Abstract
Purpose
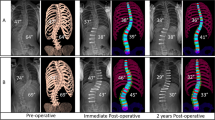
Anterior Vertebral Body Tethering (AVBT), a fusionless surgical technique based on growth modulation, aims to correct pediatric scoliosis over time. However, medium-term curvature changes of the non-instrumented distal lumbar curve remains difficult to predict. The objective was to biomechanically analyze the level below the LIV to evaluate whether adding-on or compensatory lumbar curve after AVBT can be predicted by intervertebral disc (ID) wedging and force asymmetry.
Methods
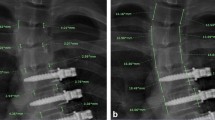
33 retrospective scoliotic cases instrumented with AVBT were used to computationally simulate their surgery and 2-year post-operative growth modulation using a finite element model. The cohort was divided into two subgroups according to the lumbar curvature evolution over 2 years: (1) correction > 10° (C); (2) maintaining ± 10° (M). The lumbar Cobb angle and residual ID wedging angle under LIV were measured. Simulated pressures and moments at the superior endplate of LIV + 1 were post-processed. These parameters were correlated at 2 years postoperatively.
Findings
On average, the LIV + 1 simulated moment was 538 Nmm for subgroup C, 155 Nmm for subgroup M with lumbar Cobb angle > 20° and 34 Nmm for angle < 20° whereas the ID angle was 1° for C and 0° for M.
Interpretation
On average, a positive moment on the LIV + 1 superior growth plate led to correction of the lumbar curvature, whereas a null moment kept it stable, and a parallel immediate postoperative ID under LIV contributed to its correction or preservation. Nevertheless, the significant interindividual variability suggested that other parameters are involved in the distal non-instrumented curvature evolution.
Level of evidence
IV





Similar content being viewed by others
References
Aronsson DD, Stokes IA (2011) Nonfusion treatment of adolescent idiopathic scoliosis by growth modulation and remodeling. J Pediatr Orthop 31(1 Suppl):S99-106
Samdani AF, Ames RJ, Kimball JS et al (2014) Anterior vertebral body tethering for idiopathic scoliosis: two-year results. Spine (Phila Pa 1976) 39(20):1688–1693
Matsumoto M, Watanabe K, Hosogane N et al (2014) Updates on surgical treatments for pediatric scoliosis. J Orthop Sci 19(1):6–14
Skaggs DL, Akbarnia BA, Flynn JM et al (2014) A classification of growth friendly spine implants. J Pediatr Orthop 34(3):260–274
Stokes IA (2007) Analysis and simulation of progressive adolescent scoliosis by biomechanical growth modulation. Eur Spine J 16(10):1621–1628
Stokes IAF, Aronsson DD, Dimock AN et al (2006) Endochondral growth plates of three species at two anatomical locations modulated by mechanical compression and tension. J Orthop Res 24(6):1327–1334
Samdani AF, Ames RJ, Kimball JS et al (2015) Anterior vertebral body thetering for idiopathic scoliosis : one-year results on the first 32 patients. E Spine J 24:1533–1539
Cobetto N, Aubin CE, Parent S (2018) Surgical planning and follow-up of anterior vertebral body growth modulation in pediatric idiopathic scoliosis using a patient-specific finite element model integrating growth modulation. Spine Deform 6(4):344–350
Cobetto N, Aubin CE, Parent S (2020) Anterior vertebral body growth modulation: assessment of the 2-year predictive capability of a patient-specific finite-element planning tool and of the growth modulation biomechanics. Spine 45(18):E1203–E1209
Murray E, Tung R, Sherman A et al (2020) Continued vertebral body growth in patients with juvenile idiopathic scoliosis following vertebral body stapling. Spine Deform 8(2):221–226
Baker C, Mildbrandt T, Potter D et al (2020) Anterior lumbar vertebral body tethering in adolescent idiopathic scoliosis: Surgical/Technical Tips. JPOSNA 2(3). Retrieved from https://www.jposna.org/index.php/jposna/article/view/145
Newton PO (2020) Spinal growth tethering: indications and limits. Ann Transl Med 8(2):27
