Abstract
This study aimed to assess the potential of home monitoring using a monitoring application for the early prediction of acute exacerbations (AEs) in patients with fibrosing interstitial lung diseases (F-ILDs) by tracking symptoms, peripheral blood oxygen saturation (SpO2), and heart rate (HR). Data on symptoms, SpO2, and HR before and after a 1-min sit-to-stand test (1STST) were collected using an online home monitoring application. Symptoms were recorded at least 3 times a week, including cough intensity and frequency (Cough Assessment Test scale (COAT) score), breathlessness grade (modified Medical Research Council (mMRC) score), and SpO2 and HR before and after 1STST. Eighty-five patients with stable F-ILDs were enrolled. We observed a significant increase in COAT and mMRC scores, alongside a significant decrease in SpO2 before and after 1STST, 2 weeks before the first recorded AE. Furthermore, a combination of variables-an increase in COAT (≥ 4) and mMRC(≥ 1) scores, a decrease in SpO2 at rest (≥ 5%), and a decrease in SpO2 after 1STST (≥ 4%)- proved the most effective in predicting AE onset in patients with F-ILDs at 2 weeks before the first recorded AE. Home telemonitoring of symptoms, SpO2 holds potential value for early AE detection in patients with F-ILDs.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Fibrosing interstitial lung diseases (F-ILDs) are a group of heterogeneous diseases characterized by a high symptom burden and often poor prognosis1. Patients with F-ILDs may experience acute respiratory deterioration, known as acute exacerbations (AEs), which are associated with hospitalization and reduced short-term survival2. Retrospective studies have reported 1-year incidences of AE-IPF, ranging from 7 to 19.1%3,4. However, data on AE-ILD frequency in non-IPF F-ILDs are scarce. The estimated 1-year incidence of AE-connective tissue disease (CTD) ranges from 1.25 to 3.3%5. Pathophysiologically, AEs of F-ILDs often present as diffuse alveolar damage6.
AE of F-ILDs is difficult to be predicted or prevented; therefore, efforts should focus on identifying the early window of AE onset in these patients7. Symptoms, such as increased breathlessness and cough may correlate with disease progression in patients with IPF8,9. Thus, assessing predictive symptoms of AE onset in patients with F-ILDs is crucial in clinical practice10.
Exertional hypoxemia is a critical feature in patients with F-ILDs11. The 6-min walk test (6MWT) is a validated submaximal exercise test used to assess exercise tolerance and exercise-induced desaturation in patients with various chronic lung diseases12. Low peripheral blood oxygen saturation (SpO2) during the 6MWT is a strong predictor of AE and mortality in patients with IPF13. International guidelines recommend assessing exercise-induced desaturation in patients with interstitial lung diseases (ILDs)14. However, the 6MWT is not feasible for home care. Thus, the 1-min sit-to-stand (1STST) test can serve as an alternative indicator for monitoring exertional SpO2 desaturation in patients with ILDs15. Further study is needed to assess the utility of SpO2 desaturation monitoring during the 1STST test in evaluating disease progression in patients with F-ILDs.
Home monitoring of symptoms and physiological variables has become increasingly feasible with telemonitoring applications16. Home monitoring application offers an acceptable and accessible platform for collecting patient-reported objective and subjective data as demonstrated in IPF cases17,18. However, whether adopting a similar approach is feasible or clinically significant for F-ILDs remains unknown. Currently, there is limited information regarding the clinical benefits of remote monitoring in identifying the risk factors for AE onset in patients with F-ILDs. Therefore, this study aims to assess the potential of the 1STST and the home monitoring of symptoms, SpO2, and heart rate (HR) at rest for the early detection of AE in patients with F-ILDs.
