Abstract
Purpose
End-stage renal disease (ESRD) is associated with increased cardiovascular risk factors, electrolyte imbalances, and iron deficiency anemia. These factors may increase the risk of adverse outcomes in patients undergoing panniculectomy. There is a paucity of data regarding outcomes in patients with ESRD undergoing panniculectomy. The purpose of this study is to investigate whether ESRD is associated with increased rate of complications following a panniculectomy.
Method
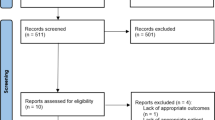
The Nationwide Inpatient Sample database (2006–2011) was used to identify patients who underwent a panniculectomy. Among this cohort, patients diagnosed with end-stage renal disease were identified. Patients excluded from the study were emergency admissions, pregnant women, patients less than 18 years old, and patients with concurrent nephrectomy or kidney transplants. Demographic factors, comorbidities, and postoperative complications were evaluated. Chi-squared and risk-adjusted multivariate logistic regression analyses were performed to determine whether end-stage renal disease was associated with increased rate of postoperative complications.
Results
A total of 34,779 panniculectomies were performed during the study period. Of these, 613 (1.8%) were diagnosed with ESRD. Patients with ESRD were older (mean age 58.9 vs. 49.3, p < 0.01) and more likely to have Medicare (63.5 vs. 18.4%, p < 0.01). They had higher rates of comorbidities, including diabetes, hypertension, congestive heart failure, chronic lung disease, chronic anemia, liver disease, peripheral artery disease, obesity, and coagulopathies (p < 0.01). The procedure was more likely to occur at a large, teaching hospital (p < 0.01). Postoperatively, patients with ESRD had a higher rate of death (3.3 vs. 0.2%, p < 0.01), wound complications (10.6 vs. 6.2%, p < 0.01), venous thromboembolism (4.9 vs. 0.8%, p < 0.01), blood transfusions (25.3% vs. 7.0%, p < 0.01), non-renal major medical complications (40.0% vs. 8.4%), and longer hospital stay (9.2 vs. 3.8 days, p < 0.01). Multivariate logistic regression analysis controlling for age, race, sex, hospital location/teaching hospital, payer, and all comorbidities demonstrated that ESRD was independently associated with increased venous thromboembolisms (OR 2.38, 95% CI 1.48–3.83) and non-renal major medical complications (OR 1.51, 95% CI 1.19–1.91). ESRD was not independently associated with increased rate of wound complications or transfusions.
Conclusion
Patients with ESRD are at increased risk of VTE and non-renal major medical complications following panniculectomy. Moreover, patients with ESRD have longer hospital stays and higher rates of mortality.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
References
Doyle SL, Lysaght J, Reynolds JV (2010) Obesity and post-operative complications in patients undergoing non-bariatric surgery. Obes Rev 11(12):875–886
Eckel RH, Bays HE, Klein S, Bade Horn D (2016) Proactive and progressive approaches in managing obesity. Postgrad Med 128(Suppl 1):21–30
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL (2016) Trends in obesity among adults in the United States, 2005 to 2014. JAMA 315(21):2284–2291
Segula D (2014) Complications of obesity in adults: a short review of the literature. Malawi Med J 26(1):20–24
Fox CS, Larson MG, Leip EP, Culleton B, Wilson PW, Levy D (2014) Predictors of new-onset kidney disease in a community-based population. JAMA 291(7):844–850
Hsu CY, McCulloch CE, Iribarren C, Darbinian J, Go AS (2006) Body mass index and risk for end-stage renal disease. Ann Intern Med 144(1):21–28
Kambham N, Markowitz GS, Valeri AM, Lin J, D’Agati VD (2001) Obesity-related glomerulopathy: an emerging epidemic. Kidney Int 59(4):1498–1509
Johansen KL (2012) The skinny on obesity and end-stage renal disease. Arch Intern Med 172(21):1651–1652
Schneider CR, Cobb W, Patel S, Cull D, Anna C, Roettger R (2009) Elective surgery in patients with end stage renal disease: what’s the risk? Am Surg 75(9):790–793 discussion 793
Wolfe RA, Ashby VB, Milford EL, Ojo AO, Ettenger RE, Agodoa LY, Held PJ, Port FK (1999) Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 341(23):1725–1730
Scandling JD (2005) Kidney transplant candidate evaluation. Semin Dial 18(6):487–494
Bailey CM, Troppmann C, Kuo J, Wong MS (2015) Panniculectomy in end-stage renal disease: six-year experience of performing panniculectomy in preparation for renal transplant. Ann Plast Surg 74(Suppl 1):S9–11
Kuo JH, Troppmann C, Perez RV, Wong MS (2011) Panniculectomy in preparation for renal transplantation: a new indication for an old procedure to reduce renal transplantation-associated wound complications. Plast Reconstr Surg 128(6):1236–1240
Kumar DR, Hanlin E, Glurich I, Mazza JJ, Yale SH (2010) Virchow’s contribution to the understanding of thrombosis and cellular biology. Clin Med Res 8(3–4):168–172
Gupta V, Winocour J, Rodriguez-Feo C, Bamba R, Shach RB, Grotting JC, Higdon KK (2016) Safety of aesthetic surgery in the overweight patient: analysis of 127,961 patients. Aesthet Surg J 36(6):718–729
Troppmann C, Santhanakrishnan C, Kuo JH, Bailey CM, Perez RV, Wong MS (2016) Impact of panniculectomy on transplant candidacy of obese patients with chronic kidney disease declined for kidney transplantation because of a high-risk abdominal panniculus: a pilot study. Surgery 159(6):1612–1622
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest to disclose.
Rights and permissions
About this article
Cite this article
Mundra, L.S., Rubio, G.A., AlQattan, H.T. et al. Panniculectomy Outcomes in Patients with End-Stage Renal Disease in Preparation for Renal Transplant. Aesth Plast Surg 42, 633–638 (2018). https://doi.org/10.1007/s00266-017-1043-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-1043-4