Abstract
Objective:Patient-satisfaction surveys have been used frequently to assess the humanistic behaviors and skills of internal medicine housestaff. In conducting their first such survey, the authors found that many practical problems affected the progress and outcome of the project. This discussion of the authors’ experiences is intended to be helpful to others considering patient-satisfaction surveys as part of their housestaff-evaluation process.
Design:A description of the practical aspects of conducting a patient-satisfaction survey as well as the problems that the authors encountered.
Setting:Both inpatient and outpatient settings at a major university internal medicine residency program.
Patients/participants:Ambulatory and hospitalized patients under the care of categorical internal medicine interns were eligible for participation in the study.
Interventions:An established, validated patient-satisfaction questionnaire with high reported reliability was given to patients.
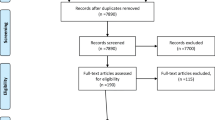
Measurements and main results:Although well over 90% of patients were willing to participate, 10% of participating outpatients and 16% of participating hospital patients could not provide a usable patient-satisfaction questionnaire even with assistance. Certain patient characteristics were responsible for these decreased completion rates. Among the hospitalized patients, 42% of all eligible patients were either too ill or too cognitively impaired to even be approached for participation in the study.
Conclusions:Patient-satisfaction surveys are labor-intensive, require significant resources, and are temporally demanding. Results from them must be viewed with certain caveats.
Similar content being viewed by others
References
Kisch AL, Reeder LG. Client evaluation of physician performance. J Health Soc Behav. 1969;10:51–8.
Woodward C, Gerrard B. Evaluation of the doctor-patient relationship. In: Neufeld VR, Norman CR, eds. Assessing clinical competence. New York: Springer Publishing, 1985;246–50.
Hulka BS, Zyzanski SJ. Validation of a patient satisfaction scale: Theory, methods and pracitce. Med Care. 1982;6:649–53.
Matthews DA, Sledge WH, Lieberman PB. Evaluation of intern performance by medical inpatients. Am J Med. 1987;83:938–44.
Linn LS, DiMatteo MR, Cope DW, Robbins A. Measuring physicians’ humanistic attitudes, values and behaviors. Med Care. 1987;25:504–15.
Burton RR, Mazzaferri EL. Assessment of interpersonal skills and humanistic qualities in medical residents. J Med Educ. 1985;60:648–50.
Cope DW, Linn LS, Leake BD, Barrett PA. Modification of residents’ behavior by preceptor feedback of patient satisfaction. J Gen Intern Med. 1986;1:394–8.
Linn LS. Interns’ attitudes and values as antecedents of clinical performance. J Med Educ. 1979;54:238–40.
Merrill JM, Boisaubin EV, Laux L, Lynch EC, Roessler R, Thronby JL. Measuring “humanism” in medical residents. South Med J. 1986;79(2):141–4.
Ware JE. Research methodology: How to survey patient satisfaction. Drug Intell Clin Pharm. 1981;15:892–9.
Ware JE, Hays RD. Methods for measuring patient satisfaction with specific medical encounters. Med Care. 1988;26:393–402.
Webster GD, and PSQ coinvestigators. Phase II of the ABIM patient satisfaction questionnaire project: Eighteen-month progress report. Philadelpha: American Board of Internal Medicine Committee on Research and Development, 1987.
Linn LS, Cope DW, Leake B. The effect of gender and training of residents on satisfaction ratings by patients. J Med Educ. 1984;59:964–6.
Comstock LM, Hooper EM, Goodwin JM. Physician behaviors that correlate with patient satisfaction. J Med Educ. 1982;57:105–12.
DeMatteo MR, DiNicola DD. Sources of assessment of physician performance: A study of comparative reliability and patterns of intercorrelation. Med Care. 1981;19:829–39.
Matthews DA, Feinstein AR. A new instrument for patients’ ratings of physician performance in the hospital setting. J Gen Intern Med. 1989;4:14–22.
Ware JE, Davies-Avery A, Steward AL. The measurement and meaning of patient satisfaction. Health Med Care Serv Rev. 1978;1:2–3.
Ware JE, Snyder MD, Wright WR. Development and validation of scales used to measure patient satisfaction: A review of the literature, overview of methods and results regarding construction of scales. Springfield, VA: National Technical Information Service, 1976.
Linn LS, Oye RK, Cope DW, DiMatteo MR. Use of nonphysician staff to evaluate humanistic behavior of internal medicine residents and faculty members. J Med Educ. 1986;51:918–20.
Lieberman PB, Sledge WH, Matthews DA. Effect of patient gender on evaluation of intern performance. Arch Intern Med. 1989;149:1825–9.
Parker SC, Hanusa BH, Kroboth FJ. Do interns care for inpatients differently than outpatients? Clin Res. 1990;38(2):741A.
Bigby JA, Pappius EM, Cook EF, Goldman L. Medical consequences of missed appointments. Arch Intern Med. 1984;144:1163–6.
Parker SC, Kroboth FJ, Parker RC, Hanusa BH, Kapoor WN. Development of an easily-completed and scored patient satisfaction questionnaire for both hospitalized and ambulatory care patients. Proceedings of the 12th annual meeting of the Society of General Internal Medicine, Washington, DC, 1989.
Kaufmann CL. Informed consent and patient decision making: Two decades of research. Soc Sci Med. 1983;17:1637–44.
Levinson W, Dunn P. Does a questionnaire show patient satisfaction [letter]? J Gen Intern Med. 1987;2:209.
American Board of Internal Medicine. Memo to directors of internal medicine residency programs: Evaluation of clinical competence. ABIM, 1986.
Arnold RM, Povar GJ, Hawell JD. The humanities, humanistic behavior and the humane physician. Ann Intern Med. 1987;106:313–8.
Author information
Authors and Affiliations
Additional information
Received from the Department of Medicine, Division of General Internal Medicine, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania.
Rights and permissions
About this article
Cite this article
Parker, S.C., Kroboth, F.J. Practical problems of conducting patient-satisfaction surveys. J Gen Intern Med 6, 430–435 (1991). https://doi.org/10.1007/BF02598165
Issue Date:
DOI: https://doi.org/10.1007/BF02598165