Methods
Participants
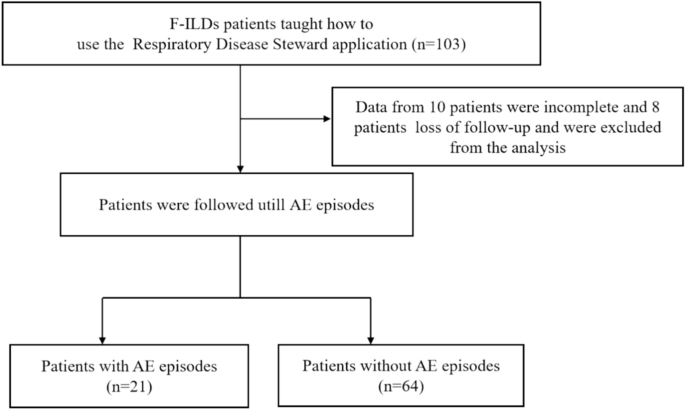
This prospective pilot study was conducted at the General Hospital of Ningxia Medical University (Yinchuan, China). Approval was obtained from the Medical ethics committee (No. KYLL-2021-456), and participants provided written informed consent. This study adhered to the principles of the Declaration of Helsinki, and patients’ privacy was strictly upheld during the statistical analysis. Recruitment occurred between November 2020 and July 2023. The inclusion criteria were as follows: (1) a clinical diagnosis of F-ILDs, including IPF, interstitial pneumonia with autoimmune features (IPAF), fibrotic idiopathic nonspecific interstitial pneumonitis (F-iNSIP), connective tissue disease- associated ILD (CTD-ILD), fibrotic hypersensitivity pneumonitis (F-HP), and unclassified ILD, confirmed through multidisciplinary evaluation by pulmonologists, radiologists, pathologists, and rheumatologists1, (2) age ≥ 18 years19; (3) stability of disease stage, with no history of AE in the past month; and (4) capability of using a smartphone. The exclusion criteria were as follows: (1) diagnosis of unstable cardiac disease, limb dysfunction, or pulmonary diseases other than ILDs, (e.g., chronic obstructive pulmonary disease (COPD), asthma, and obstructive sleep apnea-hypopnea syndrome); (2) significant mental health disorder; (3) inability to understand or use smartphones; and (4) participation in another home monitoring program for at least 3 months. The workflow of study is illustrated in Fig. 1. AE was diagnosed following the 2016 definition and the diagnostic criteria for AE of IPF: acute worsening of breathlessness (typically < 1 month), new bilateral ground glass abnormality or consolidation superimposed on a background reticular or honeycomb pattern on high-resolution computed tomography (HRCT), and exclusion of alternative causes such as left heart failure and pulmonary embolism20. Once the participants were suspected of having AE and admitted to the emergency department, AE diagnosis was confirmed through multidisciplinary treatment (MDT) based on clinical manifestations. The treatment of AE is mainly based on correcting hypoxemia, looking for reversible etiologies of respiratory decline, and palliation of symptoms.
