Abstract
Background
Burnout is a syndrome that result from chronic workplace stress and it characterized by emotional exhaustion, depersonalization and low personal accomplishments. Studies report higher burnout levels in medical personnel compared to the general population. Workplace burnout has been directly linked to medical errors and negative coping strategies such as substance abuse. The aims of this study were to assess the level of burnout in medical residents, evaluate their impressions about coping mechanisms and assess perceived impact on patient care in a low/ middle income country setting.
Methods
This was a cross sectional, mixed methods survey carried out at Aga Khan University, Nairobi Kenya. The Maslach Burnout Inventory - Human Services Survey was used to assess the level of burnout. High-risk scores for each subscale are defined as > 27 in emotional exhaustion, > 10 in depersonalization, and < 33 in personal accomplishment. Overall high risk of burnout was defined as high-risk scores in 2 or more of the 3 categories. Categorical variables were analysed using descriptive statistics and reported as frequency counts and corresponding percentages. Chi-square test was applied to test for association of burnout and the categorical variables. P value of < 0.05 was considered statistically significant. To assess the impressions on patient care and evaluate the coping mechanisms employed in the context of burnout residents participated in four focus group discussions reaching thematic saturation.
Results
95 out of 120 residents consented to participate in the study, 47.3% of whom had a high risk of burnout. A significant association was found between gender and burnout risk with more female residents having high risk of burnout compared to their male counterparts; 58.0% and 35.6% respectively (P value 0.029). Residents in paediatrics and child health had the greatest risk of burnout (8 out of 10) compared to those in other programmes (P value of 0.01). Thematic analysis from focus group discussions revealed that main sources of stress included departmental conflict and struggle to balance work and other aspects of life. All focus group discussions revealed that burnout and stress are associated with negative coping mechanisms. Respondents reported that when under stress, they felt more likely to make medical errors.
Conclusion
This study reported high risk of burnout among post graduate residents which is consistent with other global studies. The sources of stress cited by residents were mostly related to the workplace and many perceived sub-optimal patients care resulted from burnout. This highlights a need for preventive measures such as wellness programs within the training programmes.
Trial registration number
Not applicable.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Introduction
Burnout is a psychological syndrome in response to long term occupational stressors. It manifests as emotional exhaustion, depersonalization and a low sense of personal accomplishment [1].
High level of burnout is reported in people whose occupation involves human services such as health care workers, police officers and teachers. It is thought to be due to chronic workplace stress that has not been successfully managed or the result of work-home conflict [1]. For medical personnel, this could also be attributed to factors such as struggles with work life integration and longer working hours [2]. This has been linked to documented lapses in professionalism, absenteeism, self-reported delivery of sub-optimal patient care, and medical errors [3].
When compared to consultants or undergraduate medical students, medical residents were reported to have higher rates of burnout. This may be attributed to long working hours and an expectation to exponentially increase knowledge base [4]. Even with these high expectations, residents may still feel a lack of autonomy in patient management as the ultimate responsibility rests with the consultant. Residents may also struggle to balance social, work and study life [5].
Coping describes a change in an individual’s thoughts and behavior to deal with demands that are above their capability and may be active or passive [6]. Active coping strategies such as physical activity and prayer are behavioral or psychological actions that are intentionally aimed at altering the thought or nature of a stressor. Passive coping strategies such as substance abuse are those that lead people into activities geared towards avoidance or withdrawal from the stressor [7] .
Wellness in trainees and residents is an emerging area of focus for post graduate medical education (PGME) programs worldwide. Studies to explore the extent and effect of wellness programmes on burnout in medical residents are on-going in high income countries [4]. In low/ middle income countries, there is limited literature on the burnout syndrome. We aimed to study extent of burnout in post graduate medical residents, coping mechanisms and their perception of impact on patient care.
Methods
We conducted a cross sectional survey and invited all post graduate medical residents at Aga Khan University Teaching Hospital, Nairobi using a mixed method approach from August 2019 to December 2019. At the time of the study, there were 120 residents in all the programmes with each four-year programme having 4 residents per year of training.
