Abstract
Objectives
To determine whether apparent diffusion coefficient (ADC) ratio aids reliable interpretation of diffusion-weighted imaging (DWI) for prostate cancer (PCa).
Methods
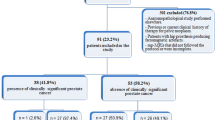
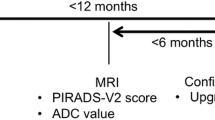
Seventy-six consecutive patients with PCa who underwent DWI and surgery were included. Based on pathologic tumour location, two readers independently performed DWI scoring according to the revised Prostate Imaging Reporting and Data System (PI-RADSv2). ADC ratios of benign to cancerous prostatic tissue were then measured independently and compared between cases showing concordant and discordant DWI scores ≥4. Area under the curve (AUC) and threshold of ADC ratio were analyzed for DWI scores ≥4.
Results
The rate of inter-reader disagreement for DWI score ≥4 was 11.8% (9/76). ADC ratios were higher in concordant vs. discordant DWI scores ≥4 (median, 1.7 vs. 1.1–1.2; p < 0.001). For DWI scores ≥4, the AUCs of ADC ratios were 0.970 for reader 1 and 0.959 for reader 2. In patients with an ADC ratio >1.3, the rate of inter-reader disagreement for DWI score ≥4 decreased to 5.9–6.0%. An ADC ratio >1.3 yielded 100% (reader 1, 54/54; reader 2, 51/51) positive predictive value for clinically significant cancer.
Conclusion
ADC ratios may be useful for reliable interpretation of DWI score ≥4 in PI-RADSv2.
Key points
• The ADC ratio correlated positively with DWI score of PI-RADSv2.
• ADC ratio >1.3 was associated with concordant interpretation of DWI score ≥4.
• ADC ratio >1.3 was associated with high PPV for clinically significant cancer.
• ADC ratio is useful for reliable interpretation of DWI scoring in PI-RADSv2.





Similar content being viewed by others
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- PI-RADSv2:
-
Prostate Imaging Reporting and Data System version 2
- DWI:
-
Diffusion-weighted imaging
- DCE:
-
Dynamic contrast-enhanced
- MR:
-
Magnetic resonance
- TR:
-
Repetition time
- TE:
-
Echo time
- PCa:
-
Prostate cancer
- CSC:
-
Clinically significant cancer
- PZ:
-
Peripheral zone
- TZ:
-
Transition zone
- ECE:
-
Extracapsular extension
- SVI:
-
Seminal vesicle invasion
- ROI:
-
Region of interest
- ROC:
-
Receiver operating-characteristic
- AUC:
-
Area under the curve
- PPV:
-
Positive predictive value
- CI:
-
confidence interval
- PSA:
-
Prostate-specific antigen
- GS:
-
Gleason score
References
Park SY, Jung DC, Oh YT et al (2016) Prostate cancer: PI-RADS version 2 helps preoperatively predict clinically significant cancers. Radiology. doi:10.1148/radiol.16151133:151133
Kayat Bittencourt L, Litjens G, Hulsbergen-van de Kaa CA, Turkbey B, Gasparetto EL, Barentsz JO (2015) Prostate cancer: the european society of urogenital radiology prostate imaging reporting and data system criteria for predicting extraprostatic extension by using 3-T multiparametric MR imaging. Radiology 276:479–489
Washino S, Okochi T, Saito K et al (2016) Combination of PI-RADS score and PSA density predicts biopsy outcome in biopsy naive patients. BJU Int. doi:10.1111/bju.13465
Woo S, Kim SY, Lee J, Kim SH, Cho JY (2016) PI-RADS version 2 for prediction of pathological downgrading after radical prostatectomy: a preliminary study in patients with biopsy-proven Gleason Score 7 (3 + 4) prostate cancer.. doi:10.1007/s00330-016-4230-9, Eur Radiol
Vargas HA, Hotker AM, Goldman DA et al (2016) Updated prostate imaging reporting and data system (PIRADS v2) recommendations for the detection of clinically significant prostate cancer using multiparametric MRI: critical evaluation using whole-mount pathology as standard of reference. Eur Radiol 26:1606–1612
Rosenkrantz AB, Ginocchio LA, Cornfeld D et al (2016) Interobserver reproducibility of the PI-RADS version 2 lexicon: a multicenter study of six experienced prostate radiologists. Radiology. doi:10.1148/radiol.2016152542:152542
