Abstract
Study Design
Numerical planning and simulation of immediate and post-two-year growth modulation effects of Anterior Vertebral Body Growth Modulation (AVBGM).
Objectives
To develop a planning tool based on a patient-specific finite element model (FEM) of pediatric scoliosis integrating growth to computationally assess the 3D biomechanical effects of AVBGM.
Summary of Background Data
AVBGM is a recently introduced fusionless compression-based approach for pediatric scoliotic patients presenting progressive curves. Surgical planning is mostly empirical, with reported issues including overcorrection (inversion of the side) of the curve and a lack of control on 3D correction.
Methods
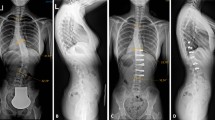
Twenty pediatric scoliotic patients instrumented with AVBGM were assessed. An osseoligamentous FEM of the spine, rib cage, and pelvis was generated before surgery using the patient′s 3D reconstruction obtained from calibrated biplanar radiographs. For each case, different scenarios of AVBGM and two years of vertebral growth and growth modulation due to gravitational loads and forces from AVBGM were simulated. Simulated correction indices in the coronal, sagittal, and transverse planes for the retained scenario were computed and a posteriori compared to actual patient′s postoperative and two years’ follow-up data.
Results
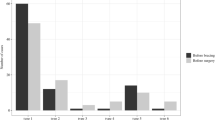
The simulated immediate postoperative Cobb angles were on average within 3° of that of the actual correction, while it was ±5° for kyphosis/lordosis angles, and ±5° for apical axial rotation. For the simulated 2-year postoperative follow-up, correction results were predicted at ±3° for Cobb angles and ±5° for kyphosis/lordosis angles, ±2% for T1–L5 height, and ±4° for apical axial rotation.
Conclusion
A numeric model simulating immediate and post-two-year effects of AVBGM enabled to assess different implant configurations to support surgical planning.
Level of Evidence
Level III.
Similar content being viewed by others
References
Asher MA, Burton DC. Adolescent idiopathic scoliosis: natural history and long term treatments effects. Scoliosis 2006;1:2.
Betz RR, Ranade A, Samdani AF. Vertebral body stapling: a fusionless treatment option for a growing child with moderate idiopathic scoliosis. Spine 2010;35:169–76.
Fletcher ND, Bruce RW. Early-onset scoliosis: current concepts and controversies. Curr Rev Muskuloskelet Med 2012;5:102–10.
Driscoll M, Aubin CE, Moreau A, et al. Biomechanical comparison of fusionless growth modulation corrective techniques in pediatric scoliosis. Med Biol Eng Comput 2011;49:1437–45.
Skaggs DL, Akbarnia BA, Flynn JM, et al. A classification of growth friendly spine implants. J Pediatr Orthop 2014;34:260–74.
Akbarnia BA. Fusionless procedures for the management of early-onset spine deformities in 2011: what do we know? J Child Orthop 2011;5:159–72.
Samdani AF, Ames RJ, Kimball JS, et al. Anterior vertebral body tethering for idiopathic scoliosis: two-year results. Spine 2014;39:1688–93.
Samdani AF, Ames RJ, Kimball JS, et al. Anterior vertebral body tethering for immature adolescent idiopathic scoliosis: one-year results on the first 32 patients. Eur Spine J 2015;24:1533–9.
Crawford CH, Lenke L. Growth modulation by means of anterior tethering resulting in progressive correction of juvenile idiopathic scoliosis. J Bone Joint Surg Am 2010;92:202–9.
Driscoll M, Aubin CE, Moreau A, et al. Finite element comparison of different growth sparring instrumentation systems for the early treatment of idiopathic scoliosis. Stud Health Technol Inform 2010;158: 89–94.
Clin J, Aubin CE, Parent S. Biomechanical simulation and analysis of scoliosis correction using a fusionless intravertebral epiphyseal device. Spine 2015;40:369–76.
Humbert L, de Guise JA, Aubert B, et al. 3D reconstruction of the spine from bi-planar x-rays using parametric models based on transversal and longitudinal inferences. Med Eng Phys 2009;31:681–7.