Quantitative methodology
Data collection methods and tools
To assess the level of burnout, the Maslach Burnout Inventory- Human Services Survey was used. This inventory is the gold standard assessment tool for the burnout syndrome because of its validity especially when used for human service workers. It also has clearer cut off points for risk of burnout than the other tools [8]. It is a validated 22-item questionnaire with each item scored using a 7-point Likert scale. Over a period of four months starting 1st August 2019 until 30th November 2019, all the 120 medical residents were invited by email to participate in the study using the global residents mailing list. A consent form and study questionnaire were attached to the email and those who agreed to participate returned the questionnaire. Ninety-five residents completed and returned questionnaires. Each participant was identified using a code and no personal identifying data that could breach confidentiality were published or made available to the institution. For this study, comparison was made to a study which had a similar sample population and sample size [9] .
Quantitative statistical analysis
The prevalence of burnout among participants was determined from the Maslach Burnout Inventory categorization of high or low risk of burnout [1]. It is a widely validated tool and suitable to measure burnout risk levels in health care workers in different populations. It also has clearer cut off points for burnout risk when compared to other tools used to measure burnout. Each participant received a score after filling out the questionnaire that grouped them into either, low or high risk of burnout. A seven-point Likert scale was used to score each item. It looks at the three aspects of burnout including emotional exhaustion (9 questions), depersonalization (5 questions), and personal accomplishment (8 questions). High-risk scores for each subscale are defined as > 27 in emotional exhaustion, > 10 in depersonalization, and < 33 in personal accomplishment. Overall high risk of burnout was defined as high-risk scores in 2 or more of the 3 categories.
Besides determining the global prevalence of burnout in the overall study population, we also assessed respondents from each programme of study and compared level of burnout between departments.
Data were analyzed using SPSS version 22. Categorical variables were analysed using descriptive statistics and reported as frequency counts and corresponding percentages. Chi-square test was applied to test for association of burnout and the categorical variables. P value of < 0.05 was considered statistically significant. It was estimated that for a population prevalence of 50% burnout, a sample size of 95 participants would achieve 80% power for the primary outcome measure.
The study was approved by the Aga Khan University Research and Ethics Committee (Ref: 2019/REC − 37 (v3)).
Qualitative methodology
Data collection methods and tools
Following purposive sampling i.e., inviting participants who filled out the Maslach questionnaire from each department and each year of study, focus group discussions were conducted to assess the perceived impression on patient care and evaluate the coping mechanisms employed in the context of burnout. They were used to attain a more in-depth insight into the research topic as they facilitated generation of a large amount of information from a small group of people [10]. 50 participants from the quantitative aspect of the study were approached for the FGD, 27 of whom agreed to participate.
There were four focus group discussions (FGDs) with an average of 6–8 participants during which thematic saturation was obtained. This is the recommended number as thematic saturation is usually obtained after 3–4 focus group discussions. The FGDs had one-off discussions lasting up to 1 h, that expounded on the 2 themes centered around coping mechanisms namely problem focused coping and emotion focused coping.
Focus group discussions were facilitated and recorded by the principal investigator and helped by a research assistant who took notes on non-verbal cues for contextual information during transcription.
Reflexivity was was acknowledged and its effect mitigated by having the transcripts listened to by the other researchers at the decoding stage. Themes were therefore agreed to jointly by all the researchers at the end of the study. The first FGD was taken as a pretest to help refine the process. The feedback helped generate a more suitable question schedule to get the best out of the actual FGDs.
Qualitative analysis
Thematic framework analysis was used for data-gathering and analysis from FGD using NVivo 12 software. This allowed concepts and categories to emerge from the data (Ritchie, 1994). The following techniques were used to develop themes derived from the focus group discussions including familiarization, identifying a thematic framework, indexing, charting & mapping and interpretation (Ritchie, 1994).
Results
Quantitative aspect of the study
Social and demographic factors
Table 1 shows the social and demographic characteristics of the respondents. Of the 95 respondents, 50 (52.6%) were female. There were more respondents in their third year of study (32 out of 95 respondents) compared to those in other study years. There was no significant difference in the distribution of participants within various study programmes.
Level of burnout
There were nearly as many respondents who had a composite score of high risk compared to those with a low risk of burnout 45 (47.37%) and 50 (52.63%) respectively.
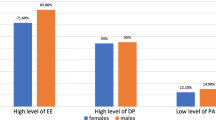
Correlation between demographic and work characteristic variables and level of burnout is shown in Table 2. A higher risk of burnout was seen in female residents compared to their male counterparts ,29 out of 50 (58.0%) and 16 out of 45 (35.6%) respectively, P value of 0.029.
