Abstract
The present study aimed to explore whether chromosomal polymorphisms (CPs) have negative effects on reproductive outcomes of in vitro fertilization/intracytoplasmic sperm injection-embryo transfer (IVF/ICSI-ET)/frozen-thawing embryo transfer (FET)? We conducted a retrospective study consisting of 21,867 assisted reproductive technology treatment cycles, among which, fresh embryo transfer cycles accounted for 10,400, and the rest were FET cycles. According to karyotype of CPs, the former was grouped as: group 1 (male carrier, n = 425), group 2 (female carrier, n = 262), and group 3 (couple without CPs, n = 9713). Accordingly, FET cycles were divided into 3 groups: group 4 (male carrier, n = 298), group 5 (female carrier, n = 311), and group 6 (couple without CPs, n = 10,858). The embryo implantation rate (IR), clinical pregnancy rate (CPR), live birth rate (LBR), and early miscarriage rate (EMR) were compared among the groups. In fresh embryo transfer cycles after IVF/ICSI, there were no significant differences in the infertility duration, BMI, basal FSH, no. of oocyte, no. of 2PN, endometrial thickness on trigger day, serum E2, P, and LH level on trigger day (P > 0.05). The female age, no. of 2PN embryo cleavage, top-quality embryo, and no. of embryo transferred were significantly different among groups (P < 0.05). The IR was 38.8%, 36.2%, and 34.0% in groups 1, 2, and 3, respectively. The CPR was 55.1%, 52.3%, and 49.7%, respectively. The LBR was 36.9%, 37.4%, and 36.4%, respectively. The CPR and LBR showed no significant differences among groups. The IR was lower and the EMR was higher in group 3 than those of groups 1 and 2. Binary logistic regression analysis indicated that female age, no. of embryo transferred, EMT, LH, and P on the trigger day were independently factors associated with CPR. Besides, no. of embryo transferred, and EMT on trigger day were associated with LBR, while the CPs was not related with CPR and LBR after IVF/ICSI-ET. In FET cycles, the infertility duration was similar (P > 0.05), but the female age, BMI, no. of embryo transferred were significantly different among groups (P > 0.05). The IR was 24.3%, 23.6% and 22.3% in group 4, 5, and 6, receptivity. The CPR was 31.8%, 30.9%, and 30.0%, the LBR was 23.8%,26.3%, and 23.8%, while the EMR was 12.6%, 13.1%, 14.4%, respectively. The IR, CPR, EMR, and LBR showed no significant differences among groups (P > 0.05). Binary logistic regression analysis indicated that female age, infertility duration, and no. of embryo transferred were independently factors affecting CPR and LBR after FET. The CPs were not associated with CPR and LBR after FET. The results suggested that uniparental carrying of CPs have no effects on the reproductive outcomes after IVF/ICSI-ET/FET. However, it is not clear whether both parents carrying CPs would affect pregnancy outcome.
Similar content being viewed by others
Introduction
Chromosomal polymorphisms (CPs) are defined as the heritable variants of segments located in heterochromatic chromosomal regions, including variations in heterochromatic segments, satellites and satellite stalks1. On non-acrocentric chromosomes, CPs typically occur in the heterochromatic regions of the long arms of chromosomes 1, 9, and 16 in human, as well as in the distal heterochromatic region of the Y chromosome (qh+)2. For acrocentric chromosomes, such as those in D and G groups, variations occur usually on satellites, satellite stalks, or short arms3. In addition, pericentric inversions on chromosomes 1, 2, and 9 are also considered as polymorphisms1,4.
The incidence of CPs is about 2–5% in the general population5. Because heterochromatic regions are rich in highly repetitive satellite DNA sequences, and with no coding proteins, CPs are generally regarded as harmless variants and have no functional or phenotypic effects on the CPs carriers6.
However, these “harmless” regions seem to be associated with many reproductive abnormalities. Recently, an increasing number of researches have shown an increased incidence of CPs variations in infertile couples7, recurrent pregnancy loss (RPL) or spontaneous miscarriages8,9.
Assisted reproductive technology (ART) was an effective treatment for infertility. Some reports suggested there were bad impacts of CPs on ART outcomes, while the others showed that the CPs had no negative effects on the pregnancy outcomes after IVF/ICSI-ET10,11. Studies by Li and Xu et al. showed that both male and female carriers have adverse impacts on reproductive outcomes after fresh IVF/ICSI-ET cycles6,12. But there were also some studies reporting that only male carriers of CPs had poor pregnancy outcomes after IVF/ICSI-ET treatment4,6,13,14,15. However, aforementioned studies only included fresh IVF/ICSI-ET cycles. Therefore, the impact of CPs on IVF/ICSI/FET outcomes is still controversial, and its impacts on pregnancy outcomes of FET were unclear.
