Abstract
Summary
This study explores the effect of supervised back extensor strength training on spinal pain, back extensor muscle strength, trunk-arm endurance, kyphosis, functional mobility, and quality of life (QoL) among sixty postmenopausal women with vertebral osteoporotic fractures.
Purpose
To compare the effects of a 6-week supervised or home-based program of back-strengthening exercise on spinal pain, back extensor strength, trunk-arm endurance, kyphosis, functional mobility, and QoL in osteoporotic postmenopausal women with vertebral fractures.
Methods
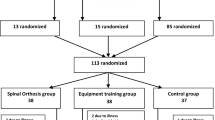
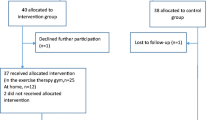
The study was designed as a randomized controlled clinical trial. Sixty osteoporotic postmenopausal women with vertebral fracture (mean age 60.3 ± 9.3 years) were included in the study. Subjects were randomly assigned into three groups (supervised program, home-based program, or control), each consisting of 20 subjects. The subjects underwent the 6-week exercise program which included strengthening exercise for the back extensor muscles. They performed three sets of 8, 10, or 12 repetitions for each of the exercises, biweekly ascending, three times per week. Spinal pain, back extensor strength, trunk and arm endurance, kyphosis, functional mobility, and QoL were measured at baseline and at the end of the exercise program.
Results
Statistically significant improvements were demonstrated on spinal pain, muscle strength and endurance, functional mobility, and QoL for the supervised exercise program compared with control and home-based exercise groups (p < 0.01). Home-based exercise program did not provide a significant improvement compared with the control group except for mobility parameters of QoL.
Conclusions
Six-week supervised back extensor strengthening training is superior to home-based program in terms of spinal pain, back extensor muscle strength, trunk endurance, functional mobility, and QoL for postmenopausal osteoporotic women with vertebral fractures.

Similar content being viewed by others
References
NIH Consensus Development Panel (2001) On osteoporosis prevention, diagnosis, and therapy. Osteoporosis prevention, diagnosis, and therapy. JAMA 285(6):785–795
Szulc P, Bouxsein ML (2011) Overview of osteoporosis: epidemiology and clinical management. Vertebral fracture initiative resource document. International Osteoporosis Foundation; Part I, Nyon, pp 1–65
Dusdal K, Grundmanis J, Luttin K, Ritchie P, Rompre C, Sidhu R, Harris SR (2011) Effects of therapeutic exercise for persons with osteoporotic vertebral fractures: a systematic review. Osteoporos Int 22(3):755–769
Evstigneeva L, Lesnyak O, Bultink IE, Lems WF, Kozhemyakina E, Negodaeva E et al (2016) Effect of twelve-month physical exercise program on patients with osteoporotic vertebral fractures: a randomized, controlled trial. Osteoporos Int 27(8):2515–2524
Kasch R, Merk H, Pinto RZ (2015) Exercise prescription for people with osteoporotic vertebral fracture. Br J Sports Med 49(7):489–490
Liu T, Sheng L, Huang Z (2017) Influence of exercise intervention on pain, quality of life and functional mobility in patients with osteoporotic vertebral fractures: a systematic review and meta-analysis. Int J Clin Exp Med 10(7):9864–9870
World Health Organization (WHO) (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: report of a WHO study group. WHO Technical Report Series, Report No. 843. WHO, Geneva, Switzerland
Genant HK, Wu CY, van Kuijk C, Nevitt MC (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8:1137–1148
Valentin G, Maribo T (2014) Hand-held dynamometry fixated with a tripod is reliable for assessment of back extensor strength in women with osteoporosis. Osteoporos Int 25(8):2143–2149
Shipp KM, Purse JL, Gold DT, Pieper CF, Sloane R, Schenkman M, Lyles KW (2000) Timed loaded standing: a measure of combined trunk and arm endurance suitable for people with vertebral osteoporosis. Osteoporos Int 11(11):914–922
Podsiadlo D, Richardson S (1991) The timed "Up & Go": a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc 39(2):142–148
Koçyigit H, Gülseren S, Erol A, Hizli N, Memis A (2003) The reliability and validity of the Turkish version of Quality of Life Questionnaire of the European Foundation for Osteoporosis (QUALEFFO). Clin Rheumatol 22(1):18–23
Francis RM, Aspray TJ, Hide G, Sutcliffe AM, Wilkinson P (2008) Back pain in osteoporotic vertebral fractures. Osteoporos Int 19(7):895–903
Paolucci T, Giovanni M, Iosa M, Grasso MR, Buzi E, et a ZF (2014) Efficacy of group-adapted physical exercises in reducing back pain in women with postmenopausal osteoporosis. Aging Clin Exp Res 26:395–402
Bergström I, Bergström K, Kronhed ACG, Karlsson S, Brinck J (2011) Back extensor training increases muscle strength in postmenopausal women with osteoporosis, kyphosis and vertebral fractures. Adv Physiother 13(3):110–117
Malmros B, Mortensen L, Jensen MB, Charles P (1998) Positive effects of physiotherapy on chronic pain and performance in osteoporosis. Osteoporos Int 8(3):215–221
Gold DT, Shipp KM, Pieper CF, Duncan PW, Martinez S, Lyles KW (2004) Group treatment improves trunk strength and psychological status in older women with vertebral fractures:results of a randomized, clinical trial. J Am Geriatr Soc 52(9):1471–1478
Yang L, He C, Lei Z, Xie W, Lan Q (2007) Effect of pain-free exercises on female osteoporosis patients with spinal compressive fracture. J Clin Rehab Tis Eng Res 11:9108–9111
Papaioannou A, Adachi JD, Winegard K, Ferko N, Parkinson W, Cook RJ, Webber C, McCartney N (2003) Efficacy of home-based exercise for improving quality of life among elderly women with symptomatic osteoporosis-related vertebral fractures. Osteoporos Int 14:677–682
Bennell KL, Matthews B, Greig A, Briggs A, Kelly A, Sherburn M, Larsen J, Wark J (2010) Effects of an exercise and manual therapy program on physical impairments, function and quality of life in people with osteoporotic vertebral fracture: a randomized, single-blind controlled pilot trial. BMC Musculoskelet Disord 11:36
Hongo M, Itoi E, Sinaki M, Miyakoshi N, Shimada Y, Maekawa S et al (2007) Effect of low-intensity back exercise on quality of life and back extensor strength in patients with osteoporosis: a randomized controlled trial. Osteoporos Int 18(10):1389–1395
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The Regional Ethics Committee for Medical Research approved the study, and the subjects gave their written informed consent to participate in the study.
Conflict of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Çergel, Y., Topuz, O., Alkan, H. et al. The effects of short-term back extensor strength training in postmenopausal osteoporotic women with vertebral fractures: comparison of supervised and home exercise program. Arch Osteoporos 14, 82 (2019). https://doi.org/10.1007/s11657-019-0632-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-019-0632-z