The department of Pediatrics and Child Health had the highest proportion of high risk of burnout at 81.8% with Obstetrics and Gynaecology reporting the lowest risk of burnout at 7.1%. This was statistically significant (P value < 0.01).
The risk of burnout did not vary significantly between different study years among residents from various programmes.
Qualitative aspect of the study
Using purposive sampling 50 participants from the quantitative aspect of the study were approached for the FGD, 27 of whom agreed to participate (Table 3). Four focus group discussions were held with 6–8 members per group. Three main themes emerged as sources of stress, active and passive coping mechanisms and effects of stress and burnout on patient care as outlined in Table 4.
Sources of stress
Participants frequently described conflict in their work environment as a major contributor to burnout. They described departmental conflict and lack of support from consultants as stressors. The tension between consultants over a patient, or differences between residents in the same department were cited. The participants also mentioned a lack of support from the consultants that contributed to stress, increased expectations from patients and hospital leadership, barriers to teamwork, and little appreciation for their work.
‘stressed consultants when the consultant is stressed out sometimes umm you maybe at the receiving end of that. they don’t realize you’re also stressed’ (FGD 1).
Several participants cited adverse outcomes in patients as contributing to stress and burnout.
‘A patient’s outcome can add to your stress when things don’t go as you expect or when things tend to change suddenly, then that outcome can remain in your mind for a while’ (FGD 3).
Other participants mentioned angry or uncooperative patients and/or their guardians as negatively impacting them.
‘it’s very different then how you talk to a patient after you’ve undergone some kind of stress or trauma and the patient is angry because maybe they have their own issues but for you, you’re like how can you be angry for waiting for 20 minutes, you don’t even know what I’ve come through’ (FGD 1).
Many of the participants talked about the struggle to balance their clinical and academic work stating that expectations from both academic and clinical work are high and time demanding. Family demands on time and finances also weighed heavily on many participants.
‘I don’t think we have protective time; we get like two days leave, and that’s where you have to balance your family life, your personal life, work life, your study, and all that in 24 hours you can’t fit all that’ (FGD 4).
Several participants described long working hours, inefficient hospital systems and work-related illnesses as significant sources of stress.
‘also working long hours in the facility yes, I could say it’s part of the sources of my stress.’ (FGD 2).
‘a lot of is still built in the systems that are failing us, the networks that are failing themselves this is reflecting down on us, so for me those ones are the biggest stress’ (FGD 1).
‘we have come into terms and conditions we didn’t have before like umm someone with chronic back pain, chronic pain and that actually because of the fatigue it’s like a vicious cycle’ (FGD 4).
Coping mechanisms
There were several passive coping methods that participants resorted to when stressed or burnt out. These coping methods are viewed as emotion based and included avoidance, behavioral dissociation, drinking alcohol and distancing oneself from the stressful situation.
‘I’ll go home have a drink and in the process of having the drink, you kind of forget’ (FGD 1).
‘I withdraw myself; I try withdraw myself emotionally and physically’ (FGD 2).
Other participants highlighted active coping methods that are also viewed as problem solving methods. These included venting, talking to mentors, social support, socializing, problem solving, physical activity, hobbies, time off and prayer.
‘I play football or jog immediately after work so that has really helped especially in the first few years of residency’ (FGD 4).
‘good support system especially like at home when you have good friends’ (FGD 1).
Perceived effects on patient care
As a result of burnout, many participants described apathy emerging as a result. This was characterized by lack of empathy, spending less time with patients and early discharge of cold cases.
‘you did in fact prematurely discharge this patient but just because you had 60 patients and you can’t go through each patient for half an hour’ (FGD 3).
A few participants described various types of medical errors that could occur because of burnout. Error in diagnosis was observed in both clinical and non-clinical participants.
‘when it finds you at the peak of the stressful moment, chances are that you might report something the opposite way’ (FGD 4).
Other participants described omission and medication errors which would occasionally occur under stress.
‘you receive a call from pharmacy there like you, you have had a long day, it’s supposed to be oral not subcutaneous, so at least now the good thing the mechanisms the hospital catches these errors but yes as a result especially of stress and that burnout you can actually make mistakes’ (FGD 1).