To further explore the associations between CPs and ART endpoints, especially pregnancy outcomes in FET, we conducted this retrospective study. This research might gain our understanding of reproductive outcomes after IVF/ICSI-ET/FET in CPs carriers.
Materials and methods
Subjects
The retrospective study was conducted using the data of infertile couples undergoing fresh IVF/ICSI-ET or FET treatments from January 2010 to December 2021 in the Reproductive Medicine Center, Xiangya Hospital, Central South University. The present research was approved by the ethical committee of Xiangya Hospital, Central South University. and was exempted from informed consent requirements owing to its retrospective design.
The inclusion criteria were as follows: age 20–40 years; BMI 18–30 kg/m2; 3 U/L < bFSH < 10 U/L; infertile couples ever underwent karyotype test. The subjects met the following criteria were excluded: abnormal chromosome karyotypes; endometrial abnormalities; severe adenomyosis or hydrosalpinx; PGT cycles; cycles with donor oocyte.
Subdivisions of study groups
For fresh IVF/ICSI-ET treatment, the participants were divided into three groups. Group 1 (male carrier) included the couples where only male was CPs carrier but female was not; group 2 (female carrier) meant the couples that only female was CPs carrier but male was not; group 3 referred to the couples that neither male nor female were CPs carriers. Accordingly, for FET treatment, all cycles were divided into three groups: group 4 (male carrier), group 5 (female carrier), and group 6 (both male and female without CPs carrier).
Ovarian stimulation and embryo transfer
The ovarian stimulation protocol was performed as described in our previous studies16. GnRH-a 0.05–0.10 mg was administered daily from 7 days after ovulation and lasted for 14–16 days (the long protocol), or injected at day 2 to day 8 of menstrual cycle (for modified short protocol). In the GnRH-a long protocol, leuprorelin acetate 3.75 mg was injected on day 2–5 of the menstrual cycle, and Gn was injected 30–35 days later. In the ultra-long protocol, leuprorelin 3.75 mg was administrated every 28 days and gave 2–3 times, and Gn was injected 21 days after the last injection.
Follicular development and endometrium were monitored with transvaginal ultrasounds. Once there were 3 follicles diameter ≥ 17 mm, women were triggered with 6000–10,000 IU hCG, and oocyte retrieval was performed 36 h later. IVF or ICSI was performed according to sperm quality. No more than two embryos were transferred 72 h after oocyte retrieval.
Endometrium preparation protocol for FET
The endometrium preparation was performed as described previously17,18. In the natural cycle (NC) FET, the dominant follicle and endometrium were monitored from the day 10 of menstrual cycle. No more than 2 frozen-thaw embryos were transferred 3 or 5 days after ovulation. In the hormone replacement treatment (HRT) cycle, estradiol valerate was given from day 3 and last at least 12 days. Progesterone was administered if the endometrial thickness was ≥ 7 mm, and one or two embryos were transferred 3 or 5 days after progesterone administration. In the ovulation induction cycles, letrozole was given from day 3 to day 7, and 37.5 IU-75 IU HMG was administrated if necessary. 10,000 IU hCG was injected for trigger. One or two embryos were transferred 5 days after ovulation.
Outcomes
The primary outcomes were live birth and clinical pregnancy, and the secondary outcomes were embryo implantation, and early miscarriage. Clinical pregnancy was confirmed by ultrasound visualization of a gestational sac 28–35 days after embryo transfer. Early miscarriage was defined as pregnancy loss before 12 gestational weeks.
Statistical analysis
All data were analyzed with SPSS 25.0. Continuous data were showed as the mean ± standard deviation (SD), and a Student’s t-test was performed. Categorical data were described as frequencies or percentages and analyzed using a Chi-square test. The association of clinical pregnancy and live birth with cycle characteristic were analyzed by multivariate logistic regression analysis. P < 0.05 was set to be statistically significant.
Ethics approval and consent to participate
The ethical committee of Xiangya Hospital, Central South University approved this study, and the study was conducted according to the Declaration of Helsinki.
Results
For fresh IVF/ICSI-ET, 10400 fresh IVF/ICSI-ET cycles were enrolled, including 425 male CPs carriers (group 1), 262 female CPs carriers and 9713 non-carriers (group 3). For FET, 11467 FET cycles were included in the present study, in which there were 298 male CPs carriers (group 4), 311 female CPs carriers (group 5), and 10,858 non-carriers (group 6).
