Abstract
Background
Bone bruises and concomitant ligament injuries after anterior cruciate ligament (ACL) injuries have attracted attention, but their correlation and potential clinical significance remain unclear.
Purpose
To assess the relationship between bone bruises and concomitant ligamentous injuries in ACL injuries.
Study design
Systematic review.
Methods
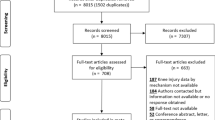
A comprehensive search of PubMed, Embase, Web of Science, and Cochrane Library was completed from inception to October 20, 2021. All articles that evaluated the relationship between bone bruises and related ligaments injuries were included. Methodological Index for Non-Randomized Studies (MINORS) was used for quality assessment as well as Review Manager 5.3 was used for data analysis.
Results
A total of 19 studies evaluating 3292 patients were included. After meta-analysis, anterolateral ligament (ALL) injuries were associated with bone bruising on the lateral tibial plateau (LTP) (RR = 2.33; 95% CI 1.44–3.77; p = 0.0006), lateral femoral condyle (LFC) (RR = 1.97; 95% CI 1.37–2.85; p = 0.0003) and medial tibial plateau (MTP) (RR = 1.62; 95% CI 1.24–2.11; p = 0.0004); Moreover, medial collateral ligament (MCL) injuries were associated with bone bruising on the femur (RR = 1.49; 95% CI 1.17–1.90; p = 0.001), and no statistical significance was found between bone bruising on the MTP and Kaplan fiber (KF) injuries (RR = 1.58; 95% CI 1.00–2.49; p = 0.05). Nonetheless, the current evidence did not conclude that bone bruises were associated with lateral collateral ligament (LCL) injuries.
Conclusion
For individuals with an ACL injury, bone bruises of the LTP, LFC, and MTP can assist in the diagnosis of ALL injuries. Furthermore, femoral bruising has potential diagnostic value for MCL injuries. Knowing these associations allows surgeons to be alert to ACL-related ligament injuries on MRI and during operations in future clinical practice.








Similar content being viewed by others
References
Yang, X. G., Wang, F., He, X., et al. (2020). Network meta-analysis of knee outcomes following anterior cruciate ligament reconstruction with various types of tendon grafts. International Orthopaedics, 44, 365–380.
Gianotti, S. M., Marshall, S. W., Hume, P. A., & Bunt, L. (2009). Incidence of anterior cruciate ligament injury and other knee ligament injuries: A national population-based study. Journal of Science and Medicine in Sport, 12, 622–627.
Lohmander, L. S., Englund, P. M., Dahl, L. L., & Roos, E. M. (2007). The long-term consequence of anterior cruciate ligament and meniscus injuries: Osteoarthritis. The American Journal of Sports Medicine, 35, 1756–1769.
Kostogiannis, I., Ageberg, E., Neuman, P., Dahlberg, L., Fridén, T., & Roos, H. (2007). Activity level and subjective knee function 15 years after anterior cruciate ligament injury: A prospective, longitudinal study of nonreconstructed patients. The American Journal of Sports Medicine, 35, 1135–1143.
Kraeutler, M. J., Bravman, J. T., & McCarty, E. C. (2013). Bone-patellar tendon-bone autograft versus allograft in outcomes of anterior cruciate ligament reconstruction: A meta-analysis of 5182 patients. The American Journal of Sports Medicine, 41, 2439–2448.
Filbay, S. R., Culvenor, A. G., Ackerman, I. N., Russell, T. G., & Crossley, K. M. (2015). Quality of life in anterior cruciate ligament-deficient individuals: A systematic review and meta-analysis. British Journal of Sports Medicine, 49, 1033–1041.
Sonnery-Cottet, B., Daggett, M., Fayard, J. M., et al. (2017). Anterolateral Ligament Expert Group consensus paper on the management of internal rotation and instability of the anterior cruciate ligament—Deficient knee. Journal of Orthopaedics and Traumatology: Official Journal of the Italian Society of Orthopaedics and Traumatology, 18, 91–106.
Dunn, W. R., Spindler, K. P., Amendola, A., et al. (2010). Which preoperative factors, including bone bruise, are associated with knee pain/symptoms at index anterior cruciate ligament reconstruction (ACLR)? A Multicenter Orthopaedic Outcomes Network (MOON) ACLR Cohort Study. The American Journal of Sports Medicine, 38, 1778–1787.
Yoon, K. H., Yoo, J. H., & Kim, K.-I. (2011). Bone contusion and associated meniscal and medial collateral ligament injury in patients with anterior cruciate ligament rupture. Journal of Bone and Joint Surgery—American Volume, 93A, 1510–1518.
