Abstract
Background
Meniscal injuries frequently require surgical intervention to restore knee joint function and stability. Intraoperative platelet-rich plasma (PRP) injection has emerged as a potential adjunctive therapy to enhance tissue healing post-meniscal repair. This systematic review and meta-analysis aimed to evaluate the efficacy of PRP in terms of pain relief, functional recovery, and overall success rates in patients undergoing meniscal repair procedures.
Methods
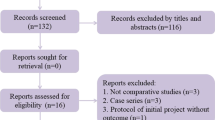
A comprehensive search strategy was employed to identify relevant studies across Scopus, PubMed, Embase, and the Cochrane Library databases. The inclusion criteria encompassed human studies, including randomized controlled trials (RCTs), cohorts, and case–control studies, focusing on intraoperative platelet-rich plasma (PRP) use post-meniscal repair and reporting outcomes related to pain, functionality, and cure rates. Exclusion criteria comprised animal studies, non-English publications, studies lacking relevant outcome measures, and those with insufficient data. Two reviewers independently screened titles and abstracts, resolving disagreements through consensus or consultation with a third reviewer, followed by a full-text assessment for potentially eligible studies. Data extraction was conducted independently by two reviewers using a standardized form. The reliability of observational studies was evaluated using the Newcastle–Ottawa Scale. Subgroup analyses and pooled effect estimates for main outcomes were computed using RevMan 5.3, a meta-analysis tool.
Results
The demographic analysis revealed that the PRP group had an average age of 41.39 years, while the control group had an average age of 42.1 years. In terms of gender distribution, the PRP group consisted of 61 men and 29 women, while the control group had 62 men and 34 women. Pain ratings showed a preference for PRP with a mean difference of 4.83 (p = 0.13). However, there was no significant difference in Lysholm scores (mean difference: − 0.44, p = 0.91) or IKDC scores (mean difference: 2.80, p = 0.14) between the PRP and control groups. Similarly, ROM measures did not show a statistically significant difference, with a mean difference of 2.80 (p = 0.18). Additionally, there was no significant distinction in failure rates between the PRP and control groups, as indicated by a weighted mean difference of 0.71 (p = 0.52). These findings suggest that while PRP may offer some benefits in pain relief, its impact on functional recovery, range of motion, and failure rates following meniscal repair procedures is inconclusive.
Conclusion
The current evidence regarding the effect of intraoperative platelet-rich plasma (PRP) injection on patients undergoing meniscal repair remains inconclusive. While some studies suggest potential benefits in terms of pain relief and functional recovery, others show no significant differences compared to control groups. The impact of PRP therapy on overall success rates, including rates of re-tear and revision surgery, is also uncertain. Further well-designed randomized controlled trials with larger sample sizes are needed to provide more robust evidence and guide clinical practice in orthopedic surgery.







Similar content being viewed by others
Data availability
Not applicable.
References
Rodeo, S. A., Monibi, F., Dehghani, B., & Maher, S. (2020). Biological and mechanical predictors of meniscus function: Basic science to clinical translation. Journal of Orthopaedic Research, 38(5), 937–945. https://doi.org/10.1002/jor.24552
Smith, N. A., Parkinson, B., Hutchinson, C. E., Costa, M. L., & Spalding, T. (2016). Is meniscal allograft transplantation chondroprotective? A systematic review of radiological outcomes. Knee Surgery, Sports Traumatology, Arthroscopy, 24(9), 2923–2935. https://doi.org/10.1007/s00167-015-3573-0
Calanna, F., Duthon, V., & Menetrey, J. (2022). Rehabilitation and return to sports after isolated meniscal repairs: A new evidence-based protocol. Journal of Experimental Orthopaedics, 9(1), 80. https://doi.org/10.1186/s40634-022-00521-8
Perelli, S. (2023). Meniscal injuries of the knee. In Textbook of musculoskeletal disorders (pp. 451–9). Springer.
