Abstract
Hyperactive platelets, in addition to their roles in thrombosis, are also important mediators of atherogenesis. Antiplatelet drugs are not suitable for use where risk of a cardiovascular event is relatively low. It is therefore important to find alternative safe antiplatelet inhibitors for the vulnerable population who has hyperactive platelets in order to reduce the risk of cardiovascular disease. Potent antiplatelet factors were identified in water-soluble tomato extract (Fruitflow®), which significantly inhibited platelet aggregation. Human volunteer studies demonstrated the potency and bioavailability of active compounds in Fruitflow®. Fruitflow® became the first product in Europe to obtain an approved, proprietary health claim under Article 13(5) of the European Health Claims Regulation 1924/2006 on nutrition and health claims made on foods. Fruitflow® is now commercially available in different countries worldwide. In addition to its reduction in platelet reactivity, Fruitflow® contains anti-angiotensin-converting enzyme and anti-inflammatory factors, making it an effective and natural cardio-protective functional food.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
During the last 50 years, tomato (Lycopersicon esculentum) has become a highly consumed healthy food [1]. Tomato contains several components that are beneficial to overall health, including vitamin E, flavonoids, phytosterols, carotenoids, several water-soluble vitamins and minerals [2]. The presence of a variety of antioxidants such as polyphenols, e.g. quercetin, kaempferol, naringenin, and carotenoids, in considerable amounts makes tomato a rich source of antioxidants [3, 4]. Since oxidative stress triggers inflammatory disorders, the basis for the development of several diseases such as immune disorders, atherosclerotic lesions and rupture of plaque [5], antioxidants present in tomato are therefore believed to slow the progression of many diseases including cardiovascular disease (CVD). In order for tomato to provide cardio-protection, it must include bioactive factors that are able to reduce several cardiovascular risk factors such as LDL cholesterol, triglycerides, homocysteine, platelet hyperactivity and blood pressure [6].
Platelets play an important role in CVD both in the pathogenesis of atherosclerosis and in the development of acute thrombotic events (Fig. 1). Their importance in CVD is indirectly confirmed by the benefit of antiplatelet agents such as aspirin, clopidogrel and glycoprotein IIb/IIIa inhibitors abciximab/eptifibatide [7]. In fact, intravascular thrombosis is a factor in the generation of a wide variety of CVDs. Platelets in individuals with diabetes, sedentary lifestyle, obesity and insulin resistance show increased activity at baseline and in response to agonists, ultimately leading to increased aggregation and plaque development [8–10]. Aspirin remains a cornerstone of antiplatelet therapy but does not benefit all patients equally, as evidenced by the phenomenon of aspirin resistance [7]. Aspirin therapy is also responsible for a number of serious side effects, rendering it unsuitable for use in primary prevention of CVD [11, 12]. However, very few new antithrombotics are currently progressing beyond phase II trials, and those that have been developed are similarly unsuitable for use in primary prevention [12]. There is an interest in naturally occurring compounds which might lack the side effects currently so prevalent. We therefore systematically investigated the effects of bioactive compounds in fruits and vegetables on human blood platelet aggregation and utilized the findings to characterize the mechanisms involved in this process, in the hope of identifying potential dietary antiplatelet components. In a variety of studies, it was demonstrated that water-soluble components of tomatoes are capable of inhibiting platelet aggregation both in vitro and in vivo [13–16]. These water-soluble tomato components were also found to inhibit angiotensin-converting enzyme (ACE) and to relax the vascular endothelium, the other important limbs of the cardiovascular system [17, 18]. A water-soluble tomato extract containing all the bioactive components was developed and later given the trade name Fruitflow®. Fruitflow® is now an established naturally derived functional food ingredient, marketed globally. Since its discovery in 1999, several mechanistic studies and human trials with Fruitflow® have been carried out. Studies included localization of the antiplatelet activity within the tomato fruit, its modes of action, its stability under various conditions and identification of the compounds with antiplatelet activity. The presence of a range of compounds suggested that all have antiplatelet activity but act on different parts of the platelet activation/aggregation pathway. The chemical properties of the active compounds indicated their potential suitability as therapeutic agents or as functional food ingredients. There are several excellent reviews available on overall health benefits of tomatoes [1, 2, 4, 5, 19, 20]. This review will discuss the background to Fruitflow® discovery and the body of biological and regulatory work involved in the granting of its authorized health claim in Europe and acceptance as a functional food by regulatory authorities worldwide.
Hyperactivity of platelets and impact on health. Platelets play an important role in CVD both in the pathogenesis of atherosclerosis and in the development of acute thrombotic events. Hyperactive platelets are involved in the development of atherosclerosis by different mechanisms such as membrane shedding, growth factor secretion and expression of several adhesive factors. In addition, hyperactive platelets are involved in the well-known penultimate thrombotic events
Epidemiology of tomato consumption and CVD risk reduction
Epidemiologic studies focused on tomato and tomato products associated their intake with a reduced risk of CVD [19, 21, 22]. However, tomatoes and tomato-based products are important dietary sources of lycopene in observational studies, and most human lycopene trials are performed using tomato-based interventions. Studies showed that increased plasma lycopene levels were associated with reductions in CVD risk factors [23–25]. The strongest population-based evidence for the beneficial effects of tomato lycopene came from a multi-centre case–control study [26]. However, a subsequent dietary intervention study observed that consumption of a carotenoid-rich diet did not have an effect on plasma antioxidant status or markers of oxidative stress [27]. Several [25, 28], but not all [28–32] prospective studies relating circulating lycopene concentrations and CVD risk have reported inverse associations, while studies based on dietary intake did not find any such significant associations [32–36]. Also, the focus on lycopene in tomatoes cannot explain the fact that, taking tomato consumption into account, individuals in the Mediterranean area have a lower risk of CVD when compared to their North American and other European counterparts [2, 37, 38]. Thus, it is difficult to separate out the potential lycopene contribution to cardiovascular health from the overall contribution from tomato products and other components present in tomatoes. The lack of coherence between available epidemiological data and dietary intervention data underscores the requirements for further studies to unravel other non-lycopene components in tomato and their roles in CVD risk reduction. Tomatoes contain several known and unknown compounds that might affect platelet function, lipid metabolism, blood pressure and endothelial function, important determinants of CVD [5, 39]. Lycopene or other antioxidants act through inhibition of LDL oxidation alone and so may only partly contribute to the CVD risk reduction. Recent studies showed that tomato also contains gamma-aminobutyric acid, 13-oxo-9,11-octadecadienoic acid and esculeoside A, which may provide heart and psychological health benefits [40]. 13-oxo-ODA is, however, found only in tomato juice [41]. Esculeoside A reduces plasma lipids and therefore may ameliorate atherosclerotic lesions in ApoE-deficient mice [42]. This indicates that other unidentified compounds (non-lycopene compounds) may also contribute to the cardio-protective effects of tomatoes as observed in epidemiological and interventional studies.
Role of platelet hyperactivity in the development of CVD
Platelet activity is thought to play a major role in the development as well as the stability of atherosclerotic plaques. Abnormal activation of blood platelets might represent a contributory risk factor for accelerated vascular disease, which occurs in hypertension, because it plays an important role in the development and progression of atherosclerosis [43]. In support of the pathophysiological role of platelets, platelet inhibitory drugs such as aspirin have been observed to reduce the incidence of myocardial infraction, stroke and death from CVD in secondary prevention trials [11, 43]. The pathophysiological state of platelets (hyperactive) is the underlying risk of problems in diabetes, smoking, obesity and sedentary lifestyle and other conditions (Table 1). Although the mechanism of the increase in platelet reactivity is uncertain in these conditions, it could be caused by sensitization of platelets to aggregation by elevated levels of agonists in vivo [44], or it could be due to the redistribution of young, more reactive platelets that are concentrated in the spleen [45] and are released into the systemic circulation. Platelets are activated by a large number of agonists that are released in the circulation during some pathologic conditions (e.g. hypertension and diabetes mellitus) [46]. Several lines of evidence point to an important role for platelets in the pathogenesis of sudden death, acute myocardial infarction and unstable angina [47]. Other evidence supporting a causal role of local platelet activation in the pathogenesis of acute coronary events comes from studies demonstrating that aspirin, an inhibitor of platelet thromboxane A2 (TxA2) synthesis, reduces the incidence of acute myocardial infarction and of cardiac death in patients with unstable angina. Recently, aspirin’s antiplatelet limitations have progressively underscored the critical need for improved platelet aggregation inhibitor therapy which is not only effective, but also safe and well tolerated [11, 48, 49]. This concept has stimulated research into prevention of platelet hyperactivity by several means including dietary supplementation. Development of the atheroma is a gradual process, understood to be influenced by well-established traditional risk factors, including (but not limited to) hypertension, cigarette smoking, diabetes mellitus, dyslipidemia and a family history of premature atherosclerotic disease. Considerable investigation into the pathophysiological effects induced by these factors has elucidated their contributions to the prothrombotic milieu within the atherosclerotic coronary artery preceding an atherothrombotic event. Activated platelets release different growth factors (e.g. PDGF and VEGF) that participate in the development of atherosclerosis by promoting VSMC proliferation [50]. Stimulated platelets release VEGF [51], and elevated VEGF levels have been found in patients with atherosclerotic risk factors such as hypertension [52]. Tests of platelet function have been used to investigate a possible role of platelet hyper-reactivity in the pathogenesis of vascular disorders and their complications. Platelet activation and aggregation are also involved in the development of hypertension in different ways. Activated platelets release different mediators, such as 5-hydroxytryptamine (5-HT or serotonin), ADP, ATP and lysophosphatidic acid [50]. A number of these agents enhance the intracellular Ca2+ concentration ([Ca2+]i) in vascular smooth muscle cells (VSMC), which promotes vasoconstriction and increases catecholamines response. Furthermore, the number of platelet α-adrenergic receptors increases in hypertensive persons [53], which may promote catecholamines responses. Catecholamines, β-adrenoceptor agonist isoprenaline and angiotensin II (Ang II) increase [Ca2+]i and promote contraction of VSMC, platelet activation and aggregation [53] which may participate in the genesis and maintenance of hypertension. Moreover, it has been shown that Ang II increases [Ca2+]i and pH in platelets from hypertensive patients, which may be associated with enhanced platelet aggregation [54]. In hypertension, platelets showed spontaneous aggregation and increased sensitivity to agonists [55, 56]. Furthermore, platelets release more β-thromboglobulin and P-selectin and have higher intracellular Ca2+ levels [57, 58]. Hypertension is associated with oxidative stress [57]. Thus, in hypertensive patients, platelets produce more reactive oxygen species which enhance platelet activity by reducing the bioavailability of nitric oxide (NO) and enhancing [Ca2+]i among other cellular effects. Platelets are directly influenced by specific adipokines and therefore have the potential to serve as an essential mediator of the cardiovascular consequences of obesity. Consistent with this, obesity has been associated with increases in platelet aggregation, elevations in surface expression of markers of platelet activation such as P-selectin and heightened platelet microparticle formation. More importantly, reduction in adipose mass leads to normalization of markers of enhanced platelet activation. However, a causal role for platelet hyperactivation in obesity-related cardiovascular disorders remains to be established. Several characteristics and proven biological activities of platelets make them an appealing candidate for triggering and maintaining the inflammatory response of obesity. Activated, but not resting platelets are able to alter the chemotactic properties of endothelial cells by inducing the secretion of monocyte chemoattractant protein. Similarly, transforming growth factor-β is released from activated platelet α-granules and has been shown to augment the release of type-1 plasminogen activator inhibitor from adipose tissue. Importantly, a recent report indicates that the recruitment of inflammatory cells in adipose tissue is facilitated by platelet adhesion along activated endothelium. Based on these observations, it seems that platelet activation, secondary to obesity, plays a causal role in triggering and maintaining the pro-inflammatory and pro-thrombotic state of obesity, creating a feedback loop involving adipose tissue, activated platelets and vascular endothelium that culminates in an environment favourable for atherothrombotic vascular events [59, 60]. Therefore platelet activation contributes to the inflammatory and thrombotic consequences of obesity. All the data indicate the importance of taming platelets in order to avoid CVD.
