Abstract
Objective
In rodents, intravenous sulfide protected against spinal cord ischemia/reperfusion (I/R) injury during aortic balloon occlusion. We investigated the effect of intravenous sulfide on aortic occlusion-induced porcine spinal cord I/R injury.
Methods
Anesthetized and mechanically ventilated “familial hypercholesterolemia Bretoncelles Meishan” (FBM) pigs with high-fat-diet-induced hypercholesterolemia and atherosclerosis were randomized to receive either intravenous sodium sulfide 2 h (initial bolus, 0.2 mg kg body weight (bw)−1; infusion, 2 mg kg bw−1 h−1; n = 4) or vehicle (sodium chloride, n = 4) prior to 45 min of thoracic aortic balloon occlusion and for 8 h during reperfusion (infusion, 1 mg kg bw−1 h−1). During reperfusion, noradrenaline was titrated to maintain blood pressure at above 80% of the baseline level. Spinal cord function was assessed by motor evoked potentials (MEPs) and lower limb reflexes using a modified Tarlov score. Spinal cord tissue damage was evaluated in tissue collected at the end of experiment using hematoxylin and eosin and Nissl staining.
Results
A balloon occlusion time of 45 min resulted in marked ischemic neuron damage (mean of 16% damaged motoneurons in the anterior horn of all thoracic motor neurons) in the spinal cord. In the vehicle group, only one animal recovered partial neuronal function with regain of MEPs and link motions at each time point after deflating. All other animals completely lost neuronal functions. The intravenous application of sodium sulfide did not prevent neuronal cell injury and did not confer to functional recovery.
Conclusion
In a porcine model of I/R injury of the spinal cord, treatment with intravenous sodium sulfide had no protective effect in animals with a pre-existing arteriosclerosis.
Similar content being viewed by others
Background
During open aortic surgery, interrupting blood flow through the aorta by applying a cross-clamp is often a key step to allow for surgical repair. Consequently, ischemia is induced in parts of the body distal to the clamp site. This significant alteration in blood flow by cross-clamping induces hemodynamic changes. Upon release of the cross-clamp, the blood flow is restored, triggering an ischemia/reperfusion (I/R) injury, leading to tissue inflammation, humoral changes, and lactate acidosis that increases the risk of multi-organ failure (MOF) and therefore affects postoperative outcome [1]. The most vulnerable organs are the kidney (renal failure, incidence 4.6–5.6%) and the spinal cord (ischemia, incidence 2.7–13.2%) [2, 3].
Hydrogen sulfide (H2S) is an endogenously produced gaseous transmitter and neuromodulator, derived from l-cysteine in several organs, such as the brain, heart, kidney, and liver [4]. H2S plays many important roles in the central nervous system under physiological and pathological states, especially in secondary neuronal injury. H2S has been shown to protect the brain from I/R injury via maintenance of mitochondrial function, inhibiting pro-inflammatory factors, neutralizing reactive oxygen species (ROS), and reducing apoptosis [5]. In a rat model of aortic balloon occlusion for 12 h, pre-emptive intraperitoneal injection of 30 μmol kg−1 sodium hydrogen sulfide (NaSH) reduced spinal cord infarct area and improved hind motor function 48 h after aortic occlusion [6]. In this study, it was reported that the reduced spinal cord injury was due to enhanced neurocyte autophagy. As of today, no data on the effects of H2S on spinal cord injury after aortic clamping in large animals is available. The transferability of the efficacy of H2S-based therapies from rodent models into larger animals may be questioned, at least in part due to their large surface area/mass ratio [7,8,9,10]. Therefore, the aim of this study was to test the hypothesis whether an intravenous (i.v.) formulation of sodium sulfide (Na2S) would induce neuroprotective effects during porcine aortic balloon occlusion-induced spinal cord I/R injury using a human-like porcine model of ubiquitous arteriosclerosis.
Materials and methods
Animals
The experiments were performed in adherence with the National Institutes of Health Guidelines on the use of Laboratory Animals and after approval of the protocol by the regional council of Tübingen (Registration number 905). Eight downsized familial hypercholesterolemia Bretoncelles Meishan (FBM) pigs of either sex with a mean bodyweight of 64 kg (range 24–92 kg) were used. The pigs were housed and fed as described previously [11, 12]. Na2S for i.v. injection was kindly provided by Csaba Szabo (Department of Anesthesiology, University of Texas Medical Branch, Galveston, TX, USA) and synthetized using H2S gas as the starting material, which was bubbled through an aqueous solution of sodium hydroxide (NaOH) and saline, formulated to pH neutrality and iso-osmolarity. This solution was filtered and placed under N2 atmosphere [13,14,15].
