Abstract
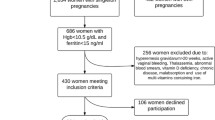
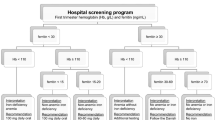
Currently, there is no consensus regarding the optimum iron supplementation during pregnancy. The aim of this study is to evaluate the effect of different iron supplementation doses (including no supplementation) during pregnancy on the iron status of the mother and on the health of the neonate. A longitudinal study was conducted involving 358 pregnant women and their newborns. Mothers were classified as non-supplemented, low iron supplemented (<60 mg/day), moderate iron supplemented (between 60 and 100 mg/day) or high iron supplemented (>100 mg/day). General clinical and obstetric histories, haemoglobin (Hb), serum ferritin (SF) and transferrin saturation were evaluated in the first, second, third trimesters, and at partum. SF and Hb decreased less sharply in the iron-supplemented groups compared to the non-supplemented group. The higher the doses of iron supplementation, the lower the percentages of iron depletion at partum (p < 0.001), iron deficiency anaemia (p < 0.001) and preterm deliveries (p = 0.009) as well as a higher birth weight of the newborn. However, the group with high supplementation had a greater percentage (27.6 %) of women at risk of haemoconcentration at partum. Our Mediterranean women began gestation with iron stores close to deficit (SF, 28.1 μg/L; 95 % CI 27.9–28.4). With these iron stores, supplementation with iron at daily doses of between 60 and 100 mg appears to be the most beneficial for the health of mother and child. These findings need to be confirmed in further randomised clinical trials.
Similar content being viewed by others
References
Bothwell TH (2000) Iron requirements in pregnancy and strategies to meet them. Am J Clin Nutr 72(Suppl 1):257S–264S
Hallberg L (2001) Perspectives on nutritional iron deficiency. Annu Rev Nutr 21:1–21
Cogswell ME, Parvanta I, Ickes L, Yip R, Brittenham GM (2003) Iron supplementation during pregnancy, anemia, and birth weight: a randomized controlled trial. Am J Clin Nutr 78:773–781
Shah PS, Ohlsson A (2009) Knowledge synthesis group on determinants of low birth weight and preterm births: effects of prenatal multimicronutrient supplementation on pregnancy outcomes: a meta-analysis. CMAJ 180:E99–E108
Aranda N, Ribot B, Garcia E, Viteri FE, Arija V (2011) Pre-pregnancy iron reserves, iron supplementation during pregnancy, and birth weight. Early Hum Dev 87:791–797
Hernandez-Martinez C, Canals J, Aranda N, Ribot B, Escribano J, Arija V (2011) Effects of iron deficiency on neonatal behavior at different stages of pregnancy. Early Hum Dev 87:165–169
Dirección General de Cohesión del Sistema Nacional de Salud y Alta Inspección (2006) Guía de prevención de defectos congénitos. Ministerio de Sanidad y Consumo, Madrid
World Health Organization (2006) Iron and folate supplementation. Standards for maternal and neonatal care. Integrated Management of Pregnancy and Childbirth (IMPAC), Geneva
Pena-Rosas JP, Viteri FE (2009) Effects and safety of preventive oral iron or iron + folic acid supplementation for women during pregnancy. Cochrane Database Syst Rev 4:CD004736
Siega-Riz AM, Hartzema AG, Turnbull C, Thorp J, McDonald T, Cogswell ME (2006) The effects of prophylactic iron given in prenatal supplements on iron status and birth outcomes: a randomized controlled trial. Am J Obstet Gynecol 194:512–519
Milman N, Bergholt T, Eriksen L, Byg KE, Graudal N, Pedersen P, Hertz J (2005) Iron prophylaxis during pregnancy—how much iron is needed? A randomized dose–response study of 20–80 mg ferrous iron daily in pregnant women. Acta Obstey Gynecol Scand 84:238–247
Chen X, Scholl TO, Stein TP (2006) Association of elevated serum ferritin levels and the risk of gestational diabetes mellitus in pregnant women: the Camden study. Diabetes Care 29:1077–1082
Hollingshead AB (2011) Four factor index of social status. Yale Journal of Sociology 8:21–52, http://www.yale.edu/sociology/yjs/yjs_fall_2011.pdf. Accessed 19 June 2012
Gomez F, Simo JM, Camps J, Cliville X, Bertran N, Ferre N, Bofill C, Joven J (2000) Evaluation of a particle-enhanced turbidimetric immunoassay for the measurement of ferritin: application to patients participating in an autologous blood transfusion program. Clin Biochem 33:191–196
Fairbanks VF, Klee GG (1999) Biochemical aspects of haematology. In: Burtis CA, Ashwood ER (eds) Tietz textbook of clinical chemistry. WB Saunders, Philadelphia, pp 1698–1705
Centers for Disease Control and Prevention (1998) Recommendations to prevent and control iron deficiency in the United States. MMWR Recomm. Rep 47:1–29
Casanueva E, Viteri FE, Mares-Galindo M, Meza-Camacho C, Loria A, Schnaas L, Valdes-Ramos R (2006) Weekly iron as a safe alternative to daily supplementation for nonanemic pregnant women. Arch Med Res 37:674–682
Scanlon KS, Yip R, Schieve LA, Cogswell ME (2000) High and low hemoglobin levels during pregnancy: differential risks for preterm birth and small for gestational age. Obstet Gynecol 96:741–748