In vitro studies with water-soluble tomato extract on human blood platelet aggregation
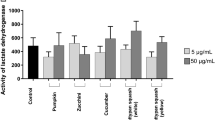
The antiaggregatory effects of different aqueous fruit extracts on human platelets in vitro have been published previously [13]. The maximum inhibitory effect (70–75 %) was found to be with tomato and kiwi fruit extracts, whereas apple and pear had very little activity (2–5 %). Grapefruit, melon and strawberry had intermediate activities on platelet aggregation (33–44 %). The antiplatelet potential of the fruits tested appeared to have no relationship with their antioxidant activity [13]. These antiplatelet compounds in tomato had a molecular mass less than 1000 Da and were highly water soluble and stable to boiling. The compounds of interest were concentrated into an aqueous extract produced by homogenizing fresh tomatoes, removing particulate matter and delipidating. The delipidated aqueous extract was then further fractioned by gel filtration using a Biogel P2 column [13]. Adenosine, a known antiplatelet factor, was identified in one fraction, but its removal from the whole extract did not substantially decrease the antiplatelet activity, indicating the presence of additional, different antiplatelet agents. Further work showed that the aqueous tomato extract consisted largely of soluble sugars (85–90 % of dry matter), which showed no in vitro antiplatelet activity [15]. The non-sugar material that was isolated (tomato total active fraction, tAF) accounted for 4 % of the aqueous tomato extract dry matter and showed strong inhibition of platelet aggregation in vitro. Isolation of many individual components from tAF followed, and it was found that most fell into one of three categories—nucleosides, simple phenolic derivatives and flavonoid derivatives. All showed antiplatelet activities consistent with their compound categories.
Proteomic experiments carried out to examine effects of tAF on platelet signalling pathways showed that tAF components altered a range of platelet functions including those regulating platelet structure, coagulation and redox status (Fig. 2). One of the most strongly affected proteins was protein disulphide isomerase (PDI), an oxidoreductase which catalyses the formation and the isomerization of disulphide bonds. In platelets, blocking PDI with inhibitory antibodies inhibits a number of platelet activation pathways, including aggregation, secretion and fibrinogen binding [61, 62]. Other investigators [63] have reported similar functional effects after blockage of cell surface thiol isomerases. Glycosides related to quercetin, of which several are present in tAF [O’Kennedy N. Fruit extracts. International Patent WO 2010/049707, May 06, 2010], have been shown to interact with PDI in this way [64, 65]. Interaction of polyphenols with PDI suggested a possible mechanism by which tomato extract components could inhibit different pathways of platelet aggregation.
Effects of Fruitflow® on the platelet proteome. Classes of protein showing statistically significant changes after treatment with Fruitflow® at a concentration of 43 mg L−1 (maximum theoretical circulating concentration after ingestion of a single 3 g/150 mg dose equivalent to 65 mg tAF or approximately three bowls of tinned tomato soup)
The functional effects of tAF components were therefore examined in a series of experiments. tAF and its sub-fractions F1, F2 and F3, prepared by semi-preparative reversed-phase HPLC as described by O’Kennedy et al 2006 [66], were observed to prevent activation of integrin αIIbß3 (ie, GPIIb/IIIa). Inhibition of the GPIIb/IIIa activation step—which is common to multiple aggregation pathways—could underlie the wide-ranging effects of tAF [15]. This is consistent with the observation that basal platelet cyclic AMP concentrations (controlled by phospholipase C enzyme family-mediated cascade reactions) are unaltered by tomato extract active components in vitro. In addition, tAF reduced the expression of P-selectin (CD62P) on the platelet surface in response to ADP-induced platelet activation in whole blood [15, 66]. In resting platelets, P-selectin is localized in the membranes of platelet α-granules. On platelet activation, it is redistributed to the platelet surface, where it initiates adhesion to leucocytes. Under conditions of blood flow and shear stress, this glycoprotein promotes platelet cohesion and stabilizes newly formed aggregates. Thus, tAF components can potentially affect the size and longevity of platelet aggregates. tAF components were also found to affect the binding of tissue factor (TF) to activated platelets, at least in part due to effects on P-selectin [O’Kennedy N and Song H-J. Therapeutic uses of tomato extracts. International Patent WO 2007/141495, December 13, 2007].
In summary, these results demonstrating the actions of tAF on different platelet functions were all consistent with potential effects mediated partly through polyphenols and PDI and partly through nucleosides elevating cAMP and cGMP levels in platelets [13, 67]. Effects on TF binding suggested that tAF components could have a larger effect on some aspects of the coagulatory response, such as thrombin generation, than previously imagined. Figure 3 summarizes the actions of different ingredients of Fruitflow® on platelet activation pathway.
Platelet activation via multiple pathways and sites of action of Fruitflow® ingredients. Key agonists, their receptors and triggering signalling pathways involved in platelet activation and subsequent aggregation. VWF von Willebrand factor, TXA2 thromboxane-A2, TP thromboxane receptor, ADP adenosine diphosphate, PAR proteinase-activated receptor, PDI protein disulphide isomerase, TF tissue factor. The activation of platelets is accompanied by a conformational change in integrin aIIbb3 (glycoprotein (GP) IIb–IIIa), exposing a binding site for fibrinogen and triggering the release of aggregating agents such as TXA2 and ADP. Adenosine nucleotides signal through P2 purinergic receptors (P2Y) on the platelet membrane. Activation of these receptors initiates a complex signalling cascade that ultimately results in platelet activation, aggregation and thrombus formation. Thrombin acts via cell surface protease-activated receptors (PARs). Both stimulate PLC giving rise to PIP2 hydrolysis and consequent activation of PI3K. Collagen acts both through receptors (GPIV) and on integrin a2b1, promoting adhesion and triggering inside-out signalling. Inside-out signalling alters platelet skeletal characteristics to allow spreading and microparticle release, leading to increase in pro-coagulant potential. Inside-out signalling also exposes PDI on the platelet surface, which can alter the pro-coagulant potential of TF in situ, or alternatively transfer to endothelial cells. Fruitflow components have been shown to affect ADP, collagen, thrombin and TXA2-mediated signalling, to affect integrin activation and subsequent fibrinogen binding, and to down-regulate platelet PDI
Development of Fruitflow®: Compositional and structural aspects
To develop prototype plant-derived antiplatelet extracts in the laboratory requires understanding of the extract components and the structure–function relationships affecting their mechanism of action and potency. These details were largely established for aqueous tomato extracts during an exploratory research phase as discussed earlier. However, to move from the laboratory prototype to a standardized food ingredient required a change in focus to extract reproducibility, cost analysis and development of a rigorous quality assurance system capable of standardizing bioactivity and controlling raw material variation, processing-induced effects and multiple sites of manufacture. Focusing on these points developed the small-scale laboratory-grade aqueous tomato extract into a commercial food grade tomato extract, which was given the trade name Fruitflow®.
Today, Fruitflow® is made in two ingredient formats. The raw material for both formats is high grade, minimally processed tomato commodity products. Fruitflow® 1 is a syrup of which more than 50 % w/w comprises tomato-derived carbohydrates, and ~3 % w/w comprises known bioactive compounds with measured antiplatelet activity. This ingredient format is especially suitable for use in drinks and foods with high water content. Fruitflow® 2 is a low-carbohydrate powder, of which more than 55 % w/w comprises bioactive compounds, dried to produce a tablet-grade powder. Fruitflow® 2 can be compressed into tablets and has flow properties which render it suitable for capsule formation or for use in dry-blend food processes. Both ingredient formats are lycopene- and fat-free, low in inorganic salts and low in organic acids. The potency of Fruitflow® 1, in terms of bioactive compound content/g, is lower than that of Fruitflow® 2, as a consequence of their different sugar content: relative potencies of the two ingredients when compared w/w are in an approximate ratio of 1:20. Thus, 3 g Fruitflow® 1 gives an equivalent dose of bioactives (approximately 65 mg) to 150 mg Fruitflow® 2. Of this quantity, 6–10 % (up to 9 mg) are known nucleoside derivatives (F1), 13–15 % (up to 10 mg) are known phenolic conjugates (F2), and 8–10 % (up to 7 mg) are known flavonoid derivatives (F3), including a minimum of 2.4 mg quercetin derivatives per dose. This amount of bioactive compounds, which comprises a single daily dose, is equivalent to that found in about 3 average servings of tinned tomato soup.
