Summary
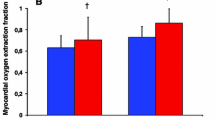
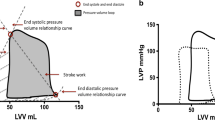
We tested the hypothesis that positive inotropic stimulation by isoproterenol alters the relationship between regional segment work and regional myocardial oxygen consumption. Regional parameters were compared with external cardiac work and global LV oxygen consumption. In anesthetized openchest dogs, regional myocardial segment length (ultrasonic dimension crystals) and force development (miniature force transducer) were measured. The integrated multiples of myocardial shortening by corresponding force during an averaged beat expressed segment work (area under the systolic portion of the length-force loop). External cardiac work was calculated from aortic blood pressure and cardiac output. Global and regional myocardial MVO2 were evaluated at baseline and during intravenous infusion of isoproterenol (0.5 and 1.0 μg/kg per min). Regional coronary blood flow was measured with radioactive microspheres, and microspectrophotometry of frozen myocardial biopsies was used to evaluate O2 saturation in small arteries and veins. These parameters were used to calculate regional MVO2. Arterial and coronary sinus O2 saturation was used to calculate global LV O2 consumption. Regional myocardial O2 balance was estimated by measurement of NADH redox level using surface fluorometry. It was found that 0.5 μg/kg per min isoproterenol increased regional segment work/minute from 4650±495 to 6750±750 mm·g/min. Corresponding regional oxygen consumption was disproportionately increased from 5.43±0.61 to 15.24±1.37 ml/min per 100 g. External cardiac work was found to decrease from 728±13 to 562±25 mmHg·1/min (due to decreased aortic blood pressure), whereas global myocardial O2 consumption increased. Regional myocardial O2 extraction and NADH fluorescence were elevated, indicating impaired tissue oxygenation. Regional MVO2 was increased by 153±56%, but regional work by only 45.3±33% (P<0.05). These results indicate that regional contraction efficiency was markedly reduced by isoproterenol.
Similar content being viewed by others
References
Acad B, Guggenheimer E, Sonn J, Kedem J (1983) Differential effects of inotropic agents on the intracellular NADH redox level in the in vivo dog heart. J Cardiovasc Pharmacol 5:284–290
Belloni FL, Sparks HV (1977) Dynamics of myocardial oxygen consumption and coronary vascular resistance. Am J Physiol 233:H34-H43
Berne RM (1964) Regulation of coronary blood flow. Physiol Rev 44:1–219
Boerth RC, Hammermeister KE, Warbasse JR (1978) Comparative influence of ouabain, norepinephrine and heart rate on myocardial oxygen consumption and inotropic state in dogs. Am Heart J 96:355–362
Braunwald E (1971) Control of myocardial oxygen consumption. Am J Cardiol 27:416–432
Buckberg GD, Luck JC, Payne DB, Archie JP, Fixler DE (1971) Some sources of error in measuring regional blood flow with radioactive microspheres. J Appl Physiol 31:598–604
Challoner DR, Steinberg D (1965) Metabolic effect of epinephrine on the QO2 of the arrested, isolated perfused rat heart. Nature 205:602–603
Feigl EO (1983) Coronary physiology. Physiol Rev 63:1–205
Grover GJ, Kostis JB, Weiss HR, Li JK, Kovacs T, Kedem J (1988) Effect of beta-adrenoceptor stimulation or blockade on regional myocardial function and regional O2 consumption during myocardial ischemia. Arch Int Pharmacodyn Ther 291:68–87
Hasenfuss G, Holubarsch C, Blanchard EM, Mulieri LA, Alpert NR, Just H (1989) Influence of isoproterenol on myocardial energetics. Experimental and clinical investigations. Basic Res Cardiol 84[Suppl 1]:147–155
Headrick J, Willis RJ (1989) Endogenous adenosine improves work rate to oxygen consumption ratio in catecholamine stimulated isovolumic rat heart. Pflugers Arch 413:354–358
Holubarsch C, Hasenfuss G, Blanchard E, Alpert NR, Mulieri LA, Just H (1986) Myothermal economy of rat myocardium chronic adaptation versus acute inotropism. Basic Res Cardiol 81[Suppl 1]:95–101
Holubarsch C, Hasenfuss G, Heiss HW, Meinertz T, Just H (1987) Acute and chronic changes of myocardial energetics in the mammalian and human heart. Basic Res Cardiol 82[Suppl 2]:377–388
