Abstract
Objective
The objective of this study is to compare glomerular and tubular functions in small for gestational age (SGA) and appropriate for gestational age (AGA) preterm infants.
Study Design
A prospective controlled study was conducted on SGA and AGA infants with gestational ages between 320/7 and 366/7 weeks, who received gentamycin in the first 72 h of life. Glomerular and tubular functions were assessed on days 1 and 5.
Results
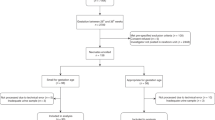
Fifty (25 SGA and 25 AGA) infants were included. On day of life 1, SGA group had higher serum sodium, serum urea, and urinary creatinine. On day 5, SGA infants had significant increase in serum creatinine (p = 0.04). Urinary NAG and FeNa were comparable among the two groups on days 1 and 5.
Conclusions
Glomerular functions were compromised in SGA preterm infants. Tubular functions were comparable.

Similar content being viewed by others
References
Antolik TL, Cunningham KJ, Alabsi S, Reimer RA. Empirical gentamicin dosing based on serum creatinine levels in premature and term neonates. Am J Health Syst Pharm. 2017;74:466–72. 2.
Stritzke A, Thomas S, Amin H, Fusch C, Lodha A. Renal consequences of preterm birth. Mol Cell Pediatr. 2017;4:2.
Konje JC, Okaro CI, Bell SC, de Chazal R, Taylor DJ. A cross-sectional study of changes in fetal renal size with gestation in appropriate- and small-for-gestational-age fetuses. Ultrasound Obstet Gynecol. 1997;10:22–6.
Aly H, Davies J, El-Dib M, Massaro A. Renal function is impaired in small for gestational age premature infants. J Matern Fetal Neonatal Med. 2013;26:388–91.
Hitron AE, Sun Y, Scarpace SB. Accuracy of empiric gentamicin dosing guidelines in neonates. J Pediatr Pharm Ther. 2010;15:264–73.
Fenton TR. A new growth chart for preterm babies: Babson and Benda’s chart updated with recent data and a new format. BMC Pediatr. 2003;3:13.
Crumby T, Rinehart E, Carby MC, Kuhl D, Talati AJ. Pharmacokinetic comparison of nomogram-based and individualized vancomycin regimens in neonates. Am J Health Syst Pharm. 2009;66:149–53.
Giapros VI, Cholevas VI, Andronikou SK. Acute effects of gentamicin on urinary electrolyte excretion in neonates. Pediatr Nephrol. 2004;19:322–5.
Giapros V, Papadimitriou P, Challa A, Andronikou S. The effect of intrauterine growth retardation on renal function in the first two months of life. Nephrol Dial Transpl. 2007;1:96–103.
Kellum JA, Lameire N, KDIGO AKI. Guideline Work Group. Diagnosis, evaluation, and management of acute kidney injury: a KDIGO summary (Part 1). Crit Care. 2013;17:204.
Jetton JG, Guillet R, Askenazi DJ, Dill L, Jacobs J, Kent AL, et al. Assessment of worldwide acute kidney injury epidemiology in neonates: design of a retrospective cohort study. Front Pediatr. 2016;4:68.
Zhu J, Xing Y, Wang X-L. [A preliminary study of renal function in small-for-gestational-age infants at early stage after birth]. Zhongguo Dang Dai Er Ke Za Zhi. 2017;19:389–92.
Vehaskari VM, Aviles DH, Manning J. Prenatal programming of adult hypertension in the rat. Kidney Int. 2001;59:238–45.
Gubhaju L, Sutherland MR, Yoder BA, Zulli A, Bertram JF, Black MJ. Is nephrogenesis affected by preterm birth? Studies in a non-human primate model. Am J Physiol Ren Physiol. 2009;297:F1668–77.
Harris RC, Cheng H. Telomerase, autophagy and acute kidney injury. Nephron. 2016;134:145–8.
Puddu M, Fanos V, Podda F, Zaffanello M. The kidney from prenatal to adult life: perinatal programming and reduction of number of nephrons during development. Am J Nephrol. 2009;30:162–70.
Lulic-Botica M, Sheer T, Edwards D, Thomas RL, Natarajan G. Impact of small-for-gestational age (SGA) status on gentamicin pharmacokinetics in neonates. J Clin Pharm. 2014;54:39–45.
Zanardo V, Giacobbo F, Zambon P, Trevisanuto D, Griffith P, Grella P, et al. Antenatal aminophylline and steroid exposure: effects on glomerular filtration rate and renal sodium excretion in preterm newborns. J Perinat Med. 1990;18:283–8.
al-Dahan J, Stimmler L, Chantler C, Haycock GB. The effect of antenatal dexamethasone administration on glomerular filtration rate and renal sodium excretion in premature infants. Pedia Nephrol. 1987;1:131–5.
Go H, Momoi N, Kashiwabara N, Haneda K, Chishiki M, Imamura T, et al. Neonatal and maternal serum creatinine levels during the early postnatal period in preterm and term infants. PLoS ONE. 2018;13:e0196721. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5967735/
Iacobelli S, Bonsante F, Ferdinus C, Labenne M, Gouyon J-B. Factors affecting postnatal changes in serum creatinine in preterm infants with gestational age <32 weeks. J Perinatol. 2009;29:232–6.
Auron A, Mhanna MJ. Serum creatinine in very low birth weight infants during their first days of life. J Perinatol. 2006;26:755–60.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Aly, H., Ez El Din, Z., Soliman, R.M. et al. Renal function in small for gestational age preterm infants. J Perinatol 39, 1263–1267 (2019). https://doi.org/10.1038/s41372-019-0431-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0431-9
- Springer Nature America, Inc.
This article is cited by
-
The impact of intrauterine growth restriction and prematurity on nephron endowment
Nature Reviews Nephrology (2023)
-
Effect of fetal growth restriction on urinary podocalyxin levels at birth in preterm neonates
Pediatric Research (2021)