The development of a quality assurance system which allows such standardization began with the implementation of an analytical HPLC system simple enough to run on the factory floor, but precise enough to measure selected important antiplatelet compounds through each process step. The individual bioactivity profiles of compounds occurring in Fruitflow® were examined, and three representative components, one from each of the three broad fractions F1, F2 and F3 (as discussed earlier, these fractions were originally defined by reverse-phase HPLC fractionation, described in [15]), were selected. These three compounds were adenosine, which represents a group of nucleosides/nucleotides found in F1, chlorogenic acid, which represents a group of phenolic derivatives found in F2, and rutin, which represents a group of flavonoid derivatives found in F3. The representative compounds were monitored throughout the developing process, from raw material to final product; losses in any one of them would reflect losses of the entire class of compounds each represented and could be quantified and assessed. In addition, total tAF content was quantified throughout. The data collected were mapped onto bioactivity (antiplatelet activity) and the validity of the measurements as a method of monitoring overall bioactivity established. The use of this bioactivity-led analysis then facilitated selection of suitable raw materials, control of raw material variability and investigation of the effects of thermal processing on bioactivity of extracts produced.
The presence within tomatoes of such a range of structurally different water-soluble secondary metabolites reflects both the complex sensory profile of the tomato and its response to stresses. Many of the bioactive compounds are produced in the tomato fruit as part of the plant defences against insect or bacterial challenges. However, as tomatoes are grown under a wide range of conditions worldwide, a similarly wide variability in secondary metabolite composition might be expected. Table 2 shows the content of antiplatelet compounds (tAF) in tomato juice and the overall antiplatelet activities of the juice, from a range of different cultivars, geographical sources and degrees of ripeness. While tomatoes from different geographical locations and of different cultivars did show differences in the quantity of antiplatelet compounds extracted, the degree of ripeness of the tomatoes appears to be the most important factor in determining bioactivity. Thus, ripeness of tomatoes at the time of harvest became a key quality assurance factor in the development of the Fruitflow® food ingredients.
The type of processing undergone by fresh tomato fruit determines the extent to which the original antiplatelet activity of the fresh fruit can be retained. High-temperature processing and/or long holding times at moderate–high temperatures are detrimental to the antiplatelet activities of final products. Table 3 shows the tAF quantified in a range of processed tomato foods. Many of the products tested displayed a very low tAF content and a correspondingly low bioactivity. It became evident from this work that control of temperature and time at temperature during processing was a key to retaining bioactivity in any process attempting to make a concentrated extract from tomato juice. On this basis, after a survey of available materials, cold break (low heat treatment), minimally processed tomato products were chosen as suitable starting materials for a high antiplatelet activity tomato extract. Once the starting material and its quality controls had been established, the Fruitflow® 1 and 2 extraction processes were designed and optimized, with reference to content of tAF and the three representative bioactives, in a way that directly optimized bioactivity. The key features of both processes were control of time spent at high temperatures and the balance necessary to achieve the desired temperature profile while avoiding microbiological and waste issues. Fruitflow® 1 is currently produced from cold break minimally processed tomato products (pastes, passatas, juices) in a 5-step process, which utilizes physical separation methods (centrifugation, filtration) at low temperatures to remove pulp and unwanted insoluble solids from the starting material, leading to a clear yellow juice. This is then concentrated by low-temperature evaporation and standardized for pH.
Fruitflow® 2 is a low-sugar derivative of Fruitflow® 1, deriving from the same raw material and using the same initial clarification processing steps. After removal of insoluble material, complex and simple sugars are extracted from the clarified tomato juice using an adsorption column process, in which the sugars which are the major constituents of tomato juice pass through a resin column without retention, while the remainder of the juice components are adsorbed from the juice and retained on the column. These retained components of interest—which can represent up to 2 % of the fresh weight of the tomato-derived starting material—are then recovered from the column, and the concentrate is dried to powder and standardized for moisture content. The resulting Fruitflow® 2 powder contains almost no sugars (glucose, fructose, pectin, starch or derivatives). The bioactive components are present in concentrations between 28–32 times higher than in Fruitflow® 1, due to the removal of the sugar and water matrix of the syrup ingredients. However, as the resin column used successfully retains the remainder of the tomato juice constituents, the relative occurrence of these components in Fruitflow® 2 remains similar to that in Fruitflow® 1 (i.e., the process does not significantly alter the relative proportions of the bioactive components).
An industrial specification for each ingredient ensures that the final product of each process is an extract whose antiplatelet activity against ADP, collagen, AA and TRAP in vitro is above a minimum level (Table 4) and as close to fresh tomato juice as possible. This specification is achieved by the monitoring of tAF and the three compounds adenosine, chlorogenic acid and rutin, representatives of F1, F2 and F3 in the fresh tomato. The specification allows a standardized usage of the ingredients, so that Fruitflow® 1 and 2 may be used interchangeably depending on the application.
The Fruitflow® 1 and 2 ingredients are now incorporated into a range of different food products, ranging from drinks to tablets. Both ingredients are stable in a wide variety of matrices, with appropriate shelf life in all, tested to industry standard ICH levels.
Human trials undertaken with Fruitflow® 1 and Fruitflow® 2
Early studies
The first study which investigated the antiplatelet effects of a water-soluble tomato extract used freshly prepared tomato juice. As this juice was low in tAF concentration, a volume of 1L was given to ensure sufficient ingestion of tAF components. No significant effects could be observed in the small study group (n = 9, Fig. 4a). However, a second study using a crudely prepared prototype tomato extract concentrate, in which the subjects consumed approximately the same dose of bioactive compounds as in the 1L study, but in a much smaller volume (~10—12 mL), did show an observable effect on platelet function at a variety of times after supplementation (Fig. 4b). It was concluded that tomato juice would be an inappropriate vehicle for its antiplatelet compounds when attempting to achieve a systemic acute antiplatelet response via oral ingestion, and work began to refine the crude prototype already tested.
Summary of results from early-stage studies using tomato extract prototypes. a % Change from baseline aggregation observed after ingestion of 1L freshly produced, filtered tomato juice, by healthy subjects (n = 9). This was a pilot study and was not placebo-controlled. Changes from baseline aggregation in response to ADP and collagen were not significant. b % Change from baseline aggregation observed after consumption of either a prototype concentrated tomato extract or control extract for a period of two weeks. The study involved healthy subjects (n = 14). Changes from baseline aggregation in response to optimal ADP agonist (concentration used titred to give optimal platelet response in each sample) were significantly different from control at t = 2 weeks
Main body of studies undertaken with standardized Fruitflow® 1 and Fruitflow® 2
After development of the Fruitflow® ingredients, and standardization of testing conditions, a unified set of studies was carried out to establish the efficacy of these novel ingredients ex vivo. A summary of the studies in which the standardized ingredients Fruitflow® 1 and Fruitflow® 2 have been used is given in Table 5. This table also allows comparison of the major outcomes of each of these studies, in terms of the extent of the antiplatelet effects measured in comparison with the study baseline and to the study control. Studies which established the onset time of an acute antiplatelet effect after oral ingestion of a dose of Fruitflow® 1 have been published elsewhere [15]. These studies showed that in all subjects, an acute lowering of platelet aggregability to ADP and collagen was observed at a time three hours after consuming Fruitflow® (Table 5, #1). The range of onset times was from one and a half hours to three hours after consumption. In contrast, the normal diurnal increases in platelet aggregability were illustrated in subjects consuming the control supplement over the time course measured. The persistence of this acute effect varied between individuals, but in all cases platelet aggregability returned to baseline 18 h after consumption of a single dose of Fruitflow® [68].
Size and variance of the acute antiplatelet effect
The range of acute antiplatelet effects observed in all studies undertaken is shown in Table 5. On average, these studies have shown an inhibition of the platelet response to ADP agonist of approximately 17–25 % and an inhibition of the response to collagen of approximately 10–18 %. Arachidonic acid-induced platelet aggregation and thrombin receptor-activating peptide (TRAP)-induced platelet aggregation have also been shown to fall after Fruitflow® administration. A study in which Fruitflow® 1 was administered to 93 healthy men and women (Table 5, #2) [16] showed that some variability in response may occur, with men responding more than women, and subjects with higher risk factors for CVD responding more highly than others. A dose–response was established in studies administering different amounts of Fruitflow® 1 (Table 5, #1); the shape of the dose–response curve is shown in Fig. 5. This dose–response work established that a dose of Fruitflow® equivalent to 65 mg tAF or approximately 3 average bowls of tinned tomato soup already caused close to the maximum level of platelet inhibition achievable by this extract and that no significant gain would be obtained in an acute setting from increasing the dose.
Dose–response curve at t = 3 h after ingestion of Fruitflow® 1 at different dosage levels, in 23 subjects (Study #2, Table 5). Dose 2 tomatoes represents a single dose of Fruitflow® 1 corresponding to 65 mg tAF components, while dose 6T represents a three doses corresponding to 195 mg tAF components. Data shown for dose 8 tomatoes (corresponding to 260 mg tAF components) are extrapolated from the curve generated
Effects of ingredient format and food matrix on the observation of antiplatelet effects
Two studies have been undertaken focusing on the two different ingredient formats, Fruitflow® 1 and Fruitflow® 2, and the likelihood of matrix effects altering the acute antiplatelet response after consumption (Table 5, #4, #6). These studies, which involved 54 subjects, showed firstly that it was not possible to distinguish between the antiplatelet effects observed for the Fruitflow® 1 and Fruitflow® 2 ingredients, when consumed in doses of 3 g and 150 mg, respectively (Table 5, #4). No difference between the two ingredient formats could be detected three hours after consumption. Secondly, the studies showed that incorporation of WSTC into water-based drinks, yoghurts and capsules was all viable means of inducing an antiplatelet effect three hours after consumption (Table 5, #6). The antiplatelet effects observed in all matrices were similar to those seen in previous studies (Table 5).