The baseline characteristics of eligible subjects were showed in Tables 1 and 2. For fresh IVF/ICSI-ET cycles, the age of women (29.46 ± 4.13 vs. 30.03 ± 3.93 vs. 30.74 ± 4.12, P = 0.000), total dosage of Gn (2118.81 ± 767.98 vs. 1900.52 ± 781.09 vs. 2106.36 ± 844.19, P = 0.000), duration of COS (11.13 ± 2.64 vs. 10.42 ± 2.56 vs. 10.94 ± 2.73, P = 0.003), no. of top-quality embryo (3.66 ± 2.34 vs. 3.40 ± 2.70 vs. 3.92 ± 2.67, P = 0.001), no. of embryo transferred (1.78 ± 0.42 vs. 1.85 ± 0.36 vs. 1.88 ± 0.33, P = 0.000), P level on trigger day (0.71 ± 0.36 vs. 0.77 ± 0.38 vs. 0.76 ± 0.38, P = 0.018) were different among groups. For FET cycles, female age (30.44 ± 4.10 vs. 30.70 ± 4.08 vs. 31.32 ± 4.11, P = 0.000), BMI (21.85 ± 2.50 vs. 21.49 ± 2.65 vs. 21.89 ± 2.53, P = 0.019), and the no. of embryo transferred (1.74 ± 0.44 vs. 1.76 ± 0.43 vs. 1.80 ± 0.40, P = 0.016) were significantly different among groups.
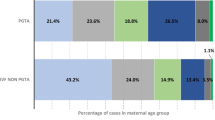
As shown in Table 3, the clinical pregnancy rate (55.0% vs. 52.3% vs. 49.7%, P = 0.071) and live birth rate (36.9% vs. 37.4% vs. 36.4%, P = 0.917) were not significantly different among groups after fresh IVF/ICSI-ET treatment. There were significantly differences in early miscarriage rate (10.7% vs.6.6% vs. 13.3%, P = 0.039) and embryo implantation rate (38.8% vs. 36.2% vs. 34.5%, P = 0.047) among groups. The clinical pregnancy outcomes after FET were showed in Table 4. There were no significant differences in clinical pregnancy rate (31.8% vs. 30.9% vs. 30%, P = 0.667), live birth rate (23.8% vs. 26.3% vs. 23.8%, P = 0.486), implantation rate (24.3% vs. 23.6% vs. 22.3%, P = 0.326), and early miscarriage rate (12.6% vs. 13.1% vs. 14.4%, P = 0.741) among groups.
The association of clinical pregnancy and live birth with cycle characteristics were assessed with logistic regression analysis. For clinical pregnancy after fresh IVF/ICSI-ET (Table 5), CPs carrier (P < 0.05), no. of embryo transferred (P < 0.01), endometrial thickness (P < 0.01), LH (P < 0.01), and P level on trigger day (P < 0.05) were correlated with clinical pregnancy. For live birth after fresh IVF/ICSI-ET, no. of embryo transferred (P < 0.01) and endometrial thickness (P < 0.01) were associated with live birth. For FET cycles (Table 6), female age (P < 0.01), duration of infertility (P < 0.01), and no. of embryo transferred (P < 0.01) were associated with clinical pregnancy and live birth.
Discussion
To the best of our knowledge, this is the first large sample size study (n = 21867) involving fresh cycles and FET cycles to comprehensively explore the effect of CPs on reproductive outcomes of ART. In this retrospective study, we found that CPs have no negative effects on pregnancy outcomes after fresh IVF/ICSI-ET and FET treatment.
CPs was considered to be benign and harmless. However, recently, some researchers have found that the heterochromatin in CP regions might inhibit or silence gene expression through the reversible transformation between heterochromatin and euchromatin19,20. Besides, other studies have shown that the heterochromatin located at the centromeres, played a vital role in cell division. Chromatin mutation in these regions may lead to abnormal division of meiotic cell, such as defective in centromeres function and centromere assembly, difficulty in homologous chromosome pairing, and disrupted cell division, which can affect the formation of functional sperm21.