Defensive practices arise because of feeling overwhelmed which may lead to various actions. Many participants described ordering many and sometimes not needed diagnostic tests during stressful situations. They also discussed treating patients for a generalizable diagnosis.
‘you’d rather ask for more tests than ask for less tests cause if you miss something again it’s an issue and then you also don’t want to see this patient, you want to just, maybe your time is up, you just want to kind of do the tests, so that you don’t review the patient another person to come and review the patient’ (FGD 1).
Discussion
The prevalence of burnout in this study was 47.3%, which is similar to that reported in studies of postgraduate residents elsewhere. A systematic review on prevalence of burnout globally showed a range between 17.6 and 76.0% [11]. A study reported from Wayne State University School of Medicine showed a prevalence rate of 50% among medical residents in different specialties [12]. From a low-middle income country context, 74% of residents reported high levels of burnout in at least one sub-scale [13]. Doctors in residency training are particularly vulnerable to burnout and stress. This may be due to the pressure of having to become competent clinicians, academicians and administrators at completion of training for a prescribed period of time [14]. These experiences are similar for residents in high as well as low-middle income countries, as detailed in a systematic review done for studies looking at Sub-Saharan African healthcare workers [4].
Contrary to previous studies that didn’t show any significant association between gender and risk of burnout, this study showed a significant association between gender and burnout risk. Female residents were found to have a higher risk of burnout when compared to their male counterparts. This may be due to a bigger work-life conflict in females compared to males as seen in a Norwegian study on physicians [15] The study found that male physicians tended to have spouses who worked part time or were full time home makers while their female counterparts had spouses who worked full time which led to more responsibility at work and at home. This theory is supported by a similar study done in Karachi that looked at stress factors affecting female and male doctors [16]. Although differences in sources of stress, and their impact on patient care between genders were not explored specifically in this current study, it can be postulated that female healthcare workers may have greater childcare and other responsibilities outside their work-role. This may, result in a stronger work-life conflict and leading to a higher incidence of burnout.
This study showed that Paediatrics and Child Health residents had higher levels of burnout followed closely by General Surgery and Anaesthesia residents. This is similar to findings from a study in Nigeria that reported the highest risk of burnout in residents in the departments of Surgery and Paediatrics and Child Health at 77.8% and 70.6% respectively [9]. These findings were also supported by a systematic review done on Arab literature for burnout in healthcare workers [17]. The same study postulated that the higher risk of burnout seen in General Surgery and Anaesthesia healthcare workers was due to the greater case load compared to other specialties and the reality of having to manage complex cases [17]. High burnout in Paediatrics and Child Health residents may also be attributed to their additional interaction with stressed and anxious parents of sick children.
Long working hours has been cited as contributing to risk of burnout in many studies done on post graduate residents. This was a recurring theme in all focus group discussions in our study. A global study of neurosurgery residents showed that spending every other night on call and having no limits of consecutive hours worked were significantly associated with high levels of burnout [18]. A study done at Wayne State University showed that risk of burnout increased with increasing number of working hours [12]. This study showed that after implementation of reduction of working hours, there was a significant decrease in the level of burnout among residents in different specialties. Similar findings on burnout and working hours have been reported in lower/ middle income countries though two studies done in Pakistan and Nigeria showed that heavy workload as opposed to long working hours was more associated with burnout [9, 13].
Long working hours subsequently limit the amount of time residents have with their families and friends. This is known as the work-home interference and has often been described as the heart of the burnout syndrome [19]. Many respondents described a lack of balance between work and life as a component of stress. They explained that their families suffer as they hardly give them quality time and attention. Similar sentiments were shared by doctors in Yemen who described conflict between home/family life and work as significant contributors to burnout [20].
In this study, respondents from all focus groups cited lack of support from consultants and departmental conflict as a significant source of stress and burnout. The departmental conflict was mainly seen as personality differences between members of the department which led to conflict and a tense working environment. As seen in a study on residents in Wayne State University, 65% of residents who were experiencing burnout described dissatisfaction with clinical faculty as a major stressor [18]. This conflict may result in degraded mentorship during residency training.