Pomero V, Mitton D, Laporte S, et al. Fast accurate stereoradiographic 3D-reconstruction of the spine using a combined geometric and statistic model. Clin Biomech 2004;19:240–7.
Descrimes JL, Aubin C-E, Skalli W, et al. Modelling of facet joints in a finite element model of the scoliotic spine and thorax: mechanical aspects. Rachis 1995;7:301–14.
Panjabi M, Brand R, White A. Three-dimensional flexibility and stiffness properties ofthe human thoracic spine. J Biomech 1976;9:185–92.
Chazal J, Tanguy A, Bourges M, et al. Biomechanical properties of spinal ligaments and a histological study of the supraspinal ligament in traction. J Biomech 1985;18:167–76.
Pezowicz C, Glowacki M. The mechanical properties of human rib in young adult. Acta Bioeng Biomech 2012;14:53–60.
Stokes I. Analysis and simulation of progressive adolescent scoliosis by biomechanical growth simulation. Eur Spine J 2007;16:1621–8.
Stokes I, Aronsson D, Dimock A, et al. Endochondral growth in growth plates of three species at two anatomical locations modulated by mechanical compression. J Orthop Res 2006;10:1327–33.
Canavese F, Dimeglio A. Normal and abnormal spine and thoracic cage development. World J Orthop 2013;4:167–74.
Schultz A, Andersson G, Ortengren R, et al. Loads on the lumbar spine. Validation of a biomechanical analysis by measurement of intradiscal pressures and myoelectric signals. J Bone Joint Surg 1982;64:713–20.
Driscoll M, Aubin CE, Moreau A, et al. The role of concave—convex biases in the progression of idiopathic scoliosis. Eur Spine J 2009; 18: 180–7.
Villemure I, Aubin CE, Dansereau J. Simulation of progressive deformities in adolescent idiopathic scoliosis using a biomechanical model integrating vertebral growth. J Biomed Eng 2002; 124: 784–90.
Pearsall DJ, Reid JG, Livingston LA. Segmental inertial parameters of the human trunk as determined from computed tomography. Ann Biomed Eng 1996;24:198–210.
Hoh DJ, Elder JB, Wang MY. Principles of growth modulation in the treatment of scoliotic deformities. Neurosurgery 2008;63:211–21.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures: NC (grants from Natural Sciences and Engineering Research Council of Canada, during the conduct of the study; grants from Canadian Institutes of Health Research, outside the submitted work); CEA (grants from Natural Sciences and Engineering Research Council of Canada, during the conduct of the study; other from Medtronic; grants from Canadian Institutes of Health Research, Natural Sciences and Engineering Research Council of Canada, Canada Research Chair, Zimmer CAS, and Canada First Research Excellence Funds, outside the submitted work); SP (grants from Natural Sciences and Engineering Research Council of Canada, during the conduct of the study; other from Scoliosis Research Society and Canadian Spine Society; personal fees from DePuy Synthes Spine, Medtronic, EOS-Imaging, and K2M; grants from DePuy Synthes Spine, Setting Scoliosis Straight Foundation, Medtronic, EOS-Imaging, Spinologics, Canadian Institutes of Health Research, Canadian Foundation for Innovation, and Natural Sciences and Engineering Council of Canada; personal fees from Fonds de Recherche Québec–Santé; grants from Orthopedic Research and Education Foundation and Rick Hansen Institutes; other from Academic Chair in Pediatric Spinal Deformities of CHU Ste-Justine, outside the submitted work; in addition, SP has a patent Spinologics licensed and stock/stock options with Spinologics).
The engineering analysis and simulation portion within this project were separately funded by the Natural Sciences and Engineering Research Council of Canada (Industrial Research Chair program with Medtronic of Canada) (grant number PCIPJ-346145).
Rights and permissions
About this article
Cite this article
Cobetto, N., Aubin, CE. & Parent, S. Surgical Planning and Follow-up of Anterior Vertebral Body Growth Modulation in Pediatric Idiopathic Scoliosis Using a Patient-Specific Finite Element Model Integrating Growth Modulation. Spine Deform 6, 344–350 (2018). https://doi.org/10.1016/j.jspd.2017.11.006
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2017.11.006