The impact of CPs on outcomes after ART was explored by previous studies, but the results were inconclusive and remained controversial. Early in 2005, Yakin et al. enrolled infertile man receiving ICSI treatment, and found that CPR and IR were significantly lower for men with CPs than that without CPs15. Similarly, a few of studies12,14 suggested that CPs had detrimental effects on spermatogenesis, negatively affected the outcomes of IVF/ICSI-ET treatment. Li et al. reported that individual genetic counseling should be afforded according to the polymorphism types6. However, researches by Hong et al. indicated that CPs appeared to have no adverse effects on the outcome of IVF-ET treatment4,11, inv(9) in one partner has satisfactory outcomes10. There were studies found that couples with CPs in male carriers have poor pregnancy outcomes after IVF-ET, with higher EMR and lower LBR after a complete cycle13.
In present study, the female age was younger in groups 1 and 2 than that in group 3. In contrast with previous studies, we did not find that male carrying CPs was associated with outcomes after ART. Our results suggested female carrying CPs led to less 2PN cleavage embryos and top-quality embryos, which might result from less Gn dosage and short duration of COS. Besides, the CPR and LBR were not significantly different among groups, although the no. of embryo transferred in the group 3 was more than that in the rest groups. The EMR was higher in group 3 than that in other groups, and this may partly resulted from the female age.
In FET cycles, the female age was older and the no. of embryos transferred was higher in group 6 than that of groups 4 and 5. The IVF outcomes, including CPR, LBR, IR, and the EMR, were all similar among groups after FET treatment. The results of our study were inconsistent with previous studies indicating that the risk of miscarriage increased when the male partner had a large Y chromosome22,23. Then, using a logistic regression model, we found that no. of embryo transferred and endometrial thickness were associated with outcomes after fresh IVF/ICSI-ET. And female age, duration of infertility, and no. of embryo transferred were related with outcomes after FET treatment. CPs seems have no effects on outcomes after embryo transfer.
The strength of this study was its large sample size involving 21,867 transfer cycles. On the whole, CPs had no significant negative effects on the clinical outcomes of ART treatment. In addition, the present study firstly assessed the impact of CPs on FET outcomes. The results of the present study indicated the CPs have no negative impacts on the embryo quality and endometrial receptivity. At last, the live birth rate was followed-up, and defined as the primary outcome.
Certainly, this study has a few limitations. Firstly, it was a retrospective study, and the potential heterogeneity and possible confounding factors were inevitable. Besides, we did not stratified infertility according to the specific type of CPs, and subject carrying any type of CPs was considered as a carrier. Despite these drawbacks, this study reflected a real state without intervention in the real world.
Conclusion
The clinical pregnancy and live birth of IVF/ICSI-ET and FET treatment did not appear to be adversely affected by CPs. Only female CPs carrier led to lower 2PN cleavage rate. In addition, the chromosome analysis method in this study had a band resolution of 400–550 BPHS; therefore, it was difficult to distinguish some potential variations from common polymorphism variations. Therefore, further research with more sensitive techniques is needed.
Data availability
The datasets supporting the conclusions of this article are included within the article.
Abbreviations
- ART:
-
Assisted reproductive technology
- IVF:
-
In vitro fertilization
- ICSI:
-
Intracytoplasmic sperm injection
- FET:
-
Frozen-thawing embryo transfer
- PGT:
-
Preimplantation genetic testing
- CPs:
-
Chromosomal polymorphisms
References
Simons, A., Shaffer, L. G. & Hastings, R. J. Cytogenetic nomenclature: Changes in the ISCN 2013 compared to the 2009 edition. Cytogenet. Genome Res. 141(1), 1–6 (2013).
Repping, S. et al. High mutation rates have driven extensive structural polymorphism among human Y chromosomes. Nat. Genet. 38(4), 463–467 (2006).
Madon, P. F., Athalye, A. S. & Firuza, R. P. Polymorphic variants on chromosomes probably play a significant role in infertility. Reprod. Biomed. Online 11(6), 726–732 (2005).
Liang, J. et al. Effect of chromosomal polymorphisms of different genders on fertilization rate of fresh IVF–ICSI embryo transfer cycles. Reprod. Biomed. Online 29(4), 436–444 (2014).
Hsu, L. Y., Benn, P. A., Tannenbaum, H. L., Perlis, T. E. & Carlson, A. D. Chromosomal polymorphisms of 1, 9, 16, and Y in 4 major ethnic groups: A large prenatal study. Am. J. Med. Genet. 26(1), 95–101 (1987).
Li, S. et al. Chromosomal polymorphisms associated with reproductive outcomes after IVF-ET. J. Assist. Reprod. Gen. 37(7), 1703–1710 (2020).
Nadă, E. S. et al. Current opportunities and new horizons into the genetic study of infertility. Rom. J. Morphol. Embryol. 62(1), 191–200 (2021).
