Abstract
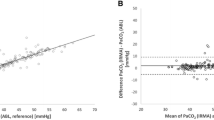
Transcutaneous oxygen tension (PiCO2) was measured in 30 patients scheduled for elective pulmonary resection requiring one-lung ventilation during anaesthesia. Simultaneous PtcO2 and arterial oxygen tension (PaO2) measurements were taken preoperatively (preop), intraoperatively during two-lung endotracheal (ET) and one-lung endobronchial ventilation (EB), and postoperatively (postop). There was a significant correlation (r) between PtcO2 and PaO2 at all time periods: 0.97 (preop); 0.91 (ET); 0.83 (EB);0.8I (postop). There were no significant differences among the transcutaneous oxygen indices (tcO2 index = PtcO2 IPaO2) in the preop (0.69 ± 0.09), ET (0.68 ± 0.10) andpostop (0.71 ± 0.12) time period. The tcO2 index was significantly lower during one-lung anaesthesia (0.61 ± 0.14). The PtcO2 was consistently lower than the corresponding PaO2 measurement, thus providing a continuous estimation of the“minimum” PaO2 level throughout anaesthesia and recovery. In four patients a marked drop in PtcO2 occurred just after the initiation of one-lung ventilation. In three, this was associated with arterial hypoxaemia and in one, haemo-dynamic compromise. In all four cases the PtcO2 was the first monitored parameter to change. As there is a substantial risk of developing hypoxaemia during thoracic anaesthesia, PtcO2 monitoring provides valuable early warning of impending hypoxaemia or haemodynamic compromise, thereby facilitating early therapeutic intervention.
Résumé
La tension d’oxygène transcutanée (PtcU2) était mesurée chez 30 patients cédulés pour résection pulmonaire élective requérant une ventilation d’un seul poumon durant l’anesthésie. La mesure simultanée de la PtcO2 et de la tension artérielle d’oxygène fPaO2) étaient faites en préopératoire (prêop), peropératoire durant la ventilation des deux poumons par tube endotrachêal (ET) et lors de la ventilation endobronchique a” un seul poumon (EB), ainsi qu’en période postopératoire (postop). lly avait une corrélation significative (r) entre la PtcO2 et la PaO2 à tous les temps étudiés: 0.97 (préop); 0.91 (ET); 0.83 (EB); 0.81 (postop). Il n’y avait aucune différence significative entre les indices transcutanés d’oxygène (tcO2 index = PtcO2IPaO2) dans la période préopératoire (0.69 ± 0.09). ET (0.68 ± 0.10) et postop (0.71 ± 0.12). L’index tcO2 était significativement plus bas lors de l’anesthésie avec un poumon unique (0.61 ± 0.14). La PtcO2 était constamment plus basse que la mesure correspondante du PaO2, fournissant ainsi une estimation continue de la valeur minimale de la PaO2 à travers l’anesthésie et le réveil. Chez quatre patients une diminution marquée de la PtcO2 est survenue juste après le début de la ventilation à un seul poumon. Chez trois de ces patients, ceci fut associé avec une hypoxémie artérielle tandis que dans l’ature elle s’est accompagnée d’un état hémodynamique compromis. Pour chacun, de ces quatre patients la PtcO2 était le premier paramètre surveillé à accuser des changements. Etant donné qu’il y a un risque substantiel de développer de l’hypoxémie lors de l’anesthésie thoracique, la surveillance de la PtcO2 fournit un indice précieux d’avertissement contre l’hypoxémie ou l’état hémodynamique compromis facilitant ainsi une intervention thérapeutique précoce.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Benumof JL, Alfery DD. Anesthesia for thoracic surgery. Chap. 40. In: Anesthesia, Miller RD, (Ed), Second Edition. New York, Churchill-Livingstone, 1986; 1371–1462.
Rafferty TD, Marrero O, Nardi D, Schachter EN, Menlelos R, Ngeow YF. Transcutaneous PO2 as a trend indicator of arterial PO2 in normal anesthetized adults. Anesth Anaig 1982; 61: 252–5.
Dennhardt T, Fricke M, Mahal S, Huch A, Huch R. Transcutaneous PO2 monitoring in anesthesia. Eur J Intensive Care Med 1976; 2: 29–33.
Tremper KK, Shoemaker WC. Transcutaneous oxygen monitoring of critically ill adults with and without low flow shock. Crit Care Med 1981 ; 9: 706–9.
Tremper KK, Waxman K, Bowman R, Shoemaker WC. Continuous transcutaneous oxygen monitoring during respiratory failure, cardiac decompensation, cardiac arrest and CPR. Crit Care Med 1980; 8: 377–81.
Gothgen I, Jacobsen E, Rasmussen JP. Transcutaneous oxygen measurement during thoracic anaesthesia, Acta Anaesthesiol Scand 1980; 24: 491–4.
Chung M, Lichtor JL, Rangachari K. Transcutaneous monitoring of PO2 and PCO2 during one-lung anesthesia. Anesthesiology 1984; 61: A164.
Tremper KK, Konchigeri HN, Cullen BF, Kapur PA, Thangathurai D, Percival C. Transcutaneous monitoring of oxygen tension during one-lung anesthesia. J Thorac Cardiovasc Surg 1984; 88: 22–5.
Capan IM, Turndorf H, Patel C, Romanathan S, Acinapuro A, Chalon J. Optimization of arterial oxygenation during one-lung anesthesia. Anesth Analg 1980; 59: 847–51.
Temper KK. Transcutaneous PO2 measurement. Can Anaesth Soc J 1984; 31; 664–77.
Beran AV, Tolle CD, Huxtable RF. Cutaneous blood flow and its relationship to transcutaneous O2/CO2 measurements. Crit Care Med 1981; 9: 736–41.
Knill RL, Clement JL, Kieraszewicz HT, Dodgson BG. Assessment of two noninvasive monitors of arterial oxygenation in anesthetized man. Anesth Analg 1982; 61: 582–6.
Hutchinson DCS, Rocca G, Honeybourne O. Estimation of arterial oxygen tension in adult subjects using a transcutaneous electrode. Thorax 1981; 36: 473–7.
Kimmich HP, Kreuger F. Model of O2 transport through skin as basis for absolute transcutaneous measurement of PaO2. Acta Anaesthesiol Scan (Suppl) 1978; 68: 16–9.
Goeckenjan G, Strasser K. Relation of transcutaneous to arterial PO2 in hypoxemia, normoxemia and hyperoxemia. Biotetemetry 1977; 4: 77–87.
Thys DM, CohenE, Eisenkraft JB, Kaplan JA. Hemodynamic effects of one-lung anesthesia during thoracic surgery. Anesthesiology 1984; 61: A91.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Chubra-Smith, N.M., Grant, R.P. & Jenkins, L.C. Perioperative transcutaneous oxygen monitoring in thoracic anaesthesia. Can Anaesth Soc J 33, 745–753 (1986). https://doi.org/10.1007/BF03027125
Issue Date:
DOI: https://doi.org/10.1007/BF03027125