Procedure
The anesthetic procedure, surgical preparation, placement of catheters, and physiological measurements have been described in detail previously [12, 16]. Briefly, after induction of anesthesia (i.v., propofol, ketamine) and subsequent endotracheal intubation, anesthesia was maintained with continuous i.v. propofol (6–8 mg kg−1 h−1) and remifentanil (15–20 μg kg−1 h− 1). Pigs were mechanically ventilated [FiO2 0.25–0.35, adjusted to keep arterial pO2 levels > 100 mmHg, tidal volume 10 mL kg−1, positive end-expiratory pressure (PEEP) 5 cmH2O, inspiratory/expiratory time ratio 1:1.5, respiratory rate 10–13 min−1 adjusted to maintain arterial pCO2 between 35 and 40 mmHg]. These ventilator settings were used because swine are particularly susceptible to atelectasis formation in dependent lung regions due to the lack of alveolar collateral ventilation [16]. Sodium heparin (200 IU h−1) was continuously infused for anticoagulation. Via surgical cut-downs, the catheters were placed in the A. carotis dextra for measurement of blood pressure in the upper half of the body (mean arterial pressure, MAP proximal), trans-pulmonary single indicator thermodilution-cardiac index (CI), and the intra-thoracic blood volume index (ITBVI), a well-accepted marker of cardiac preload [17], as well as in the V. jugularis dextra for measurement of central venous pressure (CVP) and drug infusion. Via femoral cut-down, catheter sheaths were introduced into the Aa. femorales sinistra and dextra for distal blood pressure recording (MAP distal) and placement of inflatable balloon catheters. Adapting a technique previously published by several authors [18, 19], one catheter was placed directly above the aortic trifurcation, and the other one directly downstream of the A. subclavia sinistra, the correct position of which was manually controlled via a left-sided thoracotomy. This approach was chosen to prevent any perfusion of the spinal cord via collateral flow distal to the proximal balloon [20], which could result from variable bifurcation of the A. radicularis magna anterior [21]. The intra-aortic balloon occlusion was used to avoid mechanical injury related to clamp placement and release per se [22]. After 30 to 45 min of occlusion time, the balloon catheters were deflated. We started with an occlusion time of 30 min, followed by 40 min in preliminary experiments to test the response of this pig strain to a spinal cord I/R injury. Aortic occlusion was then performed for 45 min because this ischemia time had resulted in moderate neuronal damage (5 to 15% of all motor neurons) in the spinal cord in previous experiments [23]. In addition, 45 min of aortic occlusion prevented both the large spinal cord infarction over several segments reported in pigs after a clamping period of 60 min or longer [24] and the fairly mild tissue damage observed after only 30 min of clamping [25, 26]. Pigs were normothermic at the beginning of preparation period, and body temperature dropped to 32 °C at the start of either sodium sulfide or sodium chloride infusion. Pigs of this particular strain are known to spontaneously develop hypothermia during anesthesia [12]. Hemodynamic data, motor evoked potentials (MEPs), and neuronal function were assessed during aortic balloon occlusion and at 1 h, 4 h, and 8 h of reperfusion.
Application of sodium sulfide (Na2S)
Two hours before balloon occlusion, animals were treated with saline (vehicle group) or sodium sulfide (study group). The sodium sulfide infusion rate (initial bolus 0.2 mg kg−1 followed by continuous i.v. infusion of 2 mg kg−1 h−1 during the 2 h before aortic occlusion, and 1 mg kg−1 h−1 during the 8 h reperfusion) was based on previous studies [27]. During balloon occlusion time, sodium sulfide or vehicle infusion was stopped.
Harvesting, measurements, and calculations
The animals were euthanized in deep anesthesia by giving a bolus of phenobarbital (Narkodorm Alvetra, Neumünster, Germany) and i.v. potassium chloride (20 mmol, Braun, Melsungen, Germany). Tissue samples of the lumbar and thoracic spinal cord were isolated immediately post mortem and fixed in 6% buffered paraformaldehyde, and standard 3-μm paraffin sections were stained with hematoxylin and eosin (HE). Particular attention was paid on the anterior horn (AH), because of the vulnerability due to a hypoxic damage [28]. In addition, spinal cord sections were analyzed after nuclear cresol violet staining (Nissl staining) for neuronal damage [26].
