Abstract
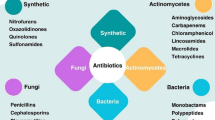
The interaction between microbial resistance and antibacterial agents occurs in a direct and an indirect fashion. Directly—through the development of resistance to the agent used, or to agents of the same class—as exemplified by the induction of β-lactamase by both grampositive and gram-negative bacteria. It also takes place through the development of resistance to compounds of different classes to the compound used, as exemplified by the loss ofStreptococcus pneumoniae susceptibility to penicillin that is accompanied by a parallel loss of sensitivity to erythromycin and to tetracycline. As for the indirect way—microbial resistance may develop through selection of resistant organisms when the patient is treated with antibiotics, when the environment is contaminated with antibiotics (hospital) or when antibacterial agents are used in agriculture and animal husbandry.
Similar content being viewed by others
References
Gerding, D. N., Larson, T. A., Hughes, R. A., Weiler, M., Shanholtzer, C., Peterson, L. R.: Aminoglycoside resistance and aminoglycoside usage: ten years experience in one hospital. Antimicrob. Agents Chemother. 35 (1991) 1284–1290.
Shimizu, K., Jumada, T., Hsieh, W. C., Chung, H. Y., Chong, Y., Hare, R. S., Miller, G. H., Sabatelli, F. J., Howard, J.: Comparison of aminoglycoside resistance patterns in Japan, Formosa, Korea, Chile and the US. Antimicrob. Agents Chemother. 28 (1985) 282–288.
Haley, R. W., Hightower, A. W., Khabbaz, R. F., Thornsberry, C., Martone, W. J., Allen, J. R., Hughes, J. M.: Emergence of methicillin resistantStaphylococcus aureus in United States hospitals. Ann. Intern. Med. 97 (1982) 297–311.
Vasquez, V., Calderon, E., Rodriguez, R.: Chloramphenicol-resistant strains ofSalmonella typhosa. N. Engl. J. Med. 286 (1972) 1220–1226.
Rao, P. S., Rajashekar, V., Varghese, G. K., Shivananda, P. G.: Emergence of multi drug resistantSalmonella typhi in rural southern India. Am. J. Trop. Med. Hyg. 48 (1993) 108–111.
Handsfield, H. H., Sandstrom, E. G., Knapp, J. S., Perrine, P. L., Whittington, W. L., Sayers, D. E., Holmes, K. K.: Epidemiology of penicillinase producingNeissera gonorrhoeae: analysis by autotyping and serogrouping. N. Engl. J. Med., 306 (1982) 950–954.
Knapp, J. S., Zenilman, J. M., Biddle, J. W., Perkins, G. H., DeWitt, W. E., Thomas, M. L., Johnson, S. R., Morse, J. A.: Frequency and distribution in the United States ofNeisseria gonorrhoeae with plasmid-mediated high-level resistance to tetracycline. J. Infect. Dis. 155 (1987) 819–822.
Fox, K. K., Knapp, J. S., Holmes, K. K., Hook, E. W. 3rd, Judson, F. N., Thompson, S. E., Washington, J. A., Whittington, W. L.: Antimicrobial resistance inNeisseria gonorrhoeae in the United States, 1988–1994: the emergence of decreased susceptibility to the fluoroquinolones. J. Infect. Dis. 175 (1987) 1396–1403.
Ejlertsen, T., Skov, R.: The beta- lactamases ofMoraxella (Branhamella) catarrhalis isolated from Danish children. APMIS 104 (1996) 557–562.
Guillemot, D., Carbon, C., Balkau, B., Geslin, P., Lecoeur, H., Vauzelle-Kervroedan, F., Bouvenot, G., Eschwege, E.: Low dosage and long treatment duration of beta lactam: risk factors for carriage of penicillin-resistantStreptococcus pneumoniae. JAMA 279 (1998) 365–370.
Arason, V. A., Kristianson, K. G., Sigurdsson, J. A., Stefansdottir, G., Molstad, S., Gudmunsson, S: Do antimicrobials increase the carriage rate of penicillin resistant pneumococci in children? Cross-sectional prevalence study. BMJ 313 (1996) 387.
Huovinen, P., Seppala, H., Kataja, J., Klaukka, T.: The relationship between erythromycin consumption and resistance in Finland. Finnish study group for antimicrobial resistance. Ciba Found. Symp. 207 (1997) 36–41.