Description of the home monitoring system
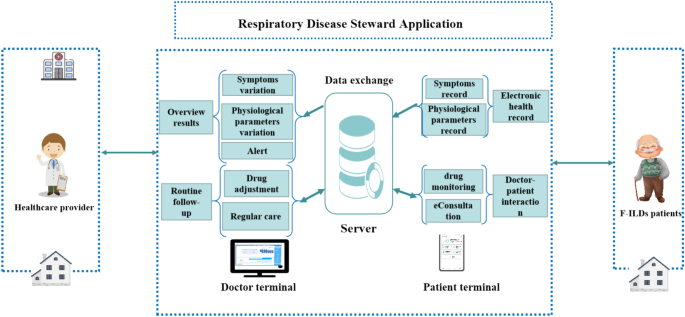
All the patients were enrolled in the home monitoring system collaboration with Zhejiang University, Hangzhou, China. The home monitoring system was described in our previous study21. The Closed-Loop Care Pathway System includes risk evaluation, follow-up, warnings, and medication management. Healthcare providers regularly follow up with patients to track their health status. The patients’ self-monitoring data and compliance were assessed daily to identify abnormal conditions. Initially, we designed and applied this system to patients with COPD, and we modified parts of the application modules for use by patients with F-ILD in this study. The system comprises a patient application, a doctor workstation, and a cloud server. The application ran on a smartphone and had two main modules: a diary and an education module. The diary module guided patients in recording their daily symptoms and physiological variables. Symptoms were recorded at least 3 times weekly. Patients were required to complete a questionnaire that included the modified Medical Research Council (mMRC) score22 and the Cough Assessment Test scale (COAT) score23). Additionally, a video-based 1STST was provided. At enrollment, patients were trained in person how to conduct 1STST, and participants were confirmed that they could conduct it correctly. Participant was required to conduct it at home at least 3 times weekly. The patients were initially enrolled in the study, and healthcare professionals provided detailed guidance to ensure their correct cooperation. The 1STST protocol adhered to previously published studies and guidelines15,24. SpO2 and HR before and after 1STST were recorded using pulse oximeters (Yuwell, FS20D, China) and transferred to system. Home monitoring system includes symptoms, COAT, mMRC scale, 1STST, SpO2, HR at rest and after 1-min sit-to-stand test (1STST) were measured at least 3 times weekly. Due to patient dependency, all three or more weekly patient completion records were included for data analysis. All the completed data from above listed monitoring indicators during the entire period of study were included in the final data analysis. Home oxygen therapy was recommended when patients had an SpO2 < 88%. Healthcare professionals monitored the data and followed up with the patients through telephone calls. The education module comprised ILD-related educational materials presented as videos and texts. All participants underwent training and received a hard copy of the instruction manual to ensure proper utilization of the home monitoring system. The proposed algorithm for telemonitoring during F-ILDs is shown in Fig. 2. Description of Home Monitoring system was summarized in Supplemental file 1.
Warning monitoring
We established an acceptable range of daily symptoms and physiological variables. If any of the following conditions were observed during home monitoring—COAT score ≥ 6, mMRC score ≥ 2 and SpO2 ≤ 88% at rest and after 1STST,—the system could automatically generate appropriate reminders for the patient. If a readout exceeded the acceptable range or if there were other unintended effects of the study, an alert was sent to the healthcare website, and the healthcare providers supervised patients through the website.
Clinical follow-up
All enrolled patients with F-ILDs were monitored using a home monitoring platform, with routine investigations conducted face-to-face and over the telephone. Respiratory symptoms, HRCT findings, and pulmonary function tests were assessed at the outpatient clinic every 3 months. The patients maintained a diary to record unscheduled medical visits, acute worsening of their respiratory symptoms, and changes in SpO2 and HR. Once a participant was suspected of having an AE, they were admitted to the emergency department for further diagnosis and treatment by MDT. The treatment is mainly based on correcting hypoxemia, looking for reversible etiologies of respiratory decline, and palliation of symptoms. Before discharge, he/she was assessed by a clinician. Within 1 month after discharge, the patients would not participate in the monitoring program but could continue to participate in the monitoring program after evaluation by the clinician. Survival was calculated from the first visit to the outcome or the end of the follow-up period.
Statistical analysis
Data were analyzed using the IBM SPSS Statistics 26 (https://www.ibm.com/support/pages/ downloading-ibm-spss-statistics-26). All quantitative variables are presented as mean ± standard deviation (SD), non-parametric data as median and interquartile range (IQR). A generalized linear model was used to analyze changes in symptoms and physiological dynamic variables during four phases: stable state and 3, 2, and 1 week before the first recorded AE. A receiver operating characteristic (ROC) curve was utilized to identify the optimal combination of symptoms and physiological variables monitored in the respiratory disease ward to predict AE onset. Survival curves were generated using the Kaplan–Meier method. Statistical significance was set at p < 0.05.
