Abstract
Endothelin-1 (ET-1) is essential for mammalian development and life, but it has also been implicated in increased cardiovascular risk under pathophysiological conditions. The aim of this study was to determine the impact of endothelial overexpression of the prepro-endothelin-1 gene on endothelium-dependent and endothelium-independent responses in the conduit and renal arteries of lean and obese mice. Obesity was induced by high-fat-diet (HFD) consumption in mice with Tie-1 promoter-driven, endothelium-specific overexpression of the prepro-endothelin-1 gene (TEThet) and in wild-type (WT) littermates on a C57BL/6N background. Isometric tension was measured in rings (with endothelium) of the aorta (A), carotid (CA) and iliac (IA) arteries as well as the main (MRA) and segmental renal (SRA) arteries; all experiments were conducted in the absence or presence of L-NAME and/or the COX inhibitor meclofenamate. The release of prostacyclin and thromboxane A2 was measured by ELISA. In the MRA, TEThet per se increased contractions to endothelin-1, but the response was decreased in SRA in response to serotonin; there were also improved relaxations to acetylcholine but not insulin in the SRA in the presence of L-NAME. HFD per se augmented the contractions to endothelin-1 (MRA) and to the thromboxane prostanoid (TP) receptor agonist U46619 (CA, MRA) as well as facilitated relaxations to isoproterenol (A). The combination of HFD and TEThet overexpression increased the contractions of MRA and SRA to vasoconstrictors but not in the presence of meclofenamate; this combination also augmented further relaxations to isoproterenol in the A. Contractions to endothelin-1 in the IA were prevented by endothelin-A receptor antagonist BQ-123 but only attenuated in obese mice by BQ-788. The COX-1 inhibitor FR122047 abolished the contractions of CA to acetylcholine. The release of prostacyclin during the latter condition was augmented in samples from obese TEThet mice and abolished by FR122047. These findings suggest that endothelial TEThet overexpression in lean animals has minimal effects on vascular responsiveness. However, if comorbid with obesity, endothelin-1-modulated, prostanoid-mediated renal arterial dysfunction becomes apparent.
Similar content being viewed by others
Introduction
The potent vasoconstrictor peptide endothelin-1 (ET-1)1 is essential for mammalian development and life2 but it has also been implicated in increased cardiovascular risk under pathophysiological conditions1,3,4,5,6,7,8. The production of ET-1 is encoded by the prepro-ET-1 gene and is succeeded by the production of prepro-ET-1 and subsequently big ET-11,9. The latter is converted to the vasoactive ET-1 peptide, which induces contractions of vascular smooth muscle upon activation of endothelin-A (ETA) as well as endothelin-B (ETB) receptors, both of which can be blocked individually with specific receptor antagonists1,9,10,11,12. Obesity augments ET-1-mediated ETA receptor-dependent vasoconstrictor tone in humans in vivo4,7,8 and increases prepro-ET-1 gene expression in the arteries of mice fed a high-fat diet13. However, the impact of overexpressing the prepro-ET-1 gene in the endothelium (the main source and origin of the vasoconstrictor peptide1,14) on changes in vascular reactivity that accompany obesity is unclear.
The renal circulation is crucial for the regulation of systolic arterial blood pressure, which increases when the blood flow to the kidneys is reduced15,16. In obese mice17 as well as in type I18 and type II diabetic rodents19, the renal vasculature is hyperresponsive to exogenous vasoconstrictor prostanoids. However, the role of endogenous endothelin-1 and endogenous prostanoids in the ability of renal arteries to constrict or dilate in this context are unclear.
Therefore, the effect of endothelial overexpression of the prepro-ET-1 gene was determined on prostanoid-mediated contractions and endothelium-dependent relaxations of isolated renal arteries from lean and obese mice; the findings in these small renal arteries were compared to results obtained in the iliac artery [large peripheral conduit blood vessel; to the best of our knowledge not explored in terms of the impact of obesity on its responsiveness], the carotid artery [standard preparation to investigate endothelium-dependent contractions in the mouse13,20,21] and the aorta [standard preparation to investigate nitric oxide (NO)-mediated relaxations in the mouse3.
Materials and methods
Animal studies
After weaning at the age of four weeks and genotyping to detect the presence or absence of the transgene22, male mice with heterozygous overexpression of the murine prepro-endothelin-1 gene (TEThet) and their wild-type (WT) littermates on a C57BL/6N background17 were randomized to either standard chow (13% kcal from fat, D5053, Lab Diet, Purina Mills, Richmond, IN, USA) or a high-fat diet (41% kcal from fat, D12079B, Research Diets Inc, New Brunswick, NJ, USA) for 8–9 months. The animals were housed at constant temperature (22°C on average) under a 12-h light-dark cycle with ad libitum access to food and water. On the day of experiments, the mice that were fasted overnight were anesthetized with an intraperitoneal injection of fentanyl citrate (0.4 mg/kg) and fluanisone (12.5 mg/kg; Janssen Pharmaceutica, Beerse, Belgium) plus midazolam (6.25 mg/kg; Roche, Basel, Switzerland) and sacrificed by exsanguination via cardiac puncture after reassurance of adequate anesthesia by the absence of a reaction to tail pinching. Blood was collected into chilled EDTA tubes and centrifuged at 2000 r/min at 4 °C for 20 min, and 100 μL aliquots of plasma were stored at −80 °C. Vascular tissues (aorta, carotid, iliac, as well as main and segmental renal arteries) were harvested for isometric tension recording experiments17,20. All procedures were approved by the institutional Committee on the Use of Live Animals for Teaching and Research (CULATR, project 2574-11) of the University of Hong Kong in line with the National Institutes of Health's Guide for the Care and Use of Laboratory Animals issued by the US Institute of Laboratory Animal Research (ILAR, Eighth Edition, 2011).
Arterial blood pressure and heart rate
At the end of the study, arterial blood pressure and heart rate were measured non-invasively in conscious animals by using the tail-cuff method (Four channel BP-2000 Blood Pressure Analysis System, Visitech Systems Inc, Raleigh, NC, USA)23.
Body mass and fat content
Body and fat mass were determined in conscious lean and obese mice at the end of the study by time-domain nuclear magnetic resonance spectroscopy (Minispec model LF90II, Bruker Instruments, Billerica, MA, USA).
Plasma levels of metabolic parameters and endothelin-1
Fasting plasma glucose levels were measured at the time of sacrifice with a portable glucometer (Roche Diagnostics, Mannheim, Germany). Insulin was assayed with an in house high-sensitivity mouse insulin immunoassay kit (#32270; Antibody and Immunoassay Services AIS of the University of Hong Kong). Endothelin-1 levels were determined in plasma samples that were thawed on ice using the Quantikine ELISA kit (DET100; R&D Systems Inc, Minneapolis, MN, USA).
