Abstract
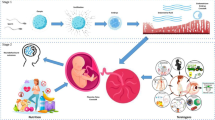
Hypertensive Disorders of Pregnancy (HDsP) remain leading causes of maternal and perinatal morbidity and mortality. Growing evidence suggests the involvement of epigenetic factors, such as gene-specific and global DNA methylation changes, both in the etiology and as an effect of HDsP. In this study, we investigated the potential association between placental DNA methylation status in selected CpGs of HSD11B2 cortisol level controlling gene, RUNX3 tumor suppressor gene, and long interspersed nucleotide element-1 (LINE-1) repetitive elements and HDsP—preeclampsia (PE), gestational hypertension (GH), and chronic hypertension (CH). Methylation-specific polymerase chain reaction (MSP) and pyrosequencing (PSQ) were used to analyze placental DNA methylation. Plasma and urine cortisol and cortisone levels were measured using high performance liquid chromatography with fluorescence detection (HPLC-FLD), whereas serum progesterone level was determined by electrochemiluminescence immunoassay. The mean percentage of HSD11B2, RUNX3, and LINE-1 methylation was not altered in the placentas of patients with HDsP, as compared to the controls. However, among patients from PE, GH, and CH groups, several significant correlations were observed between the methylation status of HSD11B2, RUNX3, or LINE-1 and children’s birth weight, gestational age at delivery, mother’s age, and body mass index as well as hormones levels. These results indicate lack of association between methylation status of HSD11B2, RUNX3, or LINE-1 repetitive elements and HDsP. However, association of these parameters with some clinical variables may suggest the role of placental DNA methylation in fetal development and should be further explored.
Similar content being viewed by others
References
Bird A. Perceptions of epigenetics. Nature. 2007;447(7143):396–398.
Wadhwa PD, Buss C, Entringer S, Swanson JM. Developmental origins of health and disease: brief history of the approach and current focus on epigenetic mechanisms. Semin Reprod Med. 2009;27(5):358–368.
Friso S, Carvajal CA, Fardella CE, Olivieri O. Epigenetics and arterial hypertension: the challenge of emerging evidence. Transl Res. 2015;165(1):154–165.
Julian CG, Pedersen BS, Salmon CS, et al. Unique DNA methylation patterns in offspring of hypertensive pregnancy. Clin Transl Sci. 2015;8(6):740–745.
World Health Organization. WHO Recommendations for Prevention and Treatment of Pre-Eclampsia and Eclampsia. Geneva, Switzerland: World Health Organization; 2011.
Roberts CL, Ford JB, Algert CS, et al. Population-based trends in pregnancy hypertension and pre-eclampsia: an international comparative study. BMJ Open. 2011;1(1):e000101. doi:10.1136/ bmjopen-2011-000101.
Foo L, Tay J, Lees CC, McEniery CM, Wilkinson IB. Hypertension in pregnancy: natural history and treatment options. Curr Hypertens Rep. 2015;17(5):36.
Tuovinen S, Eriksson JG, Kajantie E, Räikkönen K. Maternal hypertensive pregnancy disorders and cognitive functioning of the offspring: a systematic review. J Am Soc Hypertens. 2014;8(11):832–847.
Anton L, Brown AG, Bartolomei MS, Elovitz MA. Differential methylation of genes associated with cell adhesion in preeclamptic placentas. PLoS One. 2014;9(6):e100148. doi:10.1371/journal.pone.0100148.
Chu T, Bunce K, Shaw P, et al. Comprehensive analysis of preeclampsia-associated DNA methylation in the placenta. PLoS One. 2014;9(9):e107318. doi:10.1371/journal.pone.0107318.
Nomura Y, Lambertini L, Rialdi A, et al. Global methylation in the placenta and umbilical cord blood from pregnancies with maternal gestational diabetes, preeclampsia, and obesity. Reprod Sci. 2014;21(1):131–137.