Spinal cord function was evaluated by MEPs as described previously [24, 29, 29, 30]. Three electrodes were inserted into the scalp, and one into the soft palate to apply electric impulses (Digitimer Ltd., MultiPulse Stimulator D185 mark IIa) to the motor cortex. To quantify MEPs, electrodes were inserted in the muscles of the limbs to measure neuronal potential (ExcelTech Ltd., ExlTek Neuromax 1004). After electric stimulation of the cerebral motor cortex, the neural responses of the upper and the lower limbs were recorded. Decrease of more than 75% of the MEP amplitude was accepted as an indication of ischemic spinal cord dysfunction [24, 29]. MEP signal disappeared within 5 min in all animals as a sign of sufficient aortic occlusion. MEPs were triggered directly before aortic occlusion as well as 1 h, 2 h, 4 h, and 8 h after reperfusion.
In addition, spinal cord function was clinically evaluated by observing the movements of the upper and lower limbs in response to claw clamping during temporarily reduced anesthesia. The muscular response was classified as follows: 0 = no movement, 1 = muscular movement, 2 = joint movement, 3 = normal movement; an additional score of 4 was attributed if spontaneous movement was present even without stimulation by claw clamping. The reaction was measured before clamping (measuring point, MP1) and 1 h (MP2), 2 h (MP3), 4 h (MP4), and 8 h (MP5) after reperfusion. The reaction of the upper extremities was used to demonstrate the normal response.
Heart rate, MAP proximal, MAP distal, CVP, ITBVI, and CI were recorded as hemodynamic parameters. Arterial blood samples were collected to analyze blood gases, acid-base status, electrolytes, hemoglobin content, O2 saturation, and glucose levels.
Statistical analysis
All data are presented as median (interquartile range, IQR). A Mann-Whitney U test was performed for systemic hemodynamics, gas exchange, acid-base status, and histology. A p value of less than 0.05 was considered statistically significant. IBM SPSS Statistics software (Version 24.0.0.0) was used for statistical evaluation and graphical display.
Results
Mortality rates
All animals survived the experiments until the end of the observation period (reperfusion time, 8 h).
Hemodynamics, gas exchange, acid-base status
Table 1 presents data on systemic hemodynamics, gas exchange, acid-base status, and electrolytes. There were no statistically significant differences between the two groups.
Histology
Animals from all groups showed the physiological structure of the spinal cord. I/R injury caused accumulations of single reactive, predominantly mononuclear round cell/glial infiltrates, atherosclerotic alterations in arterioles/arteries, and slight swelling of the perikaryon of neurons in the anterior horn of the spinal cord (Fig. 1) of all animals. Two pigs from the vehicle group developed an infarct at both levels of the spinal cord. The cross sections presented edema, eosinophilic necrosis of ganglion cells, and motor neurons. The other animals of this group were without other pathological findings. One pig of the sulfide group showed an acute infarct with hypoxic necrosis of ganglion cells, endothelial cell damage, and edema in the lumbar and thoracic spinal cord. The remaining three animals from the sodium sulfide group were without other pathological findings.
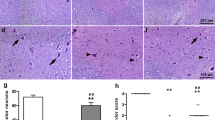
In preliminary experiments, it was shown that an increase in the clamping time resulted in an increase in the neuronal damage (data not shown). A clamping time of 45 min caused a damage of neurons in the thoracic and lumbar spinal cord (mean proportion of damaged neurons, 16.4% and 16.2%, respectively). Treatment with sodium sulfide did not reduce the damage of neurons. The mean percentage of damaged neurons in the anterior horn of the thoracic and lumbar spinal cord was 21.1% and 23.9%, respectively. The slight increase in the sodium sulfide group might be a result of the animal with the large active infarction (see above). There was no significant difference between the vehicle and the sodium sulfide group. Typical histological examples are demonstrated in Figs. 2 and 3.
Histology of the spinal cord of familial hypercholesterolemia Bretoncelles Meishan (FMB) pig. a Red frame marks swollen motor neuron with pyknotic nucleus indicating neuronal damage. b Red frames mark endothelial damage. c Red frames mark ischemic neurons with eosinophilic cytoplasm and darkened, shrunken nuclei. Blue frames indicate the formation of a vacuole within a neuron. d Red frames indicate hypoxic damage with eosinophilic gangliocyte necrosis
Motor evoked potentials (MEPs)
MEPs of the spinal cord were used to measure the extent of the damage of the spinal cord after ischemic damage. In the study groups, two animals of the vehicle group and one animal of the sodium sulfide group showed small but measurable MEPs at 2 and 4 h after balloon deflating. The function also got lost after 8 h of reperfusion.