Results
Patient demographics
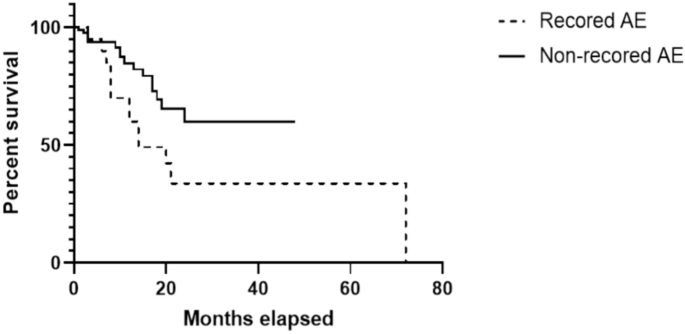
Patients demographics are presented in Table 1. Initially, 103 patients with F-ILDs were enrolled in our cohort. However, 10 patients were excluded due to incomplete data and eight were excluded owing to loss of follow-up. Overall, we analyzed 85 participants, Among them, 52 (61.2%) had IPF, while 33 (38.8%) had non-IPF F-ILDs. Among the non-IPF F-ILDs cases, nine were IPAF (10.6%), nine were F-iNSIP (10.6%), eight were CTD-ILD (9.4%), three were F-HP (3.5%), four were unclassified ILD (4.7%). The average recording time was 255.4 ± 78.1 d. The mean duration of follow-up was 18.0 months, ranged from 12 to 26 months. The mean age was 62.3 ± 8.3 years and 70 of the 85 (82.4%) patients were men. Among the 85 patients, 21 experienced AEs during follow-up. The predominant comorbidities were pulmonary hypertension (9.4%), lung cancer (4.7%), and gastrooesophageal reflux disease (4.7%). During the follow-up period, 25 (29.4) patients died. Kapla–Meier curves showed that patients with recorded AEs had a shorter median survival than those with non-recorded AEs (Fig. 3).
Patient satisfaction and use of the home monitoring application
Patients experiences with home monitoring application are presented in Table 2. Overall, 82 out of the 85 patients (96.5%) measured symptoms (mMRC and COAT score), 70 out of 85 patients (82.4%) measured 1STST, 73 out of 85 patients (85.9%) recorded medicication use, and 44 out of 85 patients (52.9%) used the information library. Patient satisfaction with the home monitoring program was high. 65 out of 85 patients (76.5%) were satisfied with the application, 61 out of 85 patients (71.8%) found it easy to use, 69 out of 85 patients (81.2%) recommend it to others, and 67 out of 85 patients (78.8%) considered it easily accessible to the hospital.
Symptoms monitored in patients with F-ILDs
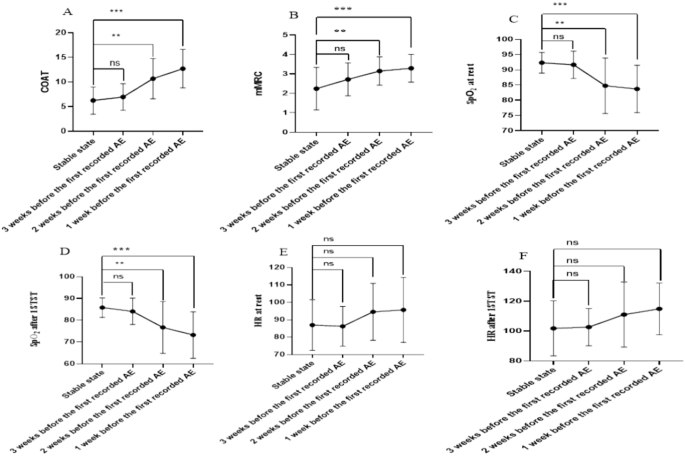
We examined symptom variations, including breathlessness and cough scores, and observed changes at baseline and during AE. We divided the disease progression into four phases: stable state, and 3, 2, and 1 week before the first recorded AE. COAT scores of the stable state and 3, 2, and 1 week before the first recorded AE were 6.0, 7.0, 10.0 and 12.0, respectively, and the differences were statistically significant (p < 0.001). For COAT scores, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, there was a significant difference between the stable state and 2 weeks and the stable state and 1 week before the first recorded AE (p < 0.001). Thus, patients had statistically high COAT scores from the stable state to 2 weeks before the first recorded AE. The variability of the COAT score increased by 4.4 ± 1.0 in the 2 weeks before the first recorded AE compared to the stable state. mMRC scores for the stable state and 3, 2 and 1 week before the the first recorded AE were 2.0, 2.0, 3.0 and 3.0, respectively and the differences were statistically significant (p < 0.001). For mMRC scores, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, a significant difference was observed between the stable state and 2 weeks (p = 0.005), and the stable state and 1 week (p < 0.001) before the first recorded AE. The variability of the mMRC score increased by 0.9 ± 0.2 2 weeks before the first recorded AE compared to the stable state. Thus, these symptom indicators indicate that the patients exhibited statistically and clinically elevated COAT and mMRC scores 2 weeks before the first recorded AE. Table 3 and Fig. 4 compare the telemonitored symptom parameters, while Table 4 shows the variations in in these parameters.