Reinold C, Dalenius K, Smith B, Brindley P, Grummer-Straw L (2011) Pregnancy nutrition surveillance 2009 report. Department of Health and Human Services. Centers for Disease Control and Prevention, Atlanta
Carrillo SM, Pérez Guillén A, Hernández Hernández RA, Herrera Mogollón HA (2010) Anthropometric nutritional evaluation of the pregnant women and its relation with the product of the gestation. Nutr Hosp 25:832–837
Río I, Castelló A, Jané M, Prats R, Barona C, Más R, Rebagliato M, Zurriaga O, Bolúmar F (2010) Reproductive and perinatal health indicators in immigrant and Spanish-born women in Catalonia and Valencia (2005–2006). Gac Sanit 24:123–127
Simpson JL, Bailey LB, Pietrzik K, Shane B, Holzgreve W (2011) Micronutrients and women of reproductive potential: required dietary intake and consequences of dietary deficiency or excess. Part II—vitamin D, vitamin A, iron, zinc, iodine, essential fatty acids. J Matern Fetal Neonatal Med 24:1–24
Walsh T, O’Broin SD, Cooley S, Donnelly J, Kennedy J, Harrison RF, McMahon C, Geary M (2011) Laboratory assessment of iron status in pregnancy. Clin Chem Lab Med 49:1225–1230
Zimmermann MB (2008) Methods to assess iron and iodine status. Br J Nutr 99(Suppl 3):S2–S9
Muñoz M, García-Erce JA, Remacha ÁF (2011) Disorders of iron metabolism. Part II: iron deficiency and iron overload. J Clin Pathol 64:287–296
Rambod M, Kovesdy CP, Kalantar-Zadeh K (2008) Combined high serum ferritin and low iron saturation in hemodialysis patients: the role of inflammation. Clin J Am Soc Nephrol 3:1691–1701
Milman N, Agger AO, Nielsen OJ (1994) Iron status markers and serum erythropoietin in 120 mothers and newborn infants. Effect of iron supplementation in normal pregnancy. Acta Obstet Gynecol Scand 73:200–204
Svanberg B, Arvidsson B, Norrby A, Rybo G, Solvell L (1975) Absorption of supplemental iron during pregnancy—a longitudinal study with repeated bone-marrow studies and absorption measurements. Acta Obstet Gynecol Scand Suppl 48:87–108
Soares NN, Mattar R, Camano L, Torloni MR (2010) Iron deficiency anemia and iron stores in adult and adolescent women in pregnancy. Acta Obstet Gynecol Scand 89:343–349
Ribot B, Aranda N, Viteri F, Hernández-Martínez C, Canals J, Arija V (2012) Depleted iron stores without anaemia early in pregnancy carries increased risk of lower birthweight even when supplemented daily with moderate iron. Hum Reprod 27:1260–1266
Milman N, Byg KE, Bergholt T, Eriksen L, Hvas AM (2006) Body iron and individual iron prophylaxis in pregnancy—should the iron dose be adjusted according to serum ferritin? Ann Hematol 85:567–573
Romslo I, Haram K, Sagen N, Augensen K (1983) Iron requirement in normal pregnancy as assessed by serum ferritin, serum transferrin saturation and erythrocyte protoporphyrin determinations. Br J Obstet Gynaecol 90:101–107
Zhang Q, Ananth CV, Li Z, Smulian JC (2009) Maternal anaemia and preterm birth: a prospective cohort study. Int J Epidemiol 38:1380–1389
Wahed F, Latif SA, Nessa A, Bhuiyan MR, Hossain MB, Akther A, Mahmud MM (2010) Gestational anemia. Mymensingh Med J 19:462–468
Scholl TO (2005) Iron status during pregnancy: setting the stage for mother and infant. Am J Clin Nutr 81:1218S–1222S
Scholl TO, Hediger ML, Fischer RL, Shearer JW (1992) Anemia vs iron deficiency: increased risk of preterm delivery in a prospective study. Am J Clin Nutr 55:985–988
Allen LH (2001) Biological mechanisms that might underlie iron’s effects on fetal growth and preterm birth. J Nutr 131(Suppl 2):581S–589S
Macedo A, Cardoso S (2010) Routine iron supplementation in pregnancy. Acta Med Port 23:785–792
Ziaei S, Norrozi M, Faghihzadeh S, Jafarbegloo E (2007) A randomised placebo-controlled trial to determine the effect of iron supplementation on pregnancy outcome in pregnant women with haemoglobin > or = 13.2 g/dl. BJOG 114:684–688
von Tempelhoff GF, Heilmann L, Rudig L, Pollow K, Hommel G, Koscielny J (2008) Mean maternal second-trimester hemoglobin concentration and outcome of pregnancy: a population-based study. Clin Appl Thromb Hemost 14:19–28
Acknowledgments
This study was financially supported by a grant (PI052462) from the Health Research Fund of the Ministry of Health and Consumption (Madrid, Spain) [Instituto de Salud Carlos III, Fondo de Investigación Sanitaria, Ministerio de Sanidad y Consumo]. The authors would like to thank all the participating pregnant women for their enthusiastic collaboration. We thank the Clinical Chemistry Laboratories of the Hospital Sant Joan de Reus (Catalunya, Spain) for help with the blood analyses. We thank Fernando Viteri, iron expert, professor emeritus at the University of California, Berkeley, and research scientist at the Children’s Hospital Oakland Research Institute, for his expert assistance with the study and Ginny Gildengorin for the discussion of the analysis.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ribot, B., Aranda, N., Giralt, M. et al. Effect of different doses of iron supplementation during pregnancy on maternal and infant health. Ann Hematol 92, 221–229 (2013). https://doi.org/10.1007/s00277-012-1578-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-012-1578-z