Abstract
Health-related quality of life, sleep quality, morning and evening types, and internet addiction are of significant importance to the development of medical students, yet they have rarely been studied. Taking this into consideration, the study aimed to confirm latent profiles in health-related quality of life, sleep quality, morning and evening types, and internet addiction in medical students and investigate the characteristics of participants in each profile to provide suggestions for students’ health. This was an observational cross-sectional study including 1221 medical student subjects at China Medical University in 2019. Multiple correspondence analysis was the initial step to verify the correspondence, dispersion, and approximation of variable categories. Latent profile analysis was used to identify the multiple correspondences between the levels of variables. Three profiles were found, including: (1) The Low sleep quality profile was characterized by the lowest sleep quality among the three existing profiles. (2) The High health-related quality of life and Low internet addiction profile was characterized by the highest level of health-related quality of life but the lowest level of internet addiction. (3) The Low health-related quality of life and High internet addiction profile was characterized by the highest standardized values of internet addiction but the lowest standardized values of health-related quality of life. This study had important implications for improving student health and supported the medical universities and hospitals in implementing targeted policies based on distinctive student characteristics.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Introduction
Sleep problems are very common in the general population, and medical students are a vulnerable group that is prone to poor sleep quality1. According to a comprehensive meta-analysis of 57 studies with 25,735 medical students, the pooled prevalence of poor sleep quality was 52.7%2. Another study found that in the United States, medical students' sleep quality was significantly worse than a healthy adult sample3. Similarly, a cross-sectional study in Etawah college also reported that medical students had worse sleep quality than nonmedical students4. As a key component of personal health in medical education, the sleep quality of students cannot be ignored.
The sleep quality of medical students at the university was affected by living habits, such as electronic use before bed and sleep duration5. As sleep-interfering processes theory indicates, sleep problems arise when the brain is highly active before bedtime, such as rumination, worrying, planning, analyzing, problem-solving, and difficulty controlling one’s thoughts6. If the person engages in sleep incompatible behaviors in bed (browsing the internet before bedtime, staying in bed late, poor sleep habits, etc.), sleep disturbances are likely to occur6. For example, a study of young adults aged 19–32 showed that using social media within 30 min of bedtime was independently associated with sleep disturbance7. Another study found that strict parental rules about internet and smartphone use before sleep might prevent negative consequences of social media use on bedtime and sleep quality8.
However, the living habits of young people transitioning from secondary education to university education have undergone profound changes, with the main manifestation being that many students have a tendency to sleep late or a nighttime preference, which is particularly prominent among medical students9. A study has shown that medical students can be obliged to change their morning and evening type because of academic commitments, such as working night shifts during internships, which can lead to long-term sleep deprivation and cumulative sleep deficits10. In addition, there is a high prevalence of internet addiction among medical undergraduate students11,12. The researchers found that although some medical students used the internet for academic searches, the majority of them used it for entertainment13. A study of 337 medical students in Tumakuru also confirmed that medical students had a significantly higher prevalence of internet addiction than the general population14. More than half of medical students lost sleep due to late-night internet use15.
The above findings are concerning because the evening type and internet addiction can have compounding effects, such as causing medical students to be absent from daytime activities, with negative effects on academic performance and health-related quality of life16,17. As a result, sleep quality and health-related quality of life interact with each other and progress negatively, creating a chronic cycle.
Health-related quality of life refers to a subjective rating of the impact of an individual’s health on his or her overall well-being18. Currently, students in the health professions have a worse health-related quality of life and a relatively low awareness of issues related to quality of life, compared to the general population19,20,21. The poor health-related life quality of medical students remains a significant issue for the profession to address.
Therefore, this study focused on sleep quality, morning and evening patterns, internet addiction, and health-related quality of life to identify and manage the health problems of medical students early. A growing body of research has examined the associations between health-related quality of life, sleep quality, morning and evening type, and internet addiction in the general population, including studies on medical students22,23,24,25. However, few studies have used a person-centered approach (i.e., the interest is finding heterogeneous groups of individuals) to explain the relationship between the responses to the observed set of categorical variables. These studies often treat the group of medical students as a single distribution, ignoring the measurable differences among individuals within the group. The use of data-based, person-centered classification is crucial to ensure the healthy growth of students in their lives and to develop targeted primary prevention measures based on profile characteristics26,27.
We examine the different health-related quality of life, sleep quality, morning and evening type, and internet addiction clusters by latent profile analysis (LPA), using data from a cross-sectional survey of medical students at China Medical University. Identifying these elements and potential risk categories among medical students will improve their health and formulate policies in a way that does not affect their performance.