Papalia, R., Del Buono, A., Osti, L., Denaro, V., & Maffulli, N. (2011). Meniscectomy as a risk factor for knee osteoarthritis: A systematic review. British Medical Bulletin, 99(1), 89–106. https://doi.org/10.1093/bmb/ldq043
Li, Z., & Weng, X. (2022). Platelet-rich plasma use in meniscus repair treatment: A systematic review and meta-analysis of clinical studies. Journal of Orthopaedic Surgery and Research, 17(1), 446. https://doi.org/10.1186/s13018-022-03293-0
Medina-Porqueres, I., Martin-Garcia, P., Sanz-De-Diego, S., Gomez-Caceres, A., Moya-Torrecilla, F., Reyes-Eldblom, M., et al. (2022). Clinical and functional outcome of meniscal injuries treated with platelet-rich plasma: A single-center case series. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph19127118
Patil, P. (2023). Therapeutic uses of platelet-rich plasma (PRP) in sport injuries—A narrative review. Journal of Orthopaedic Reports 100287.
Dos Santos, R. G., Santos, G. S., Alkass, N., Chiesa, T. L., Azzini, G. O., da Fonseca, L. F., et al. (2021). The regenerative mechanisms of platelet-rich plasma: A review. Cytokine, 144(155560), 155560. https://doi.org/10.1016/j.cyto.2021.155560
Verma, R., Kumar, S., Garg, P., & Verma, Y. K. (2023). Platelet-rich plasma: A comparative and economical therapy for wound healing and tissue regeneration. Cell and Tissue Banking, 24(2), 285–306. https://doi.org/10.1007/s10561-022-10039-z
Dragoo, J. L., Braun, H. J., Durham, J. L., Ridley, B. A., Odegaard, J. I., Luong, R., et al. (2012). Comparison of the acute inflammatory response of two commercial platelet-rich plasma systems in healthy rabbit tendons. American Journal of Sports Medicine, 40(6), 1274–1281. https://doi.org/10.1177/0363546512442334
Laudy, A. B. M., Bakker, E. W. P., Rekers, M., & Moen, M. H. (2015). Efficacy of platelet-rich plasma injections in osteoarthritis of the knee: A systematic review and meta-analysis. British Journal of Sports Medicine, 49(10), 657–672. https://doi.org/10.1136/bjsports-2014-094036
Sundman, E. A., Cole, B. J., & Fortier, L. A. (2011). Growth factor and catabolic cytokine concentrations are influenced by the cellular composition of platelet-rich plasma. American Journal of Sports Medicine, 39(10), 2135–2140. https://doi.org/10.1177/0363546511417792
Cecerska-Heryć, E., Goszka, M., Serwin, N., Roszak, M., Grygorcewicz, B., Heryć, R., et al. (2022). Applications of the regenerative capacity of platelets in modern medicine. Cytokine & Growth Factor Reviews, 64, 84–94. https://doi.org/10.1016/j.cytogfr.2021.11.003
Mishra, A., Woodall, J., Jr., & Vieira, A. (2009). Treatment of tendon and muscle using platelet-rich plasma. Clinics in Sports Medicine, 28(1), 113–125. https://doi.org/10.1016/j.csm.2008.08.007
McRobb, J., Kamil, K. H., Ahmed, I., Dhaif, F., & Metcalfe, A. (2023). Influence of platelet-rich plasma (PRP) analogues on healing and clinical outcomes following anterior cruciate ligament (ACL) reconstructive surgery: A systematic review. European Journal of Orthopaedic Surgery & Traumatology, 33(2), 225–253. https://doi.org/10.1007/s00590-021-03198-4
Zhang, J., Middleton, K. K., Fu, F. H., Im, H.-J., & Wang, J.H.-C. (2013). HGF mediates the anti-inflammatory effects of PRP on injured tendons. PLoS ONE, 8(6), e67303. https://doi.org/10.1371/journal.pone.0067303
Chen, X., Jones, I. A., Togashi, R., Park, C., & Vangsness, C. T., Jr. (2020). Use of platelet-rich plasma for the improvement of pain and function in rotator cuff tears: A systematic review and meta-analysis with bias assessment. American Journal of Sports Medicine, 48(8), 2028–2041. https://doi.org/10.1177/0363546519881423
Everts, P. A., van Erp, A., DeSimone, A., Cohen, D. S., & Gardner, R. D. (2021). Platelet rich plasma in orthopedic surgical medicine. Platelets, 32(2), 163–174. https://doi.org/10.1080/09537104.2020.1869717
