Abstract
Background
Postoperative pain is a major challenge for patients undergoing breast reconstruction after surgical treatment of breast cancer, resulting in prolonged hospitalizations and additional resource utilization. Evidence on the efficacy of techniques to minimize postoperative pain in autologous breast reconstruction is lacking. We sought to determine whether preoperative paravertebral block (PVB), a regional anesthetic technique, affects postoperative pain control and hospital length of stay (LOS) in patients undergoing autologous breast reconstruction.
Methods
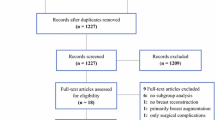
Consecutive patients undergoing postmastectomy autologous breast reconstruction between 2012 and 2015 were identified from a prospectively collected database to compare those who received PVB to those who did not. Primary outcomes included self-reported pain score, time to oral-only narcotic usage (TTON), and LOS. Sample differences were compared using Wilcoxon rank-sum and Chi square tests for continuous and categorical variables. Kaplan–Meier analysis was used to evaluate TTON and LOS, with Mantel-Cox test used to compare groups.
Results
Of 78 patients, 39 received PVB and 39 did not. Study groups did not differ regarding age, body mass index, American Society of Anesthesiologists class, mastectomy type, flap type, or cancer stage (p > 0.05). Patients in the PVB group reported significantly lower postoperative pain at 2 (p < 0.01) and 24 h (p < 0.01) and shorter median TTON (66 vs. 76 h, p < 0.01). Importantly, median LOS was reduced for patients receiving a PVB in both hours (95 vs. 116, p < 0.01) and hospital nights (4 vs. 5, p = 0.05).
Conclusions
Preoperative PVB is associated with improved postoperative pain control and shorter hospitalizations for patients with breast cancer undergoing postmastectomy autologous reconstruction.



Similar content being viewed by others
References
American Cancer Society. Cancer facts and figures, 2016. Atlanta: American Cancer Society; 2016.
Albornoz CR, Bach PB, Mehrara BJ, et al. A paradigm shift in U.S. breast reconstruction: increasing implant rates. Plast Reconstr Surg. 2013;131:15–23.
Sisco M, Du H, Warner JP, Howard MA, Winchester DP, Yao K. Have we expanded the equitable delivery of postmastectomy breast reconstruction in the new millennium? Evidence from the National Cancer Data Base. J Am Coll Surg. 2012;215:658–66.
Dean C, Chetty U, Forrest AP. Effects of immediate breast reconstruction on psychosocial morbidity after mastectomy. Lancet. 1983;1(8322):459–62.
Eltahir Y, Werners LL, Dreise MM, et al. Quality-of-life outcomes between mastectomy alone and breast reconstruction: comparison of patient-reported BREAST-Q and other health-related quality-of-life measures. Plast Reconstr Surg. 2013;132:201e-209e.
Jagsi R, Li Y, Morrow M, et al. Patient-reported quality of life and satisfaction with cosmetic outcomes after breast conservation and mastectomy with and without reconstruction: results of a survey of breast cancer survivors. Ann Surg. 2015;261:1198–206.
Winters ZE, Benson JR, Pusic AL. A systematic review of the clinical evidence to guide treatment recommendations in breast reconstruction based on patient-reported outcome measures and health-related quality of life. Ann Surg. 2010;252:929–42.
Andreae MH, Andreae DA. Regional anaesthesia to prevent chronic pain after surgery: a Cochrane systematic review and meta-analysis. Br J Anaesth. 2013;111:711–20.
Coveney E, Weltz CR, Greengrass R, et al. Use of paravertebral block anesthesia in the surgical management of breast cancer: experience in 156 cases. Ann Surg. 1998;227:496–501.
Fahy AS, Jakub JW, Dy BM, et al. Paravertebral blocks in patients undergoing mastectomy with or without immediate reconstruction provides improved pain control and decreased postoperative nausea and vomiting. Ann Surg Oncol. 2014;21:3284–9.
Shah A, Rowlands M, Krishnan N, Patel A, Ott-Young A. Thoracic intercostal nerve blocks reduce opioid consumption and length of stay in patients undergoing implant-based breast reconstruction. Plast Reconstr Surg. 2015;136:584e-591e.
Coopey SB, Specht MC, Warren L, Smith BL, Winograd JM, Fleischmann K. Use of preoperative paravertebral block decreases length of stay in patients undergoing mastectomy plus immediate reconstruction. Ann Surg Oncol. 2013;20:1282–6.
Wolf O, Clemens MW, Purugganan RV, et al. A prospective, randomized, controlled trial of paravertebral block versus general anesthesia alone for prosthetic breast reconstruction. Plast Reconstr Surg. 2016;137:660e–6e.
Matros E, Albornoz CR, Razdan SN, et al. Cost-effectiveness analysis of implants versus autologous perforator flaps using the BREAST-Q. Plast Reconstr Surg. 2015;135:937–46.
Lee KT, Mun GH. Prosthetic breast reconstruction in previously irradiated breasts: a meta-analysis. J Surg Oncol. 2015;112:468–75.
Atisha D, Alderman AK. A systematic review of abdominal wall function following abdominal flaps for postmastectomy breast reconstruction. Ann Plast Surg. 2009;63:222–30.
Gart MS, Smetona JT, Hanwright PJ, et al. Autologous options for postmastectomy breast reconstruction: a comparison of outcomes based on the American College of Surgeons National Surgical Quality Improvement Program. J Am Coll Surg. 2013;216:229–38.
Jagsi R, Jiang J, Momoh AO, et al. Complications after mastectomy and immediate breast reconstruction for breast cancer: a claims-based analysis. Ann Surg. 2016;263:219–27.
Gartner R, Jensen MB, Nielsen J, Ewertz M, Kroman N, Kehlet H. Prevalence of and factors associated with persistent pain following breast cancer surgery. JAMA. 2009;302:1985–92.
Hickey OT, Burke SM, Hafeez P, Mudrakouski AL, Hayes ID, Shorten GD. Severity of acute pain after breast surgery is associated with the likelihood of subsequently developing persistent pain. Clin J Pain. 2010;26:556–60.
Macdonald L, Bruce J, Scott NW, Smith WC, Chambers WA. Long-term follow-up of breast cancer survivors with post-mastectomy pain syndrome. Br J Cancer. 2005;92:225–30.
Knight MA, Nguyen DTt, Kobayashi MR, Evans GR. Institutional review of free TRAM flap breast reconstruction. Ann Plast Surg. 2006;56:593–8.
Acknowledgment
R.P.P. is supported by a National Institutes of Health (NIH) Ruth L. Kirschstein National Research Service Award Institutional Research Training Grant, T32CA190194 (PI: Colditz), by the Foundation for Barnes-Jewish Hospital, and by Siteman Cancer Center. The content is solely the responsibility of the authors and does not necessarily represent the official view of the NIH.
Disclosure
T.M.M. receives research Grant and consulting fees from LifeCell, Allergan, and Andrew Technologies; none of these relationships relate to or had an impact on this study. The other authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parikh, R.P., Sharma, K., Guffey, R. et al. Preoperative Paravertebral Block Improves Postoperative Pain Control and Reduces Hospital Length of Stay in Patients Undergoing Autologous Breast Reconstruction after Mastectomy for Breast Cancer. Ann Surg Oncol 23, 4262–4269 (2016). https://doi.org/10.1245/s10434-016-5471-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5471-1