Vascular reactivity
Carotid arteries and the aorta with the renal and iliac arteries attached were excised and immediately placed into ice-cold modified Krebs-Ringer bicarbonate solution (pH 7.4) of the following composition (in mmol/L): NaCl, 129; KCl, 4.7; KH2PO4, 1.18; MgSO4, 1.17; NaHCO3, 14.9; glucose, 5.5; calcium disodium EDTA, 0.026; and CaCl2, 2.5 (control solution)20. The vessels were cut into rings (2–3 mm in length) under a dissection microscope after removal of the adherent adipose and connective tissues. Arterial rings were suspended between jaws of four channel Halpern-Mulvany myographs (models 610M and 620M; Danish Myo Technology A/S, Aarhus, Denmark) using either pins (aorta) or 40 μm stainless steel wire (carotid, iliac, and renal arteries) for the measurement of isometric tension [in mN (9.81 mN=1 g)]. The optimal resting tension was determined for each preparation by repeated exposure to 60 mmol/L high potassium (high K+) depolarizing solution as previously described20. These submaximal responses to high K+ were used as reference contractions. Due to the limited availability of renal arterial tissue in mice, some vasoconstrictors (ET-1, U46619) were examined in the main branches, while others (phenylephrine, serotonin) were explored in segmental renal arterial rings, taking advantage of the higher number per animal of the latter preparation compared to the main renal arteries. The relaxations to acetylcholine and insulin were also performed in the segmental renal arterial rings.
Prostanoid measurements
Aliquots (200 μL) of myograph chamber solution were collected after exposure of the carotid arterial rings to a final concentration (10−4 mol/L) of acetylcholine in the absence of presence of either BQ-123 or FR122047 (both 10−6 mol/L) in addition to L-NAME (3×10−4 mol/L). The aliquots were stored at −80 °C until determination of the concentrations of 6-keto prostaglandin F1α and thromboxane B2 (the stable metabolites of prostacyclin and thromboxane A2, respectively) in undiluted aliquots could be performed using commercially available ELISA kits (Cayman Chemical Company, Ann Arbor, MI, USA) according to the manufacturer's instructions20,24.
Drugs
Acetylcholine chloride, (cyclo(-D-Trp-D-Asp(ONa)-Pro-D-Val-Leu-)) (BQ-123), BQ-788, endothelin-1, (−)-isoproterenol hydrochloride, Nω-nitro-L-arginine methyl ester (L-NAME), meclofenamic acid sodium salt (meclofenamate), DL-norepinephrine hydrochloride, 1H-[1,2,4]oxadiazolo[4,3-a]quinoxalin-1-one (ODQ), R-(−)-phenylephrine hydrochloride, prazosin hydrochloride, DL-propranolol hydrochloride, and sodium nitroprusside dihydrate were purchased from Sigma-Aldrich (St Louis, MO, USA); phentolamine hydrochloride was obtained from Ciba (Basel, Switzerland); and 9,11-dideoxy-9α,11α-methanoepoxy prostaglandin F2α (U46619) was acquired from Enzo Life Sciences (Farmingdale, NY, USA). FR122047 hydrochloride was purchased from Tocris Bioscience (Bristol, UK). Bosentan was graciously provided by Actelion (Allschwil, Switzerland), and S18886 was a kind gift from the Institut de Recherche Servier (Suresnes, France). Insulin was used in the soluble form of Actrapid (Novo Nordisk A/S, Bagsværd, Denmark) as described25. All drugs were dissolved in distilled water except U46619 and insulin, which were prepared in ethanol (10−2 mol/L stock) and diluted in control solution (from 6×10−4 mol/L stock), respectively; and stock solutions (10−2 mol/L) of ODQ and S18886 were prepared in dimethyl sulfoxide (DMSO). Final concentrations did not exceed 0.1% for either DMSO or ethanol. Concentrations are stated as the final molar concentration in the myograph chamber solution.
Calculations and statistical analysis
The results are shown as the mean±standard error of the mean (SEM), whereby n equals the number of mice per group. Contractions are expressed as the percent of the reference contraction to high K+ (60 mmol/L potassium chloride with equimolar substitution of sodium by potassium) obtained at the beginning of the experiment, and relaxations as the percentage of pre-contractile response to either phenylephrine or U46619. Distribution normality was tested with the D'Agostino-Pearson test (GraphPad Software, San Diego, CA, USA). Concentrations causing half maximal responses (EC50) were calculated and compared using nonlinear regression and expressed as negative logarithms (pD2 values). The calculated maximal responses (Emax) are presented as percentages of the reference contraction. Either one-way ANOVA or the Kruskal-Wallis test followed by Bonferroni or Dunn's analysis, respectively, were used to analyze significant differences between unpaired groups as appropriate. Two-way ANOVA with repeated measurements were used for multiple comparisons of concentration-response curves followed by Bonferroni post hoc analysis where appropriate. Student's t-test was used for direct comparisons of samples showing a normal distribution, while the Mann-Whitney U test was applied for non-parametric samples. P values less than 0.05 were considered to indicate statistically significant differences.
Results
Physiological and plasma parameters
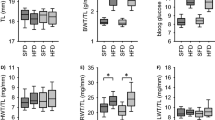
Mice consuming a high-fat diet for 8–9 months increased their body weight compared to controls; the relative fat mass doubled irrespective of the genotype. The plasma levels of ET-1 were comparable in lean and obese WT and TEThet mice. Fasting insulin and fasting glucose levels were higher in obese mice compared to lean animals, but all mice remained in the normoglycemic range. Similarly, the systolic arterial blood pressure values were within normal limits in all the groups. Heart rate increased with obesity, significantly more so when combined with TEThet overexpression. These parameters are summarized in Table 1.
Contractions to endothelin-1
Experiments with vasoconstrictor agents were performed in arteries incubated with L-NAME (3×10−4 mol/L, 30-min pre-incubation)17 to determine the potential of ET-126,27. In main renal arteries, the response to endothelin-1 (10−11 to 10−7 mol/L) was shifted to the left in rings from lean mice with endothelial overexpression of the prepro-endothelin-1 (ET-1) gene (TEThet) compared to corresponding preparations from their WT littermates (Figure 1). Obesity augmented the pD2 values of contractions to ET-1 in the renal arteries of WT but not TEThet mice (Figure 1). This was the only difference in the presence of the cyclooxygenase inhibitor meclofenamate (10−6 mol/L)20, which equilibrated the renal arterial responses to ET-1 among the other groups (Figure 1). Carotid arterial rings from the four experimental groups contracted similarly to increasing, cumulative concentrations of ET-1 without differences in the pD2 values for the responses to the vasoconstrictor peptide (WT lean 8.6±0.1, TEThet lean 8.7±0.1, WT obese 8.6±0.1, TEThet obese 8.8±0.2).
Contractions to endothelin-1 in isolated main renal arteries of lean wild-type (WT; A, n=6), lean heterozygous prepro-endothelin-1 gene overexpressing (TEThet; B, n=9), obese WT (C, n=5) and obese TEThet mice (D, n=5). All experiments were performed in the presence of L-NAME (3×10−4 mol/L) and either without or with meclofenamate (10−6 mol/L) as indicated. The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the mean±SEM. *P<0.05, **P<0.01 vs WT lean. $P<0.05 vs corresponding experiments in the absence of meclofenamate in each individual group.