Vincken, P. W., Ter Braak, B. P., van Erkel, A. R., Coerkamp, E. G., Mallens, W. M., & Bloem, J. L. (2006). Clinical consequences of bone bruise around the knee. European Radiology, 16, 97–107.
Batty, L. M., Murgier, J., Feller, J. A., O’Sullivan, R., Webster, K. E., & Devitt, B. M. (2020). radiological identification of injury to the Kaplan fibers of the iliotibial band in association with anterior cruciate ligament injury. The American Journal of Sports Medicine, 48, 2213–2220.
Lee, D. W., Lee, J. H., Kim, J. N., et al. (2018). Evaluation of anterolateral ligament injuries and concomitant lesions on magnetic resonance imaging after acute anterior cruciate ligament rupture. Arthroscopy—The Journal of Arthroscopic and Related Surgery, 34, 2398–2406.
Aravindh, P., Wu, T., Chan, C. X., Wong, K. L., & Krishna, L. (2018). Association of compartmental bone bruise distribution with concomitant intra-articular and extra-articular injuries in acute anterior cruciate ligament tears after noncontact sports trauma. Orthopaedic Journal of Sports Medicine. https://doi.org/10.1177/2325967118767625
Balendra, G., Willinger, L., Pai, V., et al. (2021). Anterolateral complex injuries occur in the majority of “isolated” anterior cruciate ligament ruptures. Knee Surgery, Sports Traumatology, Arthroscopy Official Journal of the ESSKA, 30, 176–183.
Marot, V., Corin, B., Reina, N., Murgier, J., Berard, E., & Cavaignac, E. (2021). Femoral and tibial bone bruise volume is not correlated with ALL injury or rotational instability in patients with ACL-deficient knee. Knee Surgery Sports Traumatology Arthroscopy, 29, 900–906.
Slim, K., Nini, E., Forestier, D., Kwiatkowski, F., Panis, Y., & Chipponi, J. (2003). Methodological index for non-randomized studies (minors): Development and validation of a new instrument. ANZ Journal of Surgery, 73, 712–716.
Ekhtiari, S., Horner, N. S., Bedi, A., Ayeni, O. R., & Khan, M. (2018). The learning curve for the Latarjet procedure: A systematic review. Orthopaedic Journal of Sports Medicine, 6, 2325967118786930.
Dimitriou, D., Reimond, M., Foesel, A., et al. (2021). The deep lateral femoral notch sign: A reliable diagnostic tool in identifying a concomitant anterior cruciate and anterolateral ligament injury. Knee Surgery, Sports Traumatology, Arthroscopy: Official Journal of the ESSKA, 29, 1968–1976.
Ferretti, A., Monaco, E., Redler, A., et al. (2019). High prevalence of anterolateral ligament abnormalities on MRI in knees with acute anterior cruciate ligament injuries. Orthopaedic Journal of Sports Medicine. https://doi.org/10.1177/2325967119852916
Helito, C. P., Partezani Helito, P. V., Leao, R. V., Demange, M. K., & Bordalo-Rodrigues, M. (2017). Anterolateral ligament abnormalities are associated with peripheral ligament and osseous injuries in acute ruptures of the anterior cruciate ligament. Knee Surgery Sports Traumatology Arthroscopy, 25, 1140–1148.
Helito, C. P., Partezani Helito, P. V., Boulitreau Assirati, L. F., Longo, C. H., Bordalo-Rodrigues, M., & de Souza, F. F. (2019). Magnetic resonance imaging evaluation of the anterolateral ligament in acute anterior cruciate ligament injuries in an adolescent population. Arthroscopy—The Journal of Arthroscopic and Related Surgery, 35, 2136–2142.
Li, K., Li, J., Zheng, X., et al. (2020). Increased lateral meniscal slope is associated with greater incidence of lateral bone contusions in noncontact ACL injury. Knee Surgery Sports Traumatology Arthroscopy., 28, 2000–2008.
Shekari, I., Shekarchi, B., Abbasian, M., Sajjadi, M. M., Moghaddam, A. M., & Kazemi, S. M. (2020). Predictive factors associated with anterolateral ligament injury in the patients with anterior cruciate ligament tear. Indian Journal of Orthopaedics, 54, 655–664.
Song, G.-Y., Zhang, H., Wang, Q.-Q., Zhang, J., Li, Y., & Feng, H. (2016). Bone contusions after acute noncontact anterior cruciate ligament injury are associated with knee joint laxity, concomitant meniscal lesions, and anterolateral ligament abnormality. Arthroscopy—The Journal of Arthroscopic and Related Surgery., 32, 2331–2341.
Song, Y., Yang, J.-H., Choi, W. R., & Lee, J. K. (2019). Magnetic resonance imaging-based prevalence of anterolateral ligament abnormalities and associated injuries in knees with acute anterior cruciate ligament injury. Journal of Knee Surgery, 32, 866–871.