Seppala, H., Klaukka, T., Vuopio-Varkila, J., Muotiala, A., Helenius, H., Lager, K., Huovinen, P.: The effect of changes in the consumption of macrolide antibiotics on erythromycin resistance in group A streptococci in Finland. Finnish study group for antimicrobial resistance. N. Engl. J. Med. 377 (1997) 441–446.
Austin, D. J., Kristianson, K. G., Anderson, R. M.: The relationship between the volume of antimicrobial consumption in human communities and the frequency of resistance. Proc. Natl. Acad. Sci. USA 96 (1999) 1152–1156.
Martinez, E., de la Cruz, F.: Genetic elements involved in Tn21 sitespecific integration, a novel mechanism for the dissemination of antibiotic resistance genes. EMBO J. 9 (1990) 1275–1281.
Gould, L. M.: A review of the role of antibiotic policies in the control of antibiotic resistance. J. Antimicrob. Chemother. 43 (1999) 359–365.
Shulman, J. A., Terry, P. M., Hough, C. E.: Colonization with gentamicin resistantPseudomonas aeruginosa, pyocine type 5, in a burn unit. J. Infect. Dis. 124 (1971) 18–23.
Ridley, M., Lynn, R., Barrie, D., Stead, K. C.: Antibiotic resistance ofStaphylococcus aureus and hospital antibiotic policies. Lancet i (1970) 230–233.
Barber, M., Dutton, A. A. C., Beard, M. A., Elmes, P. C., Williams, R.: Reversal of antibiotic resistance in hospital staphylococcal infections. BMJ 1 (1960) 11–17.
Bulger, R. J., Sherris, J. C.: Decreased incidence of antibiotic resistance amongStaphylococcus aureus: a study in a university hospital over a nine year period. Ann. Intern. Med. 69 (1968) 1099–1108.
Meyer, K. S., Urban, C., Eagan, J. A., Beger, B. J., Rahal, J. J.: Nosocomial outbreak ofKlebsiella infection resistant to late generation cephalosporins. Ann. Intern. Med. 119 (1993) 353–358.
Rahal, J. J., Urban, C., Horn, D., Freeman, K., Segal-Maurer, A. S., Maurer, J. et al.: Class restriction of cephalosporins use to control total cephalosporin resistance in nosocomialKlebsiella. JAMA 280 (1998) 1233–1237.
Levy, S. B.: Balancing the drug-resistant, equation. Trends Microbiol. 2 (1994) 341–432.
Archibald, I., Phillips, L., Monnet, D., McGowan, J. E., Tenover, F., Gaynes, R.: Antimicrobial resistance in isolates from inpatients and outpatients in the United States: increasing importance of the intensive care unit. Clin. Infect. Dis. 24 (1997) 211–215.
Lipsitch, M., Levin, B. K.: The population dynamics of antimicrobial chemotherapy. Antimicrob. Agents Chemother. 41 (1997) 363–373.
Schentag, J. J., Birmingham, M. C., Paladino, J. A.: In nosocomial pneumonia, optimizing antibiotics other than aminoglycosides is a more important determinant of successful clinical outcome, and a better means of avoiding resistance. Semin. Respir. Infect. 12 (1997) 279–283.
Schentag, J. J., Strenkoski-Nix, L. C., Nix, D. E., Forrest, A.: Pharmacodynamic interactions of antibiotics alone and in combinations. Clin. Infect. Dis. 27 (1998) 40–46.
Lode, H., Borner, K., Gilbert, B., Gordts, B., Verbuggen, A. M.: Surveillance of aminoglycoside resistance: European data. Am. J. Med. 80 (Suppl. 6B) (1986) 76–81.
Moody, M. M., De Jongh, C. A., Schimpf, S. C., Tillman, G. L.: Long term amikacin use. Effects on aminoglycoside susceptibility patterns of gram-negative bacilli. JAMA 248 (1982) 1199–1202.
Katzenstein, D.: Combination therapies for HIV infection and genomic drug resistance. Lancet 350 (1997) 970–971.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rubinstein, E. Antimicrobial resistance—Pharmacological solutions. Infection 27 (Suppl 2), S32–S34 (1999). https://doi.org/10.1007/BF02561668
Issue Date:
DOI: https://doi.org/10.1007/BF02561668