In the iliac arterial rings, contractions to ET-1 were of a larger amplitude (Emax WT lean 168%±23%, TEThet lean 164%±11%, WT obese 171%±10%, and TEThet obese 102%±10% high K+) than in the carotid preparations (Emax WT lean 27%±2%, TEThet lean 22%±1%, WT obese 23%±1%, and TEThet obese 26%±3% high K+) and were comparable between preparations from both lean genotypes (Figure 2). However, responses to the highest concentrations were lower in the iliac arteries of obese TEThet compared to WT mice and lean controls (Figure 2D). Due to the overall high amplitude of the contractions to ET-1 in the iliac artery, this preparation was selected to compare the effects and efficacy of endothelin receptor antagonists across all of the groups. Therefore, concentration-response curves to ET-1 were obtained in iliac arteries in the presence of the endothelin-A (ETA) receptor antagonist BQ-12311, the endothelin-B (ETB) receptor antagonist BQ-78812 or the dual ETA/B receptor antagonist bosentan10 (all 10−6 mol/L) in addition to L-NAME. The endothelin-A (ETA) receptor blocker BQ-123 prevented contractions in all iliac preparations (Figure 2A-2D), while the ETB-selective antagonist BQ-788 shifted the ET-1 concentration-response curve to the right only in the arterial preparations from obese animals (Figure 2C and 2D). The dual ETA/B receptor antagonist bosentan was equally effective as BQ-123 in preventing contractions in response to ET-1 (Figure 2A to 2D). Therefore, the ETA receptor-selective antagonist was chosen for further experiments examining ET-1-modulated vasoconstrictor responses.
Contractions to endothelin-1 (ET-1) in iliac arterial rings from lean (A and B) and obese (C and D) wild-type (WT) mice and mice with heterozygous endothelial overexpression of the prepro-ET-1 gene (TEThet). All the experiments were performed in the presence of L- NAME (3×10−4 mol/L) and BQ-123, BQ-788, or bosentan (all 10−6 mol/L). The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets where calculation possible) are given as the mean±SEM; n=6–9. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
Thromboxane prostanoid receptor activation
Contractions of main renal arteries to the full thromboxane prostanoid (TP) receptor agonist U46619 (10−11 to 3×10−6 mol/L) were augmented by obesity (Figure 3), confirming earlier findings17. The cyclooxygenase inhibitor meclofenamate reduced the response to U46619 in all the groups (Figure 3), but foremost in preparations from obese TEThet mice in which responses were shifted to the right even compared to WT littermates fed a high-fat diet (Figure 3). Contractions to the TP receptor agonist in the obese WT group remained augmented during cyclooxygenase inhibition, while they were not different in obese TEThet mice compared to their lean controls in the presence of meclofenamate (Figure 3). By contrast to renal arteries, the leftward shift of TP receptor agonist-induced responses in the carotid arteries of obese mice in the presence of L-NAME only [pD2: WT and TEThet obese 7.9±0.1 compared to lean controls (WT lean 7.5±0.1 and TEThet lean 7.8±0.1; n=4–7, P<0.01)], remained during additional cyclooxygenase inhibition with meclofenamate (pD2 WT and TEThet lean 7.4±0.1, WT obese 7.6±0.1, and TEThet obese 7.5±0.1; n=7–12, P<0.05) irrespective of the genotype.
Contractions to the full TP receptor agonist U46619 in main renal arterial rings from lean wild-type (WT; A, n=5) and heterozygous prepro-endothelin-1 gene overexpressing (TEThet; B, n=6), and obese WT (C, n=9) and TEThet mice (D, n=6). All experiments were performed in the presence of L-NAME (3×10−4 mol/L) and without or with meclofenamate (10−6 mol/L) as indicated. The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls; $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
Serotonin
Segmental renal arterial contractions to serotonin (10−10 to 3×10−5 mol/L) in the presence of L-NAME only were shifted to the right by TEThet overexpression in lean mice. Obesity shifted the response to the left in TEThet but not WT mice. These differences were absent in the additional presence of meclofenamate (Figure 4).
Contractions to serotonin in segmental renal arterial rings from lean wild-type (WT; A, n=6), lean heterozygous prepro-endothelin-1 gene overexpressing (TEThet; B, n=9), obese WT (C, n=7) and obese TEThet mice (D, n=4–5). All the experiments were performed in the presence of L-NAME (3×10−4 mol/L) and without or with meclofenamate (10−6 mol/L) as indicated. The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the mean±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
Phenylephrine
In the presence of L-NAME only, contractions to phenylephrine (10−10 to 10−4 mol/L) in segmental renal arterial rings were not different between lean TEThet and WT mice, while they were shifted to the left in obese TEThet compared to WT mice (Figure 5). Addition of the cyclooxygenase inhibitor meclofenamate shifted the vasoconstrictor response to α1-adrenoceptor activation to the right in corresponding preparations from all animals except in those of lean WT mice. Meclofenamate lowered the sensitivity to phenylephrine in the rings from obese versus lean animals irrespective of the genotype (Figure 5).
Contractions to the α1-adrenoceptor agonist phenylephrine in segmental renal arterial rings from lean wild-type (WT; A, n=6), lean heterozygous prepro-endothelin-1 gene overexpressing (TEThet; B, n=9), obese WT (C, n=7) and obese TEThet mice (D, n=4–5). All the experiments were performed in the presence of L-NAME (3×10−4 mol/L) and without or with meclofenamate (10−6 mol/L) as indicated. The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
Relaxation responses to acetylcholine
Relaxations [during pre-contraction with phenylephrine (3×10−8 to 2×10−6 mol/L to obtain approximately 50% of high K+ reference contractions) and in the presence of meclofenamate] of segmental renal arteries were examined in the absence or presence of the nitric oxide synthase inhibitor L-NAME (3×10−4 mol/L). In the presence of meclofenamate only, preparations from lean TEThet mice were more sensitive to the endothelium-dependent muscarinic agonist compared to corresponding rings from WT littermates. This difference was less pronounced in the renal arteries of obese animals since WT preparations exhibited an improved response in obesity (Figure 6). Irrespective of the body weight, L-NAME attenuated the relaxations to acetylcholine (10−10 to 10−4 mol/L) only in rings from WT but not in those from TEThet mice, where these relaxations were largely preserved (Figure 6). By contrast, maximal nitric oxide-dependent relaxations to acetylcholine in the aorta (phenylephrine-contracted to 64% to 77% of high K+) were similar across the groups in the presence (Figure 7A) or absence of meclofenamate (Figure 7B). Likewise, in aortic rings precontracted (74% to 108% of high K+) with U46619, relaxations to norepinephrine [10−10 to 10−4 mol/L; in the presence of prazosin and propranolol (both 10−6 mol/L) in addition to meclofenamate to prevent activation of α1- and β-adrenoceptors, respectively; Figure 7C] did not differ between the groups; relaxations to norepinephrine under these experimental conditions are comparable to the release of nitric oxide upon activation of endothelial α2-adrenoceptors28.
Relaxations to the endothelium-dependent agonist acetylcholine in segmental renal arterial rings from lean wild-type (WT; A, n=5), lean heterozygous prepro-endothelin-1 gene overexpressing (TEThet; B, n=5) mice, and obese WT (C, n=9) and TEThet mice (D, n=5–6). All experiments were performed in the presence of meclofenamate (10−6 mol/L) and without or with L-NAME (3×10−4 mol/L) as indicated. The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of meclofenamate only in each individual group.