Illes RW, Silverman NA, Krukenkamp IB, Levitsky S (1988) The conondrum of the effect of beta blockade on myocardial oxygen consumption. J Surg Res 44:336–341
Kedem J, Mayevsky A, Sonn J, Acad B (1981) An experimental approach for evaluation of the O2 balance in local myocardial regions in vivo. Q J Exp Physiol 66:501–514
Kedem J, Talafih K, Weiss HR (1985) Improvement in regional myocardial O2 supply and O2 consumption by nitroglycerin during ischemia. Eur J Pharmacol 112:47–56
Kedem J, Sonn J, Scheinowitz M, Weiss HR (1989b) Relationship between local oxygen consumption and local and external cardiac work: effect of tachycardia. Cardiovasc Res 23:1043–1052
Kedem J, Scholz PM, Weiss HR (1991) Augmented efficiency of regional myocardial work by ouabain. Cardiovasc Res 25:916–922
Kizakevich PN, McDermott J, Gollan F (1976) An automated system for systolic time interval analysis. Proc Dig Equip Users Soc 2:795–798
Krukenkamp IB, Silverman NA, Pridjian A, Levitsky S (1987) Correlation between the linearized Frank-Starling relationship and myocardial energetics in the ejecting heart. J Thorac Cardiovasc Surg 93:728–740
Le Winter MM, Kent RS, Kroener JM, Carew TB, Covell JW (1975) Regional differences in myocardial performance in the left ventricle of the dog. Circ Res 37:191–199
Metzenauer P, Dedecke R, Gobel H, Martorana PA, Stroman F, Szelenyi I (1989) Effects of the novel beta-adrenergic partial agonist alifedrine on cardia performance in dogs with acute ischemic left ventricular failure. J Cardiovasc Pharmacol 14:103–108
Opie LH (1986) Oxygen demand: ventricular function in the heart: physiology, metabolism, pharmacology and therapy. Grune and Stratton, London, pp 166–187
Opie LH, Thandroyen FT, Muller C, Bricknell OL (1979) Adrenaline-induced oxygen wastage and enzyme release from working rat heart-effects of calcium antagonism, beta blockade, nicotinic acid and coronary artery ligation. J Mol Cell Cardiol 11:1073–1094
Restorff WV, Holtz J, Bassenge E (1975) Exercise induced augmentation of myocardial oxygen extraction in spite of normal coronary dilatory capacity in dogs. Pflugers Arch 372: 181–185
Rooke GA, Feigl EO (1982) Work as a correlate of canine left ventricular oxygen consumption, and the problem of catecholamine oxygen wasting. Circ Res 50:273–286
Sarnoff SJ, Gilmore JP, Weisfeldt ML, Daggett WM, Mansfield PB (1965) Influence of norepinephrine on myocardial oxygen consumption under controlled conditions. Am J Cardiol 16:217–226
Sonn J, Acad B, Mayevsky A, Kedem J (1981) Effect of coronary vasodilation produced by hypopnea upon regional myocardial oxygen balance. Arch Int Physiol Biochim 89:445–456
Suga H, Hisano R, Hirata S, Hayashi T, Ninomiya I (1982) Mechanism of higher oxygen consumption rate: pressure-loaded versus volume-loaded heart. Am J Physiol 242:H942-H948
Suga H, Yamada O, Goto Y, Igarashi Y (1984) Oxygen consumption and pressure-volume area of abnormal contractions in canine heart. Am J Physiol 246:H154-H160
Vatner SF, Higgins CB, Franklin D (1972) Regional circulatory adjustments to moderate and severe chronic anemia in conscious dogs at rest and during exercise. Circ Res 30:731–740
Vinten-Johansen J, Barnard RJ, Buckberg GD, Becker H, Duncan HW, Robertson JM (1982) Left ventricular O2 requirements of pressure and volume loading in the normal canine heart and inaccuracy of pressure-derived indices of O2 demand. Cardiovasc Res 16:439–447
Weiss HR (1979) Regional oxygen consumption and supply in the dog heart-effect of atrial pacing. Am J Physiol 236:H231-H237
Weiss HR (1980) Effect of coronary artery occlusion on regional arterial and venous O2 saturation, O2 extraction, blood flow, and O2 consumption in the dog heart. Circ Res 47: 400–407
Weiss HR, Sinha AK (1978) Regional oxygen saturation of small arteries and veins in the canine myocardium. Circ Res 42:119–126
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kedem, J., Sonn, J., Scheinowitz, M. et al. Effect of isoproterenol on regional myocardial segment work, O2 consumption, and oxygen balance. Res. Exp. Med. 192, 323–334 (1992). https://doi.org/10.1007/BF02576289
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02576289