Abstract
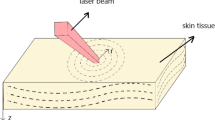
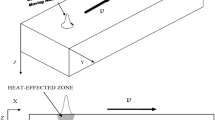
The thermo-mechanical behavior within biological tissues irradiated by a pulse laser is studied in this paper. The governing equations involving the local heat non-equilibrium effect and thermo-mechanical coupled effect are proposed in the context of generalized thermo-elastic model with dual-phase-lag times. An effective procedure constructed on the finite difference method is then employed to solve these equations numerically. The values of phase-lag times rooted in the local heat non-equilibrium are estimated, and the interaction between the temperature and thermal deformation is also evaluated via an effective characteristic parameter. The thermo-mechanical response irradiated by a pulse laser as a therapeutic heat source has been predicted on this basis. The parametric study of the characteristic parameters including the effective phase-lag times and thermo-mechanical coupling factor on the temperature, displacement and stresses of the target tissue is further studied. The results state that the transport properties predicted by introduction of phase-lag times and their effect on tissue temperature, displacement and normal stresses are dominated by their ratio. Furthermore, the coupled effect between the temperature and thermal deformation can be evaluated by the thermo-mechanical coupled coefficient and can be ignored in the treatments on tissues with a small thermo-mechanical coefficient in general.








Similar content being viewed by others
Data availability
No data associated in the manuscript.
References
A. Andreozzi, L. Brunese, M. Iasiello, C. Tucci, G.P. Vanoli, Numerical analysis of the pulsing heat source effects in a tumor tissue. Comput. Methods Programs Biol. 200, 105887 (2021). https://doi.org/10.1016/j.cmpb.2020.105887
P. Keangin, P. Rattanadecho, A numerical investigation of microwave ablation on porous liver tissue. Adv. Mech. Eng. 10, 1–13 (2018). https://doi.org/10.1177/1687814017734133
H. Hu, J. Wang, Z. Wu, Y. Liu, Y. Ma, J. Zhao, No benefit of wearing compression stocking after endovenous thermal ablation of varicose veins: a systematic review and meta-analysis. Eur. J. Vasc. Endovasc. 63, 103–111 (2022). https://doi.org/10.1016/j.ejvs.2021.09.034
A. Andreozzi, M. Iasiello, P.A. Netti, A thermoporoelastic model for fluid transport in tumor tissues. J. R. Soc. Interface 16, 20190030 (2019). https://doi.org/10.1098/rsif.2019.0030
A. Andreozzi, M. Iasiello, P.A. Netti, Effect of pulsating heat source on interstitial fluid transport in tumour tissues. J. R. Soc. Interface 17, 20200612 (2020). https://doi.org/10.1098/rsif.2020.0612
S. Singh, R. Melnik, Domain heterogeneity in radiofrequency therapies for pain relief: a computational study with coupled models. Bioengineering 7, 35 (2020). https://doi.org/10.3390/bioengineering7020035
N.A. Martin, S. Falder, A review of the evidence for threshold of burn injury. Burns 43, 1624–1639 (2017). https://doi.org/10.1016/j.burns.2017.04.003
A. Andreozzi, L. Brunese, M. Iasiello, C. Tucci, G.P. Vanoli, Modeling heat transfer in tumors: a review of thermal therapies. Ann. Biomed. Eng. 47, 676–693 (2019). https://doi.org/10.1007/s10439-018-02177-x
F. Xu, K.A. Seffen, T.J. Lu, Non-Fourier analysis of skin biothermomechanics. Int. J. Heat Mass Transf. 51, 2237–2259 (2008). https://doi.org/10.1016/j.ijheatmasstransfer.2007.10.024
J.H. Zhou, J.K. Chen, Y. Zhang, Theoretical analysis of thermal damage in biological tissues caused by laser irradiation. Mol. Cell Biomech. 4, 27–39 (2007)
K.C. Liu, Analysis for high-order effects in thermal lagging to thermal responses in biological tissue. Int. J. Heat Mass Transf. 81, 347–354 (2015). https://doi.org/10.1016/j.ijheatmasstransfer.2014.10.035
