Abstract
Background
Some reports have stated that pancreatoduodenectomy for elderly patients have comparable morbidity and mortality to that of young patients. However, the long-term outcomes of these patients have not been fully evaluated, especially for pancreatic head cancer.
Methods
A total of 227 patients who underwent pancreatoduodenectomy for pancreatic head cancer between 2007 and 2014 were included. They were stratified according to age: young (<70 years), elderly (70 to <80 years), and very elderly (≥80 years). The short- and long-term outcomes were evaluated.
Results
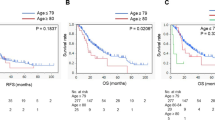
There were no significant differences in terms of morbidity among the three groups. The median disease-free survival times were 15 months in the young, 11 months in the elderly, and 7 months in the very elderly. The disease-free survival of the young patients was significantly better than that in both the elderly and the very elderly (p = 0.012 and p = 0.016). The median overall survival times were 30 months in the young, 20 months in the elderly, and 14 months in the very elderly. The overall survival of the young patients was significantly better than that in both the elderly and the very elderly (p = 0.007 and p < 0.001). The difference was marginal between the elderly and the very elderly (p = 0.053). Multivariate analysis revealed that lymph node metastasis (p < 0.001), age ≥80 years (p = 0.013), lack of adjuvant chemotherapy (p = 0.003), blood transfusion (p = 0.015), and CA 19-9 ≥300 U/ml (p = 0.040) were significant prognostic factors.
Conclusions
Patient age influenced the survival after pancreatoduodenectomy for pancreatic cancer.

Similar content being viewed by others
References
World report on ageing and health 2015. http://www.who.int/ageing/publications/world-report-2015/.
Cancer Statistics in Japan. ublicat. http://ganjoho.jp/data/reg_stat/statistics/brochure/2015/cancer_statistics_2015.pdf.
Gouma DJ, van Geenen RC, van Gulik TM, et al. Rates of complications and death after pancreaticoduodenectomy: risk factors and the impact of hospital volume. Ann Surg. 2000;232(6):786–95.
DeOliveira ML, Winter JM, Schafer M, et al. Assessment of complications after pancreatic surgery: a novel grading system applied to 633 patients undergoing pancreaticoduodenectomy. Ann Surg. 2006; 244(6):931–937; discussion 937–939.
DiCarlo V, Balzano G, Zerbi A, Villa E. Pancreatic cancer resection in elderly patients. Br J Surg. 1998;85(5):607–10.
Petrowsky H, Clavien PA. Should we deny surgery for malignant hepato-pancreatico-biliary tumors to elderly patients? World J Surg. 2005;29(9):1093-100.
Ballarin R, Spaggiari M, Di Benedetto F, et al. Do not deny pancreatic resection to elderly patients. J Gastrointest Surg. 2009;13(2):341–8.
Sohn TA, Yeo CJ, Cameron JL, et al. Should pancreaticoduodenectomy be performed in octogenarians? J Gastrointest Surg. 1998;2(3):207–16.
Makary MA, Winter JM, Cameron JL, et al. Pancreaticoduodenectomy in the very elderly. J Gastrointest Surg. 2006;10(3):347–56.
Khan S, Sclabas G, Lombardo KR, et al. Pancreatoduodenectomy for ductal adenocarcinoma in the very elderly: is it safe and justified? J Gastrointest Surg. 2010;14(11):1826–31.
Tani M, Kawai M, Hirono S, et al. A pancreaticoduodenectomy is acceptable for periampullary tumors in the elderly, even in patients over 80 years of age. J Hepatobiliary Pancreat Surg. 2009;16(5):675–80.
Hatzaras I, Schmidt C, Klemanski D, et al. Pancreatic resection in the octogenarian: a safe option for pancreatic malignancy. J Am Coll Surg. 2011;212(3):373–7.
Oguro S, Shimada K, Kishi Y, et al. Perioperative and long-term outcomes after pancreaticoduodenectomy in elderly patients 80 years of age and older. Langenbeck’s Arch Surg. 2013;398(4):531–8.