Mishra, A. K., Skrepnik, N. V., Edwards, S. G., Jones, G. L., Sampson, S., Vermillion, D. A., et al. (2014). Efficacy of platelet-rich plasma for chronic tennis elbow: A double-blind, prospective, multicenter, randomized controlled trial of 230 patients: A double-blind, prospective, multicenter, randomized controlled trial of 230 patients. American Journal of Sports Medicine, 42(2), 463–471. https://doi.org/10.1177/0363546513494359
Yang, C.-P., Hung, K.-T., Weng, C.-J., Chen, A.C.-Y., Hsu, K.-Y., & Chan, Y.-S. (2021). Clinical outcomes of meniscus repair with or without multiple intra-articular injections of platelet rich plasma after surgery. Journal of Clinical Medicine, 10(12), 2546. https://doi.org/10.3390/jcm10122546
Fabbro, M. D., Bortolin, M., Taschieri, S., Ceci, C., & Weinstein, R. L. (2016). Antimicrobial properties of platelet-rich preparations. A systematic review of the current pre-clinical evidence. Platelets, 27(4), 276–285. https://doi.org/10.3109/09537104.2015.1116686
Bennell, K. L., Paterson, K. L., Metcalf, B. R., Duong, V., Eyles, J., Kasza, J., et al. (2021). Effect of intra-articular platelet-rich plasma vs placebo injection on pain and medial tibial cartilage volume in patients with knee osteoarthritis: The RESTORE randomized clinical trial: The RESTORE randomized clinical trial. JAMA, 326(20), 2021–2030. https://doi.org/10.1001/jama.2021.19415
Sheth, U., Simunovic, N., Klein, G., Fu, F., Einhorn, T. A., Schemitsch, E., et al. (2012). Efficacy of autologous platelet-rich plasma use for orthopaedic indications: A meta-analysis. Journal of Bone and Joint Surgery. American Volume, 94(4), 298–307. https://doi.org/10.2106/JBJS.K.00154
Pujol, N., Salle De Chou, E., Boisrenoult, P., & Beaufils, P. (2015). Platelet-rich plasma for open meniscal repair in young patients: any benefit? Knee Surgery, Sports Traumatology, Arthroscopy, 23(1), 51–58. https://doi.org/10.1007/s00167-014-3417-3
Yi, X., Lee, J. E., Lee, Y. H., Yu, X., & Lee, H. S. (2023). Clinical efficacy of platelet-rich plasma combined with arthroscopic meniscal plasty on pain, function and physiologic indicators in elderly patients with knee meniscus injury: A retrospective observational study. American Journal of Translational Research, 15(6), 3806–3814.
Griffin, J. W., Hadeed, M. M., Werner, B. C., Diduch, D. R., Carson, E. W., & Miller, M. D. (2015). Platelet-rich plasma in meniscal repair: Does augmentation improve surgical outcomes? Clinical Orthopaedics and Related Research, 473(5), 1665–1672. https://doi.org/10.1007/s11999-015-4170-8
Filardo, G. (2012). Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: Single-versus double-spinning approach. Knee Surgery, Sports Traumatology, 20, 2082–2091.
Khoshbin, A., Leroux, T., Wasserstein, D., Marks, P., Theodoropoulos, J., Ogilvie-Harris, D., et al. (2013). The efficacy of platelet-rich plasma in the treatment of symptomatic knee osteoarthritis: A systematic review with quantitative synthesis. Arthroscopy, 29(12), 2037–2048. https://doi.org/10.1016/j.arthro.2013.09.006
Tomio, J., Yamana, H., Matsui, H., Yamashita, H., Yoshiyama, T., & Yasunaga, H. (2017). Tuberculosis screening prior to anti-tumor necrosis factor therapy among patients with immune-mediated inflammatory diseases in Japan: A longitudinal study using a large-scale health insurance claims database. International Journal of Rheumatic Diseases, 20(11), 1674–1683. https://doi.org/10.1111/1756-185x.13190
Moraes, V. Y., Lenza, M., Tamaoki, M. J., Faloppa, F., & Belloti, J. C. (2014). Platelet-rich therapies for musculoskeletal soft tissue injuries. Cochrane Database of Systematic Reviews, (4), CD010071. https://doi.org/10.1002/14651858.CD010071.pub3
Smith, H. C. (2012). Risk factors for anterior cruciate ligament injury: A review of the literature-part 1: Neuromuscular and anatomic risk. Sports Health, 4(1), 69–78.
