Abstract
Purpose
The aim of this study was to compare clinical and second-look arthroscopic outcomes between bone marrow aspirate concentrate (BMAC) augmentation and human umbilical cord blood-derived mesenchymal stromal cell (hUCB-MSC) implantation in high tibial osteotomy (HTO) for medial compartmental knee osteoarthritis and identify the relationship between articular cartilage regeneration and HTO outcomes.
Methods
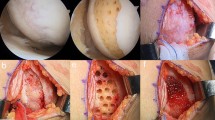
A total of 176 patients who underwent HTO combined with a BMAC or hUCB-MSC procedure for medial compartment osteoarthritis (Kellgren–Lawrence grade 3) between June 2014 and September 2018 with a minimum follow-up of 2 years were reviewed. After HTO, multiple holes were drilled at cartilage defect sites of the medial femoral condyle (MFC), and then prepared BMAC or hUCB-MSCs in combination with scaffolds were implanted in the MFC lesions. After propensity score matching based on sex, age, body mass index, and lesion size, 55 patients in each of the BMAC and hUCB-MSC groups were successfully matched. Second-look arthroscopic findings were assessed according to the International Cartilage Repair Society (ICRS) Cartilage Repair Assessment (CRA) grading system and Koshino staging system. Clinical outcomes were evaluated using the International Knee Documentation Committee (IKDC), Knee Injury and Osteoarthritis Outcome Score (KOOS), Short-Form 36 (SF-36), and Tegner activity scores.
Results
At a mean follow-up of 33 months, clinical outcomes including IKDC, KOOS, SF-36, and Tegner activity scores were significantly improved in both groups (p < 0.001); however, there were no differences between the two groups. Second-look arthroscopy showed better healing of regenerated cartilage in the hUCB-MSC group (Grade I [4 cases, 9.1%]; Grade II [30 cases, 68.2%]; Grade III [11 cases, 22.7%]) than in the BMAC group (Grade I [1 case, 2.7%]; Grade II [20 cases, 54.1%]; Grade III [11 cases, 29.7%]; Grade IV [5 cases, 13.5%]) according to the ICRS CRA grading system (p = 0.040). There was no significant intergroup difference in terms of defect coverage based on the Koshino staging system (p = 0.057). Moreover, ICRS CRA grades at second-look arthroscopy were significantly correlated with clinical outcomes (r = − 0.337; p = 0.002).
Conclusion
There were no significant differences in the clinical outcomes between the two groups. Both treatments provided similar, reliable outcomes in terms of pain relief, functional scores, and quality of life at a mean follow-up of 33 months. However, hUCB-MSC implantation was more effective than BMAC augmentation for articular cartilage regeneration.



Similar content being viewed by others
References
Akizuki S, Shibakawa A, Takizawa T, Yamazaki I, Horiuchi H (2008) The long-term outcome of high tibial osteotomy: a ten- to 20-year follow-up. J Bone Joint Surg Br 90:592–596
Amendola A, Bonasia DE (2010) Results of high tibial osteotomy: review of the literature. Int Orthop 34:155–160
Ando W, Tateishi K, Katakai D, Hart DA, Higuchi C, Nakata K et al (2008) In vitro generation of a scaffold-free tissue-engineered construct (TEC) derived from human synovial mesenchymal stem cells: biological and mechanical properties and further chondrogenic potential. Tissue Eng Part A 14:2041–2049
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res 46:399–424
Bode G, Ogon P, Pestka J, Zwingmann J, Feucht M, Sudkamp N et al (2015) Clinical outcome and return to work following single-stage combined autologous chondrocyte implantation and high tibial osteotomy. Int Orthop 39:689–696
Bode G, von Heyden J, Pestka J, Schmal H, Salzmann G, Sudkamp N et al (2015) Prospective 5-year survival rate data following open-wedge valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 23:1949–1955