Comparison of telemonitoring symptoms and physiological parameters. (A) Comparison of COAT during the four phases of disease progression. (B) Comparison of mMRC scores during the four phases of disease progression. (C) Comparison of SpO2 at rest during the four phases of disease progression. (D) Comparison of SpO2 after 1STST during the four phases of disease progression. (E) Comparison of HR at rest during the four phases of disease progression course. (F) Comparison of HR after the 1STST during the four phases of disease progression course. **p < 0.01, ***p < 0.001, nsP > 0.05.
Physiological indicator monitoring in patients with F-ILD
Subsequently, we observed change of SpO2 and HR at rest and after 1STST during the four disease progression phases. The SpO2 at rest in these phases were 92.3%, 91.7%, 86.4% and 83.7%, respectively (p < 0.001). For SpO2 at rest, there was no significant difference between the stable state and 3 weeks before the first recorded AE; however, significant differences were observed between the stable state and 2 weeks (p = 0.002), and the stable state and 1 week (p < 0.001) before the first recorded AE. Thus, patients exhibited statistically decreased SpO2 at rest from 2 weeks before the first recorded AE. The variability of SpO2 at rest decreased by −6.0% ± 1.7 at 2 weeks before the first recorded AE compared to the stable state. The SpO2 after 1STST of the four phases was 85.8%, 84.1%, 76.7% and 73.2%, respectively. For SpO2 after 1STST, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, significant differences were observed between the stable state and 2 weeks (p = 0.007) and between the stable state and 1 week (p < 0.001) before the first recorded AE. Hence, patients had significantly decreased SpO2 after 1STST 2 weeks before the first recorded AE. The variability of SpO2 after 1STST decreased by −9.1%±2.3 at 2 weeks before the first recorded AE compared to the stable state. There was no significant difference in HR at rest and after 1STST between the four phases of disease progression. Table 3 and Fig. 4 compare the telemonitored physiological parameters, while Table 4 shows their variations.
Monitoring symptoms and physiological indicators for prediction of the onset of AE
Next, we identified the best-monitored symptoms and physiological indicators for predicting AE onset in patients with F-ILDs. We used changes in COAT scores, mMRC scores, and SpO2 to test the probability of the AE occurrence in patients with F-ILDs as nodes through the ROC curve, which are presented in Table 5. The best cut-off value for the change in the COAT score was 4.0 (sensitivity: 52.4%, specificity: 94.1%), with an area under the curve (AUC) of 0.773. The best cut-off value for the change in mMRC score was 1.0 (sensitivity: 66.7%, specificity: 52.9%), with an AUC of 0.592; The best cut-off value for the change in SpO2 at rest was −5.0 (sensitivity: 88.2%, specificity: 71.4%), with an AUC of 0.881; The best cut-off value for the change in SpO2 after 1STST was −4.0 (sensitivity: 64.7%, specificity: 61.9%), with an AUC of 0.633. Notably, a combination of parameters showing changes in COAT score (≥ 4), mMRC score (≥ 1), SpO2 at rest (≥ −5), and SpO2 after 1STST (≥ −4) was the best indicator for predicting AE occurrence in patients with F-ILDs 2 weeks before the first recorded AE (AUC = 0.854). This combination demonstrated sensitivity and specificity of 81.4% and 88.2%, respectively.
