Abstract
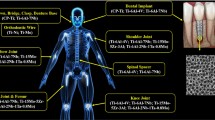
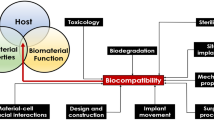
Porosity is a feature that can be designed into 3D printed parts, notably surgical implants, and porosity is associated with improved biocompatibility and osseointegration. It is imperative to evaluate the electrochemical behavior of 3D printed-porous Ti to identify the optimum porosity with low corrosion kinetics for biomedical applications. The objective of this study was to evaluate the corrosion kinetics, mechanical properties, and biocompatibility of 3D printed porous Titanium alloy metal. 3D printed porous Ti samples of 11 mm diameter and 7 mm thick with five porosity levels (0%, 20%, 40%, 60%, and 80%) were manufactured, mechanically tested, studied for characterization and Electrochemical behavior. The cell proliferations was also conducted on different groups for the examination of their biocompatibility, which might indicate the influence of porosity to the cellular activities. The results showed that increasing porosity corresponds with decreasing mechanical strength and increasing corrosion characteristics. Corrosion current, Icorr values ranged from 10−7 to 10−4 A, and Ecorr values ranged from + 100 to − 600 mV for all five porosity-level samples. Analysis of EIS data indicated that capacitance values ranged from 0.00025 to 0.0015F. In addition, sample porosity showed evidence of other corrosion forms such as crevice corrosion and intergranular corrosion. The results of cell proliferations demonstrated all groups of specimens are biocompatible and the ones with 0% and 40% porosity exhibited the highest increments of cells, implying their potential in biomedical application. The study revealed that 3D printed Ti samples with larger porosity were subjected to increased electrochemical corrosion. A porosity between 40 and 60% 3D printed porous Ti study sample was found optimum for the biomedical application. The development of future biomedical devices will have to maintain a balanced approach between the osseointegration of large porosities and increased corrosion tendencies to optimize safer devices through additive manufacturing or 3D printing for better patient outcomes. Further studies will evaluate 3D-printed tribocorrosion properties and biocompatibility via osteoblast culture.











Similar content being viewed by others
References
Jones CA, Beaupre LA, Johnston DWC, Suarez-Almazor M (2007) Total joint arthroplasties: current concepts of patient outcomes after surgery. Rheum Dis Clin N Am 33:71–86
Harding P, Holland AE, Delany C, Hinman RS (2014) Do activity levels increase after total hip and knee arthroplasty? Clin Orthop 472:1502–1511
Fitzgerald JD et al (2004) Patient quality of life during the 12 months following joint replacement surgery. Arthritis Care Res 51:100–109
Okazak Y, Nishimura E, Nakada H, Kobayashi K (2001) Surface analysis of Ti-15Zr-4Nb-4Ta alloy after implantation in rat tibia. Biomaterials 22:599–607
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Jt Surg Am 89:780–785
Iamthanaporn K, Chareancholvanich K, Pornrattanamaneewong C (2015) Revision primary total hip replacement: causes and risk factors. J Med Assoc Thail Chotmaihet Thangphaet 98:93–99
Hallab NJ, Cunningham BW, Jacobs JJ (2003) Spinal implant debris-induced osteolysis. Spine 28:S125
Mahomed NN et al (2003) Rates and outcomes of primary and revision total hip replacement in the United States medicare population. J. Bone Jt Surg Am 85A:27–32
Zeng L, Xiang N, Wei B (2014) A comparison of corrosion resistance of cobalt-chromium-molybdenum metal ceramic alloy fabricated with selective laser melting and traditional processing. J Prosthet Dent 112:1217–1224
Heinl P, Körner C, Singer RF (2008) Selective electron beam melting of cellular titanium: mechanical properties. Adv Eng Mater 10:882–888
ScienceDirect (2019) Mechanical evaluation of porous titanium (Ti6Al4V) structures with electron beam melting (EBM). https://www.sciencedirect.com/science/article/pii/S1751616109001210?via%3Dihub
Murr LE et al (2009) Microstructure and mechanical behavior of Ti–6Al–4V produced by rapid-layer manufacturing, for biomedical applications. J Mech Behav Biomed Mater 2:20–32
Banks J (2013) Adding value in additive mafnufacturing: researchers in the United Kingdom and Europe look to 3D printing for customization. IEEE Pulse 4:22–26
Klein GT, Lu Y, Wang MY (2013) 3D printing and neurosurgery—ready for prime time? World Neurosurg 80:233–235
Gross BC, Erkal JL, Lockwood SY, Chen C, Spence DM (2014) Evaluation of 3D printing and its potential impact on biotechnology and the chemical sciences. Anal Chem 86:3240–3253
Tuomi JT et al (2017) In vitro cytotoxicity and surface topography evaluation of additive manufacturing titanium implant materials. J Mater Sci Mater Med 28:53
Alvarez K, Nakajima H (2009) Metallic scaffolds for bone regeneration. Materials 2:790–832
Butscher A et al (2011) Structural and material approaches to bone tissue engineering in powder-based three-dimensional printing. Acta Biomater 7:907–920
Asaoka K, Kuwayama N, Okuno O, Miura I (1985) Mechanical properties and biomechanical compatibility of porous titanium for dental implants. J Biomed Mater Res 19:699–713
der Stok JV et al (2013) Selective laser melting-produced porous titanium scaffolds regenerate bone in critical size cortical bone defects. J Orthop Res 31:792–799
