Abstract
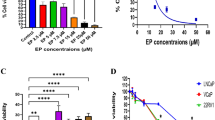
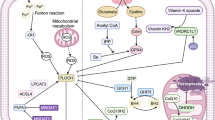
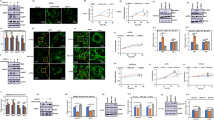
Berberine has drawn extensive attention toward their wide range of biochemical and pharmacological effects, including antineoplastic effect in recent years, but the precise mechanisms remain unclear. Treatment of human breast cancer cells (MCF-7 and MDA-MB-231 cells) with berberine induced inhibition of cell viability in concentration- and time-dependent manner irrespective of their estrogen receptor (ER) expression. Hoechst33342 staining confirmed berberine induced breast cancer cell apoptosis in time-dependent manner. Because apoptosis induction is considered to be a crucial strategy for cancer prevention and therapy, berberine may be an effective chemotherapeutic agent against breast cancer. To explore the precise mechanism, berberine-induced oxidative stress and mitochondrial-related apoptotic pathway in human breast cancer cells were investigated in this study. In both MCF-7 and MDA-MB-231 cells, berberine increased the production of reactive oxygen species (ROS), which activated the pro-apoptotic JNK signaling. Phosphorylated JNK triggered mitochondria membrane potential (ΔΨm) depolarization and downregulation expression of anti-apoptotic protein Bcl-2 concomitant with the upregulation expression of pro-apoptotic protein Bax. Downregulation of anti-apoptotic Bcl-2 family protein in parallel with loss of ΔΨm, leading to increased the release of cytochrome c and apoptosis-inducing factor (AIF) from mitochondria, and eventually triggered the caspase-dependent and caspase-independent apoptosis. Taken together, our study reveled that berberine exerted an antitumor activity in breast cancer cells by reactive oxygen species generation and mitochondrial-related apoptotic pathway. These finding provide an insight into the potential of berberine for breast cancer therapy.









Similar content being viewed by others
References
Basu S, Nachat-Kappes R, Caldefie-Chezet F, Vasson MP. Eicosanoids and adipokines in breast cancer: from molecular mechanisms to clinical considerations. Antioxid Redox Signal. 2013;18:323–60.
Bray F, Jemal A, Grey N, Ferlay J, Forman D. Global cancer transitions according to the Human Development Index (2008–2030): a population-based study. Lancet Oncol. 2012;13:790–801.
Kim K, Zang R, Choi SC, Ryu SY, Kim JW. Current status of gynecological cancer in China. J Gynecol Oncol. 2009;20:72–6.
Jiang X. Harnessing the immune system for the treatment of breast cancer. J Zhejiang Univ Sci B. 2014;15:1–15.
Imanshahidi M, Hosseinzadeh H. Pharmacological and therapeutic effects of Berberis vulgaris and its active constituent, berberine. Phytother Res. 2008;22:999–1012.
Singhal KC. Anthelmintic activity of berberine hydrochloride against Syphacia obvelata in mice. Indian J Exp Biol. 1976;14:345–7.
Satou T, Akao N, Matsuhashi R, Koike K, Fujita K, Nikaido T. Inhibitory effect of isoquinoline alkaloids on movement of second-stage larvae of Toxocara canis. Biol Pharm Bull. 2002;25:1651–4.
Kuo CL, Chi CW, Liu TY. The anti-inflammatory potential of berberine in vitro and in vivo. Cancer Lett. 2004;203:127–37.
Tang J, Feng Y, Tsao S, Wang N, Curtain R, Wang Y. Berberine and Coptidis rhizoma as novel antineoplastic agents: a review of traditional use and biomedical investigations. J Ethnopharmacol. 2009;126:5–17.
Trentham-Dietz A. Epidemiologic breast cancer research at the UW-Madison: a summary of past accomplishments and future directions. Wmj. 2009;108:284–5.
Lowe SW, Lin AW. Apoptosis in cancer. Carcinogenesis. 2000;21:485–95.
Formentini L, Sanchez-Arago M, Sanchez-Cenizo L, Cuezva JM. The mitochondrial ATPase inhibitory factor 1 triggers a ROS-mediated retrograde prosurvival and proliferative response. Mol Cell. 2012;45:731–42.
Gnocchi D, Leoni S, Incerpi S, Bruscalupi G. 3,5,3'-triiodothyronine (T3) stimulates cell proliferation through the activation of the PI3K/Akt pathway and reactive oxygen species (ROS) production in chick embryo hepatocytes. Steroids. 2012;77:589–95.
Lenaz G. Mitochondria and reactive oxygen species. Which role in physiology and pathology? Adv Exp Med Biol. 2012;942:93–136.