Method
Sample
This study was a cross-sectional study. A total of 1224 medical students participated in the survey. We compiled and collected the questionnaires through the Questionnaire Star Platform (Changsha Ranxing Information Technology Co., Changsha, China) to investigate the demographic data and health-related quality of life, sleep quality, morning and evening type, and internet addiction of medical students. After removing irregular responses, the study comprised 1221 medical students. This study was approved by the Ethics Committees of China Medical University (No. CMU1210400026). The research was performed in accordance with the Declaration of Helsinki.
Measures
Sociodemographic data included sex and age. The study variables also included health-related quality of life, sleep quality, morning and evening type, and internet addiction of medical students.
Health promoting lifestyle profile II (HPLP II)
The HPLP II was used to measure health-related quality of life28. The HPLP II consists of 52 Likert scale items, with a higher score indicating a higher level of health-related quality of life. HPLP-II contains 6 domains: interpersonal relations, spiritual growth, nutrition, stress management, health responsibility, and physical activity. Items are rated using a four-point rating scale, with 1 meaning “never,” 2 meaning “sometimes,” 3 meaning “very often” and 4 meaning “routine.” Total HPLP II scores range from 52 to 208. A score of 52–104 indicates poor marked as “unhealthy”, 105–156 indicates moderate marked as “moderate”, and 157–208 indicates good marked as “health”. The Cronbach’s alpha in this sample for HPLP II is 0.974.
Pittsburgh sleep quality index (PSQI)
Students completed the PSQI to measure sleep quality29,30. The scale consists of 19 questions evaluating the following seven dimensions: fall asleep time, sleep time, sleep efficiency, sleep disorders, sleep drugs, daytime dysfunction and self-rated sleep quality. The score range for the 16 items is 0–3 points. Item 1 refers to bedtime, item 3 refers to wake-up time, and sleep efficiency is calculated based on items 1, 3, and 4, with a score range of 0–3. The PSQI ranges from 0 to 21, which assesses sleep quality for the past month31. The PSQI indicates good sleep quality, with 0–5 points marked as “very good”, 6–10 points denoted as “better”, 11–15 points indicated as “general”, and “poor” sleep quality referring to 16–21 points32. The PSQI has been validated in college students and has high reliability6,30.
Morningness-eveningness questionnaire (MEQ)
The MEQ is a self-assessed questionnaire consisting of 19 items that assesses an individual’s chronotype33. The total score ranges from 16 to 86 points, consisting of 11 items with a scoring range of 1–4 points, two items with scores of 0, 2, 4, or 6 points, one item with scores of 0, 2, 3, or 5 points, and five items with a scoring range of 1–5 points. This questionnaire establishes three behavioral categories: evening types (late bedtimes and late wake-up, score = 16–41) marked as “evening”, intermediate types (regular type, score = 42–58) marked as “intermediate”, and morning types (early to bed and early to rise, score = 59–86) marked as “morning”. The MEQ has been used in many studies and has demonstrated good measurement performance among college students34,35.
Internet addiction test
The Internet Addiction Test measures the level of internet addiction based on 20 items using a five-point Likert scale36. Each question is scored by 1 meaning “hardly ever,” 2 meaning “occasionally,” 3 meaning “sometimes,” 4 meaning “very often,” and 5 meaning “always.” Scores over 50 indicate occasional or frequent internet addictive behavior. A higher score indicates a higher level of internet addiction. The Cronbach’s alpha in this sample for the internet addiction scale is 0.935.
Data analysis
Data analyses were performed using the SPSS Statistics Version 23.0 (IBM Corp., Armonk, NY, USA) and EmpowerStats (X&Y Solutions, Inc., Boston, MA, USA). LPA was performed using Mplus Version 7.0 (Muthén and Muthén, Los Angeles, CA, USA). The Shapiro–Wilk test revealed the nonnormal distribution of the data. Comparisons of distributions between three groups were made by the Kruskal–Wallis test (including Dunn-Bonferroni post hoc correction). All tests were two-sided, and statistical significance was set at P < 0.05.
LPA was conducted to examine the latent profiles of health-related quality of life, sleep quality, morning and evening type, and internet addiction among medical students. Until the fitness measures reached their ideal levels, models were estimated by gradually increasing the number of profiles from the start (2 profile) to the final model. A log-likelihood test was utilized for model fitting, and the ensuing metrics were commonly employed to signify the aptness: the Akaike information criterion (AIC), the Bayesian information criterion (BIC), and the sample size adjusted Bayesian information criterion (aBIC), with a smaller value indicating better model fitness37. In LPA, entropy values are frequently computed to assess the precision of classification, on a scale of 0 to 1, with a predilection for higher values. In addition, P was calculated by the Lo-Mendell-Rubin test, and Vuong-Lo-Mendell-Rubin are crucial metrics for determining whether the model best suits the data37. If P is less than 0.05, it means that the model fits the data significantly superior to the antecedent model38.