It is interesting to frame the results of this study in the broader context of a job stress model such as the Bakker and Demerouti Job Demands-Resources model [21]. This model predicts the development of burnout in human services employees from a specific set of occupational conditions. In the absence of job resources such as participation in decision-making, self-development and supervisor support, high levels of disengagement in employees can be predicted. When job demands such as high workload, time pressure and shift working are present, the model predicts employee exhaustion. The findings of our study denote a constellation of both job demands and a lack of job resources which, predictably, result in the emotional exhaustion, depersonalization and reduced effectiveness described by the study participants [1, 21].
Though the factors identified in this study are interesting and can be a starting point for measures to mitigate burnout among residents, a note of caution should be sounded. This is a cross-sectional study with relatively low sample size, and a direct causal relationship between burnout and the identified sources of stress cannot be inferred from these findings. Further research, using experimental, quasi-experimental or causal inference methodological approaches that allow causal analysis may be more revealing. Whereas burnout may be common among healthcare workers, the manifestations may be varied among individuals. This shows that some individuals may thrive in the same apparently stressful working environment. One factor thought to influence the likelihood of burnout is the coping mechanisms of an individual [22].
Coping mechanisms can be divided into two distinct groups, active and passive coping [2]. Various methods of active coping were described in the focus group discussions mainly physical activity, prayer, and social support at work. In a study looking at Emergency care nurses in Detroit, the authors found that task-oriented methods were linked to significantly low levels of burnout compared to emotion based coping methods such as avoidance [22]. Similarly, a study looking at Internal Medicine residents found that active coping mechanisms, particularly prayer and meditation were associated with lower levels of burnout [23],
In all focus group discussions, respondents highlighted apathy to patients and medical errors as consequences of burnout. They highlighted early discharge of cold cases and diagnostic or prescription errors particularly when feeling stressed or overwhelmed. These views are supported by a study reported on Internal Medicine residents in Washington which showed a significant association between high levels of burnout and sub-optimal patient care practices. These practices included discharging patients to make the service manageable, making prescription and diagnostic errors that are not due to lack of knowledge and having little or no emotional reaction to the death of a patient [3].
Several respondents in all focus group discussions talked about giving blanket diagnoses while ordering for general tests to ‘buy time’ and hopefully manage a patient’s condition without having to spend too much time with one patient. According to the respondents, these practices are consequences of long working hours and lack of support.
The study gains strength from the high response rate of 79%. The use of a universally applicable, validated assessment tool for burnout and the mixed methodological approach renders further strength to the study findings.
However, the cross-sectional nature of the study, the relatively small overall sample size, and the low number of participants in the sub-groups analysis mandates cautious interpretation of the findings. A causal relationship between sources of stress and burnout and its consequences cannot be imputed.
Consequent to this study, the authors suggest more in-depth research on the topic, in this setting. Further, they propose that residents should have regular education and discussions about burnout, its symptoms and how to mitigate its effects on their social, psychological and educational lives. Measures to promote resilience and well-being should be put in place.
Conclusion
This study reports a significant risk of burnout amongst post graduate residents in a low-middle income African country. This information creates awareness of the emerging burden of occupational mental health issues in lower-middle income countries where research on burn out in medical residents is scarce. It also confirmed that negative coping mechanisms linked to high levels of burnout may negatively affect patient care with potential adverse effects.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Maslach C, Schaufeli WB, Leiter MP. Job burnout. Annu Rev Psychol. 2001;52:397–422.
Shanafelt TD, Hasan O, Dyrbye LN, Sinsky C, Satele D, Sloan J et al. Changes in Burnout and Satisfaction With Work-Life Balance in Physicians and the General US Working Population Between 2011 and 2014. Mayo Clin Proc. 2015;90(12):1600-13.
Shanafelt TD, Bradley KA, Wipf JE, Back AL. Burnout and self-reported patient care in an internal medicine residency program. Ann Intern Med. 2002;136(5):358–67.
Busireddy KR, Miller JA, Ellison K, Ren V, Qayyum R, Panda M. Efficacy of interventions to reduce Resident Physician Burnout: a systematic review. J Grad Med Educ. 2017;9(3):294–301.
Ríos A, Sánchez Gascón F, Martínez Lage JF, Guerrero M. Influence of residency training on personal stress and impairment in family life: analysis of related factors. Med Princ Pract. 2006;15(4):276–80.