Dai, W.-L., Zhou, A.-G., Zhang, H., & Zhang, J. (2017). Efficacy of platelet-rich plasma in the treatment of knee osteoarthritis: A meta-analysis of randomized controlled trials. Arthroscopy, 33(3), 659-670.e1. https://doi.org/10.1016/j.arthro.2016.09.024
Everts, P., Onishi, K., Jayaram, P., Lana, J. F., & Mautner, K. (2020). Platelet-rich plasma: New performance understandings and therapeutic considerations in 2020. International Journal of Molecular Sciences, 21(20), 7794. https://doi.org/10.3390/ijms21207794
Pavlovic, V., Ciric, M., Jovanovic, V., & Stojanovic, P. (2016). Platelet Rich Plasma: A short overview of certain bioactive components. Open Med (Warsz)., 11(1), 242–247. https://doi.org/10.1515/med-2016-0048
Foster, T. E., Puskas, B. L., Mandelbaum, B. R., Gerhardt, M. B., & Rodeo, S. A. (2009). Platelet-rich plasma: From basic science to clinical applications: From basic science to clinical applications. American Journal of Sports Medicine, 37(11), 2259–2272. https://doi.org/10.1177/0363546509349921
Tang, Y., Wang, H., Sun, Y., Jiang, Y., Fang, S., Kan, Z., et al. (2021). Using platelet-rich plasma hydrogel to deliver mesenchymal stem cells into three-dimensional PLGA scaffold for cartilage tissue engineering. ACS Applied Bio Materials, 4(12), 8607–8614. https://doi.org/10.1021/acsabm.1c01160
Nabavizadeh, S. S., Talaei-Khozani, T., Zarei, M., Zare, S., Hosseinabadi, O. K., Tanideh, N., et al. (2022). Attenuation of osteoarthritis progression through intra-articular injection of a combination of synovial membrane-derived MSCs (SMMSCs), platelet-rich plasma (PRP) and conditioned medium (secretome). Journal of Orthopaedic Surgery and Research, 17(1), 102. https://doi.org/10.1186/s13018-021-02851-2
Kon, E., Filardo, G., Di Martino, A., & Marcacci, M. (2011). Platelet-rich plasma (PRP) to treat sports injuries: Evidence to support its use. Knee Surgery, Sports Traumatology, Arthroscopy, 19(4), 516–527. https://doi.org/10.1007/s00167-010-1306-y
Potekaev, N. N., Borzykh, O. B., Medvedev, G. V., Pushkin, D. V., Petrova, M. M., Petrov, A. V., et al. (2021). The role of extracellular matrix in skin wound healing. Journal of Clinical Medicine, 10(24), 5947. https://doi.org/10.3390/jcm10245947
Blalock, D., Miller, A., Tilley, M., & Wang, J. (2015). Joint instability and osteoarthritis. Clinical Medicine Insights: Arthritis and Musculoskeletal Disorders, 8, 15–23. https://doi.org/10.4137/CMAMD.S22147
Laver, L., Marom, N., Dnyanesh, L., Mei-Dan, O., Espregueira-Mendes, J., & Gobbi, A. (2017). PRP for degenerative cartilage disease: A systematic review of clinical studies. Cartilage, 8(4), 341–364. https://doi.org/10.1177/1947603516670709
Sánchez, M., Anitua, E., Orive, G., Mujika, I., & Andia, I. (2009). Platelet-rich therapies in the treatment of orthopaedic sport injuries. Sports Medicine (Auckland, N. Z.), 39(5), 345–354. https://doi.org/10.2165/00007256-200939050-00002
Shen, L., Yuan, T., Chen, S., Xie, X., & Zhang, C. (2017). The temporal effect of platelet-rich plasma on pain and physical function in the treatment of knee osteoarthritis: Systematic review and meta-analysis of randomized controlled trials. Journal of Orthopaedic Surgery and Research, 12(1), 16. https://doi.org/10.1186/s13018-017-0521-3
Weber, A. E., Bolia, I. K., & Trasolini, N. A. (2021). Biological strategies for osteoarthritis: From early diagnosis to treatment. International Orthopaedics, 45(2), 335–344. https://doi.org/10.1007/s00264-020-04838-w
Kon, E., Di Matteo, B., Delgado, D., Cole, B. J., Dorotei, A., Dragoo, J. L., et al. (2020). Platelet-rich plasma for the treatment of knee osteoarthritis: An expert opinion and proposal for a novel classification and coding system. Expert Opinion on Biological Therapy, 20(12), 1447–1460. https://doi.org/10.1080/14712598.2020.1798925
Trams, E., Kulinski, K., Kozar-Kaminska, K., Pomianowski, S., & Kaminski, R. (2020). The clinical use of platelet-rich plasma in knee disorders and surgery—A systematic review and meta-analysis. Life, 10, 94.