Nitric oxide-mediated relaxations to the endothelium-dependent agonists acetylcholine (A and B) and norepinephrine (C) in aortic rings from lean and obese wild-type (WT) and TEThet mice in the presence of meclofenamate (Meclo), prazosin and propranolol (all 10−6 mol/L) or in the absence/presence of meclofenamate alone as indicated; n=5–10. The data are expressed as changes in tension relative to the pre-contractions to phenylephrine (PE) or U46619 (U46), and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of meclofenamate only in each individual group.
At higher concentrations (10−6 to 10−4 mol/L) of acetylcholine, a secondary increase in tension was observed in the absence but not in the presence of meclofenamate (Figure 7), indicative of the occurrence of endothelium-dependent contractions13,29. These secondary contractions were larger in the aortic rings from obese TEThet mice (Figure 7B).
Relaxations to sodium nitroprusside, isoproterenol, and insulin
Endothelium-independent relaxations to sodium nitroprusside (10−11 to 10−6 mol/L, in the presence of L-NAME) and the β-adrenergic agonist isoproterenol [10−10 to 3×10−6 mol/L, in the presence of meclofenamate, oxadiazolo[4,3-a]quinoxalin-1-one (ODQ, 10−5 mol/L; inhibitor of soluble guanylyl cyclase) were obtained in aortic preparations contracted to a similar degree across the groups with phenylephrine (84% to 92% of the response to high K+); the same procedure was performed with phentolamine (10−5 mol/L; a non-selective α-adrenoceptor antagonist)] and U46619 (80% to 98% of high K+), respectively. Relaxations to sodium nitroprusside in the aorta were not different between the groups (Figure 8A), demonstrating an absence of an impact of the genotype on the sensitivity of vascular smooth muscle to nitric oxide. Paralleling the observed in vivo changes in heart rate, the aortic relaxations to the β-adrenoceptor agonist isoproterenol were facilitated by obesity in WT mice, especially in those of the TEThet genotype (Figure 8B).
Relaxations to the nitric oxide donor sodium nitroprusside (A) and the β-adrenoceptor agonist isoproterenol (B) in aortic rings from lean and obese wild-type (WT) and TEThet mice in the presence of L-NAME (3×10−4 mol/L) or meclofenamate (Meclo, 10−6 mol/L), ODQ, and phentolamine (both 10−5 mol/L), respectively, as indicated; n=6–10. The data are expressed as changes in tension relative to pre-contractions to phenylephrine (PE) or U46619 (U46), and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
Insulin in phenylephrine-contracted (10−7 to 9×10−7 mol/L to obtain approximately 50% of high K+ reference contractions) segmental renal arterial rings (all in the presence of meclofenamate) caused concentration-dependent decreases in tension that were comparable in all the groups irrespective of the absence or presence of L-NAME (Figure 9).
Relaxations to insulin in segmental renal arterial rings from lean wild-type (WT; n=5), lean heterozygous prepro-endothelin-1 gene overexpressing (TEThet; n=5), obese WT (n=9) and obese TEThet mice (n=6). All the experiments were performed in the presence of meclofenamate (10−6 mol/L) and without (A) or with L-NAME (B; 3×10−4 mol/L) as indicated. The data are expressed as changes in tension relative to pre-contractions to phenylephrine, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the means±SEM. *P<0.05 vs WT lean.
Prostanoid-mediated contractions to acetylcholine
Quiescent rings from carotid arteries were exposed to increasing concentrations of acetylcholine in the presence of L-NAME. The contractions were comparable in preparations from lean WT and TEThet mice (Figure 10A). Obesity increased the contractions in preparations from both genotypes but more so in rings from obese TEThet mice (Figure 10B). In the four groups, the contractions to acetylcholine were abolished by either the selective COX-1 inhibitor FR122047 (10−6 mol/L) or by the TP receptor antagonist S18886 (10−7 mol/L; Emax 0±0% high K+), which confirmed earlier findings in the rat aorta30,31.
Contractions to acetylcholine in carotid arterial rings (with endothelium) from lean (A) and obese (B) wild-type (WT) and TEThet mice. All the experiments were in the presence of L-NAME (3×10−4 mol/L; n=14–18) as well as the endothelin-A receptor antagonist BQ-123 (10−6 mol/L; n=7–13). The data are expressed as the percentage of reference contractions to a 60 mmol/L high potassium solution, and the negative logarithms of the calculated concentrations that cause a half maximal responses (pD2 values in brackets for each group) are given as the mean±SEM. The release of the stable prostacyclin breakdown product 6-keto prostaglandin F1α (C; 6-keto PGF1α) from carotid arterial rings from lean and obese WT and TEThet mice from these experiments in the presence of either L-NAME only (3×10−4 mol/L; white bars) or with BQ-123 (10−6 mol/L; black bars) is shown. The data are expressed in percentage of WT controls and are shown as the mean±SEM. **P<0.01 vs WT obese. #P<0.05 vs lean controls. $$P<0.01 vs experiments in the presence of L-NAME only in each individual group.
The acetylcholine-stimulated release of 6-keto prostaglandin F1α (6-keto PGF1α) was increased in carotid rings from obese TEThet mice under control conditions, and BQ-123 especially reduced the relative release of 6-keto PGF1α in these preparations (Figure 10C), with the levels becoming comparable across the groups (Table 2). However, the addition of the ETA receptor-selective antagonist did not significantly alter the contractions to acetylcholine across the groups (Figure 10). Only very low levels of the prostanoid were detected after incubation with FR122047. The levels of thromboxane B2 (TXB2) released by the carotid arteries were similarly low in all the groups with values around the detection limit of the assay (Table 2).
Discussion
The present results demonstrate the following:
a) Tie-1 promoter-driven heterozygous overexpression of the prepro-ET-1 gene (TEThet)17,22,32 has marginal effects on vascular reactivity under lean conditions, such as slightly increased responses to ET-1 itself, a decreased sensitivity to serotonin and preserved relaxations to acetylcholine during nitric oxide synthase inhibition in renal arteries.
b) High-fat diet consumption leading to an augmented body weight and an increase in plasma insulin levels was associated with a higher contractility to ET-1 in renal arteries from WT mice in addition to elevated thromboxane prostanoid (TP) receptor responsiveness. Contractions to ET-1 in iliac arteries were partially endothelin-B receptor-dependent, and aortic relaxations to acetylcholine, norepinephrine, and sodium nitroprusside were preserved in preparations from obese animals. Furthermore, obesity increased the heart rate, which was paralleled by facilitated relaxations to the β-adrenoceptor agonist isoproterenol in aortic rings.
c) These findings were aggravated in obese TEThet mice, in which augmented renal arterial contractions were consistently curtailed in the presence of the cyclooxygenase inhibitor meclofenamate. Isolated prostanoid-mediated contractions to acetylcholine examined in carotid arteries revealed a higher production/release of the endothelium-derived contracting factor (EDCF) prostacyclin in preparations from TEThet mice with diet-induced obesity.
The high-fat diet imposed in the present study increased the body mass due to excess adipose tissue. Since the animals remained normoglycemic and normotensive, their obesity can be regarded as an independent cardiovascular risk factor33 rather than a feature of the metabolic syndrome34.