Neurologic function
The clinical evaluation of the neurological function was evaluated at different time points. The reference at the upper extremities was always 7 points (3 points for normal reaction to claw clamping and 4 additional points for spontaneous movements). Furthermore, each animal showed maximal reflexes of the hind legs before balloon occlusion. In the sodium chloride group, only one animal showed link motions (2 points) at each time point during reperfusion. All other animals in both groups lost muscular reaction.
Discussion
The present study tested the hypothesis if a (pre-)treatment with sodium sulfide (Na2S) would reduce neuronal damage in a clinically relevant porcine model of thoracic aortic balloon occlusion-induced spinal cord I/R injury. However, treatment with intravenous Na2S had no protective effect on I/R injury of the spinal cord.
In this study, swine were investigated because of their striking anatomical and physiological similarity to humans [31]. Furthermore, most studies focusing on pathophysiology utilize young animals, without any cardiovascular disease background, even though these animals are clearly not reflective of the pathophysiology of our patient population. However, the existence of atherosclerotic plaques in the vasculature represents an important independent risk factor for abdominal aortic aneurysms [32]. Therefore, we used a recently described porcine model of ubiquitous human-like atherosclerosis that is closer to the clinical situation for the therapy of aortic aneurysm [11, 12]. These FBM pigs are a cross-bread of Rapacz farm pigs with smaller Chinese Meishan and French Bretoncelles strains. They are homologous for the R84 low-density lipoprotein (LDL) receptor mutation and feature human-like thin-cap fibroatheromas (TCFA) at a young age after an atherogenic diet as previously described [11, 12]. They also have altered gene expression, like a downregulated erythropoietin receptor (EPO-R) expression, a lower systemic endothelial NO (eNO) production, but higher renal eNO levels when compared to other pig strains [12]. The downregulated EPO-R may be related to inflammation and oxidative stress and is a putative mechanism of EPO resistance in patients with heart and kidney failure [33, 34]. These circumstances might have contributed to the result that there was no attenuation of the I/R injury during Na2S infusion, especially since multiple studies have noted that the therapeutic effect of H2S donation requires the presence of an intact eNO synthase system [35,36,37,38].
The duration of aortic occlusion was based on previous experiments and the clinical situation of thoracic aortic cross-clamping in open surgical repair. In a pig model, this ischemia had resulted in neuronal injury (5–15% of all motor neurons) in the spinal cord at 4 h of reperfusion [23]. In addition, 45 min of aortic occlusion prevented both the large spinal cord infarction over several segments reported in pigs after a clamping period of 60 min or longer [24] and the fairly mild tissue damage observed after only 30 min of clamping [26]. In our pigs with a pre-existing ubiquitous atherosclerosis, 45 min of ischemia and 8 h of reperfusion had resulted in the same extent of neuronal damage. Furthermore, half of the non-treated animals developed an infarct at both levels of the spinal cord and only one animal recovered partial neuronal function with regain of MEPs (Table 2) and link motions (Table 3) at each time point after reperfusion. The restriction in regaining neuronal function was also observed in a previous study using a pig model with the same balloon occlusion time [30].
This pig strain spontaneously develops hypothermia during anesthesia [12]. Core temperature was not externally influenced since hypothermia is an independent protective measurement possibly interfering with the effects of hydrogen sulfide [39, 40] and normothermia was not restored in order to avoid any pro-inflammatory and/or pro-apoptotic effects [41, 42].