H.H. Pennes, Analysis of tissue and arterial blood temperature in the resting forearm. J. Appl. Physiol. 1, 93–22 (1948). https://doi.org/10.1152/jappl.1948.85.1.5
A. Bhowmik, R. Singh, R. Repaka, S.C. Mishra, Conventional and newly developed bioheat transport models in vascularized tissues: a review. J. Therm. Biol. 38, 107–125 (2013). https://doi.org/10.1016/j.jtherbio.2012.12.003
A. Andreozzi, M. Iasiello, C. Tucci, An overview of mathematical models and modulated-heating protocols for thermal ablation. Adv. Heat Transf. 52, 489–541 (2020). https://doi.org/10.1016/bs.aiht.2020.07.003
J. Liu, X. Chen, L.X. Xu, New thermal wave aspects on burn evaluation of skin subjected to instantaneous heating. IEEE Trans. Biomed. Eng. 46, 420–428 (1999). https://doi.org/10.1109/10.752939
H. Askarizadeh, H. Ahmadikia, Analytical analysis of the dual-phase-lag model of bio-heat transfer equation during transient heating of skin tissue. Heat Mass Transf. 50, 1673–1684 (2014). https://doi.org/10.1007/s00231-014-1373-6
Y.M. Xuan, W. Roetzel, Bioheat equation of the human thermal system. Chem. Eng. Technol. 20, 268–276 (1997). https://doi.org/10.1002/ceat.270200407
A. Nakayama, F. Kuwahara, A generalized bioheat transfer model based on the theory of porous media. Int. J. Heat Mass Transf. 51, 3190–3199 (2008). https://doi.org/10.1016/j.ijheatmasstransfer.2007.05.030
Y.W. Zhang, Generalized dual-phase lag bioheat equations based on nonequilibrium heat transfer in living biological tissues. Int. J. Heat Mass Transf. 52, 4829–4834 (2009). https://doi.org/10.1016/j.ijheatmasstransfer.2009.06.007
Y.X. Li, Y. Li, P.F. Luo, X.G. Tian, Relationship between the nonlocal effect and lagging behavior in bioheat transfer. ASME J. Heat Transf. 143, 051201–051208 (2021). https://doi.org/10.11151/1.4049997
M.J. Li, Y.Z. Wang, D. Liu, Generalized bio-heat transfer model combining with the relaxation mechanism and nonequilibrium heat transfer. ASME J. Heat Transf. 144, 031209–031218 (2022). https://doi.org/10.1115/1.4053414
S.M. Lin, C.Y. Li, Analytical solutions of non-Fourier bio-heat conductions for skin subjected to pulsed laser heating. Int. J. Therm. Sci. 110, 146–58 (2016). https://doi.org/10.1016/j.ijthermalsci.2016.06.034
K.C. Liu, Y. Wang, Y. Chen, Investigation on the bio-heat transfer with the dual-phase-lag effect. Int. J. Therm. Sci. 58, 29–35 (2012). https://doi.org/10.1016/j.ijthermalsci.2012.02.026
J. Dutta, B. Kundu, Thermal wave propagation in blood perfused tissues under hyperthermia treatment for unique oscillatory heat flux at skin surface and appropriate initial condition. Heat Mass Transf. 54, 3199–3217 (2018). https://doi.org/10.1007/s00231-018-2360-0
N. Afrin, J.H. Zhou, Y.W. Zhang, D.Y. Tzou, J.K. Chen, Numerical simulation of thermal damage to living biological tissues induced by laser irradiation based on a generalized dual phase lag model. Numer. Heat Transf. A-Appl. 61, 483–501 (2012). https://doi.org/10.1080/10407782.2012.667648
K.C. Liu, Y.S. Chen, Analysis of heat transfer and burn damage in a laser irradiated living tissue with the generalized dual-phase-lag model. Int. J. Therm. Sci. 103, 1–9 (2016). https://doi.org/10.1016/j.ijthermalsci.2015.12.005
Y.F. Yin, M. Li, Y.H. Li, J.Z. Song, Skin pain sensation of epidermal electronic device/skin system considering non-Fourier heat conduction. J. Mech. Phys. Solids 138, 103927–104022 (2020). https://doi.org/10.1016/j.jmps.2020.103927
F. Xu, T.J. Lu, K.A. Seffen, Biothermomechanics of skin tissues. J. Mech. Phys. Solids 56, 1852–1884 (2008). https://doi.org/10.1016/j.jmps.2007.11.011
X. Li, Y. Zhong, R. Jazar, A. Subic, Thermal-mechanical deformation modelling of soft tissues for thermal ablation. Bio-Med. Mater. Eng. 24, 2299–2310 (2014). https://doi.org/10.3233/BME-141043