Zhu, Y., Yuan, M., Meng, H. Y., Wang, A. Y., Guo, Q. Y., Wang, Y., et al. (2013). Basic science and clinical application of platelet-rich plasma for cartilage defects and osteoarthritis: A review. Osteoarthritis Cartilage, 21(11), 1627–1637. https://doi.org/10.1016/j.joca.2013.07.017
Szwedowski, D., Szczepanek, J., Paczesny, Ł, Zabrzyński, J., Gagat, M., Mobasheri, A., et al. (2021). The effect of platelet-rich plasma on the intra-articular microenvironment in knee osteoarthritis. International Journal of Molecular Sciences, 22(11), 5492. https://doi.org/10.3390/ijms22115492
Şen, E. İ, Yıldırım, M. A., Yeşilyurt, T., Kesiktaş, F. N., & Dıraçoğlu, D. (2020). Effects of platelet-rich plasma on the clinical outcomes and cartilage thickness in patients with knee osteoarthritis. Journal of Back and Musculoskeletal Rehabilitation, 33(4), 597–605. https://doi.org/10.3233/BMR-181209
Tucker, J. D. (2021). Randomized, placebo-controlled analysis of the knee synovial environment following platelet-rich plasma treatment for knee osteoarthritis. PM&R, 13, 707–719.
McLarnon, M., & Heron, N. (2021). Intra-articular platelet-rich plasma injections versus intra-articular corticosteroid injections for symptomatic management of knee osteoarthritis: Systematic review and meta-analysis. BMC Musculoskeletal Disorders, 22(1), 550. https://doi.org/10.1186/s12891-021-04308-3
Zicaro, J. P., Garcia-Mansilla, I., Zuain, A., Yacuzzi, C., & Costa-Paz, M. (2021). Has platelet-rich plasma any role in partial tears of the anterior cruciate ligament? Prospective comparative study. World Journal of Orthopedics, 12(6), 423–432. https://doi.org/10.5312/wjo.v12.i6.423
Zhu, T., Zhou, J., Hwang, J., & Xu, X. (2022). Effects of platelet-rich plasma on clinical outcomes after anterior cruciate ligament reconstruction: A systematic review and meta-analysis. Orthopaedic Journal of Sports Medicine, 10(1), 23259671211061536. https://doi.org/10.1177/23259671211061535
Andriolo, L., Matteo, D., Kon, B., Filardo, E., Venieri, G., & Marcacci, G. (2015). PRP augmentation for ACL reconstruction. BioMed Research International.
Barman, A., Bandyopadhyay, D., Mohakud, S., Sahoo, J., Maiti, R., Mukherjee, S., Prakash, S., Roy, S. S., & Viswanath, A. (2023). Comparison of clinical outcome, cartilage turnover, and inflammatory activity following either intra-articular or a combination of intra-articular with intra-osseous platelet-rich plasma injections in osteoarthritis knee: A randomized, clinical trial. Injury, 54(2), 728–737.
Walton, J., Kozina, E., Woo, F., & Jadidi, S. (2023). A review of patellar tendinopathy in athletes involved in jumping sports. Cureus, 15(10), e47459. https://doi.org/10.7759/cureus.47459
Tischer, T. (2020). Platelet-rich plasma (PRP) as therapy for cartilage, tendon and muscle damage-German working group position statement. Journal of Experimental Orthopaedics, 7(1), 1–11.
Charousset, C., Zaoui, A., Bellaiche, L., & Bouyer, B. (2014). Are multiple platelet-rich plasma injections useful for treatment of chronic patellar tendinopathy in athletes? A prospective study. American Journal of Sports Medicine, 42(4), 906–911. https://doi.org/10.1177/0363546513519964
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Thahir, M., Misbah, I., Bhaskaran, J. et al. Efficacy of Intraoperative Platelet-Rich Plasma After Meniscal Repair: Systematic Review and Meta-analysis. JOIO (2024). https://doi.org/10.1007/s43465-024-01155-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43465-024-01155-x