The protective effects of compounds that release H2S endogenously on I/R injury are controversial. In porcine models of IR injury, Na2S exerted protective effects, such as maintaining mitochondrial function, neutralizing ROS and anti-inflammatory capacities, and reducing apoptosis especially in hearts and kidneys [5]. Administration of exogenous therapeutic Na2S prior to the onset of reperfusion after acute myocardial ischemia reduced the apoptotic response to I/R injury in a pig model [13]. In addition, its anti-inflammatory properties improved myocardial function and coronary microvascular reactivity by reducing infarct size [14, 15]. Ex vivo experiments of porcine kidneys, which were subjected to 25 min of warm ischemia and 18 h of cold storage under sulfide treatment, showed an improvement of renal function associated with a reduction of oxidative stress [43]. During porcine aortic occlusion-induced kidney I/R injury, pretreatment with Na2S attenuated tissue injury and organ dysfunction as a result of reduced inflammation and oxidative and nitrosative stress [27]. Administration of H2S in a large animal model of severe hemorrhagic shock resulted in a significant decrease in resuscitative requirements, decreased metabolic acidosis, and less end-organ histologic injury compared with standard resuscitation. On the other hand, it did not induce profound metabolic suppression as seen in rodents and appears to have alternative mechanisms of action in large animals, such as altered gene expression for hypoxia-inducible factor 1α (HIF 1α) and vascular endothelial growth factor receptor (VEGFr) [44]. In contrast, the present study showed that pretreatment with Na2S had no protective effect on the neuronal damage after aortic balloon occlusion in pigs. It could be speculated that the neuroprotection of sodium sulfide is dose-dependent. Current evidence seems to suggest that the presence of H2S in the ischemic brain may either be deleterious or protective depending on its concentration, deleterious when high and protective when low [45]. Deleterious actions include adversely influenced mitochondrial function, such as inhibited oxidative phosphorylation, as well as N-methyl-d-aspartate (NMDA) receptor and calcium-mediated cell death. H2S acts protective via its anti-inflammatory, anti-oxidative, and anti-apoptotic capacities [45]. Sulfide levels in our study were not measured because on the one hand sulfide interacts with numerous blood components (e.g., hemoglobin, iron, and dissolved oxygen) [46, 47]. For example, ex vivo spiking blood with defined amounts of sulfide does not allow for its quantitative recovery, so that sulfide administration in vivo may not necessarily yield detectable concentration changes unless toxic doses are used [48, 49]. In addition, it interferes with different reagents during chemical analysis, making it hard to measure accurate values. And a third point to be considered is that measured levels do not reflect the effect of the applied sulfide on the targeted cells or tissues. Different cells have different capacities to trap or oxidize sulfide. Especially cells with a high amount of metallo compounds or high expression of sulfide quinone reductase (e.g., hepatocytes or colonocytes) are immune against toxic sulfide levels whereas other cell types (e.g., cardiomyocytes or neurons) are more vulnerable [46, 47].
Limitations of the study
It could be argued that we did not achieve sufficiently high sulfide levels in the spinal cord tissue. After administration of 3 mg/kg NaSH in rats challenged with traumatic brain injury, a significant rise of sulfide levels in brain tissue could be measured by Jiang et al. [50], suggesting that the comparable amounts in our experiment also yielded sufficient tissue sulfide levels. Nevertheless, since we did not measure tissue sulfide concentrations, we cannot exclude insufficient adsorption into the spinal cord due to different pharmacokinetics.
A balloon occlusion time of 45 min has probably been too long for the integrity of the spinal cord, mediating an irreversible I/R injury. In surgical settings, a maximum of 30 min for the cross-clamping is needed to prevent spinal cord injury. Another major limitation of this study was the low sample size of the experimental animals. However, since there was no improvement of the neurological damage after sodium sulfide application, the experiments were stopped for ethical reasons according to the 3Rs of animal research [51].
Conclusion