Effects of chronic consumption
Once the time of onset, persistence and size of effect related to a single dose had been established, studies examining the effects of continuous (i.e. daily) consumption of Fruitflow® were undertaken. These studies showed that the size of the antiplatelet effect observed after consuming a single dose of Fruitflow® daily for two or for four weeks was not significantly different from the size of effect observed after a single dose, that is, the observed effects were not cumulative (Table 5, #3). Suppression of platelet function achieved through chronic consumption was continuous—measurements of platelet function were taken in fasted subjects in the morning, approximately 24 h after consumption of their last Fruitflow® dose, and suppression of original baseline platelet function was observed after two and four weeks.
Safety considerations
Compounds found in Fruitflow® have been shown to affect many aspects of platelet function, including (via effects on TF immobilization and signalling) thrombin generation. Therefore, during all human intervention studies, care was taken to incorporate specific safety-focused measures to examine whether any effects on the intrinsic or extrinsic clotting pathways could be detected alongside antiplatelet effects. An antiplatelet which also affected blood coagulation pathways could raise safety concerns. However, in all intervention studies undertaken, clotting time measurements showed no significant increases from baseline levels (Table 5). Fruitflow® does not directly affect blood coagulation at any dose tested.
Even without affecting blood coagulation directly, many antiplatelet drugs, taken on a chronic basis, give rise to excessive platelet inhibition and are associated with internal bleeding. These potentially serious side effects mean that antiplatelet therapy, a fundamental aspect of CVD secondary prevention, is contraindicated for primary prevention as the benefit conferred (lowering risk of a first CVD event in relatively low risk groups) is outweighed by the increased risk of gastric or intracranial bleeding [49]. This judgement was recently revisited by the US FDA, in the context of increasing obesity and type 2 diabetes mellitus levels in relatively young populations, but was upheld [69]. The known side effects of existing antiplatelet drugs related to internal bleeding were clearly pertinent for consideration during Fruitflow® development. However, Fruitflow® differs fundamentally from antiplatelet drugs in the reversibility of its action. The widely used antiplatelet drugs have irreversible mechanisms of action. Over the course of ten days, approximately 90 % of the circulating platelet population can be irreversibly affected for the lifetime of those platelets. This level of platelet inhibition is then maintained by daily drug treatment. Conversely, the antiplatelet effects of Fruitflow® are not irreversible, or cumulative, and can be overcome by increased agonist concentrations. This very significant difference in mode of action renders Fruitflow® suitable for use by the general population as a dietary functional ingredient, while antiplatelet drugs cannot be used.
As Fruitflow® is designed as a food ingredient, with potential for incorporation into a variety of food products, a specific study was undertaken to examine the likely effects of overconsumption (Table 5, #5). As the amount of Fruitflow® in any one food product serving is low, equivalent to approximately three bowls of tinned tomato soup, and as dose–response studies had shown that increasing the dose significantly would not result in a much bigger acute effect on platelets, no significant dangers were anticipated. The results of the study confirmed this position; drinking 1L of a drink containing four daily doses of Fruitflow® did not dangerously reduce platelet aggregability compared to baseline. In fact, the reduction in platelet functionality observed was rather less than that observed for a single serving of the same product. This underlines again the effects of food volume on observable systemic antiplatelet effects.
Comparing the dietary antiplatelet Fruitflow® with the antiplatelet drug aspirin
A study comparing a single dose of Fruitflow® with 75 mg aspirin, either as a single dose or taken continuously for one week, was undertaken in order to benchmark the effects of a dietary antiplatelet (Table 5, #7). A comparison of the effects of Fruitflow® and aspirin on the platelet proteome was first carried out, to examine similarities and differences in mechanisms of action. This comparison showed that aspirin and Fruitflow® affect broadly similar proteomic pathways, with aspirin affecting the signalling pathways more strongly than Fruitflow®—assuming full metabolism of the entire ingested dose. Proteins affected by Fruitflow® and aspirin are associated with platelet structure, platelet coagulation, platelet membrane trafficking and platelet secretion - actin-binding proteins, fibrinogen beta chain 5, Ras-related proteins, redox system proteins and HSP70s. Of the 26 proteins with altered expression after treatment, 11 were affected by both Fruitflow® and aspirin, 14 by aspirin alone and one by Fruitflow® alone. The single protein affected only by Fruitflow® was identified as PDI, known to disrupt inside-out signalling as described earlier.
The intervention study which followed in 47 healthy subjects showed that the effects of a single dose of Fruitflow® were similar, in terms of antiplatelet action, effects on thromboxane synthesis and time to form a primary haemostatic clot (PFA-100 closure time), to those of a single 75 mg dose of aspirin (Table 5, #7). When aspirin was taken daily for seven days, the associated increase in PFA-100 closure time was three times higher than that associated with a single aspirin dose. The cumulative antiplatelet effect of aspirin when taken daily is well known and reflects its irreversible disabling of platelet COX-1 and associated signalling. Fruitflow®’s effects are not cumulative in this way, as its effects do not irreversibly disable platelet signalling pathways. Thus, taking the results for the study population as a whole, daily aspirin supplementation may be viewed as approximately three times as efficacious as daily Fruitflow® supplementation, due to the irreversibility of its action. This overall result seemed to echo the proteomic data, but further examination showed that it masked some interesting behaviour in study subgroups. The antiplatelet effects of aspirin in healthy subjects are extremely heterogeneous, with some subjects experiencing a very large increase in time to form a primary haemostatic clot, while others respond poorly (Fig. 6). Approximately 50 % of aspirin responders had a response to the drug which was lower than the average response for the treatment group, in terms of time to form a primary haemostatic clot. This group of subjects had a residually strong response to collagen after 7 days of aspirin treatment, and over one-third of the group responded better to Fruitflow® supplementation than to 7-day aspirin supplementation. At the other end of the spectrum, for 18 % of the study population, taking aspirin for 7 days more than trebled the time to clot. This underlines the reasons behind the known internal bleeding risks associated with aspirin and its unsuitability for use in primary prevention. While the response to Fruitflow®, in terms of time to clot data, was also heterogeneous, it was markedly less so than the response to aspirin (Fig. 6). The majority of the subject group experienced increases in time to form a primary haemostatic clot of up to twofold, with less subjects at either extreme. It would appear that the proteomic predictions of stronger aspirin-led effects on platelet signalling may not be observed ex vivo, possibly due to wide variability in the extent of aspirin metabolism, but also possibly due to differences in the relative importance of platelet collagen signalling pathways between individuals. Fruitflow®, with its wider range of antiplatelet compounds, may have a less variable metabolism and thus achieve its more moderate effects more widely. These more moderate effects, which can be related to the reversibility of the antiplatelet action of Fruitflow® rather than its mode of action per se, render it a possible option for use in primary prevention of CVD, in contrast to aspirin at any dosage. However, outcomes-based studies on dietary supplements such as Fruitflow® are needed before their true potential can be properly assessed.
Increases in PFA-100 closure time by aspirin and Fruitflow®. Time to form a primary clot after treatment with either 7d aspirin (top) or Fruitflow® (bottom) was determined. The proportions of the study population experiencing less than twofold, up to twofold and over threefold increases in time to form primary clot are shown, illustrating the heterogeneity of the responses observed
EFSA approval of Fruitflow® and its commercialization in different countries
In 2006, the European Union (EU) adopted a regulation on the use of nutrition and health claims for foods which lays down harmonized EU-wide rules for the use of health or nutritional claims on foodstuffs (Regulation (EC) No 1924/2006). One of the key objectives of this regulation is to ensure that any claim made on a food label in the EU is clear and substantiated by scientific evidence. Different categories of claim are defined. Health claims are defined as pertaining to relationships between food and health either with regard to a function of the body (Article 13 claims), or with regard to reducing a risk factor for a disease (Article 14a claims), or with regard to children’s development (Article 14b claims). Nutrient claims are defined as pertaining to foods with particular nutritional properties with regard to either the energy, or the nutrients, they provide. Allowed nutrient claims are clearly defined within the regulation. However, companies wishing to associate their food or ingredient with a health claim must submit a dossier in support of the desired claim, which is then assessed by the EFSA Panel on Dietetic Products, Nutrition and Allergies. Key to the dossier is the inclusion of human intervention studies showing evidence of the health benefit claimed, for the food/ingredient of interest. More than 2,200 unique claims have been submitted for assessment to date, of which over 95 % have been Article 13 claims, with an overall approval rate of close to 10 %. The first Article 13 claim based on newly developed evidence or proprietary data [a special category under Article 13(5)] to be achieved, in December 2009, was for Fruitflow®, when the EU Commission authorized the health claim “water-soluble tomato concentrate (WSTC) I and II helps maintain normal platelet aggregation, which contributes to healthy blood flow”. The authorized claim was based on the eight human studies (seven proprietary), and seven non-human studies (three proprietary), conducted with Fruitflow®, which is given in Table 5.
Thus, Fruitflow® is now authorized by EFSA for daily consumption, with the conditions that 3 g Fruitflow® 1 or 150 mg Fruitflow® 2 must be included in either foods (e.g. fruit juices, flavoured drinks or yoghurt drinks with a total volume up to 250 mL), or in powdered, tabletted or encapsulated food supplements (to be taken with up to 250 mL water).
New functionalities of Fruitflow®: Anti-inflammatory and blood pressure-lowering effects
Atherosclerosis is considered as a chronic inflammatory disease of the arterial vessel wall and is a major cause of mortality and morbidity in the world [70–72]. Inflammation plays a critical role in the initiation and progression of atherosclerosis; it involves the recruitment of inflammatory cells from the circulation and their transmigration through the endothelial wall, resulting in vascular damage, narrowing and hardening of the arteries [71]. The intake of tomatoes and tomato products has been associated with a decreased risk of chronic inflammatory diseases such as atherosclerosis and is linked with a healthy Mediterranean diet [1, 33, 73]. Moreover, several in vitro animal and human studies have shown that tomato concentrates and phytochemicals from tomato have anti-inflammatory activities and may reduce the risk of CVD [73–78].