Brittberg M, Winalski CS (2003) Evaluation of cartilage injuries and repair. J Bone Joint Surg Am 85-A(Suppl 2):58–69
Cavallo M, Sayyed-Hosseinian SH, Parma A, Buda R, Mosca M, Giannini S (2018) Combination of high tibial osteotomy and autologous bone marrow derived cell implantation in early osteoarthritis of knee: a preliminary study. Arch Bone Jt Surg 6:112–118
Cavinatto L, Hinckel BB, Tomlinson RE, Gupta S, Farr J, Bartolozzi AR (2019) The role of bone marrow aspirate concentrate for the treatment of focal chondral lesions of the knee: a systematic review and critical analysis of animal and clinical studies. Arthroscopy 35:1860–1877
Chung YW, Yang HY, Kang SJ, Song EK, Seon JK (2020) Allogeneic umbilical cord blood-derived mesenchymal stem cells combined with high tibial osteotomy: a retrospective study on safety and early results. Int Orthop. https://doi.org/10.1007/s00264-020-04852-y
Cotter EJ, Wang KC, Yanke AB, Chubinskaya S (2018) Bone marrow aspirate concentrate for cartilage defects of the knee: from bench to bedside evidence. Cartilage 9:161–170
Ding DC, Shyu WC, Lin SZ (2011) Mesenchymal stem cells. Cell Transplant 20:5–14
Dugdale TW, Noyes FR, Styer D (1992) Preoperative planning for high tibial osteotomy. The effect of lateral tibiofemoral separation and tibiofemoral length. Clin Orthop Relat Res 0:248–264
Ferruzzi A, Buda R, Cavallo M, Timoncini A, Natali S, Giannini S (2014) Cartilage repair procedures associated with high tibial osteotomy in varus knees: clinical results at 11 years’ follow-up. Knee 21:445–450
Filardo G, Zaffagnini S, De Filippis R, Perdisa F, Andriolo L, Candrian C (2018) No evidence for combining cartilage treatment and knee osteotomy in osteoarthritic joints: a systematic literature review. Knee Surg Sports Traumatol Arthrosc 26:3290–3299
Flynn A, Barry F, O’Brien T (2007) UC blood-derived mesenchymal stromal cells: an overview. Cytotherapy 9:717–726
Fujisawa Y, Masuhara K, Shiomi S (1979) The effect of high tibial osteotomy on osteoarthritis of the knee. An arthroscopic study of 54 knee joints. Orthop Clin North Am 10:585–608
Gao J, Dennis JE, Solchaga LA, Awadallah AS, Goldberg VM, Caplan AI (2001) Tissue-engineered fabrication of an osteochondral composite graft using rat bone marrow-derived mesenchymal stem cells. Tissue Eng 7:363–371
Gigante A, Cecconi S, Calcagno S, Busilacchi A, Enea D (2012) Arthroscopic knee cartilage repair with covered microfracture and bone marrow concentrate. Arthrosc Tech 1:e175-180
Gobbi A, Karnatzikos G, Scotti C, Mahajan V, Mazzucco L, Grigolo B (2011) One-step cartilage repair with bone marrow aspirate concentrated cells and collagen matrix in full-thickness knee cartilage lesions: results at 2-year follow-up. Cartilage 2:286–299
Gobbi A, Whyte GP (2016) One-stage cartilage repair using a hyaluronic acid-based scaffold with activated bone marrow-derived mesenchymal stem cells compared with microfracture: five-year follow-up. Am J Sports Med 44:2846–2854
Goshima K, Sawaguchi T, Shigemoto K, Iwai S, Nakanishi A, Ueoka K (2019) Assessment of unloading effects after open wedge high tibial osteotomy using quantitative bone scintigraphy. J Orthop Sci 24:680–685
Harris JD, McNeilan R, Siston RA, Flanigan DC (2013) Survival and clinical outcome of isolated high tibial osteotomy and combined biological knee reconstruction. Knee 20:154–161
Jin QH, Chung YW, Na SM, Ahn HW, Jung DM, Seon JK (2020) Bone marrow aspirate concentration provided better results in cartilage regeneration to microfracture in knee of osteoarthritic patients. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06099-x