Van Dyck, P., Clockaerts, S., Vanhoenacker, F. M., et al. (2016). Anterolateral ligament abnormalities in patients with acute anterior cruciate ligament rupture are associated with lateral meniscal and osseous injuries. European Radiology, 26, 3383–3391.
Bernholt, D. L., DePhillipo, N. N., Crawford, M. D., Aman, Z. S., Grantham, W. J., & LaPrade, R. F. (2020). Incidence of displaced posterolateral tibial plateau and lateral femoral condyle impaction fractures in the setting of primary anterior cruciate ligament tear. American Journal of Sports Medicine, 48, 545–553.
Korthaus, A., Warncke, M., Pagenstert, G., Krause, M., Frosch, K.-H., & Kolb, J. P. (2021). Lateral femoral notch sign and posterolateral tibial plateau fractures and their associated injuries in the setting of an anterior cruciate ligament rupture. Archives of Orthopaedic and Trauma Surgery, 142, 1605–1612.
Willinger, L., Balendra, G., Pai, V., et al. (2021). High incidence of superficial and deep medial collateral ligament injuries in “isolated” anterior cruciate ligament ruptures: a long overlooked injury. Knee Surgery, Sports Traumatology, Arthroscopy: Official Journal of the ESSKA, 30, 167–175.
Berthold, D. P., Willinger, L., LeVasseur, M. R., et al. (2021). High rate of initially overlooked Kaplan fiber complex injuries in patients with isolated anterior cruciate ligament injury. The American Journal of Sports Medicine, 49, 2117–2124.
Ward, P., Chang, P., Radtke, L., & Brophy, R. H. (2021). Clinical implications of bone bruise patterns accompanying anterior cruciate ligament tears. Sports Health, 14, 595–591.
Goncharov, E. N., Koval, O. A., Bezuglov, E. N., & Goncharov, N. G. (2018). Anatomical features and significance of the anterolateral ligament of the knee. International Orthopaedics, 42, 2859–2864.
Runer, A., Birkmaier, S., Pamminger, M., et al. (2016). The anterolateral ligament of the knee: A dissection study. The Knee, 23, 8–12.
Blanke, F., Boljen, M., Lutter, C., Oehler, N., Tischer, T., & Vogt, S. (2021). Does the anterolateral ligament protect the anterior cruciate ligament in the most common injury mechanisms? A Human knee model study. The Knee, 29, 381–389.
Lee, D. W., Kim, J. G., Kim, H. T., & Cho, S. I. (2020). Evaluation of anterolateral ligament healing after anatomic anterior cruciate ligament reconstruction. The American Journal of Sports Medicine, 48, 1078–1087.
Oh, Y. K., Lipps, D. B., Ashton-Miller, J. A., & Wojtys, E. M. (2012). What strains the anterior cruciate ligament during a pivot landing? The American Journal of Sports Medicine, 40, 574–583.
Song, G. Y., Zhang, H., Wang, Q. Q., Zhang, J., Li, Y., & Feng, H. (2016). Risk factors associated with grade 3 pivot shift after acute anterior cruciate ligament injuries. The American Journal of Sports Medicine, 44, 362–369.
Inderhaug, E., Stephen, J. M., Williams, A., & Amis, A. A. (2017). Biomechanical comparison of anterolateral procedures combined with anterior cruciate ligament reconstruction. The American Journal of Sports Medicine, 45, 347–354.
Rasmussen, M. T., Nitri, M., Williams, B. T., et al. (2016). An in vitro robotic assessment of the anterolateral ligament, part 1: Secondary role of the anterolateral ligament in the setting of an anterior cruciate ligament injury. The American Journal of Sports Medicine, 44, 585–592.
Nitri, M., Rasmussen, M. T., Williams, B. T., et al. (2016). An in vitro robotic assessment of the anterolateral ligament, part 2: Anterolateral ligament reconstruction combined with anterior cruciate ligament reconstruction. The American Journal of Sports Medicine, 44, 593–601.
Musahl, V., Rahnemai-Azar, A. A., Costello, J., et al. (2016). The influence of meniscal and anterolateral capsular injury on knee laxity in patients with anterior cruciate ligament injuries. The American Journal of Sports Medicine, 44, 3126–3131.
Devitt, B. M., O’Sullivan, R., Feller, J. A., et al. (2017). MRI is not reliable in diagnosing of concomitant anterolateral ligament and anterior cruciate ligament injuries of the knee. Knee Surgery, Sports Traumatology, Arthroscopy: Official Journal of the ESSKA, 25, 1345–1351.
Young, B. L., Ruder, J. A., Trofa, D. P., & Fleischli, J. E. (2020). Visualization of concurrent anterolateral and anterior cruciate ligament injury on magnetic resonance imaging. Arthroscopy, 36, 1086–1091.