Activation of the inflammatory pathways in macrophages plays a critical role in the initiation and progression of endothelial dysfunction which eventually results in atherosclerosis. The influence of Fruitflow® on the inflammatory response of macrophages and on endothelial dysfunction in human umbilical vein endothelial cells (HUVEC) has recently been investigated [18]. In this study, Fruitflow® was able to regulate the production of cytokines and interleukins in LPS-stimulated macrophages. It decreased the production of pro-inflammatory cytokines (TNF-α, IL-1β and IL-12), while the production of the anti-inflammatory IL-10 was increased. Consequently, Fruitflow® reduced the production of inflammatory mediators related to chronic inflammation. Nuclear factor-κB (NF-κB) is an important pro-inflammatory transcription factor, and its activation is involved in the pathology of vascular inflammatory diseases. Gene expression analysis indicated that Fruitflow® reduced the expression levels of NF-κB, suggesting that Fruitflow® regulated the gene expression of inflammatory mediators via the NF-κB pathway. The data are in agreement with the recent publication from Navarrete et al. [79] which investigated the effects of an aqueous extract of tomato (produced in a similar manner to the laboratory-scale aqueous extracts described here) on the expression of pro-inflammatory cytokine in LPS-activated monocyte-derived THP-1 macrophages. The Navarrete aqueous tomato extract was shown to inhibit the expression of cytokines (TNF-α, IL-1β) and the activation of NF-κB in the LPS-stimulated macrophages. Intercellular adhesion molecule-1 (ICAM-1) and vascular cell adhesion molecule-1 (VCAM-1) are two critical adhesion molecules that are expressed on endothelial cells and mediate adhesion of leucocytes and their interactions with inflamed endothelial cells leading to endothelium damage [80]. Activation of the endothelial cells and the production of inflammatory mediators by atherosclerotic lesions results in the up-regulation of the adhesion molecules (ICAM-1, VCAM-1). Thus, ICAM-1 and VCAM-1 are considered as early markers of endothelial dysfunction and atherosclerosis. In the Schwager et al study (2016), Fruitflow® significantly decreased the production and the gene expression of ICAM-1 and VCAM-1 in activated HUVEC. This suggests that Fruitflow® may be capable of altering some of the pathologies typically seen in endothelial dysfunction. Tomato is a rich source of lipophilic and hydrophilic phytochemicals which could influence the inflammatory response [73]. Fruitflow® is standardized using three “natural” constituents: adenosine, chlorogenic acid and rutin, which are representative of the three main groups of active constituents and have been shown to inhibit both platelet aggregation and inflammatory pathways. Adenosine has been suggested to play a role in immune and inflammatory processes and to improve various inflammatory diseases [81–84]. Chlorogenic acid is a polyphenol with anti-inflammatory activity, which inhibits the LPS-triggered activation of NF-κB and the associated inflammatory response [85, 86]. In macrophages, rutin suppressed oxidative stress and modulated the gene expression of mediators involved in chronic inflammation [87, 88] [89]. Collectively, the data indicate that compounds contained in Fruitflow® have the capacity to modulate signalling pathways which alter vascular function, the development of atherosclerotic lesions and consequently the risk of CVD by various mechanisms including anti-inflammatory effects. The extent to which such pathways can be affected in humans after ingestion of Fruitflow® is not yet known and could form an interesting topic for future studies. Figure 7 summarizes the effects of Fruitflow® on the endothelial response to inflammatory stimuli via different mechanisms such as activation of NF-κB and the up-regulation of adhesion molecules.
Fruitflow® inhibits the activation of macrophage and endothelial cells via different mechanisms. The endothelium reacts to inflammatory stimuli derived from activation of cytokines such as NF-κB, and the up-regulation of adhesion molecules (ICAM, VCAM), which play a role in leucocyte adhesion and transmigration across the endothelial layer. NF-κB is a key transcription factor which induces the release of pro-inflammatory mediators (cytokines, chemokines and adhesion molecules) that further promote vascular inflammation leading to the initiation and development of atherosclerosis. This Fruitflow® inhibits the activation of macrophage and endothelial cells, which could help to reduce leucocyte recruitment and promote a reduction in tissue inflammation
Hypertension is another very important risk factor for CVD including coronary heart disease, stroke, congestive heart failure and peripheral vascular disease [90]. Clinically, hypertension is characterized by abnormally high blood pressure with the systolic reading greater than 140 mmHg and diastolic reading greater than 90 mmHg. Lowering blood pressure has been linked to 35 %–40 % reductions in the incidence of stroke, 20 %–25 % in myocardial infarction and up to 50 % in heart failure, making hypertension a strong target for therapeutic intervention. Because dietary changes are a first-line intervention for hypertension, food products themselves are increasingly under consideration for the specific effects they may have on blood pressure. In recent years, there has been considerable interest in the potential for using natural food components as functional foods to treat hypertension, especially for people with borderline to mild high blood pressure that does not warrant the prescription of antihypertensive drugs. Increasingly, nutraceuticals and food products have been investigated for their effects on hypertension. Polyphenols inhibit and down-regulate expression of angiotensin-converting enzyme (ACE) and renin. In addition, polyphenols have also been associated with the formation of endothelial nitric oxide leading to vasodilation and lowering of blood pressure. The renin–angiotensin system is a powerful mechanism for controlling blood pressure [91, 92]. In hypertensive patients with elevated plasma rennin–angiotensin activity, a fivefold increased incidence of myocardial infarction was demonstrated [93]. ACE (EC 3.4.15.1, dipeptidyl carboxypeptidase) is a glycoprotein peptidyldipeptide hydrolase that cleaves histidyl leucine dipeptide from angiotensin I forming the potent vasoconstrictor angiotensin II. Studies demonstrated that ACE inhibitors (ACEIs) significantly reduced the morbidity and mortality in patients with myocardial infarction and the incidence of ischaemic events in patients with CVD, even in the absence of their blood pressure-lowering effects [94–96]. The therapeutic administration of certain ACEIs has also been associated with positive health effects beyond the regulation of blood pressure [97]. Polyphenols inhibit and down-regulate expression of ACE and renin [98]. Tomato juice was earlier shown to lower blood pressure in human volunteers, and this effect was thought to be associated with its high antioxidant content [99, 100]. We therefore tested whether Fruitflow® inhibited human serum ACE activity and rabbit lung ACE activity [17]. The IC50 value of Fruitflow® for ACE inhibition in serum was 1.91 ± 0.24 mg/ml (0.038 μg catechin equivalent(CE)/ml), whereas for captopril, the value was 0.56 ± 0.08 μg/ml. Fruitflow® also inhibited rabbit lung ACE activity in a dose-dependent manner. Orange or banana extract had no such anti-ACE activity. Flavonoid-rich plant extracts have been demonstrated as natural competitive ACEIs where the ACE activity is identified as a critical factor in regulating high blood pressure. These compounds are known to be inhibitors of cyclic nucleotide phosphodiesterase and TxA2 synthesis, two main determining factors in human blood platelet activation/aggregation processes. Consequently, it is possible that the consumption of these bioactive components of Fruitflow® might reduce more than one CVD risk factor, such as platelet hyperactivity and hypertension. As yet, these data are based on in vitro experiments, and it is clear that further work is required to provide clear information on the metabolic fate of these compounds, and the dosage required for physiological benefits. While a functional food approach offers interesting possibilities for cardio-protection, the requirement for long-term randomized controlled trials remains. Advances in the knowledge of both platelet biology and the mechanism of action of Fruitflow® bioactive compounds will provide new avenues to develop dietary strategies aimed at promoting cardiovascular health.
Fruitflow® and other platelet inhibiting food ingredients
Nutritional modification of cellular functions by dietary lipids and other nutritive and non-nutritive factors offers an attractive avenue to correct, modify or prevent many pathophysiological processes including platelet hyperactivity [101]. The mediation of such effects is thought to be primarily achieved through alterations of cell membrane composition and other endogenous lipid stores, with a consequent reduction in AA-derived eicosanoid production and modification of the functional activity of various receptors on platelet membranes [101]. Eicosapentaenoic acid, 20:5n-3 (EPA) and DHA substitute biologically less potent eicosanoids, while the non-nutritive compounds act to reduce all eicosanoid formation specially TxA2, an important platelet-aggregating agent. Numerous epidemiological studies and clinical trials have reported the health benefits of different omega 3 polyunsaturated fatty acids (PUFAs), including a lower risk of coronary heart diseases [102]. There are several reviews available on the effects of alpha-linolenic (ALA), EPA and docosahexaenoic, 22:6n-3 (DHA) acids on some risk factors associated with atherothrombosis, including platelet activation, plasma lipid concentrations and oxidative modification of LDL [102, 103]. The role of platelets in haemostasis and thrombosis has been known for a long time and is well defined, but more recently a new concept has emerged stating that platelets play a central role in the atherothrombotic process [9, 10]. Dyerberg and Bang showed that Inuits had attenuated platelet reactivity [104] as they consumed omega 3 fatty acids. Platelet aggregation response was diminished with omega 3 fatty acids consumption [105–107]. A meta-analysis conducted by Gao et al. [108] has demonstrated that omega 3 PUFAs are associated with a significant reduction in platelet aggregation. In addition, low intake of EPA may reduce platelet aggregation, without changing the fatty acid platelet composition [109, 110]. In the same way, following supplementation with DHA [111] platelet function was reduced and a retroconversion of DHA into DPA and EPA was evidenced. More recently, a dose–response study with middle-aged healthy volunteers ingesting increasing amounts of DHA indicated that platelet reactivity was decreased after 400 and 800 mg DHA/day [112]. It is difficult to attribute precisely the effects to each fatty acid, and their beneficial and complementary effects could well be linked to formation or diminution of specific eicosanoids and/or docosanoids.
Combinations of antiplatelet drugs are known to have different physiological effects than single agents. Taking a similar strategy from a functional food perspective, a combination of tomato extract with antiplatelet activity [13] and n-3 fatty acids was investigated for effects on platelet aggregation in vitro. The combination of tomato extract and omega 3 fatty acids inhibited in vitro platelet aggregation to a greater extent than either alone, and this inhibition was correlated with intracellular platelet cAMP levels [113]. Such data indicate that combinations of Fruitflow® and omega 3 fatty acids—and potentially other non-nutritive compounds such as resveratrol and other polyphenols—may be effective in improving platelet function. Further human intervention studies should be conducted in order to determine the scale of benefits which may arise following consumption of Fruitflow® combined with other bioactive substances.