Multiple correspondence analysis (MCA) was used to identify the most important relationships among variables in the dataset by a graphical representation of the similarity between the given observations (Euclidian distance). In a preliminary step, MCA was used to confirm correspondence, dispersion, and approximation in variable categories. The exploratory method provided the concepts of the index variables and the number of latent profiles through the principal plane. The inertia value and Cronbach’s alpha were used to define the number of dimensions to retain in the final MCA39. The results of the first two MCA dimensions were plotted to illustrate relationships between variables as MCA principal dimensions. According to LPA, respondents are assigned to the cluster with the highest attribution probability based on their responses to observed variables. To find the various correspondences between the levels of the categorical variables, a multivariate analysis was used for categorical variables.
Patient and public involvement
The design of the study aimed to address questions about health-related quality of life, sleep quality, morning and evening type, and internet addiction in medical students. In the formative research stage, we seek input from participants in research design and behavior. All students participated voluntarily and were not remunerated. Although there was no specific public involvement in the development of the research question and outcomes, any student, as a participant in the survey, can obtain contact information to keep up-to-date research results. The preliminary findings were then tested and analyzed in depth before the current study.
Ethics approval and consent to participate
The study was approved by the institution’s ethics committee (No. CMU1210400026). Written informed consent was obtained from participants included in the study. Any personal information obtained in this study remained confidential. The research was performed in accordance with the Declaration of Helsinki.
Results
Participant characteristics
Most of the students (n = 736; 60.28%) in the study were aged 20 years old. The proportion of female students was higher than that of males, and there were 807 females and 414 males in this study. Significant differences were observed between males and females in sleep quality and morning and evening type (P < 0.05). There were no significant differences between males and females in health-related quality of life and internet addiction. There was no difference between health-related quality of life, sleep quality, internet addiction, and morning and evening type in different age groups (P > 0.05). Details are presented in Table 1.
MCA
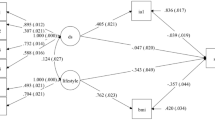
A graphical representation of lifestyle associations was provided by MCA (Fig. 1). A total of 67.38% of the variability was explained by dimensions 1 and 2. The internal correlation coefficients (Cronbach’s alpha) were 0.417 and 0.258 respectively, indicating that there is a moderate internal correlation.
The MCA plot showed that individuals with “health quality of life,” “no internet addiction,” “morning type,” and “very good sleep quality” (on the left of the graph) were mostly located opposite individuals with “unhealthy and moderate quality of life,” “internet addiction,” “evening type,” and “poor, general and better sleep quality” (on the right of the graph). Among them, the “very good sleep quality” appeared on the left side alone, while the “poor, general, and better sleep quality” appeared on the right side alone, which indicated that the “very good sleep quality” was quite different from the other three categories. Similarly, the “unhealthy and moderate quality of life” was concentrated on the right, suggesting that people with very good sleep quality would be most likely to have a healthy lifestyle. In addition, individuals with “no internet addiction” and “morning type” were located opposite individuals with “internet addiction” and “evening type”. It can also be noted that there is spatial proximity between “evening type” and “unhealthy quality of life”, which displays a close correlation. In short, MCA analysis was able to differentiate the health-related quality of life, sleep quality, morning and evening type and internet addiction.
LPA
The fit indices of the LPA models showed that the three-profile model had a lower AIC40, BIC41, and aBIC37. The four-profile model entropy was better than the three-profile model entropy. However, the Lo-Mendel-Rubin likelihood and Vuong-Lo-Mendell-Rubin values for the four-profile model were not significant37,38. Considering the above, the three-profile model was chosen as our default, no-covariates latent profile model since it had overall superior metrics compared to alternative models employing other manifest variables and numbers of latent profiles, as well as enabling better profile interpretation (see Appendix 1).
Three profiles were named based on their most prominent characteristics and included the Low sleep quality profile, the High health-related quality of life and Low internet addiction profile, and the Low health-related quality of life and High internet addiction profile (Fig. 2). The largest profile (n = 579; 47.42%), which we named the Low sleep quality profile, was characterized by the poorest sleep quality and highest morning and evening type scores that indicated a tendency towards morningness among the three existing profiles. The second-largest profile (n = 499; 40.87%), which we named the High health-related quality of life and Low internet addiction profile, was characterized by the highest level of health-related quality of life but the lowest level of internet addiction. The smallest profile (n = 143; 11.71%), which we named the Low health-related quality of life and High internet addiction profile, was characterized by the highest standardized values of internet addiction but the lowest standardized values of health-related quality of life; this profile of respondents also scored the lowest in the morning and evening type that indicated the greatest eveningness preference among the three existing profiles.