In line with earlier studies35, obesity increased the heart rate, especially in TEThet mice. This is in accordance with the regulatory role of ET-1 on cardiac sympathetic innervation36. The plasma ET-1 levels determined in the present study are similar to those reported for lean C57BL/6 WT control mice14,37,38. In such animals, 3 weeks of high-fat diet elevates ET-1 in the circulation37, but the present experiments show that this effect is lost after 30 weeks of diet-induced obesity. This observation is in line with the absence of plasma ET-1 elevation following 10 weeks of high-fat feeding39. By contrast to the homozygous TET-1 mice32, the heterozygous TEThet mice used in the present study (which were generated by several backcrosses of TET-1 mice onto a C57BL/6N background) had no increase in plasma ET-1 in response to either diet.
Endothelin-A (ETA) receptor blockade by BQ-123 was equally effective in iliac preparations from all the groups in preventing contractions to ET-1, confirming the general dependency on this receptor subtype in the vasoconstrictor response to this peptide40. However, a functional relevance of ETB receptors in vascular smooth muscle was revealed in iliac arteries from obese mice, where the ETB receptor-selective antagonist BQ-788 attenuated contractions to ET-1 in line with previous studies in hypercholesterolemic animals41,42. Similar to arteries of transgenic mice with endothelium-selective32,38,43 or global overexpression of the prepro-ET-1 gene44, maximal contractions to ET-1 were attenuated in iliac rings from obese TEThet mice. Unlike in systemic conduit vessels such as carotid and iliac arteries, contractions to ET-1 were augmented in renal arteries from obese animals. This highlights the potential of the vasoconstrictor peptide to contribute to an increased vascular risk in the renal circulation. The aggravation by obesity was partially cyclooxygenase-dependent, suggesting the contribution of endogenously released vasoconstrictor prostanoids as demonstrated in the response to ET-1 in the aortae of spontaneously hypertensive rats6. Cyclooxygenase inhibition also attenuated contractions to the peptide in renal arteries from lean mice, but its effect was marginal in obese TEThet mice. This permits the conclusion that moderate endothelial overexpression of the prepro-ET-1 gene does not potentiate the cyclooxygenase-dependent aspect of the response to exogenously added peptide in mouse renal arteries. Moreover, the lack of augmentation of contractions to ET-1 in renal arteries from obese TEThet mice can be seen in the context of desensitization to the peptide itself as observed in the iliac arteries of these animals and as indicated in other models of ET-1 overexpression32,38,43,44.
The attenuation of contractions to direct TP receptor activation by U46619 during cyclooxygenase inhibition by meclofenamate across the groups is indicative of the contribution of endogenous prostanoids to these vasoconstrictor responses. Thereby, activation of endothelial TP receptors can lead to the release of endogenous prostanoids45,46. The latter appears to be of the utmost importance with regard to obesity augmented contractions to the TP receptor agonist17 in TEThet mice, where the difference in responses between the renal arteries from lean and obese mice was abolished by meclofenamate. By contrast, in WT animals, contractions to U46619 remained amplified by obesity during cyclooxygenase inhibition. Therefore, this may then be seen as an increased TP receptor responsiveness of vascular smooth muscle cells, assuming that the contribution of endogenous prostanoids can be excluded in the presence of meclofenamate. In line with this interpretation, in conduit arteries such as the carotid arteries of obese mice in the presence of meclofenamate, the potencies of the TP receptor agonist were increased compared to preparations from lean control animals irrespective of the genotype. These observations highlight the relevance of endogenous prostanoids in augmented contractions upon TP receptor activation in the renal arteries with regard to an up-regulated ET-1 system in obesity. The same was true regarding the augmented segmental renal arterial contractions to serotonin that were described in obese TEThet mice17 with attenuated responses in preparations from obese animals to the same levels as in lean controls during cyclooxygenase inhibition. These findings indicate that serotonin releases vasoconstrictor prostanoids from the renal arteries of obese TEThet mice with endothelial prepro-ET-1 gene overexpression, which was similar to that demonstrated in the kidney vasculature of spontaneously hypertensive rats47. Given the confirmed high reactivity of renal arteries to serotonin [possibly involving decreased desensitization48 and taking into consideration the possible potentiating effects of local ET-1 peptide on such vasoconstrictor agents49, the monoamine may contribute to arterial blood pressure regulation50,51 in obesity. Moreover, the potentiation of phenylephrine-induced contractions in segmental renal arterial rings from obese TEThet mice compared to WT mice was fully sensitive to cyclooxygenase inhibition. Therefore, meclofenamate decreased the responses to the α1-adrenoceptor agonist, particularly in preparations from obese animals. This indicates that adrenergic stimulation may also lead to the release of prostanoids under pathophysiological conditions such as obesity. Prostanoid release by phenylephrine is not as well documented as for serotonin47,52 and ET-15,6,9,26, but experiments in aortic rings from diabetic rats have suggested a possible involvement of vasoconstrictor prostanoids in contractions to the α1-adrenceptor agonist53. The apparent potentiation of the response to phenylephrine in preparations from obese TEThet mice can be attributed to endogenous ET-1 aggravating adrenergic contractions (similar to serotonin responses) as shown with norepinephrine in human arteries49.
With all of the increases in the vasoconstrictor agonist-induced renal arterial responses, it is tempting to hypothesize why obese mice, particularly those of the TEThet genotype, did not present hypertensive levels in their systolic arterial blood pressures considering the pivotal role of kidneys in regulating blood pressure54. Moreover, an increased vasomotor tone in renal arteries caused by continuous vasoconstrictor signaling in vivo would functionally have a similar effect as that described for renal artery stenosis15,16. A possible explanation for the absence of hypertension in vivo can be seen in the largely preserved renal arterial relaxations to insulin. This hormone relaxes canine carotid arteries irrespective of the presence or absence of endothelial cells55, while responses in rat mesenteric arteries and aortae appear to be largely endothelial NOS-dependent56. In the present study, the contribution of vasodilator prostaglandins, as suggested by hemodynamic investigations in the perfused rat kidney57, are unlikely to be involved in the relaxations to insulin based on the results obtained during cyclooxygenase inhibition. The observations in murine segmental renal arterial rings are in line with findings in rat renal arteries in which insulin caused comparable relaxations in preparations from diabetic and non-diabetic animals with the response being largely NO-independent in the latter58. In addition, insulin given to diabetic animals in vivo subsequently facilitates NO-mediated relaxations of small resistance arteries ex vivo59. In obese mice with higher circulating levels of insulin, this could counteract the augmented vasoconstrictor responses in the kidney vasculature in vivo.
ET-1 not only promotes the release and action of vasoconstrictor prostanoids6,9 but also that of NO in isolated arteries, including those from spontaneously hypertensive rats60, and can induce endothelium-dependent hyperpolarization (EDH)-mediated relaxation in isolated mesenteric arteries61. This alternative mechanism of relaxation may indeed be involved in the renal vasculature as demonstrated in human interlobar arteries62. In the present study, endothelium-dependent relaxations to acetylcholine in segmental renal arteries from animals in all the groups were similar in the absence and presence of L-NAME, indicating preserved NO- and EDH-mediated responses in these preparations, respectively. Since nitric oxide synthase inhibition attenuated the relaxations in preparations from WT rather than TEThet mice, facilitated hyperpolarization by ET-161 cannot be excluded for these renal arterial preparations. Preserved nitric oxide-mediated relaxations in the aortae of obese TEThet mice are in line with the findings in endothelial ET-1 overexpressing ApoE-deficient mice fed a high-fat diet63.