Muller BG, Shih JH, Sankineni S et al (2015) Prostate cancer: interobserver agreement and accuracy with the revised prostate imaging reporting and data system at multiparametric MR imaging. Radiology 277:741–750
Barentsz JO, Weinreb JC, Verma S et al (2016) Synopsis of the PI-RADS v2 guidelines for multiparametric prostate magnetic resonance imaging and recommendations for use. Eur Urol 69:41–49
Rosenkrantz AB, Margolis DJ (2016) Commentary regarding the inter-reader reproducibility of PI-RADS version 2. Abdom Radiol (NY) 41:907–909
Sasaki M, Ida M, Yamada K, Watanabe Y, Matsui M (2007) Standardizing display conditions of diffusion-weighted images using concurrent b0 images: a multi-vendor multi-institutional study. Magn Reson Med Sci 6:133–137
Kivrak AS, Paksoy Y, Erol C, Koplay M, Ozbek S, Kara F (2013) Comparison of apparent diffusion coefficient values among different MRI platforms: a multicenter phantom study. Diagn Interv Radiol 19:433–437
Sasaki M, Yamada K, Watanabe Y et al (2008) Variability in absolute apparent diffusion coefficient values across different platforms may be substantial: a multivendor, multi-institutional comparison study. Radiology 249:624–630
Bhowmik NM, Yu J, Fulcher AS, Turner MA (2016) Benign causes of diffusion restriction foci in the peripheral zone of the prostate: diagnosis and differential diagnosis. Abdom Radiol (NY) 41:910–918
Ploussard G, Epstein JI, Montironi R et al (2011) The contemporary concept of significant versus insignificant prostate cancer. Eur Urol 60:291–303
Wolters T, Roobol MJ, van Leeuwen PJ et al (2011) A critical analysis of the tumor volume threshold for clinically insignificant prostate cancer using a data set of a randomized screening trial. J Urol 185:121–125
American Collage of Radiology. PI-RADS v2. http://www.acr.org/Quality-Safety/Resources/PIRADS. Accessed August 2016
Hambrock T, Somford DM, Huisman HJ et al (2011) Relationship between Apparent Diffusion Coefficients at 3.0-T MR Imaging and Gleason Grade in Peripheral Zone Prostate Cancer. Radiology. DOI:10.1148/radiol.091409
Verma S, Rajesh A, Morales H et al (2011) Assessment of aggressiveness of prostate cancer: correlation of apparent diffusion coefficient with histologic grade after radical prostatectomy. AJR Am J Roentgenol 196:374–381
Kim JY, Kim SH, Kim YH, Lee HJ, Kim MJ, Choi MS (2014) Low-risk prostate cancer: the accuracy of multiparametric MR imaging for detection. Radiology 271:435–444
Rosenkrantz AB, Lim RP, Haghighi M, Somberg MB, Babb JS, Taneja SS (2013) Comparison of interreader reproducibility of the prostate imaging reporting and data system and likert scales for evaluation of multiparametric prostate MRI. AJR Am J Roentgenol 201:W612–W618
Metens T, Miranda D, Absil J, Matos C (2012) What is the optimal b value in diffusion-weighted MR imaging to depict prostate cancer at 3T? Eur Radiol 22:703–709
Grant KB, Agarwal HK, Shih JH et al (2015) Comparison of calculated and acquired high b value diffusion-weighted imaging in prostate cancer. Abdom Imaging 40:578–586
Zaytoun OM, Stephenson AJ, Fareed K et al (2012) When serial prostate biopsy is recommended: most cancers detected are clinically insignificant. BJU Int 110:987–992
Acknowledgements
The scientific guarantor of this publication is Young Taik Oh. The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was waived by the Institutional Review Board. Methodology: retrospective, cross sectional study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, S.Y., Shin, SJ., Jung, D.C. et al. PI-RADS version 2: quantitative analysis aids reliable interpretation of diffusion-weighted imaging for prostate cancer. Eur Radiol 27, 2776–2783 (2017). https://doi.org/10.1007/s00330-016-4678-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-016-4678-7