Menaldi SL, Raharjanti NW, Wahid M, Ramadianto AS, Nugrahadi NR, Adhiguna G, et al. Burnout and coping strategies among resident physicians at an Indonesian tertiary referral hospital during COVID-19 pandemic. PLoS ONE. 2023;18(1):e0280313.
Ceslowitz SB. Burnout and coping strategies among hospital staff nurses. J Adv Nurs. 1989;14(7):553–8.
Maslach C, Jackson SE, Leiter MP, Zalaquett C, Wood R. Evaluating stress: a book of resources. USA: Scarecrow; 1997.
Ogundipe OA, Olagunju AT, Lasebikan VO, Coker AO. Burnout among doctors in residency training in a tertiary hospital. Asian J Psychiatr. 2014;10:27–32.
Hennink MM, Kaiser BN, Weber MB. What influences saturation? Estimating sample sizes in Focus Group Research. Qual Health Res. 2019;29(10):1483–96.
Prins JT, Gazendam-Donofrio SM, Tubben BJ, van der Heijden FM, van de Wiel HB, Hoekstra-Weebers JE. Burnout in medical residents: a review. Med Educ. 2007;41(8):788–800.
Martini S, Arfken CL, Churchill A, Balon R. Burnout comparison among residents in different medical specialties. Acad Psychiatry. 2004;28(3):240–2.
Zubairi AJ, Noordin S. Factors associated with burnout among residents in a developing country. Ann Med Surg (Lond). 2016;6:60–3.
Dyrbye LN, West CP, Satele D, Boone S, Tan L, Sloan J, et al. Burnout among U.S. medical students, residents, and early career physicians relative to the general U.S. population. Acad Med. 2014;89(3):443–51.
Innstrand ST, Langballe EM, Espnes GA, Aasland OG, Falkum E. Personal vulnerability and work-home interaction: the effect of job performance-based self-esteem on work/home conflict and facilitation. Scand J Psychol. 2010;51(6):480–7.
Khuwaja AK, Qureshi R, Andrades M, Fatmi Z, Khuwaja NK. Comparison of job satisfaction and stress among male and female doctors in teaching hospitals of Karachi. J Ayub Med Coll Abbottabad. 2004;16(1):23–7.
Elbarazi I, Loney T, Yousef S, Elias A. Prevalence of and factors associated with burnout among health care professionals in arab countries: a systematic review. BMC Health Serv Res. 2017;17(1):491.
Jean WC, Ironside NT, Felbaum DR, Syed HR. The impact of work-related factors on risk of Resident Burnout: A Global Neurosurgery Pilot Study. World Neurosurg. 2020;138:e345–53.
Shanafelt TD, Sloan JA, Habermann TM. The well-being of physicians. Am J Med. 2003;114(6):513–9.
Al-Dubai SA, Rampal KG. Prevalence and associated factors of burnout among doctors in Yemen. J Occup Health. 2010;52(1):58–65.
Bakker AB, Demerouti E. The job demands-resources model: state of the art. J Managerial Psychol. 2007;22(3):309–28.
Howlett M, Doody K, Murray J, LeBlanc-Duchin D, Fraser J, Atkinson PR. Burnout in emergency department healthcare professionals is associated with coping style: a cross-sectional survey. Emerg Med J. 2015;32(9):722–7.
Doolittle BR, Windish DM, Seelig CB. Burnout, coping, and spirituality among internal medicine resident physicians. J Grad Med Educ. 2013;5(2):257–61.
Acknowledgements
We are appreciative of James Orwa who assisted with statistical analysis and other technical aspects.
Funding
Funding for the research was provided by the Aga Khan University Teaching Hospital.
Author information
Authors and Affiliations
Contributions
C.M contributed to the conception and design of the study and substantial revision of the initial manuscript. E.O. contributed to the conception of the conception and design of the study, data collection, analysis and drafting of the initial manuscript. D.K contributed to the conception, design and review of the manuscript. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Aga Khan University Research and Ethics Committee (Ref: 2019/REC − 37 (v3)) and informed consent was granted by all the participants.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it.The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Muteshi, C., Ochola, E. & Kamya, D. Burnout among medical residents, coping mechanisms and the perceived impact on patient care in a low/ middle income country. BMC Med Educ 24, 828 (2024). https://doi.org/10.1186/s12909-024-05832-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12909-024-05832-1