Discussion
The widespread use of smartphones and the internet has facilitated the home monitoring of heterogeneous group of F-ILDs, which primarily affect the lung parenchyma, causing dyspnea and often resulting in high mortality25. Crucial health changes can be detected using bedside monitors, which provide vital data noninvasively. Consequently, home monitoring has been recommended for the early detection of AEs in lung diseases, such as COPD. A similar technology may offer an early and and effective signal that could aid in distinguishing AE in patients with ILD16. However, the usefulness of measuring symptoms and physiological variables to detect AE in patients with F-ILDs remains unclear. We conducted this pilot study to assess the efficacy of home monitoring symptoms and variation in physiological parameters in predicting the onset of AE in patients with F-ILDs. Our results revealed high patient satisfaction and successful application of the home monitoring program. This approach can be readily integrated into home monitoring devices, providing alerts to physicians about patients at risk of experiencing AE. To our knowledge, this is the first study of such a home monitoring approach for predicting patients with F-ILDs.
Patients experiencing AE undergo a rapid decline in lung function, leading to poor quality of life, decreased physical activity and increased mortality2. Consequently, AE imposes a substantial burden on health-care costs, emphasizing the importance of early identification. AE may be differentiated from variations in the symptoms and physiological parameters that characterize F-ILDs7. Our findings revealed that median survival was shorter in patients with F-ILDs and AE than in those without AE. Symptoms of particular concern in patients with F-ILDs, such as breathlessness and cough, have been previously overlooked but are now gaining increased attention10,26. We utilized the mMRC and COAT questionnaires to assess breathlessness and cough, respectively. We observed a significant increase in COAT and a decrease in mMRC 2 weeks before the first recorded AE in patients with F-ILDs. A Japanese study reported that SpO2 could predict disease prognosis in patients with IPF. SpO2 measurements using a pulse oximeter are widely used to evaluate oxygen saturation and can be estimated rapidly and noninvasively27. For patients with idiopathic interstitial pneumonia (IIP), oxygen desaturation during the 6MWT is a strong predictor of mortality28. However, the 6MWT is time-consuming and requires a 30 m corridor, which is rare in healthcare settings. Conversely, the 1STST requires only a chair and can be efficiently conducted quickly, making it feasible in healthcare settings. Oishi et al.15 found that nadir desaturation during the 1STST correlated with nadir desaturation during 6MWT in patients with ILDs. Fedi et al.24 suggested that 1STSTs may be valuable for evaluating displacement and exercise-induced changes in SpO2 in patients with IPF. Therefore, we selected the 1STST as an alternative to the 6MWT to assess patients' SpO2, and HR. Furthermore, our findings revealed that before and after 1STST, the mean value of SpO2 significantly decrease 2 weeks before the first recorded AE. These findings corroborate the hypothesis that monitoring symptoms (including breathlessness and cough), and SpO2 (at rest and after 1STST) in patients with F-ILDs may facilitate the early detection of AE.
Furthermore, our findings indicated that a combination of variables, including an increase in COAT (≥ 4) and mMRC (≥ 1) scores and, a decrease in SpO2 at rest (≥ 5%), and after 1STST (≥ 4%) yielded the highest predictive value for AE onset in patients with F-ILDs 2 weeks before the first recorded AE (AUC = 0.854). Ultimately, SpO2 is cost-efficient and reliable parameter, while symptom monitoring can aid in predict the AE of F-ILDs.