Stokes IA (2002) Mechanical effects on skeletal growth. J Muskuloskelet Neuronal Interact 2:327–335
Samdani AF, Pahys JM, Ames RJ et al (2021) Prospective follow-up report on anterior vertebral body tethering for idiopathic scoliosis: interim results from an FDA IDE study. J Bone Joint Surg Am 103(17):1611–1619
Cobetto N, Parent S, Aubin CE (2018) 3D correction over 2years with anterior vertebral body growth modulation: a finite element analysis of screw positioning, cable tensioning and postoperative functional activities. Clin Biomech (Bristol, Avon) 51:26–33
Villemure I, Aubin CE, Dansereau J et al (2002) Simulation of progressive deformities in adolescent idiopathic scoliosis using a biomechanical model integrating vertebral growth modulation. J Biomech Eng 124(6):784–790
Villemure I, Stokes IA (2009) Growth plate mechanics and mechanobiology. A survey of present understanding. J Biomech 42(12):1793–1803
Chazal J (1985) Biomechanical properties of spinal ligaments and a histological study of the supraspinal ligament in traction. J Biomech 18(3):167–176
Panjabi M (1976) Three-dimensional flexibility and stiffness properties of the human thoracic spine. J Biomech 9(4):185–192
Pezowicz C, Głowacki M (2012) The mechanical properties of human ribs in young adult. Acta Bioeng Biomech 14(2):53–60
Petit Y, Aubin CE, Labelle H (2002) Relation between patient positioning, trunk flexibility and surgical correction of the scoliotic spine. In: Tanguy A, Peuchot B (eds) Research into spinal deformities 3. IOS press, Amsterdam, pp. 400–403. no. 0926–9630 (Print)
Clin J, Aubin CE, Lalonde N et al (2011) A new method to include the gravitational forces in a finite element model of the scoliotic spine. Med Biol Eng Comput 49(8):967–977
Samdani AF, Pahys J, Samuel S et al (2021) “Unsuccessful vertebral body tethering : incidence and predictive factors” presented at the SRS 56th Annual Meeting, Saint-Louis, Missouri.
Kwan KY, Yuk Kwan Tang C, Parent S et al (2021) “Does LIV selection affect radiographic outcomes in vertebral body tethering? analysis of a prospective case series of 102 patients from the PSSG database” presented at the SRS 56th Annual Meeting, Saint-Louis, Missouri.
Acknowledgements
The data for this study came from an institutional database of cases operated on by Dr. Stefan Parent MD, PhD. whom we would like to thank for his contribution to the studies that preceded the current one.
Funding
This research was undertaken thanks, in part, to funding from the Canada First Research Excellence Fund through the TransMedTech Institute and the Natural Sciences and Engineering Research Council of Canada (Industrial Research Chair program with Medtronic of Canada).
Author information
Authors and Affiliations
Contributions
CR: design, acquisition, analysis, interpretation of data for the work, drafting, final approbation, agree to be accountable. NC: analysis, interpretation of the data for the work, revising, final approbation, agree to be accountable. NL: interpretation of the data for the work, revising, final approbation, agree to be accountable. CEA: interpretation of the data for the work, drafting and revising, final approbation, agree to be accountable.
Corresponding author
Ethics declarations
Conflict of interest
Natural Sciences and Engineering Research Council of Canada (industrial research chair program with Medtronic of Canada). Outside of the current work: contracts with Medtronic.
Ethical approval
Approval was obtained from both the ethics committee of Polytechnique Montreal and the Sainte-Justine University Hospital Center. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Raballand, C., Cobetto, N., Larson, A. et al. Prediction of post-operative adding-on or compensatory lumbar curve correction after anterior vertebral body tethering. Spine Deform 11, 27–33 (2023). https://doi.org/10.1007/s43390-022-00558-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-022-00558-w