Abstract
Background
Low back muscles exercise reportedly influence the risk of osteoporotic vertebral fractures. The exact relationship between the low back muscles exercise and the incidence of vertebral refractures remain unclear.
Objective
To investigate the ability of exercise to strengthen the low back muscles to prevent vertebral refracture after surgery, through clinical analysis of the vertebral fracture risk reduction program.
Methods
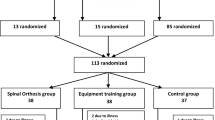
In total 152 patients with vertebral fractures who had undergone percutaneous vertebroplasty (PVP) and anti-osteoporosis treatment were randomly divided into observation and control groups. The observation group performed exercises to strengthen the back muscles after surgery. The clinical efficacy and incidence of re-fractures were compared between groups.
Results
The observation group had reduced physical dysfunction and pain following surgery. After 3 months, the vertebral body height had significantly decreased (P < 0.05) in the control group but not in the observation group (P > 0.05). In the observation and control groups, the incidence of vertebral refractures was 9.2% (7/76) and 17.1% (13/76), respectively (P < 0.05).
Conclusion
Postoperative exercise to strengthen the back muscles can improve physical function, relieve pain and promote the recovery of vertebral height; it can also assist in maintaining bone density, thereby significantly reducing the risk of refracture. This approach is safe and effective and can help improve the quality of life in patients with vertebral fractures.
Zusammenfassung
Hintergrund
Übungen zur Stärkung der unteren Rückenmuskulatur beeinflussen angeblich das Risiko osteoporotischer Wirbelkörperfrakturen. Die genaue Beziehung zwischen den Übungen für die untere Rückenmuskulatur und die Inzidenz von Wirbelkörperfrakturen bleibt unklar.
Ziel
Mittels einer klinischen Analyse des Programms zur Reduzierung des Risikos von Wirbelkörperfrakturen wird untersucht, inwieweit Übungen die untere Rückenmuskulatur stärken können, um eine erneute Fraktur der Wirbelkörper nach einer Operation zu verhindern.
Methoden
Insgesamt 152 Patienten mit Wirbelkörperfrakturen, die eine perkutane Vertebroplastik (PV) und eine Osteoporosetherapie erhielten, wurden in eine Beobachtungsgruppe und eine Kontrollgruppe randomisiert. Die Beobachtungsgruppe führte nach der Operation Übungen zur Stärkung der Rückenmuskulatur aus. Die klinische Wirksamkeit und Inzidenz von Wirbelkörperfrakturen wurden zwischen beiden Gruppen verglichen.
Ergebnisse
Die Beobachtungsgruppe zeigte eine reduzierte körperliche Dysfunktion und weniger Schmerzen nach der Operation. Nach 3 Monaten hatte sich die Wirbelkörperhöhe in der Kontrollgruppe signifikant verringert (p < 0,05), nicht aber in der Beobachtungsgruppe (p > 0,05). In der Beobachtung- und Kontrollgruppe betrug die Inzidenz erneuter Wirbelkörperfrakturen 9,2 % (7/76) bzw. 17,1 % (13/76; p < 0,05).
Schlussfolgerung
Postoperative Übungen zur Stärkung der Rückenmuskulatur können die körperliche Funktion verbessern, Schmerzen lindern und die Heilung der Wirbelkörperhöhe unterstützen. Sie können auch bei der Erhaltung der Knochendichte helfen und damit das Risiko einer Refraktur signifikant senken. Es handelt sich hierbei um ein sicheres und wirksames Verfahren, das zur Verbesserung der Lebensqualität bei Patienten mit Wirbelkörperfrakturen beitragen kann.

Similar content being viewed by others
Abbreviations
- BMD:
-
Bone mineral density
- ECG:
-
Electrocardiograph
- ODI:
-
Oswestry disability index
- PVP:
-
Percutaneous vertebroplasty
- SD:
-
Standard deviation
- VAS:
-
Visual analog scale
References
Nieuwenhuijse MJ, Putter H, van Erkel AR, Dijkstra PD (2013) New vertebral fractures after percutaneous vertebroplasty for painful osteoporotic vertebral compression fractures: a clustered analysis and the relevance of intradiskal cement leakage. Radiology 266:862–870
Kim YJ, Lee JW, Park KW, Yeom JS, Jeong HS, Park JM et al (2009) Pulmonary cement embolism after percutaneous vertebroplasty in osteoporotic vertebral compression fractures: incidence, characteristics, and risk factors. Radiology 251:250–259
Zielinski KA, Henry SM, Ouellette-Morton RH, DeSarno MJ (2013) Lumbar multifidus muscle thickness does not predict patients with low back pain who improve with trunk stabilization exercises. Arch Phys Med Rehabil 94:1132–1138
Prioreschi A, Tikly M, McVeigh JA (2014) A three month controlled intervention of intermittent whole body vibration designed to improve functional ability and attenuate bone loss in patients with rheumatoid arthritis. BMC Musculoskelet Disord 15:403
Levy HP (1993) Ehlers-Danlos syndrome, hypermobility type. In: Pagon RA, Adam MP, Ardinger HH, Wallace SE, Amemiya A, Bean LJH et al (eds) GeneReviews (R). University of Washington, Seattle
Sinaki M (2013) Yoga spinal flexion positions and vertebral compression fracture in osteopenia or osteoporosis of spine: case series. Pain Pract 13:68–75
Burns JE, Yao J, Munoz H, Summers RM (2016) Automated detection, localization, and classification of traumatic vertebral body fractures in the thoracic and lumbar spine at CT. Radiology 278:64–73
Lin H, Bao LH, Zhu XF, Qian C, Chen X, Han ZB (2010) Analysis of recurrent fracture of a new vertebral body after percutaneous vertebroplasty in patients with osteoporosis. Orthopaed Surg 2:119–123
Van Meirhaeghe J, Bastian L, Boonen S, Ranstam J, Tillman JB, Wardlaw D (2013) A randomized trial of balloon kyphoplasty and nonsurgical management for treating acute vertebral compression fractures: vertebral body kyphosis correction and surgical parameters. Spine 38:971–983
Frankel B, Krishna V, Vandergrift A, Bauer DC, Nicholas J (2013) Natural history and risk factors for adjacent vertebral fractures in the fracture intervention trial. Spine 38:2201–2207
Eck JC, Sharan A, Ghogawala Z, Resnick DK, Watters WC 3rd, Mummaneni PV et al (2014) Guideline update for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 7: lumbar fusion for intractable low-back pain without stenosis or spondylolisthesis. J Neurosurg Spine 21:42–47
Katzman WB, Huang MH, Lane NE, Ensrud KE, Kado DM (2013) Kyphosis and decline in physical function over 15 years in older community-dwelling women: the study of osteoporotic fractures. J Gerontol A Biol Sci Med Sci 68:976–978
Acknowledgements
We thank our co-workers in the University of The Second Affiliated Hospital, Shantou University Medical College, and Central Hospital of Panyu District for their invaluable technical help and we would like to thank Editage [www.editage.cn] for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
D. Deng, Z. Lian, W. Cui, H. Liang, L. Xiao and G. Yao declare that they have no competing interests.
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
DeLi Deng and Zhen Lian contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Deng, D., Lian, Z., Cui, W. et al. Function of low back muscle exercise. Orthopäde 48, 337–342 (2019). https://doi.org/10.1007/s00132-018-3577-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00132-018-3577-9