Conclusions
This review provides information that substantiates the cardio-protective claims of Fruitflow®. Normal platelet activity is the key for the maintenance of haemostasis and normal blood flow. Hyperactive platelets interact with vessel walls by shedding macro-particles, secreting several adhesive growth factors, and inflammatory agents interrupt the blood flow and produce a pro-thrombotic state in people with obesity, diabetes, a sedentary lifestyle or hypertension, and in people who smoke. In general, the molecular events underpinning these processes are broadly similar. It has long been known that disturbances in blood flow, changes in platelet reactivity and enhanced coagulation reactions facilitate pathological thrombus formation, and the maintenance of normal platelet activity is critical to overall haemostasis. Fruitflow® developed from tomato containing bioavailable cardio-protective compounds can be of benefit to the people who are vulnerable to develop CVD. The outlined data suggest that Fruitflow® may be useful in the primary prevention of CVD. An array of extensive basic, mechanistic, compositional and several human trials are testimony to its cardio-protective benefits.
Abbreviations
- CVD:
-
Cardiovascular disease
- tAF:
-
Total active fraction
- ACE:
-
Angiotensin-converting enzyme
- EPA:
-
Eicosapentaenoic acid, 20:5n-3
- TRAP:
-
Thrombin receptor-activating peptide
- DHA:
-
Docosahexaenoic, 22:6n-3
- WSTC:
-
Water-soluble tomato concentrate
- EFSA:
-
European Food Safety Authority
- PDI:
-
Protein disulphide isomerase
- TF:
-
Tissue factor
- PRP:
-
Platelet-rich plasma
- VSMC:
-
Vascular smooth muscle cells
- TxA2 :
-
Thromboxane A2
References
Canene-Adams K, Campbell JK, Zaripheh S, Jeffery EH, Erdman JW Jr (2005) The tomato as a functional food. J Nutr 135(5):1226–1230
Agarwal S, Rao AV (2000) Tomato lycopene and its role in human health and chronic diseases. CMAJ : Canadian Medical Association journal 163(6):739–744
Jacques PF, Lyass A, Massaro JM, Vasan RS, D’Agostino RB Sr (2013) Relationship of lycopene intake and consumption of tomato products to incident CVD. Br J Nutr. doi:10.1017/S0007114512005417
Weisburger JH (2002) Lycopene and tomato products in health promotion. Exp Biol Med (Maywood) 227(10):924–927
Willcox JK, Catignani GL, Lazarus S (2003) Tomatoes and cardiovascular health. Crit Rev Food Sci Nutr 43(1):1–18. doi:10.1080/10408690390826437
Garcia-Alonso FJ, Jorge-Vidal V, Ros G, Periago MJ (2012) Effect of consumption of tomato juice enriched with n-3 polyunsaturated fatty acids on the lipid profile, antioxidant biomarker status, and cardiovascular disease risk in healthy women. Eur J Nutr 51(4):415–424. doi:10.1007/s00394-011-0225-0
Muller I, Massberg S, Zierhut W, Binz C, Schuster A, Rudiger-von Hoch S, Braun S, Gawaz M (2002) Effects of aspirin and clopidogrel versus oral anticoagulation on platelet function and on coagulation in patients with nonvalvular atrial fibrillation (CLAFIB). Pathophysiol Haemost Thromb 32(1):16–24
Natarajan A, Zaman AG, Marshall SM (2008) Platelet hyperactivity in type 2 diabetes: role of antiplatelet agents. Diabetes Vasc Dis Res 5(2):138–144. doi:10.3132/dvdr.2008.023
Massberg S, Brand K, Gruner S, Page S, Muller E, Muller I, Bergmeier W, Richter T, Lorenz M, Konrad I, Nieswandt B, Gawaz M (2002) A critical role of platelet adhesion in the initiation of atherosclerotic lesion formation. J Exp Med 196(7):887–896
Kaplan ZS, Jackson SP (2011) The role of platelets in atherothrombosis. Hematol Am Soc Hematol Educ Prog 2011:51–61. doi:10.1182/asheducation-2011.1.51
Cai G, Zhou W, Lu Y, Chen P, Lu Z, Fu Y (2016) Aspirin resistance and other aspirin-related concerns. Neurol Sci 37(2):181–189. doi:10.1007/s10072-015-2412-x
Hennekens CH, Dalen JE (2014) Aspirin in the primary prevention of cardiovascular disease: current knowledge and future research needs. Trends Cardiovasc Med 24(8):360–366. doi:10.1016/j.tcm.2014.08.006
Dutta-Roy AK, Crosbie L, Gordon MJ (2001) Effects of tomato extract on human platelet aggregation in vitro. Platelets 12(4):218–227. doi:10.1080/09537100120058757
O’Kennedy N, Crosbie L, Song V, Broom JI, Webb DJ, Duttaroy AK (2006) Potential for use of lycopene-free tomato extracts as dietary antiplatelet agents. Atherosclerosis 188(1):S9–S9
O’Kennedy N, Crosbie L, van Lieshout M, Broom JI, Webb DJ, Duttaroy AK (2006) Effects of antiplatelet components of tomato extract on platelet function in vitro and ex vivo: a time-course cannulation study in healthy humans. Am J Clin Nutr 84(3):570–579
O’Kennedy N, Crosbie L, Whelan S, Luther V, Horgan G, Broom JI, Webb DJ, Duttaroy AK (2006) Effects of tomato extract on platelet function: a double-blinded crossover study in healthy humans. Am J Clin Nutr 84(3):561–569
Biswas D, Uddin MM, Dizdarevic LL, Jorgensen A, Duttaroy AK (2014) Inhibition of angiotensin-converting enzyme by aqueous extract of tomato. Eur J Nutr. doi:10.1007/s00394-014-0676-1
Schwager J, Richard N, Mussler B, Raedestroff D (2016) Tomato extract modulates the inflammatory profile of immune cells and endothelial cells. Molecul 21(2):168. doi:10.3390/molecules21020168
Giovannucci E (1999) Tomatoes, tomato-based products, lycopene, and cancer: review of the epidemiologic literature. J Natl Cancer Inst 91(4):317–331
Giovannucci E (1999) RESPONSE: re: tomatoes, tomato-based products, lycopene, and prostate cancer: review of the epidemiologic literature. J Natl Cancer Inst 91(15):1331A–1331
Giovannucci E (2002) A review of epidemiologic studies of tomatoes, lycopene, and prostate cancer. Exp Biol Med (Maywood) 227(10):852–859
Giovannucci E, Rimm EB, Liu Y, Stampfer MJ, Willett WC (2002) A prospective study of tomato products, lycopene, and prostate cancer risk. J Natl Cancer Inst 94(5):391–398
Rissanen TH, Voutilainen S, Nyyssonen K, Salonen R, Kaplan GA, Salonen JT (2003) Serum lycopene concentrations and carotid atherosclerosis: the Kuopio Ischaemic Heart Disease Risk Factor Study. Am J Clin Nutr 77(1):133–138
Ried K, Fakler P (2011) Protective effect of lycopene on serum cholesterol and blood pressure: meta-analyses of intervention trials. Maturitas 68(4):299–310. doi:10.1016/j.maturitas.2010.11.018
Rissanen T, Voutilainen S, Nyyssonen K, Salonen R, Salonen JT (2000) Low plasma lycopene concentration is associated with increased intima-media thickness of the carotid artery wall. Arterioscler Thromb Vasc Biol 20(12):2677–2681
Kohlmeier L, Kark JD, Gomez-Gracia E, Martin BC, Steck SE, Kardinaal AF, Ringstad J, Thamm M, Masaev V, Riemersma R, Martin-Moreno JM, Huttunen JK, Kok FJ (1997) Lycopene and myocardial infarction risk in the EURAMIC Study. Am J Epidemiol 146(8):618–626
Paterson E, Gordon MH, Niwat C, George TW, Parr L, Waroonphan S, Lovegrove JA (2006) Supplementation with fruit and vegetable soups and beverages increases plasma carotenoid concentrations but does not alter markers of oxidative stress or cardiovascular risk factors. J Nutr 136(11):2849–2855
Sesso HD, Buring JE, Norkus EP, Gaziano JM (2005) Plasma lycopene, other carotenoids, and retinol and the risk of cardiovascular disease in men. Am J Clin Nutr 81(5):990–997
Hak AE, Ma J, Powell CB, Campos H, Gaziano JM, Willett WC, Stampfer MJ (2004) Prospective study of plasma carotenoids and tocopherols in relation to risk of ischemic stroke. Stroke 35(7):1584–1588. doi:10.1161/01.STR.0000132197.67350.bd
Ito Y, Kurata M, Suzuki K, Hamajima N, Hishida H, Aoki K (2006) Cardiovascular disease mortality and serum carotenoid levels: a Japanese population-based follow-up study. J Epidemiol 16(4):154–160
Street DA, Comstock GW, Salkeld RM, Schuep W, Klag MJ (1994) Serum antioxidants and myocardial infarction. Are low levels of carotenoids and alpha-tocopherol risk factors for myocardial infarction? Circulation 90(3):1154–1161
Tavani A, Gallus S, Negri E, Parpinel M, La Vecchia C (2006) Dietary intake of carotenoids and retinol and the risk of acute myocardial infarction in Italy. Free Radic Res 40(6):659–664. doi:10.1080/10715760600615649
Sesso HD, Liu S, Gaziano JM, Buring JE (2003) Dietary lycopene, tomato-based food products and cardiovascular disease in women. J Nutr 133(7):2336–2341
Osganian SK, Stampfer MJ, Rimm E, Spiegelman D, Manson JE, Willett WC (2003) Dietary carotenoids and risk of coronary artery disease in women. Am J Clin Nutr 77(6):1390–1399
Ascherio A, Rimm EB, Hernan MA, Giovannucci E, Kawachi I, Stampfer MJ, Willett WC (1999) Relation of consumption of vitamin E, vitamin C, and carotenoids to risk for stroke among men in the United States. Ann Intern Med 130(12):963–970
Hirvonen T, Virtamo J, Korhonen P, Albanes D, Pietinen P (2000) Intake of flavonoids, carotenoids, vitamins C and E, and risk of stroke in male smokers. Stroke 31(10):2301–2306