In summary, in this porcine model of aortic occlusion-induced I/R injury, we demonstrated that pretreatment and continuous infusion with sodium sulfide did not protect spinal cord tissue from neuronal damage. Further studies are warranted to investigate the possible protective effects of different doses or other ways of application (e.g., inhalative), or other carriers of sulfide as sodium (e.g., chelates) on experimental models with pre-existing arteriosclerosis.
Abbreviations
- CVP:
-
Central venous pressure
- eNO:
-
Endothelial nitrogen oxide
- EPO-R:
-
Erythropoietin receptor
- FBM:
-
Familial hypercholesteremia Bretoncelles Meishan
- FiO2 :
-
Fraction of inspiratory oxygen
- H2S:
-
Hydrogen sulfide
- HE:
-
Hematoxylin and eosin
- HIF:
-
Hypoxia-inducible factor
- I/R:
-
Ischemia/reperfusion
- IQR:
-
Interquartile range
- IU:
-
International unit
- LDL:
-
Low-density lipoprotein
- MAP:
-
Mean arterial pressure
- MEP:
-
Motor evoked potential
- MOF:
-
Multi-organ failure
- MP:
-
Measuring point
- NaOH:
-
Sodium hydroxide
- NaSH:
-
Sodium hydrogen sulfide
- NMDA:
-
N-Methyl-d-aspartate
- PEEP:
-
Positive end-expiratory pressure
- ROS:
-
Reactive oxygen species
- TCFA:
-
Thin-cap fibroatheroma
- VEGFr:
-
Vascular endothelial growth factor receptor
References
Zammert M, Gelman S (2016) The pathophysiology of aortic cross-clamping. Best Pract Res Clin Anaesthesiol 30(3):257–269. https://doi.org/10.1016/j.bpa.2016.07.006
Alonso Pérez M, Llaneza Coto JM, Del Castro Madrazo JA et al (2017) Debranching aortic surgery. J Thorac Dis 9(Suppl 6):S465–S477. https://doi.org/10.21037/jtd.2017.03.87
Gelman S (1995) The pathophysiology of aortic cross-clamping and unclamping. Anesthesiology 82(4):1026–1060
Kimura H (2013) Physiological role of hydrogen sulfide and polysulfide in the central nervous system. Neurochem Int 63(5):492–497. https://doi.org/10.1016/j.neuint.2013.09.003
Guo W, J-t K, Cheng Z-y et al (2012) Hydrogen sulfide as an endogenous modulator in mitochondria and mitochondria dysfunction. Oxidative Med Cell Longev 2012:878052. https://doi.org/10.1155/2012/878052
Li L, H-k J, Y-p L et al (2015) Hydrogen sulfide protects spinal cord and induces autophagy via miR-30c in a rat model of spinal cord ischemia-reperfusion injury. J Biomed Sci 22:50
Aslami H, Schultz MJ, Juffermans NP (2009) Potential applications of hydrogen sulfide-induced suspended animation. Curr Med Chem 16(10):1295–1303
Wagner F, Asfar P, Calzia E et al (2009) Bench-to-bedside review: hydrogen sulfide--the third gaseous transmitter: applications for critical care. Crit Care 13(3):213. https://doi.org/10.1186/cc7700
Módis K, Bos EM, Calzia E et al (2014) Regulation of mitochondrial bioenergetic function by hydrogen sulfide. Part II. Pathophysiological and therapeutic aspects. Br J Pharmacol 171(8):2123–2146. https://doi.org/10.1111/bph.12368
Hartmann C, Nussbaum B, Calzia E et al (2017) Gaseous mediators and mitochondrial function: the future of pharmacologically induced suspended animation? Front Physiol 8:691. https://doi.org/10.3389/fphys.2017.00691
Thim T, Hagensen MK, Drouet L et al (2010) Familial hypercholesterolaemic downsized pig with human-like coronary atherosclerosis: a model for preclinical studies. EuroIntervention 6(2):261–268
Matějková Š, Scheuerle A, Wagner F et al (2013) Carbamylated erythropoietin-FC fusion protein and recombinant human erythropoietin during porcine kidney ischemia/reperfusion injury. Intensive Care Med 39(3):497–510. https://doi.org/10.1007/s00134-012-2766-y
Sodha NR, Clements RT, Feng J et al (2008) The effects of therapeutic sulfide on myocardial apoptosis in response to ischemia-reperfusion injury. Eur J Cardiothorac Surg 33(5):906–913. https://doi.org/10.1016/j.ejcts.2008.01.047
Sodha NR, Clements RT, Feng J et al (2009) Hydrogen sulfide therapy attenuates the inflammatory response in a porcine model of myocardial ischemia/reperfusion injury. J Thorac Cardiovasc Surg 138(4):977–984. https://doi.org/10.1016/j.jtcvs.2008.08.074
Osipov RM, Robich MP, Feng J et al (2009) Effect of hydrogen sulfide in a porcine model of myocardial ischemia-reperfusion: comparison of different administration regimens and characterization of the cellular mechanisms of protection. J Cardiovasc Pharmacol 54(4):287–297. https://doi.org/10.1097/FJC.0b013e3181b2b72b
Kuriyama T, Latham LP, Horwitz LD et al (1984) Role of collateral ventilation in ventilation-perfusion balance. J Appl Physiol Respir Environ Exerc Physiol 56(6):1500–1506
Nirmalan M, Willard TM, Edwards DJ et al (2005) Estimation of errors in determining intrathoracic blood volume using the single transpulmonary thermal dilution technique in hypovolemic shock. Anesthesiology 103(4):805–812
