Abstract
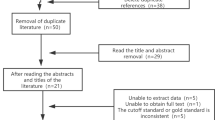
Obstructive Sleep Apnea (OSA) corresponds to episodes of complete or partial upper airway obstruction during sleep. The gold standard for diagnosing OSA is polysomnography; however, metabolomics is an innovative and highly sensitive method that seeks to identify and quantify small molecules in biological systems. Identify the metabolites most frequently associated with obstructive sleep apnea in adults. The search for articles was conducted between October 2020 and August 2021, in electronic databases, such as MEDLINE/PubMed, Scielo, Embase, and Cochrane, through the combination of descriptors: obstructive sleep apnea, metabolomic, adult. This systematic review included all cross-sectional studies published, including human patients aged 18 years or older, of both genders who underwent type I or II polysomnography and metabolomics study. The search strategy selected 3697 surveys, and 4 of them were selected to be a part of this systematic review. Based on the analyzed surveys, it was found that all of them were able to diagnose OSA, reaching a sensitivity of 75–97%, and specificity that ranged from 72 to 100%; besides differentiating patients with OSA (severe, moderate, and mild) from simple snorers with a mean sensitivity of 77.2% and specificity of 66.25%. These findings suggest that, in addition to being used as a screening and diagnostic strategy for OSA, metabolomics has the potential to be used for severity stratification and to monitor the disease's progression.





Similar content being viewed by others
Change history
13 July 2023
A Correction to this paper has been published: https://doi.org/10.1007/s41105-023-00475-z
References
American Academy of Sleep Medicine. International Classification of Sleep Disorders: Diagnostic and Coding Manual. 2005;
Benjafield AV, Ayas NT, Eastwood PR, Heinzer R, Ip MSM, Morrell MJ, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687–98.
Tufik S, Santos-Silva R, Taddei JA, Bittencourt LRA. Obstructive sleep apnea syndrome in the sao paulo epidemiologic sleep study. Sleep Med. 2010;11(5):441–6. https://doi.org/10.1016/j.sleep.2009.10.005.
Kapur V, Blough DK, Sandblom RE, Hert R, De Maine JB, Sullivan SD, et al. The medical cost of undiagnosed sleep apnea. Sleep. 1999;22(6):749–55.
Kryger MH, Roos L, Delaive K, Walld R, Horrocks J. Utilization of health care services in patients with severe obstructive sleep apnea. Sleep. 1996;19(9 SUPPL):S111–6.
Kuczyński W, Kudrycka A, Małolepsza A, Karwowska U, Białasiewicz P, Białas A. The epidemiology of obstructive sleep apnea in poland—polysomnography and positive airway pressure therapy. Int J Environ Res Public Health. 2021;18(4):1–7.
Zancanella E. Monitorização domiciliar do sono: Uma criteriosa opção! Braz J Otorhinolaryngol. 2013;79(3):266. https://doi.org/10.5935/1808-8694.20130049.
Fabbri M, Beracci A, Martoni M, Meneo D, Tonetti L, Natale V. Measuring subjective sleep quality: a review. Int J Environ Res Public Health. 2021;18(3):1–57.
Walker DI, Valvi D, Rothman N, Lan Q, Miller GW, Jones DP. The metabolome: A key measure for exposome research in epidemiology. Curr Epidemiol Rep. 2019;6:93–103 (Epub 2019 Apr 26. PMID: 31828002; PMCID: PMC6905435).
Xie G, Zhang S, Zheng X, Jia W. Metabolomics approaches for characterizing metabolic interactions between host and its commensal microbes. Electrophoresis. 2013;34:1–46.
Martin FP, Ezri J, Cominetti O, Da Silva L, Kussmann M, Godin JP, et al. Urinary metabolic phenotyping reveals differences in the metabolic status of healthy and inflammatory bowel disease (IBD) children in relation to growth and disease activity. Int J Mol Sci. 2016;17(8):1–15.
Dawiskiba T, Deja S, Mulak A, Zabek A, Jawień E, Pawełka D, et al. Serum and urine metabolomic fngerprinting in diagnostics of inflammatory bowel diseases. World J Gastroenterol. 2014;20(1):163–74.
Silva RA, Pereira TCS, Souza AR, Ribeiro PR. 1H NMR-based metabolite profiling for biomarker identification. Clin Chim Acta. 2020;502:269–79. https://doi.org/10.1016/j.cca.2019.11.015.
Xu H, Zheng X, Jia W, Yin S. Chromatogaphy/mass spectrometry-based biomarkers in the field of obstructive sleep apnea. Med (United States). 2015;94(40):1–9.
American Academy of Sleep Medicine. International classification of sleep disorders, 3rd edn. 2014;475–84.
Raby BA. Personalized medicine. Vestn Ross Akad Meditsinskikh Nauk. 2019;74(1):61–70.
Lebkuchen A, Carvalho VM, Venturini G, Salgueiro JS, Freitas LS, Dellavance A, et al. Metabolomic and lipidomic profile in men with obstructive sleep apnoea: implications for diagnosis and biomarkers of cardiovascular risk. Sci Rep. 2018;8(1):1–12.