Our study has several strengths and numerous potential limitations that warrant acknowledgment. First the study was conducted at a single center study and small smaple size. Second, An inherent bias was present due to comorbidities, notably, the predominant comorbidities in this study included pulmonary hypertension (9.4%), lung cancer (4.7%), and gastrooesophageal reflux disease (4.7%), which could potentially impact the validity and reliability of the monitoring parameters results. Third, a latent safety risk is associated with participants conducting the 1STST at home. To mitigate this, we designed warning monitoring and feedback from healthcare providers to address any potential events. Furthermore, home oxygen therapy was recommended for patients with a SpO2 < 88%. Fourth, our pilot study could not yield the highest evidence level, so a randomized controlled trial should be conducted in further studies.
Conclusion
In summary, this study is the first to provide data on weekly variations in symptoms and physiological parameters in patients with stable F-ILDs. We further outlined how this information could facilitate the confirmation of AE onset in these patients.
Data availability
The data that supporting the findings of this study are available upon reasonable request from the corresponding author.
References
Wijsenbeek, M. & Cottin, V. Spectrum of fibrotic lung diseases. N. Engl. J. Med. 383(10), 958–968 (2020).
Suzuki, A. et al. Acute exacerbations of fibrotic interstitial lung diseases. Respirology 25(5), 525–534 (2020).
Kim, D. S. et al. Acute exacerbation of idiopathic pulmonary fibrosis: Frequency and clinical features. Eur. Respir. J. 27, 143–150 (2006).
Song, J. W., Hong, S. B., Lim, C. M., Koh, Y. & Kim, D. S. Acute exacerbation of idiopathic pulmonary fibrosis: Incidence, risk factors and outcome. Eur. Respir. J. 37, 356–363 (2011).
Suda, T. et al. Acute exacerbation of interstitial pneumonia associated with collagen vascular diseases. Respir. Med. 103, 846–853 (2009).
Oda, K. et al. Autopsy analyses in acute exacerbation of idiopathic pulmonary fibrosis. Respir. Res. 15, 109 (2014).
Biondini, D. et al. Acute exacerbations of idiopathic pulmonary fibrosis (AE-IPF): An overview of current and future therapeutic strategies. Expert Rev. Respir. Med. 14(4), 405–414 (2020).
Ryerson, C. J. et al. Cough predicts prognosis in idiopathic pulmonary fibrosis. Respirology 16(6), 969–975 (2011).
Ley, B., Bradford, W. Z. & Vittinghoff, E. Predictors of mortality poorly predict common measures of disease progression in idiopathic pulmonary fibrosis. Am. J. Respir. Crit. Care Med. 194(6), 711–718 (2016).
Kreuter, M. et al. Palliative care in interstitial lung disease: Living well. Lancet Respir. Med. 5(12), 968–980 (2017).
Marillier, M. et al. Influence of exertional hypoxemia on cerebral oxygenation in fibrotic interstitial lung disease. Respir. Physiol. Neurobiol. 285, 103601 (2021).
Eaton, T., Young, P., Milne, D. & Wells, A. U. Six-minute walk, maximal exercise tests: Reproducibility in fibrotic interstitial pneumonia. Am. J. Respir. Crit. Care Med. 171(10), 1150–1157 (2005).
Kondoh, Y. et al. Disease severity staging system for idiopathic pulmonary fibrosis in Japan. Respirology 22(8), 1609–1614 (2017).
Raghu, G. et al. An official ATS/ERS/JRS/ALAT statement: Idiopathic pulmonary fibrosis: Evidence-based guidelines for diagnosis and management. Am. J. Respir. Crit. Care Med. 183(6), 788–824 (2011).
Oishi, K. et al. The 1-min sit-to-stand test to detect desaturation during 6-min walk test in interstitial lung disease. NPJ Prim. Care Respir. Med. 32(1), 5 (2022).
Althobiani, M. A. et al. Home monitoring of physiology and symptoms to detect interstitial lung disease exacerbations and progression: A systematic review. ERJ Open Res. 7(4), 00441–02021 (2021).