Appleton AA, Armstrong DA, Lesseur C, et al. Patterning in placental 11-B hydroxysteroid dehydrogenase methylation according to prenatal socioeconomic adversity. PLoS One. 2013;8(9):e74691. doi:10.1371/journal.pone.0074691.
Marsit CJ, Maccani MA, Padbury JF, Lester BM. Placental 11-beta hydroxysteroid dehydrogenase methylation is associated with newborn growth and a measure of neurobehavioral outcome. PLoS One. 2012;7(3):e33794. doi:10.1371/journal.pone.0033794.
Alikhani-Koopaei R, Fouladkou F, Frey FJ, Frey BM. Epigenetic regulation of 11 beta-hydroxysteroid dehydrogenase type 2 expression. J Clin Invest. 2004;114(8):1146–1157.
Hu W, Weng X, Dong M, Liu Y, Li W, Huang H. Alteration in methylation level at 11ß-hydroxysteroid dehydrogenase type 2 gene promoter in infants born to preeclamptic women. BMC Genet. 2014;15:96.
Dy J, Guan H, Sampath-Kumar R, Richardson BS, Yang K. Placental 11beta-hydroxysteroid dehydrogenase type 2 is reduced in pregnancies complicated with idiopathic intrauterine growth restriction: evidence that this is associated with an attenuated ratio of cortisone to cortisol in the umbilical artery. Placenta. 2008;29(2):193–200.
Causevic M, Mohaupt M. 11beta-Hydroxysteroid dehydrogenase type 2 in pregnancy and preeclampsia. Mol Aspects Med. 2007;28(2):220–226.
Gao WL, Li D, Xiao ZX, et al. Detection of global DNA methylation and paternally imprinted H19 gene methylation in preeclamptic placentas. Hypertens Res. 2011;34(5):655–661.
Kulkarni A, Chavan-Gautam P, Mehendale S, Yadav H, Joshi S. Global DNA methylation patterns in placenta and its association with maternal hypertension in pre-eclampsia. DNA Cell Biol. 2011;30(2):79–84.
Wilhelm-Benartzi CS, Houseman EA, Maccani MA, et al. In utero exposures, infant growth, and DNA methylation of repetitive elements and developmentally related genes in human placenta. Environ Health Perspect. 2012;120(2):296–302.
Zhao Y, Shi HJ, Xie CM, Chen J, Laue H, Zhang YH. Prenatal phthalate exposure, infant growth, and global DNA methylation of human placenta. Environ Mol Mutagen. 2015;56(3):286–292.
Maccani JZ, Maccani MA. Altered placental DNA methylation patterns associated with maternal smoking: current perspectives. Adv Genomics Genet. 2015;2015(5):205–214.
Januar V, Desoye G, Novakovic B, Cvitic S, Saffery R. Epigenetic regulation of human placental function and pregnancy outcome: considerations for causal inference. Am J Obstet Gynecol. 2015;213(suppl 4):S182–S196.
Majchrzak-Celińska A, Paluszczak J, Szalata M, Barciszewska AM, Nowak S, Baer-Dubowska W. DNA methylation analysis of benign and atypical meningiomas: correlation between RUNX3 methylation and WHO grade. J Cancer Res Clin Oncol. 2015;141(9):1593–1601.
Majchrzak-Celińska A, Paluszczak J, Szalata M, et al. The methylation of a panel of genes differentiates low-grade from highgrade gliomas. Tumour Biol. 2015;36(5):3831–3841.
Maccani JZ, Koestler DC, Houseman EA, Marsit CJ, Kelsey KT. Placental DNA methylation alterations associated with maternal tobacco smoking at the RUNX3 gene are also associated with gestational age. Epigenomics. 2013;5(6):619–630.
Gadzinowski J, Kaliszewska-Drozdowska MD, Kosińska M, Mazela J, Stoińska B. Birth weight and gestational age of newborns from Wielkopolski and Lubuski regions. Ginekol Pol. 2003;74(3):186–192.