Chakraborty, A., Kar, S., Mohapatra, P. C. & Banerjee, B. A case-control study identifying the frequency and spectrum of chromosomal anomalies and variants in a cohort of 1000 couples with a known history of recurrent pregnancy loss in the Eastern region of India. J. Hum. Reprod. Sci. 14(4), 422–430 (2021).
Sahin, F. I. et al. Chromosome heteromorphisms: An impact on infertility. J. Assist. Reprod. Genet. 25(5), 191–195 (2008).
Liang, S., Yang, J., Wu, H., Teng, X. & Duan, T. Effects of chromosome 9 inversion on IVF/ICSI: A 7-year retrospective cohort study. Mol. Genet. Genom. Med. 7(9), e856 (2019).
Hong, Y., Zhou, Y.-W., Tao, J., Wang, S.-X. & Zhao, X. Do polymorphic variants of chromosomes affect the outcome of in vitro fertilization and embryo transfer treatment?. Hum. Reprod. 26(4), 933–940 (2011).
Xu, X. et al. The effect of chromosomal polymorphisms on the outcomes of fresh IVF/ICSI-ET cycles in a Chinese population. J. Assist. Reprod. Genet. 33(11), 1481–1486 (2016).
Ni, T. et al. Male chromosomal polymorphisms reduce cumulative live birth rate for IVF couples. J. Assist. Reprod. Genet. 34(8), 1017–1025 (2017).
Guo, T. et al. The role of male chromosomal polymorphism played in spermatogenesis and the outcome of IVF/ICSI-ET treatment. Int. J. Androl. 35(6), 802–809 (2012).
Yakin, K., Balaban, B. & Urman, B. Is there a possible correlation between chromosomal variants and spermatogenesis?. Int. J. Urol. 12(11), 984–989 (2005).
Yang, T. et al. Associations between dyslipidaemia and pregnancy outcomes in the first complete cycle of IVF/ICSI: A real-world analysis. Reprod. Biomed. Online 43(6), 1095–1105 (2021).
Zhao, J., Yan, Y., Huang, X., Sun, L. & Li, Y. Blastocoele expansion: An important parameter for predicting clinical success pregnancy after frozen-warmed blastocysts transfer. Reprod. Biol. Endocrinol. 17, 15 (2019).
Zhu, L., Che, H. S., Xiao, L. & Li, Y. P. Uterine peristalsis before embryo transfer affects the chance of clinical pregnancy in fresh and frozen-thawed embryo transfer cycles. Hum. Reprod. 29(6), 1238–1243 (2014).
Traldi, J. B. et al. First karyotype description of Hypostomus iheringii (Regan, 1908): A case of heterochromatic polymorphism. Comp. Cytogenet. 6(2), 115–125 (2012).
Leach, T. J., Chotkowski, H. L., Wotring, M. G., Dilwith, R. L. & Glaser, R. L. Replication of heterochromatin and structure of polytene chromosomes. Mol. Cell Biol. 20(17), 6308–6316 (2000).
Gerton, J. L. & Hawley, R. S. Homologous chromosome interactions in meiosis: Diversity amidst conservation. Nat. Rev. Genet. 6(6), 477–487 (2005).
Nielsen, J. Large Y, chromosome (Yq+) and increased risk of abortion. Clin. Genet. 13(5), 415–416 (1978).
Genest, P. Chromosome variants and abnormalities detected in 51 married couples with repeated spontaneous abortions. Clin. Genet. 16(6), 387–389 (1979).
Funding
This project was supported by Natural Science Foundation of Hunan Province of China (No. 2021JJ31128).
Author information
Authors and Affiliations
Contributions
Z.J. contributed to the study design and acquisition of data, article drafting and revising as well as organization of the final approval of the version to be published. H.B. contributed substantially to the interpretation of the data and helped with revision of the article. H.J. contributed significantly to the acquisition, analysis and interpretation of the data. X.B. and L.Y. contributed to conception and design, acquisition of data and analysis and interpretation of data.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhao, J., Huang, B., Hao, J. et al. Chromosomal polymorphisms have no negative effect on reproductive outcomes after IVF/ICSI-ET/FET. Sci Rep 12, 19052 (2022). https://doi.org/10.1038/s41598-022-20132-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-20132-8
- Springer Nature Limited
This article is cited by
-
Diverse impacts of female chromosomal polymorphisms on assisted reproduction outcomes: a retrospective cohort study
BMC Pregnancy and Childbirth (2024)