Papakostas JC, Matsagas MI, Toumpoulis IK et al (2006) Evolution of spinal cord injury in a porcine model of prolonged aortic occlusion. J Surg Res 133(2):159–166. https://doi.org/10.1016/j.jss.2005.10.007
Simon F, Scheuerle A, Gröger M et al (2011) Comparison of carbamylated erythropoietin-FC fusion protein and recombinant human erythropoietin during porcine aortic balloon occlusion-induced spinal cord ischemia/reperfusion injury. Intensive Care Med 37(9):1525–1533. https://doi.org/10.1007/s00134-011-2303-4
Blaisdell FW, Cooley DA (1962) The mechanism of paraplegia after temporary thoracic aortic occlusion and its relationship to spinal fluid pressure. Surgery 51:351–355
Wadouh F, Lindemann EM, Arndt CF et al (1984) The arteria radicularis magna anterior as a decisive factor influencing spinal cord damage during aortic occlusion. J Thorac Cardiovasc Surg 88(1):1–10
Weigang E, Luehr M, von Samson P et al (2005) Development of a special balloon occlusion device to prevent adverse events in high-risk patients during open aortic surgery. Eur Surg Res 37(4):204–209. https://doi.org/10.1159/000087864
Maier C, Scheuerle A, Hauser B et al (2007) The selective poly(ADP)ribose-polymerase 1 inhibitor INO1001 reduces spinal cord injury during porcine aortic cross-clamping-induced ischemia/reperfusion injury. Intensive Care Med 33(5):845–850. https://doi.org/10.1007/s00134-007-0585-3
Meylaerts SA, de Haan P, Kalkman CJ et al (2000) Prevention of paraplegia in pigs by selective segmental artery perfusion during aortic cross-clamping. J Vasc Surg 32(1):160–170. https://doi.org/10.1067/mva.2000.107571
Kick J, Hauser B, Bracht H et al (2007) Effects of a cantaloupe melon extract/wheat gliadin biopolymer during aortic cross-clamping. Intensive Care Med 33(4):694–702. https://doi.org/10.1007/s00134-006-0518-6
Maharajh GS, Pascoe EA, Halliday WC et al (1996) Neurological outcome in a porcine model of descending thoracic aortic surgery. Left atrial-femoral artery bypass versus clamp/repair. Stroke 27(11):2095–2100 discussion 2101
Simon F, Scheuerle A, Gröger M et al (2011) Effects of intravenous sulfide during porcine aortic occlusion-induced kidney ischemia/reperfusion injury. Shock 35(2):156–163. https://doi.org/10.1097/SHK.0b013e3181f0dc91
Duggal N, Lach B (2002) Selective vulnerability of the lumbosacral spinal cord after cardiac arrest and hypotension. Stroke 33(1):116–121
Meylaerts SA, de Haan P, Kalkman CJ et al (1999) The influence of regional spinal cord hypothermia on transcranial myogenic motor-evoked potential monitoring and the efficacy of spinal cord ischemia detection. J Thorac Cardiovasc Surg 118(6):1038–1045. https://doi.org/10.1016/S0022-5223(99)70099-1
Simon F, Scheuerle A, Calzia E et al (2008) Erythropoietin during porcine aortic balloon occlusion-induced ischemia/reperfusion injury. Crit Care Med 36(7):2143–2150. https://doi.org/10.1097/CCM.0b013e31817d7912
Bassols A, Costa C, Eckersall PD et al (2014) The pig as an animal model for human pathologies: a proteomics perspective. Proteomics Clin Appl 8(9–10):715–731. https://doi.org/10.1002/prca.201300099
Toghill BJ, Saratzis A, Bown MJ (2017) Abdominal aortic aneurysm-an independent disease to atherosclerosis? Cardiovasc Pathol 27:71–75. https://doi.org/10.1016/j.carpath.2017.01.008
van der Putten K, Braam B, Jie KE et al (2008) Mechanisms of disease: erythropoietin resistance in patients with both heart and kidney failure. Nat Clin Pract Nephrol 4(1):47–57. https://doi.org/10.1038/ncpneph0655
Stenvinkel P, Bárány P (2002) Anaemia, rHuEPO resistance, and cardiovascular disease in end-stage renal failure; links to inflammation and oxidative stress. Nephrol Dial Transplant 17(Suppl 5):32–37
Coletta C, Papapetropoulos A, Erdelyi K et al (2012) Hydrogen sulfide and nitric oxide are mutually dependent in the regulation of angiogenesis and endothelium-dependent vasorelaxation. Proc Natl Acad Sci U S A 109(23):9161–9166. https://doi.org/10.1073/pnas.1202916109
King AL, Polhemus DJ, Bhushan S et al (2014) Hydrogen sulfide cytoprotective signaling is endothelial nitric oxide synthase-nitric oxide dependent. Proc Natl Acad Sci U S A 111(8):3182–3187. https://doi.org/10.1073/pnas.1321871111
Bibli S-I, Szabo C, Chatzianastasiou A et al (2017) Hydrogen sulfide preserves endothelial nitric oxide synthase function by inhibiting proline-rich kinase 2: implications for cardiomyocyte survival and cardioprotection. Mol Pharmacol 92(6):718–730. https://doi.org/10.1124/mol.117.109645