Puzzitiello, R. N., Agarwalla, A., Zuke, W. A., Garcia, G. H., & Forsythe, B. (2018). Imaging diagnosis of injury to the anterolateral ligament in patients with anterior cruciate ligaments: Association of anterolateral ligament injury with other types of knee pathology and grade of pivot-shift examination: a systematic review. Arthroscopy, 34, 2728–2738.
Han, A. X., Tan, T. J., Nguyen, T., & Lee, D. Y. H. (2020). Timing of magnetic resonance imaging affects the accuracy and interobserver agreement of anterolateral ligament tears detection in anterior cruciate ligament deficient knees. Knee Surgery & Related Research, 32, 64.
Andrews, K., Lu, A., McKean, L., & Ebraheim, N. (2017). Review: Medial collateral ligament injuries. Journal of Orthopaedics, 14, 550–554.
Zhang, H., Sun, Y., Han, X., et al. (2014). Simultaneous reconstruction of the anterior cruciate ligament and medial collateral ligament in patients with chronic ACL-MCL lesions: A minimum 2-year follow-up study. The American Journal of Sports Medicine, 42, 1675–1681.
Svantesson, E., Hamrin Senorski, E., Alentorn-Geli, E., et al. (2019). Increased risk of ACL revision with non-surgical treatment of a concomitant medial collateral ligament injury: A study on 19,457 patients from the Swedish National Knee Ligament Registry. Knee Surgery, Sports Traumatology, Arthroscopy: Official Journal of the ESSKA, 27, 2450–2459.
Ball, S., Stephen, J. M., El-Daou, H., Williams, A., & Amis, A. A. (2020). The medial ligaments and the ACL restrain anteromedial laxity of the knee. Knee Surgery, Sports Traumatology, Arthroscopy: Official Journal of the ESSKA, 28, 3700–3708.
Bollier, M., & Smith, P. A. (2014). Anterior cruciate ligament and medial collateral ligament injuries. The Journal of Knee Surgery, 27, 359–368.
Sugita, T., & Amis, A. A. (2001). Anatomic and biomechanical study of the lateral collateral and popliteofibular ligaments. The American Journal of Sports Medicine, 29, 466–472.
Murphy, B. J., Smith, R. L., Uribe, J. W., Janecki, C. J., Hechtman, K. S., & Mangasarian, R. A. (1992). Bone signal abnormalities in the posterolateral tibia and lateral femoral condyle in complete tears of the anterior cruciate ligament: A specific sign? Radiology, 182, 221–224.
Grawe, B., Schroeder, A. J., Kakazu, R., & Messer, M. S. (2018). Lateral collateral ligament injury about the knee: Anatomy, evaluation, and management. The Journal of the American Academy of Orthopaedic Surgeons., 26, e120–e127.
Bonadio, M. B., Helito, C. P., Gury, L. A., Demange, M. K., Pécora, J. R., & Angelini, F. J. (2014). Correlation between magnetic resonance imaging and physical exam in assessment of injuries to posterolateral corner of the knee. Acta Ortopedica Brasileira, 22, 124–126.
Van Dyck, P., De Smet, E., Roelant, E., Parizel, P. M., & Heusdens, C. H. W. (2019). Assessment of anterolateral complex injuries by magnetic resonance imaging in patients with acute rupture of the anterior cruciate ligament. Arthroscopy, 35, 521–527.
Geeslin, A. G., Chahla, J., Moatshe, G., et al. (2018). Anterolateral knee extra-articular stabilizers: a robotic sectioning study of the anterolateral ligament and distal iliotibial band Kaplan fibers. The American Journal of Sports Medicine, 46, 1352–1361.
Batty, L., Murgier, J., O’Sullivan, R., Webster, K. E., Feller, J. A., & Devitt, B. M. (2019). The Kaplan fibers of the iliotibial band can be identified on routine knee magnetic resonance imaging. The American journal of sports medicine., 47, 2895–2903.
Acknowledgements
The authors would like to acknowledge the help of Wenjia Du in writing the discussion part by giving beneficial suggestions.
Funding
The National Natural Science Foundation of China (81874017, 81960403, and 82060405); Lanzhou Science and Technology Plan Program (20JR5RA320); Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02, CY2021-MS-A07).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any conflicts to report.
Ethical approval
As a systematic review, ethical approval was not appropriate for this work.
Informed consent
For this type of study, informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yi, Z., Jiang, J., Liu, Z. et al. The Association Between Bone Bruises and Concomitant Ligaments Injuries in Anterior Cruciate Ligament Injuries: A Systematic Review and Meta-analysis. JOIO 57, 20–32 (2023). https://doi.org/10.1007/s43465-022-00774-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-022-00774-6