Agarwal S, Rao AV (1998) Tomato lycopene and low density lipoprotein oxidation: a human dietary intervention study. Lipids 33(10):981–984
Rissanen T, Voutilainen S, Nyyssonen K, Salonen JT (2002) Lycopene, atherosclerosis, and coronary heart disease. Exp Biol Med (Maywood) 227(10):900–907
Ribeiro AB, Chiste RC, Lima JL, Fernandes E (2016) Solanum diploconos fruits: profile of bioactive compounds and in vitro antioxidant capacity of different parts of the fruit. Food Funct 7(5):2249–2257. doi:10.1039/c6fo00326e
Hwang ES, Stacewicz-Sapuntzakis M, Bowen PE (2012) Effects of heat treatment on the carotenoid and tocopherol composition of tomato. J Food Sci 77(10):C1109–1114. doi:10.1111/j.1750-3841.2012.02909.x
Kim YI, Hirai S, Goto T, Ohyane C, Takahashi H, Tsugane T, Konishi C, Fujii T, Inai S, Iijima Y, Aoki K, Shibata D, Takahashi N, Kawada T (2012) Potent PPARalpha activator derived from tomato juice, 13-oxo-9,11-octadecadienoic acid, decreases plasma and hepatic triglyceride in obese diabetic mice. PLoS ONE 7(2):e31317. doi:10.1371/journal.pone.0031317
Nohara T, Ono M, Ikeda T, Fujiwara Y, El-Aasr M (2010) The tomato saponin, esculeoside a. J Nat Prod 73(10):1734–1741. doi:10.1021/np100311t
Davi G, Patrono C (2007) Platelet activation and atherothrombosis. N Engl J Med 357(24):2482–2494. doi:10.1056/NEJMra071014
Thomas DP (1967) Effect of catecholamines on platelet aggregation caused by thrombin. Nature 215(5098):298–299
Blajchman MA, Senyi AF, Hirsh J, Genton E, George JN (1981) Hemostatic function, survival, and membrane glycoprotein changes in young versus old rabbit platelets. J Clin Investig 68(5):1289–1294
Tran H, Anand SS (2004) Oral antiplatelet therapy in cerebrovascular disease, coronary artery disease, and peripheral arterial disease. JAMA 292(15):1867–1874. doi:10.1001/jama.292.15.1867
Fuster V, Chesebro JH (1986) Mechanisms of unstable angina. N Engl J Med 315(16):1023–1025. doi:10.1056/NEJM198610163151608
Dai Y, Ge J (2012) Clinical use of aspirin in treatment and prevention of cardiovascular disease. Thrombosis 2012:245037. doi:10.1155/2012/245037
Sarbacker GB, Lusk KA, Flieller LA, Van Liew JR (2016) Aspirin use for the primary prevention of cardiovascular disease in the elderly. Consult Pharm 31(1):24–32. doi:10.4140/TCP.n.2016.24
Duhamel TA, Xu YJ, Arneja AS, Dhalla NS (2007) Targeting platelets for prevention and treatment of cardiovascular disease. Expert Opin Ther Targets 11(12):1523–1533. doi:10.1517/14728222.11.12.1523
Mohle R, Green D, Moore MA, Nachman RL, Rafii S (1997) Constitutive production and thrombin-induced release of vascular endothelial growth factor by human megakaryocytes and platelets. Proc Natl Acad Sci USA 94(2):663–668
Nadar SK, Blann AD, Lip GY (2004) Plasma and platelet-derived vascular endothelial growth factor and angiopoietin-1 in hypertension: effects of antihypertensive therapy. J Intern Med 256(4):331–337. doi:10.1111/j.1365-2796.2004.01367.x
Holmsen H (1985) Platelet metabolism and activation. Semin Hematol 22(3):219–240
Touyz RM, Schiffrin EL (1993) Effects of angiotensin II and endothelin-1 on platelet aggregation and cytosolic pH and free Ca2 + concentrations in essential hypertension. Hypertension 22(6):853–862
Pechan J, Okrucka A (1991) Diltiazem inhibits the spontaneous platelet aggregation in essential hypertension. Cardiology 79(2):116–119
Andrioli G, Ortolani R, Fontana L, Gaino S, Bellavite P, Lechi C, Minuz P, Manzato F, Tridente G, Lechi A (1996) Study of platelet adhesion in patients with uncomplicated hypertension. J Hypertens 14(10):1215–1221
Kjeldsen SE, Gjesdal K, Eide I, Aakesson I, Amundsen R, Foss OP, Leren P (1983) Increased beta-thromboglobulin in essential hypertension: interactions between arterial plasma adrenaline, platelet function and blood lipids. Acta Med Scand 213(5):369–373
Oshima T, Matsuura H, Matsumoto K, Kido K, Kajiyama G (1988) Role of cellular calcium in salt sensitivity of patients with essential hypertension. Hypertension 11(6 Pt 2):703–707
Fuentes E, Rojas A, Palomo I (2016) NF-kappaB signaling pathway as target for antiplatelet activity. Blood Rev. doi:10.1016/j.blre.2016.03.002
Ferroni P, Martini F, D’Alessandro R, Magnapera A, Raparelli V, Scarno A, Davi G, Basili S, Guadagni F (2008) In vivo platelet activation is responsible for enhanced vascular endothelial growth factor levels in hypertensive patients. Clin Chim Acta Int J Clin Chem 388(1–2):33–37. doi:10.1016/j.cca.2007.09.026
Cho J (2013) Protein disulfide isomerase in thrombosis and vascular inflammation. J Thromb Haemost 11(12):2084–2091. doi:10.1111/jth.12413
Manickam N, Sun X, Li M, Gazitt Y, Essex DW (2008) Protein disulphide isomerase in platelet function. Br J Haematol 140(2):223–229. doi:10.1111/j.1365-2141.2007.06898.x
Jordan PA, Stevens JM, Hubbard GP, Barrett NE, Sage T, Authi KS, Gibbins JM (2005) A role for the thiol isomerase protein ERP5 in platelet function. Blood 105(4):1500–1507. doi:10.1182/blood-2004-02-0608
Jasuja R, Passam FH, Kennedy DR, Kim SH, van Hessem L, Lin L, Bowley SR, Joshi SS, Dilks JR, Furie B, Furie BC, Flaumenhaft R (2012) Protein disulfide isomerase inhibitors constitute a new class of antithrombotic agents. J Clin Investig 122(6):2104–2113. doi:10.1172/JCI61228
Sheu JR, Hsiao G, Chou PH, Shen MY, Chou DS (2004) Mechanisms involved in the antiplatelet activity of rutin, a glycoside of the flavonol quercetin, in human platelets. J Agric Food Chem 52(14):4414–4418. doi:10.1021/jf040059f
O’Kennedy N, Crosbie L, van Lieshout M, Broom JI, Webb DJ, Duttaroy AK (2006) Effects of antiplatelet components of tomato extract on platelet function in vitro and ex vivo: a time-course cannulation study in healthy humans. Am J Clin Nutr 84(3):570–579
Fuentes E, Castro R, Astudillo L, Carrasco G, Alarcon M, Gutierrez M, Palomo I (2012) Bioassay-guided isolation and HPLC determination of bioactive compound that relate to the antiplatelet activity (adhesion, secretion, and aggregation) from solanum lycopersicum. Evid Based Complement Alternat Med 2012:147031. doi:10.1155/2012/147031
O’Kennedy N, Crosbie L, Whelan S, Luther V, Horgan G, Broom JI, Webb DJ, Duttaroy AK (2006) Effects of tomato extract on platelet function: a double-blinded crossover study in healthy humans. Am J Clin Nutr 84(3):561–569
George MM, Copeland KC (2013) Current treatment options for type 2 diabetes mellitus in youth: today’s realities and lessons from the TODAY study. Curr Diab Rep 13(1):72–80. doi:10.1007/s11892-012-0334-z
Libby P (2002) Inflammation in atherosclerosis. Nature 420(6917):868–874. doi:10.1038/nature01323
Viola J, Soehnlein O (2015) Atherosclerosis—a matter of unresolved inflammation. Semin in Immunol 27(3):184–193. doi:10.1016/j.smim.2015.03.013
Conti P, Shaik-Dasthagirisaeb Y (2015) Atherosclerosis: a chronic inflammatory disease mediated by mast cells. Central-European journal of immunology / Polish Society for Immunology and eleven other Central-European immunological societies 40(3):380–386. doi:10.5114/ceji.2015.54603
Raiola A, Rigano MM, Calafiore R (2014) Enhancing the health-promoting effects of tomato fruit for biofortified food. 2014:139873. doi:10.1155/2014/139873
Ghavipour M, Saedisomeolia A, Djalali M, Sotoudeh G, Eshraghyan MR, Moghadam AM, Wood LG (2013) Tomato juice consumption reduces systemic inflammation in overweight and obese females. Br J Nutr 109(11):2031–2035. doi:10.1017/s0007114512004278
Ghavipour M, Sotoudeh G, Ghorbani M (2015) Tomato juice consumption improves blood antioxidative biomarkers in overweight and obese females. Clin Nutr (Edinburgh, Scotland) 34(5):805–809. doi:10.1016/j.clnu.2014.10.012
Tsitsimpikou C, Tsarouhas K, Kioukia-Fougia N, Skondra C, Fragkiadaki P, Papalexis P, Stamatopoulos P, Kaplanis I, Hayes AW, Tsatsakis A, Rentoukas E (2014) Dietary supplementation with tomato-juice in patients with metabolic syndrome: a suggestion to alleviate detrimental clinical factors. Food Chem Toxicol 74:9–13. doi:10.1016/j.fct.2014.08.014
Burton-Freeman B, Talbot J, Park E, Krishnankutty S, Edirisinghe I (2012) Protective activity of processed tomato products on postprandial oxidation and inflammation: a clinical trial in healthy weight men and women. Mol Nutr Food Res 56(4):622–631. doi:10.1002/mnfr.201100649
Vilahur G, Cubedo J, Padro T, Casani L, Mendieta G, Gonzalez A, Badimon L (2015) Intake of cooked tomato sauce preserves coronary endothelial function and improves apolipoprotein A-I and apolipoprotein J protein profile in high-density lipoproteins. Transl Res J Lab Clin Med 166(1):44–56. doi:10.1016/j.trsl.2014.11.004
