Abstract
Background
Although virtual reality (VR) simulators can be used ability to objectively assess skills in endoscopy, the evaluation is solely quantitative. We have developed a novel method for the objective assessment of technical skills in lower gastrointestinal (GI) endoscopy that incorporates qualitative as well as quantitative measures.
Methods
We developed a virtual endoscopy suite by deconstructing the VR simulator to enable a more realistic and ergonomic placement of the monitor. Trainee endoscopists with varying levels of experience performed the case 4 task of the simulator. Ten essential components of endoscopic performance were rated on a five-point Likert scale (global score) by three independent observers. These observers viewed two videos (one showing scope handling and the other showing the monitor image), which were synchronized and played simultaneously.
Results
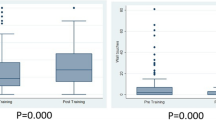
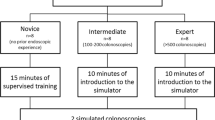
The study population comprised six experts (group 1, >200 procedures), seven subjects with intermediate experience (group 2, 20–80 procedures), and seven novices (group 3, 1–10 procedures). The global score was found to discriminate the level of skills across all three groups (p<0.001). There were significant differences between groups 1 and 2 (p=0.003) and groups 2 and 3 (p=0.004). There was a significant correlation between the global score and the percentage of red-out (without vision) as recorded by the simulator (correlation coefficients=−0.61,p=0.004).
Conclusion
This novel method for the assessment of technical skills in lower GI endoscopy has construct validity and high interrater reliability.
Similar content being viewed by others
References
Adams IJ, Ali Z, Shorthouse AJ (2001) Inadequacy of colonoscopy revealed by three-dimensional electromagnetic imaging. Dis Colon Rectum 44: 978–983
Bisschops R, Wilmer A, Tack J (2002) A survey of gastroenterology training in Europe. Gut 50: 724–729
Cass OW (1993) Objective evaluation of endoscopy skills during training. Ann Intern Med 118: 40–44
Cass OW (1999) Training to competence in gastrointestinal endoscopy: a plea for continuous measuring of objective end-points. Endoscopy 31: 751–754
Cass OW, Freeman ML, Cohen J, Zuckerman G, Watkins J, Nord J, Locke GR, Jensen D, Diehl D, Cerulli M, Lycke K, Fennerty M, Edmundowicz S, Etzkorn K, Al-Kawas F, Cave D, Lehman G (Aces study group) (1998) Acquisition of competency in endoscopy skills (ACES) during training: a multi-centre study [Abstract]. Gastrointest Endosc 43: 308
Colt HG, Crawford SW, Galbraith O (2001) Virtual reality bronchoscope simulation: a revolution in procedural training. Chest 120: 1333–1339
Cuschieri A, Francis N, Crosby J, Hanna GB (2001) What do master surgeons think of surgical competence and revalidation. Am J Surg 182: 110–116
Dafnis G, Granath F, Pahlman, Hannuksela H, Ekbom A, Blomqvist P (2001) The impact of endoscopists experience and learning curves and interendoscopist variation on colonoscopy completion rates. Endoscopy 33: 511–517
Datta V, Mackay S, Mandalia M, Darzi A (2001) The use of electromagnetic motion tracking analysis to objectively measure open surgical skill in the laboratory-based model. J Am Coll Surg 193: 479–485
Datta V, Mandalia M, Mackay S, Darzi A (2002) The PreOp Flexible Sigmoidoscopy Trainer: validation and early evaluation of a virtual reality based system. Surg Endosc 16: 1459–1463
Freeman ML (2001) Training and competence in gastrointestinal endoscopy. Rev Gastroenterol Disord 1: 73–86
Kneebone RL, Nestel D, Moorthy K, Taylor, P, Bann, S, Munz Y, Darzi A (2003) Learning the skills of flexible sigmoidoscopy—the wider perspective. Med Educ 37 (Suppl 1): 50–58
MacDonald J, Ketchum J, Williams RG, Rogers LQ (2003) A lay person versus a trained endoscopist. Surg Endosc 17: 896–898
Marshall JB (1995) Technical proficiency of trainees performing colonoscopy: a learning curve. Gastrointest Endosc 42: 287–291
Marshall JB, Brown DN (1996) Photodocumentation of total colonoscopy. How successful are endoscopists? Do reviewers agree? Gastrointest Endosc 44: 423–428
Martin JA, Regehr G, Reznick R, MacRae H, Murnaghan J, Hutchison C, Brown M (1997) Objective Structured Assessment of Technical Skill (OSATS) for surgical residents. Br J Surg 84: 273–278
Regehr G, MacRae H, Reznick RK, Szalay D (1998) Comparing the psychometric properties of checklists and global rating scales for assessing performance on an OSCE-format examination. Acad Med 73: 993–997
Sedlack RE, Kolars JC (2003) Validation of a computer-based colonoscopy simulator. Gastrointest Endosc 57: 214–218
Shah SG, Thomas-Gibson S, Brooker JC, Suzuki N, Williams CB, Thapar C, Saunders BP (2002) Use of video and magnetic endoscope imaging for rating competence at colonoscopy: validation of a measurement tool. Gastrointest Endosc 56: 568–573
Traverso LW (2002) Guidelines for granting of privileges for gastrointestinal endoscopy: focus on outcomes, not number of procedures performed. Surg Endosc 16: 229
Tuggy ML (1998) Virtual reality flexible sigmoidoscopy simulator training: impact on resident performance. J Am Board Fam Pract 11: 426–433
Wexner SD, Garbus JE, Singh JJ, the SAGES colonoscopy outcomes study group (2001) A prospective analysis of 13,580 colonoscopies: reevaluation of credentialing guidelines. Surg Endosc 15: 251–261
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Moorthy, K., Munz, Y., Orchard, T.R. et al. An innovative method for the assessment of skills in lower gastrointestinal endoscopy. Surg Endosc 18, 1613–1619 (2004). https://doi.org/10.1007/BF02637131
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02637131