Meulenberg PM, Hofman JA. Differences between concentrations of salivary cortisol and cortisone and of free cortisol and cortisone in plasma during pregnancy and postpartum. Clin Chem. 1990;36(1):70–75.
Główka FK, Kosicka K, Karaźniewicz-Łada M. HPLC method for determination of fluorescence derivatives of cortisol, cortisone and their tetrahydro- and allo-tetrahydro-metabolites in biological fluids. J Chromatogr B Analyt Technol Biomed Life Sci. 2010;878(3-4):283–289.
Kosicka K, Siemiątkowska A, Krzyścin M, et al. Glucocorticoid metabolism in hypertensive disorders of pregnancy: analysis of plasma and urinary cortisol and cortisone. PLoS One. 2015;10(12):e0144343. doi:10.1371/journal.pone.0144343.
Armstrong DA, Lesseur C, Conradt E, Lester BM, Marsit CJ. Global and gene-specific DNA methylation across multiple tissues in early infancy: implications for children’s health research. FASEB J. 2014;28(5):2088–2097.
Non AL, Binder AM, Barault L, Rancourt RC, Kubzansky LD, Michels KB. DNA methylation of stress-related genes and LINE-1 repetitive elements across the healthy human placenta. Placenta. 2012;33(3):183–187.
Kile ML, Baccarelli A, Tarantini L, Hoffman E, Wright RO, Christiani DC. Correlation of global and gene-specific DNA methylation in maternal-infant pairs. PLoS One. 2010;5(10): e13730. doi:10.1371/journal.pone.0013730.
Michels KB, Harris HR, Barault L. Birthweight, maternal weight trajectories and global DNA methylation of LINE-1 repetitive elements. PLoS One. 2011;6(9):e25254. doi:10.1371/journal.pone.0025254.
He ZM, Li J, Hwa YL, Brost B, Fang Q, Jiang SW. Transition of LINE-1 DNA methylation status and altered expression in first and third trimester placentas. PLoS One. 2014;9(5): e96994. doi:10.1371/journal.pone.0096994.
Hogg K, Blair JD, McFadden DE, von Dadelszen P, Robinson WP. Early onset pre-eclampsia is associated with altered DNA methylation of cortisol-signalling and steroidogenicgenes in the placenta. PLoS One. 2013;8(5):e62969. doi:10.1371/journal.pone.0062969.
Schoof E, Girstl M, Frobenius W, et al. Decreased gene expression of 11beta-hydroxysteroid dehydrogenase type 2 and 15-hydroxyprostaglandin dehydrogenase in human placenta of patients with preeclampsia. J Clin Endocrinol Metab. 2001;86(3):1313–1317.
Aufdenblatten M, Baumann M, Raio L, et al. Prematurity is related to high placental cortisol in preeclampsia. Pediatr Res. 2009;65(2):198–202.
Togher KL, Togher KL, O’Keeffe MM, et al. Epigenetic regulation of the placental HSD11B2 barrier and its role as a critical regulator of fetal development. Epigenetics. 2014;9(6):816–822.
Drake AJ, McPherson RC, Godfrey KM, et al. An unbalanced maternal diet in pregnancy associates with offspring epigenetic changes in genes controlling glucocorticoid action and foetal growth. Clin Endocrinol (Oxf) 2012;77(6):808–815.
Louwen F, Muschol-Steinmetz C, Reinhard J, Reitter A, Yuan J. A lesson for cancer research: placental microarray gene analysis in preeclampsia. Oncotarget. 2012;3(8):759–773.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Majchrzak-Celińska, A., Kosicka, K., Paczkowska, J. et al. HSD11B2, RUNX3, and LINE-1 Methylation in Placental DNA of Hypertensive Disorders of Pregnancy Patients. Reprod. Sci. 24, 1520–1531 (2017). https://doi.org/10.1177/1933719117692043
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719117692043