Differences in health-related quality of life, sleep quality, morning and evening type, and internet addiction among medical students for the three profiles. Abbreviations: HRQL, standardized values of health-related quality of life; IA, standardized values of internet addiction; ME, standardized values of morning and evening type; SQ, standardized values of sleep quality. Standardization is to convert the original values of a column of variables into standard scores, and the formula is (original value—mean value of variables)/standard error. After standardization, data with 0 as the average and 1 as the standard deviation are obtained.
To determine whether the three profiles differed significantly, Kruskal–Wallis tests were carried out (Table 2). The results showed that health-related quality of life, sleep quality, morning and evening type, and internet addiction had significant differences among the three profiles (P < 0.001). Especially, the students in profile II scored significantly higher in health-related quality of life than the other two groups, while the scores in sleep quality and internet addiction were significantly lower than those of the other groups. Besides, the students in profile III scored significantly lower in terms of health-related quality of life and morning and evening types than the other two profiles.
Discussion
First, this study explored the profiles of health-related quality of life, sleep quality, morning and evening type, and internet addiction in medical students. LPA identified three profiles (the Low sleep quality profile, the High health-related quality of life and Low internet addiction profile, and the Low health-related quality of life and High internet addiction profile) in this population. Second, these profiles demonstrated differential associations between health-related quality of life, sleep quality, morning and evening type, and internet addiction of medical students, documenting that sleep quality is not only associated with unhealthy lifestyles or morning and evening types, but also related to internet addiction.
Our results suggest that significant differences were observed between males and females in sleep quality, and morning and evening type. Therein, male medical students have poorer sleep quality than female medical students. Both males and females are troubled by changes in their emotional and social environments during their college years42. A study showed that the abnormal sleep state of students is mainly affected by the pressure of social interaction43. This was particularly true during the COVID-19 pandemic when most students were subjected to closed management on campus and heightened anxiety44. Female college students often have more emotional support than male students, and they can often face and solve the problems they encounter through discussions among their partners. Male students are likely to be infected with the bad habit of playing games all night, which may reduce the quality of sleep45,46,47. In addition, from the perspective of sleep conditions, men are more likely to go to bed later than women, resulting in decreased total sleep time48.
A combination of these properties is more likely to be associated with unhealthy lifestyles according to the MCA: staying up and waking up later, and poor sleep quality. In contrast, healthy lifestyles are more likely to be accompanied by very good sleep quality, which was consistent with the overall observation. On the one hand, the heavy schoolwork burden, numerous subjects and fierce competition among peers make medical students have strong learning motivation, which forces them to spend more rest time to complete academic tasks and sleep late49,50. On the other hand, although the internet provided students with good learning, communication and entertainment platforms during the recent epidemic, it also had a subtle impact on their lifestyles and behaviors51. In the face of huge learning pressure and potential interpersonal barriers, medical students are more inclined to take online communication as a way to lessen pressure and obtain a sense of identity and belonging from the virtual media platform52,53. Unrestrained Internet surfing will lead to high brain excitement, affect sleep time and sleep efficiency, cause serious sleep disorders and have a negative impact on daytime learning and life54. However, medical students’own health literacy and awareness of physical health care are higher than those of the general population, which makes some medical students highly self-disciplined, that is, they have very good sleep quality under a healthy lifestyle to reduce the adverse effects caused by occupational exposure or learning pressure55,56. A study showed that a brief and personalized online sleep education can help college students develop good sleep habits, thereby significantly improving their sleep quality57. Tsai et al. pointed out in a review article that cognitive behavioral therapy for insomnia has a large effect in the sleep quality improvement among young insomniacs, which may be an effective and inexpensive measure to address sleep deprivation and poor sleep habits among college students58. Therefore, the above methods might be applied to improve the sleep quality of medical students.
The LPA data stressed three latent profiles of medical students’ health-related quality of life, sleep quality, morning and evening type, and internet addiction. The emergence of these distinct profiles suggests that medical students’ health does consistently correlate with their lifestyles. For example, in the Low health-related quality of life and High internet addiction profile, students experienced a relatively low level of health-related quality of life but a high degree of internet addiction. Such students’ learning motivation may be weakened due to internet addiction, so they are more vulnerable to academic setbacks59. They may feel more anxious and nervous when facing academic and employment pressures unique to medical students, thus affecting sleep time and sleep efficiency, and possibly leading to serious sleep disorders60. They may also shrink back when facing challenges in clinical practice and communicating with teachers and their families, thus spending more time on online entertainment, such as web chat, online shopping, watching videos, etc61.
