Abstract
Purpose
Although diversity, equity, and inclusion (DEI) principles are increasingly recognized as a critical component of surgical education, most departments of surgery lack a structured DEI curriculum. The purpose of this paper is to describe how our institution’s Department of Surgery created an innovative curriculum that integrates the individual experiences of members of our department into our department’s educational curriculum.
Methods
We developed a novel DEI curriculum that was customized based on a departmental survey. The curriculum was integrated into our General Surgery Grand Rounds and Morbidity and Mortality (M&M) conferences started in 2020 and is ongoing.
Results
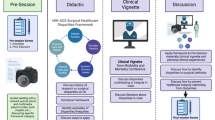
The departmental environmental scan and needs assessment included 99 quantitative and qualitative questions. 204 individuals participated (response rate, 51%). The needs assessment queried participants’ knowledge of DEI-related topics, perceptions of privilege, and insight into the overall climate in the department. Areas that were felt to be of particular concern were viewed as educational opportunities and prioritized as elements of the curriculum. A total of 13 DEI sessions were included over the course of 2 academic years. Topics included, but were not limited to, implicit bias mitigation, inclusive language, inclusive teaching, and microaggressions. Additional discussion sessions were incorporated that concentrated on trauma-informed care and op-ed writing. These sessions were held via Zoom and later transitioned to hybrid sessions with an average of 66 Zoom participants and 42 in-person participants. The cornerstone of the curriculum is an annual department-sponsored asynchronous screening of a DEI-related documentary, followed by a reflective discussion session. Additionally, a Health Equity Classification System was developed and incorporated into our weekly morbidity and mortality conferences and served as an adjunct to the traditional Clavien–Dindo taxonomy to discuss surgical complications that involve bias and health access issues.
Conclusions
When effectively implemented, DEI curricula have the potential to equip trainees and practicing surgeons with the proper tools to meaningfully engage with one another and the community they serve. Elements of a DEI curriculum that were felt to be critical for success included ensuring the content of the curriculum was tailored for the audience, alignment with the department’s global DEI efforts, and integration of innovative pedagogical methods that encouraged reflection.
Similar content being viewed by others
Data availability
The departmental environmental scan and needs assessment generated and analyzed during the current study are not publicly available because they were intended for internal use only, but are available from the corresponding author on reasonable request.
References
Deane B, Ferdman BM. Diversity at work the practice of inclusion. Wiley; 2014.
O’Donovan D. Diversity and inclusion in the Workplace. Manag Ind Eng. 2017;10:73–108. https://doi.org/10.1007/978-3-319-66864-2_4.
Rosenkranz KM, Arora TK, Termuhlen PM, Stain SC, Misra S, Dent D, Nfonsam V. Diversity, equity and inclusion in medicine: Why it matters and how do we achieve it? J Surg Educ. 2021;78(4):1058–65. https://doi.org/10.1016/j.jsurg.2020.11.013.
Meneses E, McKenney M, Elkbuli A. Diversity and inclusion among us general surgery residency programs: translating initiatives into action. Am Surg. 2020;87(1):166–7. https://doi.org/10.1177/0003134820948887.
(N.d.). Retrieved from https://www.culturalcomplications.com/. Accessed 21 May 2023
Sartania N, Sneddon S, Boyle JG, McQuarrie E, de Koning HP. Increasing collaborative discussion in case-based learning improves student engagement and knowledge acquisition. Med Sci Educ. 2022;32(5):1055–64. https://doi.org/10.1007/s40670-022-01614-w.
Fredricks JA, Blumenfeld PC, Paris AH. School engagement: Potential of the concept, state of the evidence. Rev Educ Res. 2004;74(1):59–109. https://doi.org/10.3102/00346543074001059.
McLean SF. Case-based learning and its application in medical and health-care fields: a review of worldwide literature. J Med Educ Curric Dev. 2016. https://doi.org/10.4137/jmecd.s20377.
Stain SC, Mitchell M, Belue R, Mosley V, Wherry S, Adams CZ, Williams PC. Objective assessment of videoconferenced lectures in a surgical clerkship. Am J Surg. 2005;189(1):81–4. https://doi.org/10.1016/j.amjsurg.2004.04.012.
Haider AH, Scott VK, Rehman KA, Velopulos C, Bentley JM, Cornwell EE, Al-Refaie W. Racial disparities in surgical care and outcomes in the United States: a comprehensive review of patient, provider, and systemic factors. J Am Coll Surg. 2013. https://doi.org/10.1016/j.jamcollsurg.2012.11.014.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nicholson, K., Reid, R., Roggin, K. et al. Integration of a needs-based diversity, equity, and inclusion curriculum into surgical education. Global Surg Educ 3, 1 (2024). https://doi.org/10.1007/s44186-023-00202-9
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44186-023-00202-9