Abstract
Study Design
Multicenter retrospective review.
Objective
To assess the effectiveness of using the stable sagittal vertebra (SSV) for selecting the lowest instrumented vertebrae (LIV) to prevent distal junctional kyphosis (DJK) in selective thoracic fusions.
Summary of Background Data
Cho et al. reported that including the SSV in a fusion decreased the rate of DJK in thoracic hyperkyphosis.
Methods
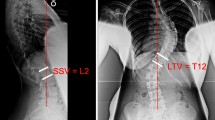
A retrospective review was performed of patients from two pediatric hospitals with adolescent idiopathic scoliosis who underwent selective posterior thoracic fusion with the LIV at L2 or above from 2000 to 2012. Patients with less than 2 years’ follow-up were excluded. The primary outcome measure was DJK, defined radiographically as ≥10° between the superior end plate of the LIV and the inferior end plate of the vertebra below on a standing lateral radiograph. We investigated the SSV, which was defined as the vertebral level at which 50% of the vertebral body was in front of the posterior sacral vertical line (PSVL) on a standing lateral radiograph. This particular definition was referred to as SSV.
Results
A total of 113 patients met the inclusion criteria. Mean age was 14.4 years. Mean Cobb angle was 58°. The overall rate of DJK was 7% (8/113). When the LIV was superior to SSV, the rate of DJK was 17% (8/46) versus 0% (0/67) when the LIV was at or inferior to SSV (p=.01). The rates of DJK for patients with the LIV one, two, and three levels above SSV were 17% (4/24), 7% (1/14), and 43% (3/7), respectively. There was no significant association between preoperative or postoperative maximum kyphosis, thoracic kyphosis, thoracolumbar kyphosis, pelvic incidence, sagittal balance or coronal balance, and development of DJK.
Conclusion
Although LIV selection is complex, choosing the LIV at or below the SSV is a simple rule that minimizes the risk of DJK.
Level of Evidence
Level IV.
Similar content being viewed by others
References
Lenke LG, Edwards 2nd CC, Bridwell KH. The Lenke classification of adolescent idiopathic scoliosis: how it organizes curve patterns as a template to perform selective fusions of the spine. Spine 2003;28:S199–207.
Lenke LG, Betz RR, Bridwell KH, et al. Spontaneous lumbar curve coronal correction after selective anterior or posterior thoracic fusion in adolescent idiopathic scoliosis. Spine 1999;24:1663–71; discussion 72.
Newton PO, O’Brien MF. Idiopathic scoliosis: The Harms Study Group treatment guide. New York: Thieme; 2011.
Lenke LG, Betz RR, Haher TR, et al. Multisurgeon assessment of surgical decision-making in adolescent idiopathic scoliosis: curve classification, operative approach, and fusion levels. Spine 2001;26:2347–53.
King HA, Moe JH, Bradford DS, Winter RB. The selection of fusion levels in thoracic idiopathic scoliosis. J Bone Joint Surg Am 1983;65:1302–13.
Trobisch PD, Ducoffe AR, Lonner BS, Errico TJ. Choosing fusion levels in adolescent idiopathic scoliosis. J Am Acad Orthop Surg 2013;21:519–28.
Danielsson AJ, Cederlund CG, Ekholm S, Nachemson AL. The prevalence of disc aging and back pain after fusion extending into the lower lumbar spine. A matched MR study twenty-five years after surgery for adolescent idiopathic scoliosis. Acta Radiol 2001;42:187–97.
Suk SI, Lee SM, Chung ER, et al. Determination of distal fusion level with segmental pedicle screw fixation in single thoracic idiopathic scoliosis. Spine 2003;28:484–91.
Takahashi J, Newton PO, Ugrinow VL, Bastrom TP. Selective thoracic fusion in adolescent idiopathic scoliosis: factors influencing the selection of the optimal lowest instrumented vertebra. Spine 2011;36:1131–41.
Cho KJ, Lenke LG, Bridwell KH, et al. Selection of the optimal distal fusion level in posterior instrumentation and fusion for thoracic hyperkyphosis: the sagittal stable vertebra concept. Spine 2009;34:765–70.