The present study confirms that diet-induced obesity enhances endothelium-dependent contractions to acetylcholine13. The predominance of prostacyclin production compared to the marginal levels of thromboxane A2 illustrates its primary role as an endothelium-derived contracting factor in rodent blood vessels5,6,9,20,24,30,64. Since ETA receptor blockade with BQ-123 reduced prostacyclin release in all the groups, particularly in carotid arterial rings from obese TEThet mice, the present study confirms that ET-1 promotes the release of endothelium-derived vasoconstrictor prostanoids5,6,9,26,65, which is compatible with endothelium-selective overexpression in the TEThet model. This augmented prostacyclin production may partially explain the potentiated prostanoid-mediated contractions in obese TEThet mice, in which the effect of BQ-123 in reducing prostanoid production was the largest. However, the contractions to the muscarinic agonist were unaltered in the presence of BQ-123, indicating that the responsiveness to prostanoids remains augmented in obesity irrespective of the amounts released. Furthermore, prostaglandin E2 may contribute to vasoconstrictor responses and can be augmented by ET-165. In the renal circulation of larger rodents, prostaglandin E2 indeed has vasoconstrictor activity66. The present study does not allow for the definitive identification of the prostanoid that is mainly responsible for the increased vasoconstrictor tone in renal arteries, particularly in response to U46619, where the most pronounced shifts by cyclooxygenase inhibition were observed. In the human renal circulation, high concentrations of both prostacyclin and prostaglandin E2 have vasoconstrictor activity due to activation of TP receptors67.
Collectively, the present findings underscore a novel and direct role for endothelial ET-1 in regulating cyclooxygenase-dependent vasoconstrictor prostanoid formation associated with obesity, especially in the renal circulation. The finding that augmented prostanoid-mediated contractions due to ET-1 require a pathological condition such as obesity is in accordance with studies demonstrating that ET-1 could induce the release of endothelium-derived prostanoids in the arteries from spontaneously hypertensive rats but not in those from normotensive rats6. Similarly, ET-1 stimulates prostanoid release from regenerated but not native porcine coronary endothelium5. Thus, the current findings lend further support to the concept that the endothelin system plays a minor role in regulating vascular function under physiological conditions but becomes more important during pathophysiological processes and/or vascular cell injury9,68,69.
In conclusion, the present study demonstrates that endothelial overexpression of the prepro-ET-1 gene potentiates prostanoid-mediated, endothelium- and TP receptor-dependent vasoconstriction in obesity. This can be largely attributed to an augmented release of prostanoids, specifically prostacyclin, which has repeatedly been identified as a major endothelium-derived contracting factor in rodents20,24,30,64. By contrast, contractions to the vasoconstrictor peptide itself can be attenuated in ET-1 overexpressing mice, and endothelium-dependent relaxations to acetylcholine may be preserved if not even improved with obesity. This could explain the lack of an exacerbation of the cardiovascular phenotype in obese TEThet mice.
As the release of the prostanoid prostacyclin was reduced by ETA receptor blockade, and since therapeutic approaches of cyclooxygenase inhibition are associated with an increased cardiovascular risk, alternative strategies are necessary. Because ETA receptor blockade also possibly curtails prostanoid formation in obese or overweight humans, the tandem of ET-1 and prostanoid-mediated vasoconstriction appears relevant to the understanding of vascular dysfunction in obese patients and thus may help to delineate new strategies for the therapy and/or prevention of cardiovascular disorders associated with obesity. Because the increased vasoconstrictor responses were observed in renal arteries from obese normotensive animals, renal arterial dysfunction could be a crucial step in the initiation of blood pressure elevation that may occur once counter regulatory mechanisms decline in function during disease progression. Cyclooxygenases consistently appeared to be involved in this hyperresponsiveness, particularly in preparations from obese TEThet mice. This suggests that renal arteries of obese TEThet mice may have a higher propensity to release endogenous prostanoids upon stimulation by other vasoconstrictors. Therefore, although ET-1 does not directly contribute to hypertension, it could potentially function as a modulator in promoting prostanoid production and augmenting the reactivity of vascular smooth muscle, all of which could become critical in causing blood pressure elevation, especially if this phenomenon occurs within the renal vasculature.
Author contribution
All authors designed this study by helping to develop the experimental design. Oliver BARETELLA performed all of the experiments, analyzed the data and wrote the manuscript. Sookja K CHUNG contributed transgenic animals. Aimin XU and Paul M VANHOUTTE edited the manuscript. And all the authors reviewed and approved the manuscript.
References
Yanagisawa M, Kurihara H, Kimura S, Tomobe Y, Kobayashi M, Mitsui Y, et al. A novel potent vasoconstrictor peptide produced by vascular endothelial cells. Nature 1988; 332: 411–5.
Kurihara Y, Kurihara H, Suzuki H, Kodama T, Maemura K, Nagai R, et al. Elevated blood pressure and craniofacial abnormalities in mice deficient in endothelin-1. Nature 1994; 368: 703–10.
Barton M, Haudenschild CC, d'Uscio LV, Shaw S, Münter K, Lüscher TF . Endothelin ETA receptor blockade restores NO-mediated endothelial function and inhibits atherosclerosis in apolipoprotein E-deficient mice. Proc Natl Acad Sci U S A 1998; 95: 14367–72.
Cardillo C, Campia U, Iantorno M, Panza JA . Enhanced vascular activity of endogenous endothelin-1 in obese hypertensive patients. Hypertension 2004; 43: 36–40.
Park SJ, Lee JJ, Vanhoutte PM . Endothelin-1 releases endothelium-derived endoperoxides and thromboxane A2 in porcine coronary arteries with regenerated endothelium. Acta Pharmacol Sin 1999; 20: 872–8.
Taddei S, Vanhoutte PM . Role of endothelium in endothelin-evoked contractions in the rat aorta. Hypertension 1993; 21: 9–15.
Weil BR, Westby CM, Van Guilder GP, Greiner JJ, Stauffer BL, DeSouza CA . Enhanced endothelin-1 system activity with overweight and obesity. Am J Physiol Heart Circ Physiol 2011; 301: H689–95.
Mather KJ, Mirzamohammadi B, Lteif A, Steinberg HO, Baron AD . Endothelin contributes to basal vascular tone and endothelial dysfunction in human obesity and type 2 diabetes. Diabetes 2002; 51: 3517–23.
Baretella O, Vanhoutte PM . Endothelium-Dependent Contractions: Prostacyclin and Endothelin-1, Partners in Crime? Adv Pharmacol 2016; 77: 177–208.
Clozel M, Breu V, Gray GA, Kalina B, Löffler BM, Burri K, et al. Pharmacological characterization of bosentan, a new potent orally active nonpeptide endothelin receptor antagonist. J Pharmacol Exp Ther 1994; 270: 228–35.
Ihara M, Noguchi K, Saeki T, Fukuroda T, Tsuchida S, Kimura S, et al. Biological profiles of highly potent novel endothelin antagonists selective for the ETA receptor. Life Sci 1992; 50: 247–55.