Moor, C. C. et al. A home monitoring program including real-time wireless home spirometry in idiopathic pulmonary fibrosis: A pilot study on experiences and barriers. Respir. Res. 19, 105 (2018).
Marcoux, V. et al. Mobile health monitoring in patients with idiopathic pulmonary fibrosis. Ann. Am. Thorac. Soc. 16(10), 1327–1329 (2019).
Moor, C. C. et al. Home monitoring in patients with idiopathic pulmonary fibrosis: A randomized controlled trial. Am. J. Respir. Crit. Care Med. 202(3), 393–401 (2020).
Collard, H. R. et al. Acute exacerbation of idiopathic pulmonary fibrosis. An international working group report. Am. J. Respir. Crit. Care Med. 194(3), 265–275 (2016).
Deng, N. et al. A home-based pulmonary rehabilitation mHealth system to enhance the exercise capacity of patients with COPD: Development and evaluation. BMC Med. Inform. Decis. Mak. 21(1), 325 (2021).
Nishiyama, O. et al. A simple assessment of dyspnoea as a prognostic indicator in idiopathic pulmonary fibrosis. Eur. Respir. J. 36(5), 1067–1072 (2010).
Koo, H. K. et al. Development and validation of the COugh assessment test (COAT). Respirology 24(6), 551–557 (2019).
Fedi, A. et al. Concurrence of 1- and 3-min sit-to-stand tests with the 6-min walk test in idiopathic pulmonary fibrosis. Respiration 100(7), 571–579 (2021).
Wijsenbeek, M. S. et al. Home monitoring in interstitial lung diseases. Lancet Respir. Med. 11(1), 97–110 (2023).
Carvajalino, S., Reigada, C., Johnson, M. J., Dzingina, M. & Bajwah, S. Symptom prevalence of patients with fibrotic interstitial lung disease: A systematic literature review. BMC Pulm. Med. 18(1), 78 (2018).
Takei, R. et al. Pulse oximetry saturation can predict prognosis of idiopathic pulmonary fibrosis. Respir. Investig. 58, 190–195 (2020).
Lama, V. N. et al. Prognostic value of desaturation during a 6-min walk test in idiopathic interstitial pneumonia. Am. J. Respir. Crit. Care Med. 168, 1084–1090 (2003).
Acknowledgements
The authors thank Xiaoming Liu for invaluable scientific feedback on the manuscript.
Funding
This work was supported by grants from the National Natural Science Foundation of China (No. 81760004; 82060013), the Natural Science Foundation of Ningxia Hui Autonomous Region (No. 2020AAC02001; 2020AAC03404), and the Key Research and Development Program of Ningxia Hui Autonomous Region (No. 2018BEG03035; 2023BEG02021).
Author information
Authors and Affiliations
Contributions
F.H.Y. and C.J. conceived the idea, designed the experiments, analyzed and interpreted the data, and approved the final version of the manuscript. W.Z.J. conceived the idea, performed the experiments, and drafted the main critically reviewed manuscript. H.Z.Y., W.F., H.J. and Z.Y.N. contributed to the interpretation of data. Z.T.T., X.H.X., J.W.S., W.F.X. and D.N. contributed to the drafting and revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interests. This manuscript has not been published previously and is not under consideration for publication elsewhere. All authors have approved the contents of this paper and agreed to the journal’s submission policies.
Ethics approval and consent to participants
This study was conducted in accordance with the Declaration of Helsinki. The study protocol was approved by the Human Research Ethics Committee of the General Hospital of Ningxia Medical University (KYLL-2021-456). Informed consent was obtained from all patients to collect and publishing the data.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Fu, H., Wang, Z., Hu, Z. et al. Pilot study of home-based monitoring for early prediction of acute exacerbations in patients with fibrosing interstitial lung diseases. Sci Rep 14, 21101 (2024). https://doi.org/10.1038/s41598-024-71942-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-71942-x
- Springer Nature Limited