Stormark K, Christensen H, et al. Significantly altered systemic exposure to atorvastatin acid following gastric bypass surgery in morbidly obese patients. Clin Pharmacol Ther 2009; 86(3): 311–8
Laaksonen R, Janis MT, Oresic M. Lipidomics-based safety biomarkers for lipid-lowering treatments. Angiology 2008; 59(2 Suppl.): 65S–68S
Link E, Parish S, Armitage J, et al. SLCO1B1 variants and statin-induced myopathy: a genomewide study. N Engl J Med 2008; 359(8): 789–99
Acknowledgments
Ine B. Skottheim and Martin P. Bogsrud contributed equally to this work.
There are no conflicts of interest.
The authors would like to thank Arne Svilaas, Kjell-Erik Arnesen, Gisle Langslet, and Leiv Ose at Lipidklinikken, Rikshospitalet, Oslo University Hospital (Oslo, Norway) for help with recruiting patients; Anne Blegstad at Lipidklinikken, Rikshospitalet, Oslo University Hospital, and Siri Johannesen at the School of Pharmacy, University of Oslo (Oslo, Norway), for their much appreciated help with the plasma sampling; and Stein Bergan and co-workers at the Department of Medical Biochemistry, Oslo University Hospital (Oslo, Norway) for other chemistry analyses.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Skottheim, I.B., Bogsrud, M.P., Hermann, M. et al. Atorvastatin Metabolite Measurements as a Diagnostic Tool for Statin-Induced Myopathy. Mol Diag Ther 15, 221–227 (2011). https://doi.org/10.1007/BF03256413
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03256413