Cho K, Yoon DW, Lee M, So D, Hong IH, Rhee CS, et al. Urinary metabolomic signatures in obstructive sleep apnea through targeted metabolomic analysis: a pilot study. Metabolomics. 2017;13(8):0.
Xu H, Zheng X, Qian Y, Guan J, Yi H, Zou J, et al. Metabolomics profiling for obstructive sleep apnea and simple snorers. Sci Rep. 2016;6:1–9. https://doi.org/10.1038/srep30958.
Ferrarini A, Ruperez FJ, Erazo M, Martinez MP, Villar-Álvarez F, Peces-Barba G, et al. Fingerprinting based metabolomic approach with LC-MS to sleep apnea and hypopnea sindrome: a pilot study. Electrophoresis. 2013;34:2873–81.
Humer E, Pieh C, Brandmayr G. Metabolomics in sleep, insomnia and sleep apnea. Int J Mol Sci. 2020;21(19):1–17.
Finamore P, Scarlata S, Cardaci V, Incalzi RA. Exhaled breath analysis in obstructive sleep apnea syndrome: a review of the literature. Med. 2019;55(9):538.
Kawai M, Kirkness JP, Yamamura S, Imaizumi K, Yoshimine H, Oi K, et al. Increased phosphatidylcholine concentration in saliva reduces surface tension and improves airway patency in obstructive sleep apnoea. J Oral Rehabil. 2013;40(10):758–66.
Engeli S, Blüher M, Jumpertz R, Wiesner T, Wirtz H, Bosse-Henck A, et al. Circulating anandamide and blood pressure in patients with obstructive sleep apnea. J Hypertens. 2012;30(12):2345–51.
Redline S, Strohl KP. Recognition and consequences of obstructive sleep apnea hypopnea syndrome. Otolaryngol Clin North Am. 1999;32(2):303–31.
George CFP. Diagnostic techniques in obstructive sleep apnea. Prog Cardiovasc Dis. 1999;41(5):355–66.
Qiu Q, Mateika JH. Pathophysiology of obstructive sleep apnea in aging women. Curr Sleep Med Rep. 2021;7:177–85.
Stewart SA, Penz E, Fenton M, Skomro R. Investigating cost implications of incorporating level III at-home testing into a polysomnography based sleep medicine program using administrative data. Can Respir J. 2017;2017:1–7.
Konecny T, Kara T, Somers VK. Obstructive sleep apnea and hypertension: An update. Hypertension. 2014;63(2):203–9.
Bouloukaki I, Grote L, McNicholas WT, Hedner J, Verbraecken J, Parati G, et al. Mild obstructive sleep apnea increases hypertension risk, challenging traditional severity classification. J Clin Sleep Med. 2020;16(6):889–98.
Mills PJ, Dimsdale JE. Sleep apnea: A model for studying cytokines, sleep, and sleep disruption. Brain Behav Immun. 2004;18(4):298–303.
Qu D, Liu J, Lau CW, Huang Y. IL-6 in diabetes and cardiovascular complications. Br J Pharmacol. 2014;171(15):3595–603.
Chiu HY, Chen PY, Chuang LP, Chen NH, Tu YK, Hsieh YJ, et al. Diagnostic accuracy of the Berlin questionnaire, STOP-BANG, STOP, and Epworth sleepiness scale in detecting obstructive sleep apnea: a bivariate meta-analysis. Sleep Med Rev. 2017;36:57–70. https://doi.org/10.1016/j.smrv.2016.10.004.
Amra B, Javani M, Soltaninejad F, Penzel T, Fietze I, Schoebel C, Farajzadegan Z. Comparison of berlin questionnaire, STOP-bang, and epworth sleepiness scale for diagnosing obstructive sleep apnea in persian patients. Int J Prev Med. 2018;9(9):28. https://doi.org/10.4103/ijpvm.IJPVM_131_17.PMID:29619152;PMCID:PMC5869953.
American Psychiatric Association. Manual diagnóstico e estatístico de transtornos mentais [recurso eletrônico] : DSM-5. 2014.
Porto F, Sakamoto YS, Salles C. Association between obstructive sleep apnea and myocardial infarction: A systematic review. Arq Bras Cardiol. 2017;108(4):361–9.
Jaiswal S, Owens R, Malhotra A. Raising awareness about sleep disorders. Lung India. 2017;34(3):262–8.
Lechner M, Breeze CE, Ohayon MM, Kotecha B. Snoring and breathing pauses during sleep: interview survey of a United Kingdom population sample reveals a significant increase in the rates of sleep apnoea and obesity over the last 20 years - data from the UK sleep survey. Sleep Med. 2019;54:250–6. https://doi.org/10.1016/j.sleep.2018.08.029.
Funding
This survey is funded by Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) under Grant No. 126739/2020-0.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised to update the conflict of interest statement.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Salles, C., Freitas, M.C., Souza, A. et al. Metabolomic approach for obstructive sleep apnea in adults: a systematic review. Sleep Biol. Rhythms 21, 265–277 (2023). https://doi.org/10.1007/s41105-023-00445-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41105-023-00445-5