Navarrete S, Alarcon M, Palomo I (2015) Aqueous extract of tomato (Solanum lycopersicum L.) and ferulic acid reduce the expression of TNF-alpha and IL-1beta in LPS-activated macrophages. Molecules (Basel, Switzerland) 20(8):15319–15329. doi:10.3390/molecules200815319
Fotis L, Giannakopoulos D, Stamogiannou L, Xatzipsalti M (2012) Intercellular cell adhesion molecule-1 and vascular cell adhesion molecule-1 in children. Do they play a role in the progression of atherosclerosis? Hormones (Athens, Greece) 11(2):140–146
Hasko G, Cronstein B (2013) Regulation of inflammation by adenosine. Front Immunol 4:85. doi:10.3389/fimmu.2013.00085
Hasko G, Linden J, Cronstein B, Pacher P (2008) Adenosine receptors: therapeutic aspects for inflammatory and immune diseases. Nat Rev Drug Discov 7(9):759–770. doi:10.1038/nrd2638
Hasko G, Kuhel DG, Chen JF, Schwarzschild MA, Deitch EA, Mabley JG, Marton A, Szabo C (2000) Adenosine inhibits IL-12 and TNF-[alpha] production via adenosine A2a receptor-dependent and independent mechanisms. FASEB J 14(13):2065–2074. doi:10.1096/fj.99-0508com
Nemeth ZH, Lutz CS, Csoka B, Deitch EA, Leibovich SJ, Gause WC, Tone M, Pacher P, Vizi ES, Hasko G (2005) Adenosine augments IL-10 production by macrophages through an A2B receptor-mediated posttranscriptional mechanism. J Immunol (Baltimore, Md : 1950) 175(12):8260–8270
Shan J, Fu J, Zhao Z, Kong X, Huang H, Luo L, Yin Z (2009) Chlorogenic acid inhibits lipopolysaccharide-induced cyclooxygenase-2 expression in RAW264.7 cells through suppressing NF-kappaB and JNK/AP-1 activation. Int Immunopharmacol 9(9):1042–1048. doi:10.1016/j.intimp.2009.04.011
Shi H, Dong L, Jiang J, Zhao J, Zhao G, Dang X, Lu X, Jia M (2013) Chlorogenic acid reduces liver inflammation and fibrosis through inhibition of toll-like receptor 4 signaling pathway. Toxicology 303:107–114. doi:10.1016/j.tox.2012.10.025
Gao M, Ma Y, Liu D (2013) Rutin suppresses palmitic acids-triggered inflammation in macrophages and blocks high fat diet-induced obesity and fatty liver in mice. Pharm Res 30(11):2940–2950. doi:10.1007/s11095-013-1125-1
Wu CH, Wu CF, Huang HW, Jao YC, Yen GC (2009) Naturally occurring flavonoids attenuate high glucose-induced expression of proinflammatory cytokines in human monocytic THP-1 cells. Mol Nutr Food Res 53(8):984–995. doi:10.1002/mnfr.200800495
Lee W, Ku SK, Bae JS (2012) Barrier protective effects of rutin in LPS-induced inflammation in vitro and in vivo. Food Chem Toxicol 50(9):3048–3055. doi:10.1016/j.fct.2012.06.013
Ezzati M, Lopez AD, Rodgers A, Vander Hoorn S, Murray CJ (2002) Selected major risk factors and global and regional burden of disease. Lancet 360(9343):1347–1360. doi:10.1016/S0140-6736(02)11403-6
Griendling KK, Tsuda T, Berk BC, Alexander RW (1989) Angiotensin II stimulation of vascular smooth muscle cells. Secondary signalling mechanisms. Am J Hypertens 2(8):659–665
Boustany CM, Bharadwaj K, Daugherty A, Brown DR, Randall DC, Cassis LA (2004) Activation of the systemic and adipose renin-angiotensin system in rats with diet-induced obesity and hypertension. Am J Physiol Regul Integr Comp Physiol 287(4):R943–949. doi:10.1152/ajpregu.00265.2004
Winter KH, Tuttle LA, Viera AJ (2013) Hypertension. Prim Care 40(1):179–194. doi:10.1016/j.pop.2012.11.008
Law MR, Morris JK, Wald NJ (2009) Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ 338:b1665. doi:10.1136/bmj.b1665
Alderman MH, Madhavan S, Ooi WL, Cohen H, Sealey JE, Laragh JH (1991) Association of the renin-sodium profile with the risk of myocardial infarction in patients with hypertension. N Engl J Med 324(16):1098–1104. doi:10.1056/NEJM199104183241605
Pfeffer MA, Braunwald E, Moye LA, Basta L, Brown EJ Jr, Cuddy TE, Davis BR, Geltman EM, Goldman S, Flaker GC et al (1992) Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. Results of the survival and ventricular enlargement trial. The SAVE Investigators. N Engl J Med 327(10):669–677. doi:10.1056/NEJM199209033271001
Schiffrin EL (2002) Vascular and cardiac benefits of angiotensin receptor blockers. Am J Med 113(5):409–418
Huang WY, Davidge ST, Wu J (2013) Bioactive natural constituents from food sources-potential use in hypertension prevention and treatment. Crit Rev Food Sci Nutr 53(6):615–630. doi:10.1080/10408398.2010.550071
Engelhard YN, Gazer B, Paran E (2006) Natural antioxidants from tomato extract reduce blood pressure in patients with grade-1 hypertension: a double-blind, placebo-controlled pilot study. Am Heart J 151(1):100. doi:10.1016/j.ahj.2005.05.008
Ried K, Frank OR, Stocks NP (2009) Dark chocolate or tomato extract for prehypertension: a randomised controlled trial. BMC Complement Altern Med 9:22. doi:10.1186/1472-6882-9-22
Dutta-Roy AK (2002) Dietary components and human platelet activity. Platelets 13(2):67–75. doi:10.1080/09537100120111540
McEwen BJ, Morel-Kopp MC, Tofler GH, Ward CM (2015) The effect of omega-3 polyunsaturated fatty acids on fibrin and thrombin generation in healthy subjects and subjects with cardiovascular disease. Semin Thromb Hemost 41(3):315–322. doi:10.1055/s-0034-1395352
Massaro M, Scoditti E, Carluccio MA, Campana MC, De Caterina R (2010) Omega-3 fatty acids, inflammation and angiogenesis: basic mechanisms behind the cardioprotective effects of fish and fish oils. Cell Mol Biol (Noisy-le-grand) 56(1):59–82
Dyerberg J, Bang HO, Hjorne N (1975) Fatty acid composition of the plasma lipids in Greenland Eskimos. Am J Clin Nutr 28(9):958–966
Nelson GJ, Schmidt PC, Bartolini G, Kelley DS, Kyle D (1997) The effect of dietary arachidonic acid on platelet function, platelet fatty acid composition, and blood coagulation in humans. Lipids 32(4):421–425
Siess W, Roth P, Scherer B, Kurzmann I, Bohlig B, Weber PC (1980) Platelet-membrane fatty acids, platelet aggregation, and thromboxane formation during a mackerel diet. Lancet 1(8166):441–444
Phang M, Lincz LF, Garg ML (2013) Eicosapentaenoic and docosahexaenoic acid supplementations reduce platelet aggregation and hemostatic markers differentially in men and women. J Nutr 143(4):457–463. doi:10.3945/jn.112.171249
Gao LG, Cao J, Mao QX, Lu XC, Zhou XL, Fan L (2013) Influence of omega-3 polyunsaturated fatty acid-supplementation on platelet aggregation in humans: a meta-analysis of randomized controlled trials. Atherosclerosis 226(2):328–334. doi:10.1016/j.atherosclerosis.2012.10.056
Driss F, Vericel E, Lagarde M, Dechavanne M, Darcet P (1984) Inhibition of platelet aggregation and thromboxane synthesis after intake of small amount of icosapentaenoic acid. Thromb Res 36(5):389–396
Croset M, Vericel E, Rigaud M, Hanss M, Courpron P, Dechavanne M, Lagarde M (1990) Functions and tocopherol content of blood platelets from elderly people after low intake of purified eicosapentaenoic acid. Thromb Res 57(1):1–12
von Schacky C, Weber PC (1985) Metabolism and effects on platelet function of the purified eicosapentaenoic and docosahexaenoic acids in humans. J Clin Investig 76(6):2446–2450. doi:10.1172/JCI112261
Guillot N, Caillet E, Laville M, Calzada C, Lagarde M, Vericel E (2009) Increasing intakes of the long-chain omega-3 docosahexaenoic acid: effects on platelet functions and redox status in healthy men. FASEB J 23(9):2909–2916. doi:10.1096/fj.09-133421
Lazarus SA, Garg ML (2003) The effects of tomato extract (TE) and omega-3 fatty acids on platelet cAMP levels and inositol triphosphate (IP(3)) release. Asia Pac J Clin Nutr 12(Suppl):S20
Acknowledgments
We appreciate very much the insightful and critical comments by Ruedi Duss, Bernd Mussler and Ian Ford.
Contributions of authors
All authors NOK, DR and ADR undertook systematic review and wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ADR is a Professor at the University of Oslo and a member of Provexis plc’s Scientific Advisory Board, and he was the original inventor of Fruitflow®. NOK was an employee of Provexis plc, and she remains a consultant to the company and a member of its Scientific Advisory Board; NOK was closely involved in the development work for Fruitflow® including compositional analysis and human intervention studies, and she prepared documents for the dossier submitted to EFSA which resulted in the EU authorized health claim for Fruitflow®. DR is a principal scientist at DSM, and he is involved in an investigation of the effects of Fruitflow® on the inflammatory response of macrophages and on endothelial dysfunction. There are no other competing interests.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
O’Kennedy, N., Raederstorff, D. & Duttaroy, A.K. Fruitflow®: the first European Food Safety Authority-approved natural cardio-protective functional ingredient. Eur J Nutr 56, 461–482 (2017). https://doi.org/10.1007/s00394-016-1265-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-016-1265-2