Kuo PL, Chen CY, Hsu YL. Isoobtusilactone A induces cell cycle arrest and apoptosis through reactive oxygen species/apoptosis signal-regulating kinase 1 signaling pathway in human breast cancer cells. Cancer Res. 2007;67:7406–20.
Cossarizza A, Baccarani-Contri M, Kalashnikova G, Franceschi C. A new method for the cytofluorimetric analysis of mitochondrial membrane potential using the J-aggregate forming lipophilic cation 5,5',6,6'-tetrachloro-1,1',3,3'-tetraethylbenzimidazolcarbocyanine iodide (JC-1). Biochem Biophys Res Commun. 1993;197:40–5.
Kamata H, Honda S, Maeda S, Chang L, Hirata H, Karin M. Reactive oxygen species promote TNFalpha-induced death and sustained JNK activation by inhibiting MAP kinase phosphatases. Cell. 2005;120:649–61.
Nakano H, Nakajima A, Sakon-Komazawa S, Piao JH, Xue X, Okumura K. Reactive oxygen species mediate crosstalk between NF-kappaB and JNK. Cell Death Differ. 2006;13:730–7.
Antosiewicz J, Herman-Antosiewicz A, Marynowski SW, Singh SV. c-Jun NH(2)-terminal kinase signaling axis regulates diallyl trisulfide-induced generation of reactive oxygen species and cell cycle arrest in human prostate cancer cells. Cancer Res. 2006;66:5379–86.
Chandra J, Samali A, Orrenius S. Triggering and modulation of apoptosis by oxidative stress. Free Radic Biol Med. 2000;29:323–33.
Tillhon M, Guaman Ortiz LM, Lombardi P, Scovassi AI. Berberine: new perspectives for old remedies. Biochem Pharmacol. 2012;84:1260–7.
Jacobson MD. Reactive oxygen species and programmed cell death. Trends Biochem Sci. 1996;21:83–6.
Camhi SL, Lee P, Choi AM. The oxidative stress response. New Horiz. 1995;3:170–82.
Carmody RJ, Cotter TG. Signalling apoptosis: a radical approach. Redox Rep. 2001;6:77–90.
Pelicano H, Carney D, Huang P. ROS stress in cancer cells and therapeutic implications. Drug Resist Updat. 2004;7:97–110.
Selimovic D, Hassan M, Haikel Y, Hengge UR. Taxol-induced mitochondrial stress in melanoma cells is mediated by activation of c-Jun N-terminal kinase (JNK) and p38 pathways via uncoupling protein 2. Cell Signal. 2008;20:311–22.
Barreto MC, Pinto RE, Arrabaca JD, Pavao ML. Inhibition of mouse liver respiration by Chelidonium majus isoquinoline alkaloids. Toxicol Lett. 2003;146:37–47.
Hotchkiss RS, Coopersmith CM, Karl IE. Prevention of lymphocyte apoptosis—a potential treatment of sepsis? Clin Infect Dis. 2005;41 Suppl 7:S465–9.
Takahashi A, Masuda A, Sun M, Centonze VE, Herman B. Oxidative stress-induced apoptosis is associated with alterations in mitochondrial caspase activity and Bcl-2-dependent alterations in mitochondrial pH (pHm). Brain Res Bull. 2004;62:497–504.
Ajenjo N, Canon E, Sanchez-Perez I, Matallanas D, Leon J, Perona R, et al. Subcellular localization determines the protective effects of activated ERK2 against distinct apoptogenic stimuli in myeloid leukemia cells. J Biol Chem. 2004;279:32813–23.
Szegezdi E, Logue SE, Gorman AM, Samali A. Mediators of endoplasmic reticulum stress-induced apoptosis. EMBO Rep. 2006;7:880–5.
Wang X. The expanding role of mitochondria in apoptosis. Genes Dev. 2001;15:2922–33.
Saelens X, Festjens N, Vande Walle L, van Gurp M, van Loo G, Vandenabeele P. Toxic proteins released from mitochondria in cell death. Oncogene. 2004;23:2861–74.
Acknowledgments
This work was supported by grants from the Nanjing Medical Science and Technique Development Foundation, Nanjing, Jiangsu, China (Grant No.QYK10156), and the natural science foundation of Jiangsu Province (Grant No.BK20130073). We thank Pro. Sun Y (Key Laboratory of Human Functional Genomics of Jiangsu Province, Nanjing Medical University, Nanjing, People’s Republic of China) for providing MCF-7 and MDA-MB-231 breast cancer cell lines.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding authors
Additional information
Juan Xie and Yinyan Xu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Xie, J., Xu, Y., Huang, X. et al. Berberine-induced apoptosis in human breast cancer cells is mediated by reactive oxygen species generation and mitochondrial-related apoptotic pathway. Tumor Biol. 36, 1279–1288 (2015). https://doi.org/10.1007/s13277-014-2754-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-014-2754-7