Szabo C (2017) Hydrogen sulfide, an enhancer of vascular nitric oxide signaling: mechanisms and implications. Am J Physiol Cell Physiol 312(1):C3–C15. https://doi.org/10.1152/ajpcell.00282.2016
Inoue S, Mori A, Shimizu H et al (2013) Combined use of an epidural cooling catheter and systemic moderate hypothermia enhances spinal cord protection against ischemic injury in rabbits. J Thorac Cardiovasc Surg 146(3):696–701. https://doi.org/10.1016/j.jtcvs.2012.11.040
Tabayashi K, Motoyoshi N, Saiki Y et al (2008) Efficacy of perfusion cooling of the epidural space and cerebrospinal fluid drainage during repair of extent I and II thoracoabdominal aneurysm. J Cardiovasc Surg 49(6):749–755
Rocha-Ferreira E, Kelen D, Faulkner S et al (2017) Systemic pro-inflammatory cytokine status following therapeutic hypothermia in a piglet hypoxia-ischemia model. J Neuroinflammation 14(1):44. https://doi.org/10.1186/s12974-017-0821-x
Wang B, Armstrong JS, Lee J-H et al (2015) Rewarming from therapeutic hypothermia induces cortical neuron apoptosis in a swine model of neonatal hypoxic-ischemic encephalopathy. J Cereb Blood Flow Metab 35(5):781–793. https://doi.org/10.1038/jcbfm.2014.245
Hosgood SA, Nicholson ML (2010) Hydrogen sulphide ameliorates ischaemia-reperfusion injury in an experimental model of non-heart-beating donor kidney transplantation. Br J Surg 97(2):202–209. https://doi.org/10.1002/bjs.6856
Satterly SA, Salgar S, Hoffer Z et al (2015) Hydrogen sulfide improves resuscitation via non-hibernatory mechanisms in a porcine shock model. J Surg Res 199(1):197–210. https://doi.org/10.1016/j.jss.2015.04.001
Chan SJ, Wong PT-H (2017) Hydrogen sulfide in stroke: protective or deleterious? Neurochem Int 105:1–10. https://doi.org/10.1016/j.neuint.2016.11.015
Hughes MN, Centelles MN, Moore KP (2009) Making and working with hydrogen sulfide: the chemistry and generation of hydrogen sulfide in vitro and its measurement in vivo: a review. Free Radic Biol Med 47(10):1346–1353. https://doi.org/10.1016/j.freeradbiomed.2009.09.018
Haouzi P (2016) Is exogenous hydrogen sulfide a relevant tool to address physiological questions on hydrogen sulfide? Respir Physiol Neurobiol 229:5–10. https://doi.org/10.1016/j.resp.2016.03.015
Whitfield NL, Kreimier EL, Verdial FC et al (2008) Reappraisal of H2S/sulfide concentration in vertebrate blood and its potential significance in ischemic preconditioning and vascular signaling. Am J Physiol Regul Integr Comp Physiol 294(6):R1930–R1937. https://doi.org/10.1152/ajpregu.00025.2008
Furne J, Saeed A, Levitt MD (2008) Whole tissue hydrogen sulfide concentrations are orders of magnitude lower than presently accepted values. Am J Physiol Regul Integr Comp Physiol 295(5):R1479–R1485. https://doi.org/10.1152/ajpregu.90566.2008
Jiang X, Huang Y, Lin W et al (2013) Protective effects of hydrogen sulfide in a rat model of traumatic brain injury via activation of mitochondrial adenosine triphosphate-sensitive potassium channels and reduction of oxidative stress. J Surg Res 184(2):e27–e35. https://doi.org/10.1016/j.jss.2013.03.067
Russell WMS, Burch RL (1992) The principles of humane experimental technique, Chapter 4, Special ed. UFAW, Potters Bar http://altweb.jhsph.edu/pubs/books/humane_exp/chap4d
Acknowledgements
This work was supported by the German Research Foundation (DFG) within the funding program Open Access Publishing.
Funding
This work was supported by the German Research Foundation (DFG) within the funding program Open Access Publishing.
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Contributions
FS, PR, and HS conceived the study and designed the experiment. FS and MW were responsible for the anesthesia and surgery and together with AB and KL for the data collection and statistical analysis. AB, OM, and AS were responsible for the histology. CS provided the intravenous formulation of hydrogen sulfide. AB, KL, and MW drafted the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The experiments were performed in adherence with the National Institutes of Health Guidelines on the use of Laboratory Animals and after approval of the protocol by the regional council of Tübingen (Registration number 905).
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interest.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Bredthauer, A., Lehle, K., Scheuerle, A. et al. Intravenous hydrogen sulfide does not induce neuroprotection after aortic balloon occlusion-induced spinal cord ischemia/reperfusion injury in a human-like porcine model of ubiquitous arteriosclerosis. ICMx 6, 44 (2018). https://doi.org/10.1186/s40635-018-0209-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40635-018-0209-y