Lee MK, Dinorcia J, Reavey PL, et al. Pancreaticoduodenectomy can be performed safely in patients aged 80 years and older. J Gastrointest Surg. 2010;14(11):1838–46.
Melis M, Marcon F, Masi A, et al. The safety of a pancreaticoduodenectomy in patients older than 80 years: risk vs. benefits. HPB. 2012;14(9):583–8.
Turrini O, Paye F, Bachellier P, et al. Pancreatectomy for adenocarcinoma in elderly patients: postoperative outcomes and long term results: a study of the French Surgical Association. Eur J Surg Oncol. 2013;39(2):171–8.
NCCN Clinical Practice Guidelines in Oncology: Pancreatic adenocarcinoma, version 2. 2016. https://www.nccn.org/professionals/physician_gls/pdf/pancreatic.pdf.
Bassi C, Dervenis C, Butturini G, et al. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005;138(1):8–13.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004; 240(2):205–213.
Sobin L, Gosporarowicz M, Wittekind C. TNM classification of malignant tumors (7th edn). New York: Wiley-Blackwell, 2009.
Oettle H, Post S, Neuhaus P, et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA. 2007;297(3):267–77.
Uesaka K, Boku N, Fukutomi A, et al. Adjuvant chemotherapy of S-1 versus gemcitabine for resected pancreatic cancer: a phase 3, open-label, randomised, non-inferiority trial (JASPAC 01). Lancet. 2016;388(10041):248–57.
World Health Statistics 2015. 2015. http://www.who.int/gho/publications/world_health_statistics/2015/en/.
Finlayson E, Fan Z, Birkmeyer JD. Outcomes in octogenarians undergoing high-risk cancer operation: a national study. J Am Coll Surg. 2007;205(6):729–34.
Riall TS, Reddy DM, Nealon WH, Goodwin JS. The effect of age on short-term outcomes after pancreatic resection: a population-based study. Ann Surg. 2008;248(3):459–67.
Sho M, Murakami Y, Kawai M, et al. Prognosis after surgical treatment for pancreatic cancer in patients aged 80 years or older: a multicenter study. J Hepatobiliary Pancreat Sci. 2016;23(3):188–97.
Neoptolemos JP, Stocken DD, Friess H, et al. A randomized trial of chemoradiotherapy and chemotherapy after resection of pancreatic cancer. N Engl J Med. 2004;350(12):1200-10.
Kinoshita S, Sho M, Yanagimoto H, et al. Potential role of surgical resection for pancreatic cancer in the very elderly. Pancreatology. 2015;15(3):240–6.
Conroy T, Desseigne F, Ychou M, et al. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. N Engl J Med. 2011;364(19):1817–25.
Von Hoff DD, Ervin T, Arena FP, et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. N Engl J Med. 2013;369(18):1691–703.
Sugiura T, Uesaka K, Kanemoto H, et al. Serum CA19-9 is a significant predictor among preoperative parameters for early recurrence after resection of pancreatic adenocarcinoma. J Gastrointest Surg. 2012;16(5):977–85.
Yang JJ, Hu ZG, Shi WX, et al. Prognostic significance of neutrophil to lymphocyte ratio in pancreatic cancer: a meta-analysis. World J Gastroenterol. 2015;21(9):2807–15.
Kanda M, Fujii T, Kodera Y, et al. Nutritional predictors of postoperative outcome in pancreatic cancer. Br J Surg. 2011;98(2):268–74.
Yamada S, Fujii T, Yabusaki N, et al. Clinical implication of inflammation-based prognostic score in pancreatic cancer: Glasgow Prognostic Score is the most reliable parameter. Medicine. 2016; 95(18):e3582.
Disclosure
The authors declare no financial or any other type of support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sugiura, T., Okamura, Y., Ito, T. et al. Impact of Patient Age on the Postoperative Survival in Pancreatic Head Cancer. Ann Surg Oncol 24, 3220–3228 (2017). https://doi.org/10.1245/s10434-017-5994-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-5994-0