Students with high health-related quality of life and low internet addiction profile had the best sleep quality. Our results concerning the link between sleep quality and internet addiction and health-related quality of life have already been identified in previous research22. A study on the LPA of sleep quality among university students suggests that students exhibit the worse health-related quality of life in the profile with the poorest perceived sleep quality62. Similarly, a study on medical students using a LPA also indicated that a healthy lifestyle is associated with better sleep quality63. One possible explanation is that students with high health-related quality of life may be more likely to maintain positive emotions and attitudes, which can contribute to better sleep quality64. They may also prioritize social interaction, leading to a lower degree of internet addiction65. In addition, students who had high health-related quality of life may be more focused on healthy lifestyle habits, such as the morning types that involve early to bed and early to get up66. And students with low internet addiction intent to have a good sleep, for example, they can fall asleep easily and achieves better sleep quality by avoiding the use of electronic devices before bedtime67,68. These findings suggest the importance of maintaining a healthy lifestyle, managing internet use, and prioritizing morning types for better sleep quality.
We found that medical students in the Low sleep quality profile had the poorest sleep quality and a tendency towards morningness among the three profiles. This result is contrary to previous research69. This could be because students who wake up early tend to have a more regular biological clock and daily routine, making it easier for them to maintain good sleep habits70. As a result, students with poor sleep quality are more likely to prefer early rising as a way to improve their sleep quality71. According to previous research, people with poor sleep quality may experience shallower sleep, more frequent awakenings, or waking up early72. Our findings suggest that maintaining a regular sleep schedule and routine may be beneficial for improving sleep quality. It is important to note that poor sleep quality can have various negative consequences, such as waking up early, which can be improved with good sleep habits.
This study identified health-related quality of life, sleep quality, morning and evening type, and internet addiction in the student population, which may help reduce the negative impact of health-related quality of life, sleep quality, morning and evening type, and internet addiction, improving the efficiency of medical students. Moreover, at present, programmatic attention is largely focused on the general public, with less emphasis on medical students73,74. It is of great significance to study the health-related quality of life, sleep quality, morning and evening type, and internet addiction among medical students to improve healthcare service quality in the health system75.
Our study has the limitation of recruiting students from only one college. College-specific factors, such as the learning environment and course structure, may affect the results. Thus, international multicenter studies on a larger scale are required to verify the findings described herein in the future.
Conclusion
Poor sleep quality, evening type, internet addiction, and unhealthy quality of life are risk factors for the health of medical students. Classifying medical students can help predict their health and provide a basis for helping their medical universities and hospitals make targeted policies based on distinctive characteristics.
Although medical students already have some knowledge on health and medicine, they should still need to pay attention to their health, especially at work and at rest. Medical students need to be aware of the existence of these risk factors and take proactive steps to improve their lifestyles and keep healthy. Future guidance includes applying sleep-related health education and behavioural interventions to promote healthy sleep habits, such as establishing a regular sleep schedule, creating a sleep-conducive environment, and avoiding excessive internet access before bedtime. This will help promote a healthy workforce in the foreseeable future. Developing an evidence-based health model for medical students would serve as an essential part of designing and evaluating health promotion measures for medical students.
Data availability
The datasets used during the current study are available from the corresponding author on reasonable request.
References
Niño García, J. A., Barragán Vergel, M. F., Ortiz Labrador, J. A., Ochoa Vera, M. E. & González Olaya, H. L. Factors associated with excessive daytime sleepiness in medical students of a higher education institution of Bucaramanga. Rev. Colomb. Psiquiatr. (Engl. Ed.) 48, 222–231 (2019).
Rao, W. W. et al. Sleep quality in medical students: A comprehensive meta-analysis of observational studies. Sleep Breath. 24, 1151–1165 (2020).
Azad, M. C. et al. Sleep disturbances among medical students: A global perspective. J. Clin. Sleep Med. 11, 69–74 (2015).
Sharma, A., Dixit, A. M. & Krishnappa, K. A comparative study of sleep habits among medical and non-medical students in Saifai, Etawah. Int. J. Community Med. Public Health 5(9), 3876 (2018).
Haryati, H., Yunaningsi, S. P. & RAF, J. Factors affecting the sleep quality of Halu Oleo university medical school students. J. Surya Med. (Online) 5, 22–33 (2020).
Lundha, L. G. & Broman, J. E. Insomnia as an interaction between sleep-interfering and sleep-interpreting processes. J. Psychosom. Res. 49, 299–310 (2000).
Levenson, J. C., Shensa, A., Sidani, J. E., Colditz, J. B. & Primack, B. A. Social media use before bed and sleep disturbance among young adults in the United States: A nationally representative study. Sleep https://doi.org/10.1093/sleep/zsx113 (2017).
van den Eijnden, R. J. J. M., Geurts, S. M., Ter Bogt, T. F. M., van der Rijst, V. G. & Koning, I. M. Social media use and adolescents’ sleep: A longitudinal study on the protective role of parental rules regarding internet use before sleep. Int. J. Environ. Res. Public Health 18, 1346 (2021).