Ishikawa K, Ihara M, Noguchi K, Mase T, Mino N, Saeki T, et al. Biochemical and pharmacological profile of a potent and selective endothelin B-receptor antagonist, BQ-788. Proc Natl Acad Sci U S A 1994; 91: 4892–6.
Traupe T, Lang M, Goettsch W, Münter K, Morawietz H, Vetter W, et al. Obesity increases prostanoid-mediated vasoconstriction and vascular thromboxane receptor gene expression. J Hypertens 2002; 20: 2239–45.
Kisanuki YY, Emoto N, Ohuchi T, Widyantoro B, Yagi K, Nakayama K, et al. Low blood pressure in endothelial cell-specific endothelin 1 knockout mice. Hypertension 2010; 56: 121–8.
Goldblatt H, Lynch J, Hanzal RF, Summerville WW . Studies on Experimental Hypertension : I. The Production of Persistent Elevation of Systolic Blood Pressure by Means of Renal Ischemia. J Exp Med 1934; 59: 347–79.
Ponnuchamy B, Khalil RA . Cellular mediators of renal vascular dysfunction in hypertension. Am J Physiol Regul Integr Comp Physiol 2009; 296: R1001–18.
Baretella O, Chung SK, Barton M, Xu A, Vanhoutte PM . Obesity and heterozygous endothelial overexpression of prepro-endothelin-1 modulate responsiveness of mouse main and segmental renal arteries to vasoconstrictor agents. Life Sci 2014; 118: 206–12.
Michel F, Simonet S, Vayssettes-Courchay C, Bertin F, Sansilvestri-Morel P, Bernhardt F, et al. Altered TP receptor function in isolated, perfused kidneys of nondiabetic and diabetic ApoE-deficient mice. Am J Physiol Renal Physiol 2008; 294: F120–9.
Matsumoto T, Watanabe S, Kawamura R, Taguchi K, Kobayashi T . Enhanced uridine adenosine tetraphosphate-induced contraction in renal artery from type 2 diabetic Goto-Kakizaki rats due to activated cyclooxygenase/thromboxane receptor axis. Pflugers Arch 2014; 466: 331–42.
Baretella O, Xu A, Vanhoutte PM . Acidosis prevents and alkalosis augments endothelium-dependent contractions in mouse arteries. Pflugers Arch 2014; 466: 295–305.
Zhou Y, Varadharaj S, Zhao X, Parinandi N, Flavahan NA, Zweier JL . Acetylcholine causes endothelium-dependent contraction of mouse arteries. Am J Physiol Heart Circ Physiol 2005; 289: H1027–32.
Leung JW, Ho MC, Lo AC, Chung SS, Chung SK . Endothelial cell-specific over-expression of endothelin-1 leads to more severe cerebral damage following transient middle cerebral artery occlusion. J Cardiovasc Pharmacol 2004; 44 Suppl 1: S293–300.
Krege JH, Hodgin JB, Hagaman JR, Smithies O . A noninvasive computerized tail-cuff system for measuring blood pressure in mice. Hypertension 1995; 25: 1111–5.
Gluais P, Lonchampt M, Morrow JD, Vanhoutte PM, Félétou M . Acetylcholine-induced endothelium-dependent contractions in the SHR aorta: the Janus face of prostacyclin. Br J Pharmacol 2005; 146: 834–45.
Wang Y, Cheng KK, Lam KS, Wu D, Wang Y, Huang Y, et al. APPL1 counteracts obesity-induced vascular insulin resistance and endothelial dysfunction by modulating the endothelial production of nitric oxide and endothelin-1 in mice. Diabetes 2011; 60: 3044–54.
de Nucci G, Thomas R, D'Orléans-Juste P, Antunes E, Walder C, Warner TD, et al. Pressor effects of circulating endothelin are limited by its removal in the pulmonary circulation and by the release of prostacyclin and endothelium-derived relaxing factor. Proc Natl Acad Sci U S A 1988; 85: 9797–800.
Boulanger C, Lüscher TF . Release of endothelin from the porcine aorta. Inhibition by endothelium-derived nitric oxide. J Clin Invest 1990; 85: 587–90.
Miller VM, Vanhoutte PM . Endothelial α2-adrenoceptors in canine pulmonary and systemic blood vessels. Eur J Pharmacol 1985; 118: 123–9.
Lüscher TF, Vanhoutte PM . Endothelium-dependent contractions to acetylcholine in the aorta of the spontaneously hypertensive rat. Hypertension 1986; 8: 344–8.
Auch-Schwelk W, Katušić ZS, Vanhoutte PM . Thromboxane A2 receptor antagonists inhibit endothelium-dependent contractions. Hypertension 1990; 15: 699–703.
Tang EH, Ku DD, Tipoe GL, Félétou M, Man RY, Vanhoutte PM . Endothelium-dependent contractions occur in the aorta of wild-type and COX2–/– knockout but not COX1–/– knockout mice. J Cardiovasc Pharmacol 2005; 46: 761–5.
Leung JW, Wong WT, Koon HW, Mo FM, Tam S, Huang Y, et al. Transgenic mice over-expressing ET-1 in the endothelial cells develop systemic hypertension with altered vascular reactivity. PloS One 2011; 6: e26994.
Hubert HB, Feinleib M, McNamara PM, Castelli WP . Obesity as an independent risk factor for cardiovascular disease: a 26-year follow-up of participants in the Framingham Heart Study. Circulation 1983; 67: 968–77.
Alberti KG, Zimmet P, Shaw J, Group IDFETFC . The metabolic syndrome — a new worldwide definition. Lancet 2005; 366: 1059–62.
Belin de Chantemèle EJ, Mintz JD, Rainey WE, Stepp DW . Impact of leptin-mediated sympatho-activation on cardiovascular function in obese mice. Hypertension 2011; 58: 271–9.
Ieda M, Fukuda K, Hisaka Y, Kimura K, Kawaguchi H, Fujita J, et al. Endothelin-1 regulates cardiac sympathetic innervation in the rodent heart by controlling nerve growth factor expression. J Clin Invest 2004; 113: 876–84.
Adiarto S, Emoto N, Iwasa N, Yokoyama M . Obesity-induced upregulation of myocardial endothelin-1 expression is mediated by leptin. Biochem Biophys Res Commun 2007; 353: 623–7.
Amiri F, Virdis A, Neves MF, Iglarz M, Seidah NG, Touyz RM, et al. Endothelium-restricted overexpression of human endothelin-1 causes vascular remodeling and endothelial dysfunction. Circulation 2004; 110: 2233–40.
Catar RA, Muller G, Brandt A, Langbein H, Brunssen C, Goettsch C, et al. Increased gene expression of the cardiac endothelin system in obese mice. Horm Metab Res 2015; 47: 509–15.
Zhou Y, Dirksen WP, Zweier JL, Periasamy M . Endothelin-1-induced responses in isolated mouse vessels: the expression and function of receptor types. Am J Physiol Heart Circ Physiol 2004; 287: H573–8.
Hasdai D, Mathew V, Schwartz RS, Smith LA, Holmes DR. Jr, Katušić ZS, et al. Enhanced endothelin-B-receptor-mediated vasoconstriction of small porcine coronary arteries in diet-induced hypercholesterolemia. Arterioscler Thromb Vasc Biol 1997; 17: 2737–43.