J.X. Ma, X.F. Yang, Y.X. Sun, J.L. Yang, Theoretical investigation on the thermos-mechanical responses of the human skin during thermal therapy. Int. J. Mech. Sci. 161–162, 105041–105111 (2019). https://doi.org/10.1016/j.ijmecsci.2019.105041
Q. Zhang, Y.X. Sun, J.L. Yang, Thermoelastic behavior of skin tissue induced by laser irradiation based on the generalized dual-phase lag model. J. Therm. Biol. 100, 103038–103112 (2021). https://doi.org/10.1016/j.jtherbio.2021.103038
X.Y. Li, C.L. Li, Z.N. Xue, X.G. Tian, Analytical study of transient thermos-mechanical responses of dual-layer skin tissue with variable thermal material properties. Int. J. Therm. Sci. 124, 459–466 (2018). https://doi.org/10.1016/j.ijthermalsci.2017.11.022
X.Y. Li, Z.N. Xue, X.G. Tian, A modified fractional order generalized bio-thermoelastic theory with temperature-dependent thermal material properties. Int. J. Therm. Sci. 132, 249–256 (2018). https://doi.org/10.1016/j.ijthermalsci.2018.06.007
X.Y. Li, C.L. Li, Z.N. Xue, X.G. Tian, Investigation of transient thermos-mechanical responses on the triple-layered skin tissue with temperature dependent blood perfusion rate. Int. J. Therm. Sci. 139, 339–349 (2019). https://doi.org/10.1016/j.ijthermalsci.2019.02.022
Y.Z. Wang, M.J. Li, D. Liu, Thermo-mechanical interaction on transient heating of skin tissue with variable thermal material properties. Eur. J. Mech. A-Solid 86, 104173–104211 (2021). https://doi.org/10.1016/j.euromechsol.2020.104173
C.M. Gardner, S.L. Jacques, A.J. Welch, Light transport in tissue: accurate, heuristic for one-dimensional fluence rate and escape function based on upon Monte Carlo simulations. Laser Surg. Med. 18, 129–38 (1996). https://doi.org/10.1002/(SICI)1096-9101(1996)
D.Y. Tzou, K.S. Chiu, Temperature-dependent thermal lagging in ultrafast laser heating. Int. J. Heat Mass Transf. 44, 1725–1734 (2001). https://doi.org/10.1016/S0017-9310(00)00215-5
T.T. Lam, A unified solution of several heat conduction models. Int. J. Heat Mass Transf. 56, 653–666 (2013). https://doi.org/10.1016/j.ijheatmasstransfer.2012.08.055
K. Mitra, S. Kumar, A. Vedavarz, M.K. Moallemi, Experimental evidence of hyperbolic heat conduction in processed meat. ASME J. Heat Transf. 117, 568–573 (1995). https://doi.org/10.1115/1.2822615
D.Y. Tzou, The generalized lagging response in small-scale and high-rate heating. Int. J. Heat Mass Transf. 38, 3231–3240 (1995). https://doi.org/10.1016/S0017-9310(95)00052-6
P. Vadasz, Lack of oscillations in dual-phase-lagging heat conduction for a porous slab subject to imposed heat flux and temperature. Int. J. Heat Mass Transf. 48, 2822–2828 (2005). https://doi.org/10.1016/j.ijheatmasstransfer.2005.02.005
P. Yuan, Numerical analysis of an equivalent heat transfer coefficient in a porous model for simulating a biological tissue in a hyperthermia therapy. Int. J. Heat Mass Transf. 52, 1734–1740 (2009). https://doi.org/10.1016/j.ijheatmasstransfer.2008.09.033
K.C. Liu, H.T. Chen, Investigation for the dual phase lag behavior of bio-heat transfer. Int. J. Therm. Sci. 49, 1138–1146 (2010). https://doi.org/10.1016/j.ijthermalsci.2010.02.007
F. Xu, T.J. Lu, K.A. Seffen, Biothermomechanical behavior of skin tissue. Acta Mech. Sin. 24, 1–13 (2008). https://doi.org/10.1007/s10409-007-0128-8
Acknowledgements
This work was supported by the National Science Foundation of China [Grant Numbers 51676086 and 51575247].
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Y.Z., Lu, X.Y., Zheng, W.B. et al. Coupled thermo-mechanical behavior of skin tissue irradiated by a pulse laser. Eur. Phys. J. Plus 138, 698 (2023). https://doi.org/10.1140/epjp/s13360-023-04318-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1140/epjp/s13360-023-04318-1