Ninama, N. J. & Kagathara, J. Sleep wake pattern analysis: Study of 131 medical students. NHL J. Med. Sci. 1, 33–36 (2012).
Ballesio, A., Lombardo, C., Lucidi, F. & Violani, C. Caring for the carers: Advice for dealing with sleep problems of hospital staff during the COVID-19 outbreak. J. Sleep Res. 30, e13096 (2021).
Gogi, P. V., Dayala, P. P. & Rayala, S. B. S. A study on prevalence of internet addiction in medical students and its relationship with personality traits. PARIPEX-Indian J. Res. 7, 53–54 (2018).
Jafari, H., Dadipoor, S. & Haghighi, H. The relationship between demographic variables and internet addiction among medical university students in Bandar Abbas. Life Sci. J. 11, 122–126 (2014).
Damor, R. B., Gamit, S. P. & Modi, A. Pattern of smart phone and internet usage among medical students in Surat, Gujarat: A cross sectional study. Natl. J. Community Med. 9, 469–473 (2018).
Mohammed, F. S., Thimmaiah, S. M. & Akshatha D. Internet addiction and its association with stress among medical students. Int. J. Med. Sci. Innov. Res. 4, 49–56 (2019).
Taha, M. H., Shehzad, K. & Alamro, A. S. Internet use and addiction among medical students in Qassim university, Saudi Arabia. Iran. J. Ichthyol. 19, 142 (2019).
Weiwei, C. et al. A study on the correlation between chronotype and quality of life among medical college students. Chin. J. Dis. Control Prev. 26, 1321–1325+1331 (2022).
Barayan, S. S., Dabal, B. K. A. & Abdelwahab, M. M. Health-related quality of life among female university students in Dammam district: Is Internet use related?. J Fam. Community Med. 25, 20 (2018).
Taylor, R. M., Gibson, F. & Franck, L. S. A concept analysis of health-related quality of life in young people with chronic illness. J. Clin. Nurs. 17, 1823–1833 (2008).
Megahed, M. M. Health-related quality of life among students at King Khalid University Mohail Asser. Int. J. Nurs. Sci. 4, 22–25 (2014).
Lins, L., Carvalho, F. M., Menezes, M. S., Porto-Silva, L. & Damasceno, H. Health-related quality of life of students from a private medical school in Brazil. Int. J. Med. Educ. https://doi.org/10.5116/ijme.563a.5dec (2015).
Joel, T., Dhanushree, N., Preetha, J., Rishtha, B. & Praisil, S. Health-related quality of life among medical students. J. Datta Meghe Inst. Med. Sci. Univ. 16, 25 (2021).
Karimy, M. et al. The association between internet addiction, sleep quality, and health-related quality of life among Iranian medical students. J. Addict. Dis. 38, 317–325 (2020).
Usmani, S. B., Bharti, P. & Bhatti, K. The effect of Internet addiction on the sleep pattern and quality of life among medical students. Int. J. Curr. Res. Rev. 13, 159–164 (2021).
Kayaba, M., Matsushita, T., Katayama, N., Inoue, Y. & Sasai-Sakuma, T. Sleep-wake rhythm and its association with lifestyle, health-related quality of life and academic performance among Japanese nursing students: A cross-sectional study. BMC Nurs. 20, 225 (2021).
Deeksha, S. & D’Souza, L. Does internet addiction affects sleep quality of pre-university students?. Int. J. Indian Psychol. https://doi.org/10.25215/0604.052 (2018).
Qi, M. et al. A latent profile analysis of PERMA: Associations with physical activity and psychological distress among Chinese nursing college students. Int. J. Environ. Res. Public Health 19, 16098 (2022).
Shi, M., Littlefield, A. K. & Stevens, A. K. Investigating differences in sex, race/ethnicity, and impulsivity across substance user profiles: A person-centered approach. J. Am. Coll. Health 69, 725–733 (2021).
Walker, S. N., Sechrist, K. R. & Pender, N. J. The health-promoting lifestyle profile: Development and psychometric characteristics. Nurs. Res. 36, 76–81 (1987).
Buysse, D. J., Reynolds, C. F. 3rd., Monk, T. H., Berman, S. R. & Kupfer, D. J. The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Res. 28, 193–213 (1989).
Liu, X. C. & Tang, M. Q. Reliability and validity of the Pittsburgh sleep quality index. Chin. J. Psychiatry 29, 103–107 (1996).
Bongiorno, C. et al. Sleep quality and sex-related factors in adult patients with immune-mediated diabetes: A large cross-sectional study. Acta Diabetol. 60, 663–672 (2023).
Zhang, W. et al. The relationship between images posted by new mothers on WeChat moments and postpartum depression: Cohort study. J. Med. Internet Res. 22, e23575 (2020).