Xu CB, Zheng JP, Zhang W, Liu E, Edvinsson L, Zhang Y . Low density lipoprotein induces upregulation of vasoconstrictive endothelin type B receptor expression. Vascul Pharmacol 2014; 60: 42–8.
Javeshghani D, Barhoumi T, Idris-Khodja N, Paradis P, Schiffrin EL . Reduced macrophage-dependent inflammation improves endothelin-1-induced vascular injury. Hypertension 2013; 62: 112–7.
Quaschning T, Voss F, Relle K, Kalk P, Vignon-Zellweger N, Pfab T, et al. Lack of endothelial nitric oxide synthase promotes endothelin-induced hypertension: lessons from endothelin-1 transgenic/endothelial nitric oxide synthase knockout mice. J Am Soc Nephrol 2007; 18: 730–40.
Hanasaki K, Nakano K, Kasai H, Kurihara H, Arita H . Identification of thromboxane A2 receptor in cultured vascular endothelial cells of rat aorta. Biochem Biophys Res Commun 1988; 151: 1352–7.
Sung CP, Arleth AJ, Berkowitz BA . Endothelial thromboxane receptors: biochemical characterization and functional implications. Biochem Biophys Res Commun 1989; 158: 326–33.
Tuncer M, Vanhoutte PM . Role of prostanoids in the increased vascular responsiveness and delayed tachyphylaxis to serotonin in the kidney of spontaneously hypertensive rats. J Hypertens 1991; 9: 623–9.
Collis MG, Vanhoutte PM . Vascular reactivity of isolated perfused kidneys from male and female spontaneously hypertensive rats. Circ Res 1977; 41: 759–67.
Yang ZH, Richard V, von Segesser L, Bauer E, Stulz P, Turina M, et al. Threshold concentrations of endothelin-1 potentiate contractions to norepinephrine and serotonin in human arteries. A new mechanism of vasospasm? Circulation 1990; 82: 188–95.
Vanhoutte PM, ed. Serotonin and the cardiovascular system. New York: Raven Press; 1985. p 1–288.
Watts SW, Morrison SF, Davis RP, Barman SM . Serotonin and blood pressure regulation. Pharmacol Rev 2012; 64: 359–88.
Lüscher TF, Vanhoutte PM . Endothelium-dependent responses to platelets and serotonin in spontaneously hypertensive rats. Hypertension 1986; 8: II55–60.
Xavier FE, Davel AP, Rossoni LV, Vassallo DV . Time-dependent hyperreactivity to phenylephrine in aorta from untreated diabetic rats: role of prostanoids and calcium mobilization. Vasc Pharmacol 2003; 40: 67–76.
Guyton AC, Coleman TG, Cowley AV Jr, Scheel KW, Manning Jr RD, Norman Jr RA . Arterial pressure regulation. Overriding dominance of the kidneys in long-term regulation and in hypertension. Am J Med 1972; 52: 584–94.
D'Orléans-Juste P, Dion S, Mizrahi J, Regoli D . Effects of peptides and non-peptides on isolated arterial smooth muscles: role of endothelium. Eur J Pharmacol 1985; 114: 9–21.
Wu HY, Jeng YY, Yue CJ, Chyu KY, Hsueh WA, Chan TM . Endothelial-dependent vascular effects of insulin and insulin-like growth factor I in the perfused rat mesenteric artery and aortic ring. Diabetes 1994; 43: 1027–32.
Cohen AJ, McCarthy DM, Stoff JS . Direct hemodynamic effect of insulin in the isolated perfused kidney. Am J Physiol 1989; 257: F580–5.
Torffvit O, Edvinsson L . Relaxing effect of insulin in renal arteries from diabetic rats. Regul Pept 1999; 79: 147–52.
Taylor PD, Oon BB, Thomas CR, Poston L . Prevention by insulin treatment of endothelial dysfunction but not enhanced noradrenaline-induced contractility in mesenteric resistance arteries from streptozotocin-induced diabetic rats. Br J Pharmacol 1994; 111: 35–41.
Auch-Schwelk W, Vanhoutte PM . Contractions to endothelin in normotensive and spontaneously hypertensive rats: role of endothelium and prostaglandins. Blood Press 1992; 1: 45–9.
Nakashima M, Vanhoutte PM . Endothelin-1 and -3 cause endothelium-dependent hyperpolarization in the rat mesenteric artery. Am J Physiol 1993; 265: H2137–41.
Büssemaker E, Popp R, Binder J, Busse R, Fleming I . Characterization of the endothelium-derived hyperpolarizing factor (EDHF) response in the human interlobar artery. Kidney Int 2003; 63: 1749–55.
Mian MO, Idris-Khodja N, Li MW, Leibowitz A, Paradis P, Rautureau Y, et al. Preservation of endothelium-dependent relaxation in atherosclerotic mice with endothelium-restricted endothelin-1 overexpression. J Pharmacol Exp Ther 2013; 347: 30–7.
Rapoport RM, Williams SP . Role of prostaglandins in acetylcholine-induced contraction of aorta from spontaneously hypertensive and Wistar-Kyoto rats. Hypertension 1996; 28: 64–75.
Deacon K, Knox AJ . Endothelin-1 (ET-1) increases the expression of remodeling genes in vascular smooth muscle through linked calcium and cAMP pathways: role of a phospholipase A2(cPLA2)/cyclooxygenase-2 (COX-2)/prostacyclin receptor-dependent autocrine loop. J Biol Chem 2010; 285: 25913–27.
Inscho EW, Carmines PK, Navar LG . Prostaglandin influences on afferent arteriolar responses to vasoconstrictor agonists. Am J Physiol 1990; 259: F157–63.
Eskildsen MP, Hansen PB, Stubbe J, Toft A, Walter S, Marcussen N, et al. Prostaglandin I2 and prostaglandin E2 modulate human intrarenal artery contractility through prostaglandin E2-EP4, prostacyclin-IP, and thromboxane A2-TP receptors. Hypertension 2014; 64: 551–6.
De Mey JG, Vanhoutte PM . End o' the line revisited: moving on from nitric oxide to CGRP. Life Sci 2014; 118: 120–8.
Vanhoutte PM . Say No to ET. J Auton Nerv Syst 2000; 81: 271–7.
Acknowledgements
This work was supported by the Swiss National Science Foundation (grants 138 754 and 143 672 to Oliver BARETELLA) and the Hong Kong Research Grant Council (780410M). The authors thank Dr Kenneth CHENG and Godfrey MAN for their expertise with genotyping and animal handling, respectively, as well as Boris CHAN for help with blinding the assays of ET-1.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baretella, O., Chung, S., Xu, A. et al. Endothelial overexpression of endothelin-1 modulates aortic, carotid, iliac and renal arterial responses in obese mice. Acta Pharmacol Sin 38, 498–512 (2017). https://doi.org/10.1038/aps.2016.138
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2016.138
- Springer Nature Singapore Pte Ltd.
Keywords
This article is cited by
-
Paradoxical lack of increase in endothelin-1 levels in obese mice – possible role of endothelin-B receptors
Acta Pharmacologica Sinica (2017)