Jung WH, Takeuchi R, Chun CW, Lee JS, Ha JH, Kim JH et al (2014) Second-look arthroscopic assessment of cartilage regeneration after medial opening-wedge high tibial osteotomy. Arthroscopy 30:72–79
Kahlenberg CA, Nwachukwu BU, Hamid KS, Steinhaus ME, Williams RJ 3rd (2017) Analysis of outcomes for high tibial osteotomies performed with cartilage restoration techniques. Arthroscopy 33:486–492
Kanamiya T, Naito M, Hara M, Yoshimura I (2002) The influences of biomechanical factors on cartilage regeneration after high tibial osteotomy for knees with medial compartment osteoarthritis: clinical and arthroscopic observations. Arthroscopy 18:725–729
Kern S, Eichler H, Stoeve J, Kluter H, Bieback K (2006) Comparative analysis of mesenchymal stem cells from bone marrow, umbilical cord blood, or adipose tissue. Stem Cells 24:1294–1301
Kim KI, Seo MC, Song SJ, Bae DK, Kim DH, Lee SH (2017) Change of chondral lesions and predictive factors after medial open-wedge high tibial osteotomy with a locked plate system. Am J Sports Med 45:1615–1621
Kim KJ, Song EK, Seon JK, Seol JH (2015) Biomechanical study of the fixation plates for opening wedge high tibial osteotomy. Knee Surg Relat Res 27:181–186
Kim MS, Koh IJ, Choi YJ, Pak KH, In Y (2017) Collagen augmentation improves the quality of cartilage repair after microfracture in patients undergoing high tibial osteotomy: a randomized controlled trial. Am J Sports Med 45:1845–1855
Kim YS, Koh YG (2018) Comparative matched-pair analysis of open-wedge high tibial osteotomy with versus without an injection of adipose-derived mesenchymal stem cells for varus knee osteoarthritis: clinical and second-look arthroscopic results. Am J Sports Med 46:2669–2677
Koh YG, Choi YJ, Kwon OR, Kim YS (2014) Second-look arthroscopic evaluation of cartilage lesions after mesenchymal stem cell implantation in osteoarthritic knees. Am J Sports Med 42:1628–1637
Koh YG, Kwon OR, Kim YS, Choi YJ (2014) Comparative outcomes of open-wedge high tibial osteotomy with platelet-rich plasma alone or in combination with mesenchymal stem cell treatment: a prospective study. Arthroscopy 30:1453–1460
Koshino T, Wada S, Ara Y, Saito T (2003) Regeneration of degenerated articular cartilage after high tibial valgus osteotomy for medial compartmental osteoarthritis of the knee. Knee 10:229–236
Kyung HS, Lee BJ, Kim JW, Yoon SD (2015) Biplanar open wedge high tibial osteotomy in the medial compartment osteoarthritis of the knee joint: comparison between the aescula and tomofix plate. Clin Orthop Surg 7:185–190
Lind-Hansen TB, Lind MC, Nielsen PT, Laursen MB (2016) Open-wedge high tibial osteotomy: RCT 2 years RSA follow-up. J Knee Surg 29:664–672
Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11:132–138
Madry H, Gao L, Eichler H, Orth P, Cucchiarini M (2017) Bone marrow aspirate concentrate-enhanced marrow stimulation of chondral defects. Stem Cells Int 2017:1609685
Matsunaga D, Akizuki S, Takizawa T, Yamazaki I, Kuraishi J (2007) Repair of articular cartilage and clinical outcome after osteotomy with microfracture or abrasion arthroplasty for medial gonarthrosis. Knee 14:465–471
Niemeyer P, Schmal H, Hauschild O, von Heyden J, Sudkamp NP, Kostler W (2010) Open-wedge osteotomy using an internal plate fixator in patients with medial-compartment gonarthritis and varus malalignment: 3-year results with regard to preoperative arthroscopic and radiographic findings. Arthroscopy 26:1607–1616
Papachristou G, Plessas S, Sourlas J, Levidiotis C, Chronopoulos E, Papachristou C (2006) Deterioration of long-term results following high tibial osteotomy in patients under 60 years of age. Int Orthop 30:403–408