Horne, J. A. & Ostberg, O. A self-assessment questionnaire to determine morningness-eveningness in human circadian rhythms. Int. J. Chronobiol. 4, 97–110 (1976).
Kerr, A. M., Spaeth, L. D. & Gerome, J. M. Medical students’ stress and uncertainty during the COVID-19 pandemic. Health Commun. 14, 1–11 (2022).
Hamaideh, S. H. Stressors and reactions to stressors among university students. Int. J. Soc. Psychiatry 57, 69–80 (2011).
Young, K. Internet addiction: The emergence of a new clinical disorder. Cyberpsychol. Behav. 1, 237–244 (1998).
Ding, C. S. Latent profile analysis. In Fundamentals of Applied Multidimensional Scaling for Educational and Psychological Research (ed. Ding, C. S.) 135–148 (Springer, 2018).
Lo, Y., Mendell, N. R. & Rubin, D. B. Testing the number of components in a normal mixture. Biometrika 88, 767–778 (2001).
Costa, P. S., Santos, N. C., Cunha, P., Cotter, J. & Sousa, N. The use of multiple correspondence analysis to explore associations between categories of qualitative variables in healthy ageing. J. Aging Res. 2013, 1–12 (2013).
Akaike, H. Factor analysis and AIC. Psychometrika 52, 317–332 (1987).
Schwarz, G. Estimating the dimension of a model. Ann. Stat. 6, 461–464 (1978).
Diehl, K., Jansen, C., Ishchanova, K. & Hilger-Kolb, J. Loneliness at universities: Determinants of emotional and social loneliness among students. Int. J. Environ. Res. Public Health 15, 1865 (2018).
Arzani-Birgani, A., Zarei, J., Favaregh, L. & Ghanaatiyan, E. Internet addiction, mental health, and sleep quality in students of medical sciences, Iran: A cross-sectional study. J. Educ. Health Promot. 10, 409 (2021).
Hadar, L., Ergas, O., Alpert, B. & Ariav, T. Rethinking teacher education in a VUCA world: Student teachers’ social-emotional competencies during the Covid-19 crisis. Eur. J. Teach. Educ. 43, 1–14 (2020).
Whiteman, S. D., Barry, A. E., Mroczek, D. K. & Macdermid Wadsworth, S. The development and implications of peer emotional support for student service members/veterans and civilian college students. J. Couns. Psychol. 60, 265–278 (2013).
Nasser, A. M. A. & Zhang, X. Knowledge and factors related to smoking among university students at Hodeidah University, Yemen. Tob. Induc. Dis. 17, 42 (2019).
Nuñez, A. et al. Smoke at night and sleep worse? The associations between cigarette smoking with insomnia severity and sleep duration. Sleep Health 7, 177–182 (2021).
Lai, P. P. & Say, Y. H. Associated factors of sleep quality and behavior among students of two tertiary institutions in northern Malaysia. Med. J. Malays. 68, 195–203 (2013).
James, B. O., Omoaregba, J. O. & Igberase, O. O. Prevalence and correlates of poor sleep quality among medical students at a Nigerian university. Ann. Afr. Med. 5, 1–5 (2011).
Wu, Y., Qi, L., Liu, Y., Hao, X. & Zang, S. Development and psychometric testing of a learning behaviour questionnaire among Chinese undergraduate nursing students. BMJ Open 11, e043711 (2021).
Sert, H. P. & Başkale, H. Students’ increased time spent on social media, and their level of coronavirus anxiety during the pandemic predict increased social media addiction. Health Inf. Libr. J. https://doi.org/10.1111/hir.12448 (2022).
Pang, H. Examining associations between university students’ mobile social media use, online self-presentation, social support and sense of belonging. Aslib J. Inf. Manag. 72, 321–338 (2020).
Yao, T., Zheng, Q. & Fan, X. The impact of online social support on patients’ quality of life and the moderating role of social exclusion. J. Serv. Res. 18, 369–383 (2015).
Bhandari, P. M. et al. Sleep quality, internet addiction and depressive symptoms among undergraduate students in Nepal. BMC Psychiatry 17, 106 (2017).
Nakayama, K. et al. Comprehensive health literacy in Japan is lower than in Europe: A validated Japanese-language assessment of health literacy. BMC Public Health 15, 505 (2015).
Premkumar, K. et al. Self-directed learning readiness of Indian medical students: A mixed method study. BMC Med. Educ. 18, 134 (2018).
Tsai, H. J. et al. Effectiveness of digital cognitive behavioral therapy for insomnia in young people: Preliminary findings from systematic review and meta-analysis. J. Pers. Med. 12, 481 (2022).