O’Brien MF, Kuklo TR, Blanke KM, Lenke LG, editors. Spinal Deformity Study Group radiographic measurement manual. Memphis, TN: Medtronic Sofamor Danek USA; 2008.
Cochran T, Irstam L, Nachemson A. Long-term anatomic and functional changes in patients with adolescent idiopathic scoliosis treated by Harrington rod fusion. Spine 1983;8:576–84.
Dickson JH, Erwin WD, Rossi D. Harrington instrumentation and arthrodesis for idiopathic scoliosis. A twenty-one-year follow-up. J Bone Joint Surg Am 1990;72:678–83.
Lenke LG, Betz RR, Harms J, et al. Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 2001;83:1169–81.
Ameri E, Behtash H, Mobini B, et al. The prevalence of distal junctional kyphosis following posterior instrumentation and arthrodesis for adolescent idiopathic scoliosis. Acta Medica Iran 2011;49:357–63.
Luhmann SJ, Lenke LG, Bridwell KH, Schootman M. Revision surgery after primary spine fusion for idiopathic scoliosis. Spine 2009;34:2191–7.
Lowe TG, Lenke L, Betz R, et al. Distal junctional kyphosis of adolescent idiopathic thoracic curves following anterior or posterior instrumented fusion: incidence, risk factors, and prevention. Spine 2006;31:299–302.
Campos M, Dolan L, Weinstein S. Unanticipated revision surgery in adolescent idiopathic scoliosis. Spine 2012;37:1048–53.
Bago J, Ramirez M, Pellise F, Villanueva C. Survivorship analysis of Cotrel-Dubousset instrumentation in idiopathic scoliosis. Eur Spine J 2003;12:435–9.
Richards BS, Hasley BP, Casey VF. Repeat surgical interventions following “definitive” instrumentation and fusion for idiopathic scoliosis. Spine 2006;31:3018–26.
Asher M, Lai SM, Burton D, et al. Safety and efficacy of Isola instrumentation and arthrodesis for adolescent idiopathic scoliosis: two- to 12-year follow-up. Spine 2004;29:2013–23.
Lenke LG, Betz RR, Clements D, et al. Curve prevalence of a new classification of operative adolescent idiopathic scoliosis: does classification correlate with treatment? Spine 2002;27:604–11.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures
JY (none), LMA (personal fees from Biomet; Medtronic, other from Eli Lilly, personal fees from Orthobullets, nonfinancial support from Pediatric Orthopaedic Society of North America, nonfinancial support from Scoliosis Research Society, other from Journal of Pediatric Orthopaedics, outside the submitted work), AMB (none), NRG (none), KKB (none), AGG (nonfinancial support from Journal of Orthopaedic Trauma, outside the submitted work), JMF (personal fees from Biomet, outside the submitted work), VTT (other from Journal of Bone and Joint Surgery—American, other from Wolters Kluwer Health—Lippincott Williams & Wilkins, outside the submitted work), DLS (grants from Pediatric Orthopaedic Society of North America & Scoliosis Research Society, Paid to Columbia University; Ellipse [Co-PI, Paid to GSF], personal fees from ZimmerBiomet; Medtronic; Zipline Medical, Inc; Orthobullets; Grand Rounds [a healthcare navigation company], Green Sun Medical, other from Zipline Medical, Inc, Green Sun Medical, other from Orthobullets, nonfinancial support from Growing Spine Study Group, Scoliosis Research Society, Growing Spine Foundation, personal fees from ZimmerBiomet; Medtronic; Johnson & Johnson, from Medtronic & ZimmerBiomet, other from Wolters Kluwer Health—Lippincott Williams & Wilkins; Biomet Spine, other from Orthobullets, Co-Editor in Chief, outside the submitted work).
Rights and permissions
About this article
Cite this article
Yang, J., Andras, L.M., Broom, A.M. et al. Preventing Distal Junctional Kyphosis by Applying the Stable Sagittal Vertebra Concept to Selective Thoracic Fusion in Adolescent Idiopathic Scoliosis. Spine Deform 6, 38–42 (2018). https://doi.org/10.1016/j.jspd.2017.06.007
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2017.06.007