Park YB, Ha CW, Lee CH, Yoon YC, Park YG (2017) Cartilage regeneration in osteoarthritic patients by a composite of allogeneic umbilical cord blood-derived mesenchymal stem cells and hyaluronate hydrogel: results from a clinical trial for safety and proof-of-concept with 7 years of extended follow-up. Stem Cells Transl Med 6:613–621
Parker DA, Viskontas DG (2007) Osteotomy for the early varus arthritic knee. Sports Med Arthrosc Rev 15:3–14
Pascale W, Luraghi S, Perico L, Pascale V (2011) Do microfractures improve high tibial osteotomy outcome? Orthopedics 34:e251-255
Roos EM, Roos HP, Lohmander LS, Ekdahl C, Beynnon BD (1998) Knee injury and osteoarthritis outcome score (KOOS)–development of a self-administered outcome measure. J Orthop Sports Phys Ther 28:88–96
Rossi MJ, Lubowitz JH, Guttmann D (2002) Development and validation of the International Knee Documentation Committee Subjective Knee Form. Am J Sports Med 30:152
Scharstuhl A, Schewe B, Benz K, Gaissmaier C, Buhring HJ, Stoop R (2007) Chondrogenic potential of human adult mesenchymal stem cells is independent of age or osteoarthritis etiology. Stem Cells 25:3244–3251
Song JS, Hong KT, Kim NM, Jung JY, Park HS, Lee SH et al (2020) Implantation of allogenic umbilical cord blood-derived mesenchymal stem cells improves knee osteoarthritis outcomes: Two-year follow-up. Regen Ther 14:32–39
Song JS, Hong KT, Kim NM, Park HS, Choi NH (2020) Human umbilical cord blood-derived mesenchymal stem cell implantation for osteoarthritis of the knee. Arch Orthop Trauma Surg 140:503–509
Sprenger TR, Doerzbacher JF (2003) Tibial osteotomy for the treatment of varus gonarthrosis. Survival and failure analysis to twenty-two years. J Bone Joint Surg Am 85:469–474
Sterett WI, Steadman JR, Huang MJ, Matheny LM, Briggs KK (2010) Chondral resurfacing and high tibial osteotomy in the varus knee: survivorship analysis. Am J Sports Med 38:1420–1424
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 0:43–49
Veronesi F, Giavaresi G, Tschon M, Borsari V, Nicoli Aldini N, Fini M (2013) Clinical use of bone marrow, bone marrow concentrate, and expanded bone marrow mesenchymal stem cells in cartilage disease. Stem Cells Dev 22:181–192
Webb M, Dewan V, Elson D (2018) Functional results following high tibial osteotomy: a review of the literature. Eur J Orthop Surg Traumatol 28:555–563
Wright JM, Crockett HC, Slawski DP, Madsen MW, Windsor RE (2005) High tibial osteotomy. J Am Acad Orthop Surg 13:279–289
Yang HY, Kang SJ, Kwak WK, Song EK, Seon JK (2020) The influence of preoperative tibial bone marrow edema on outcomes after medial opening-wedge high tibial osteotomy. J Bone Joint Surg Am. https://doi.org/10.2106/jbjs.20.00037
Acknowledgements
No specific grant was received for this research from funding agencies in the public, commercial, or not-for-profit-sectors.
Funding
The authors declare that they have non-financial competing interests.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by HYY, EKS, SJK, WKK, and JKK. Review, editing and supervision by JKS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Human Investigation Committee (IRB) of Hwasun Chonnam National University Hospital approved this study.
Informed consent
Written informed consent for participation in the study was obtained from all patients, including permission to access patient’s records and publish individual clinical details.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, HY., Song, EK., Kang, SJ. et al. Allogenic umbilical cord blood-derived mesenchymal stromal cell implantation was superior to bone marrow aspirate concentrate augmentation for cartilage regeneration despite similar clinical outcomes. Knee Surg Sports Traumatol Arthrosc 30, 208–218 (2022). https://doi.org/10.1007/s00167-021-06450-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06450-w