Hershner, S. & O’Brien, L. M. The impact of a randomized sleep education intervention for college students. J. Clin. Sleep Med. 14, 337–347 (2018).
Yasin, D. & Mustafa, K. Relationships among internet addiction, academic motivation, academic procrastination, and school attachment in adolescents. Int. Online J. Educ. Sci. https://doi.org/10.15345/iojes.2018.05.020 (2018).
Sutay, S. S., Sheikh, N. A., Rath, R. S. & Vasudeva, A. Sleep patterns, issues, reasons for sleep problems, and their impact on academic performance among first-year medical students in central India. Maedica (Bucur.) 17, 97–102 (2022).
Delgado, C., Upton, D., Ranse, K., Furness, T. & Foster, K. Nurses’ resilience and the emotional labour of nursing work: An integrative review of empirical literature. Int. J. Nurs. Stud. 70, 71–88 (2017).
Carpi, M., Marques, D. R., Milanese, A. & Vestri, A. Sleep quality and insomnia severity among Italian university students: A latent profile analysis. J. Clin. Med. 11, 4069 (2022).
Wu, X. et al. Association between circadian rhythm and sleep quality among nursing interns: A latent profile and moderation analysis. Front. Neurosci. 16, 995775 (2022).
Baek, Y., Jung, K., Kim, H. & Lee, S. Association between fatigue, pain, digestive problems, and sleep disturbances and individuals’ health-related quality of life: A nationwide survey in South Korea. Health Qual. Life Outcomes. https://doi.org/10.1186/s12955-020-01408-x (2020).
Nagori N., Vala A. & Panchal B. Association of anxiety and quality of life with internet addiction among medical students. Natl. J. Integr. Res. Med. 7, 9–13 (2016).
Sasawaki, Y. & Shiotani, H. The influence of chronotype and working condition on sleep status and health related quality of life of daytime office workers. Kobe J. Med. Sci. 64, 189–196 (2018).
Arora, T., Broglia, E., Thomas, G. N. & Taheri, S. Associations between specific technologies and adolescent sleep quantity, sleep quality, and parasomnias. Sleep Med. 15, 240–247 (2014).
Teresa, A. et al. Exploring the complex pathways among specific types of technology, self-reported sleep duration and body mass index in UK adolescents. Int. J. Obes. 37, 1254–1260 (2013).
Sun, J., Chen, M. & Cai, W. Chronotype: Implications for sleep quality in medical students. Chronobiol. Int. 36, 1–9 (2019).
Martino, M. M. & Lopes, D. Impact of learning and sleep characteristics in nursing students. Int. J. Sci. Commer. Hum. 1, 33–42 (2013).
Carciofo, R. Morningness–eveningness and affect: The mediating roles of sleep quality and metacognitive beliefs. Sleep Biol. Rhythms 18, 17–26 (2020).
Mozafari, A., Tabaraie, M. & Mohammadi-Tahrodi, M. H. Morningness–eveningness chronotypes, insomnia and sleep quality among medical students of Qom. J. Sleep Sci. 1, 67–73 (2016).
Chern, K.-C. & Huang, J.-H. Internet addiction: associated with lower health-related quality of life among college students in Taiwan, and in what aspects?. Comput. Hum. Behav. 84, 460–466 (2018).
Glavin, E. E. et al. Relationships between sleep, exercise timing, and chronotype in young adults. J. Health Psychol. 26, 2636–2647 (2021).
Gonzalo, J. D., Dekhtyar, M., Hawkins, R. E. & Wolpaw, D. R. How can medical students add value? Identifying roles, barriers, and strategies to advance the value of undergraduate medical education to patient care and the health system. Acad. Med. 92, 1294–1301 (2017).
Acknowledgements
The authors gratefully acknowledge the participants who participated in this study.
Funding
This research was funded by Undergraduate Teaching Reform Research Project of China Medical University (No. 2023).
Author information
Authors and Affiliations
Contributions
L.Y. and Y.W. prepared conceptualization; Y.W. prepared methodology; Y.W. prepared software; L.Y., Y.W. and S.Z. prepared validation; Y.W. prepared formal analysis; Q.Q., L.Y. and Y.W. prepared investigation; L.Y. prepared data cu-ration; L.Y. and Y.W. wrote the original draft; S.Z., X.W., and C.G. review and editing draft; X.W. and Q.Q. prepared visualization; S.Z. prepared supervision; S.Z. prepared project administration. All authors have read and agreed to the published version of the manuscript. The participant has consented to the submission of the case report to the journal.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yu, L., Wu, Y., Guo, C. et al. Latent profile analysis for health-related quality of life, sleep quality, morning and evening type, and internet addiction among medical students. Sci Rep 13, 11247 (2023). https://doi.org/10.1038/s41598-023-38302-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-38302-7
- Springer Nature Limited