Li JP et al (2007) Bone ingrowth in porous titanium implants produced by 3D fiber deposition. Biomaterials 28:2810–2820
Cheng A, Cohen DJ, Boyan BD, Schwartz Z (2016) Laser-sintered constructs with bio-inspired porosity and surface micro/nano-roughness enhance mesenchymal stem cell differentiation and matrix mineralization in vitro. Calcif Tissue Int 99:625–637
Zhu W et al (2017) 3D-printed porous titanium changed femoral head repair growth patterns: osteogenesis and vascularisation in porous titanium. J Mater Sci Mater Med 28:62
ScienceDirect (2019) Manufacture, characterisation and application of cellular metals and metal foams. https://www.sciencedirect.com/science/article/pii/S0079642500000025
Learmonth ID, Young C, Rorabeck C (2007) The operation of the century: total hip replacement. Lancet Lond Engl 370:1508–1519
Li Y et al (2015) Improving osteointegration and osteogenesis of three-dimensional porous Ti6Al4V scaffolds by polydopamine-assisted biomimetic hydroxyapatite coating. ACS Appl Mater Interfaces 7:5715–5724
Kumari A, Yadav SK, Yadav SC (2010) Biodegradable polymeric nanoparticles based drug delivery systems. Colloids Surf B Biointerfaces 75:1–18
Keselowsky BG, Wang L, Schwartz Z, Garcia AJ, Boyan BD (2007) Integrin alpha(5) controls osteoblastic proliferation and differentiation responses to titanium substrates presenting different roughness characteristics in a roughness independent manner. J Biomed Mater Res A 80:700–710
Bhattarai SR et al (2008) Novel production method and in-vitro cell compatibility of porous Ti-6Al-4V alloy disk for hard tissue engineering. J Biomed Mater Res A 86A:289–299
Kuromoto NK, Simão RA, Soares GA (2007) Titanium oxide films produced on commercially pure titanium by anodic oxidation with different voltages. Mater Charact 58:114–121
Lautenschlager EP, Monaghan P (1993) Titanium and titanium alloys as dental materials. Int Dent J 43:245–253
Lara Rodriguez L, Sundaram PA, Rosim-Fachini E, Padovani AM, Diffoot-Carlo N (2014) Plasma electrolytic oxidation coatings on γTiAl alloy for potential biomedical applications. J Biomed Mater Res 102:988–1001
Brunette DM, Tengvall P, Textor M, Thomsen P (eds) (2001) Titanium in medicine: material science, surface science, engineering, biological responses and medical applications. Springer, Berlin
Hutmacher DW (2000) Scaffolds in tissue engineering bone and cartilage. Biomaterials 21:2529–2543
Ripamonti U, Reddi AH (1997) Tissue engineering, morphogenesis, and regeneration of the periodontal tissues by bone morphogenetic proteins. Crit Rev Oral Biol Med Off Publ Am Assoc Oral Biol 8:154–163
Long M, Rack HJ (1998) Titanium alloys in total joint replacement—a materials science perspective. Biomaterials 19:1621–1639
Textor M, Sittig C, Frauchiger V, Tosatti S, Brunette DM (2001) Properties and biological significance of natural oxide films on titanium and its alloys. In: Brunette DM, Tengvall P, Textor M, Thomsen P (eds) Titanium in medicine: material science, surface science, engineering, biological responses and medical applications. Springer, Berlin, pp 171–230. https://doi.org/10.1007/978-3-642-56486-4_7
ResearchGate (2005) Thick rutile layer on titanium for tribological applications | Request PDF. https://www.researchgate.net/publication/245133225_Thick_rutile_layer_on_titanium_for_tribological_applicationshttps://doi.org/10.1016/j.triboint.2005.08.004
Arabnejad S et al (2016) High-strength porous biomaterials for bone replacement: A strategy to assess the interplay between cell morphology, mechanical properties, bone ingrowth and manufacturing constraints. Acta Biomater 30:345–356
Tsai P-I, Hsu C-C, Chen S-Y, Wu T-H, Huang C-C (2016) Biomechanical investigation into the structural design of porous additive manufactured cages using numerical and experimental approaches. Comput Biol Med 76:14–23
Dunand DC (2004) Processing of Titanium Foams. Adv Eng Mater 6:369–376
Takemoto M et al (2005) Mechanical properties and osteoconductivity of porous bioactive titanium. Biomaterials 26:6014–6023
Li JP, de Wijn JR, Van Blitterswijk CA, de Groot K (2006) Porous Ti6Al4V scaffold directly fabricating by rapid prototyping: preparation and in vitro experiment. Biomaterials 27:1223–1235
Hollander DA et al (2006) Structural, mechanical and in vitro characterization of individually structured Ti-6Al-4V produced by direct laser forming. Biomaterials 27:955–963
Wehmöller M, Weihe S, Rasche C, Scherer P, Eufinger H (2004) CAD/CAM-prefabricated titanium implants for large skull defects—clinical experience with 166 patients from 1994 to 2000. Int Congr Ser 1268:667–672
St-Pierre J-P, Gauthier M, Lefebvre L-P, Tabrizian M (2005) Three-dimensional growth of differentiating MC3T3-E1 pre-osteoblasts on porous titanium scaffolds. Biomaterials 26:7319–7328
An J, Teoh JEM, Suntornnond R, Chua CK (2015) Design and 3D printing of scaffolds and tissues. Engineering 1:261–268
Bini F, Marinozzi A, Marinozzi F, Patanè F (2002) Microtensile measurements of single trabeculae stiffness in human femur. J Biomech 35:1515–1519
Olivares-Navarrete R et al (2008) Integrin α2β1 plays a critical role in osteoblast response to micron-scale surface structure and surface energy of titanium substrates. Proc Natl Acad Sci U S A 105:15767–15772
Acknowledgements
The authors gratefully acknowledge the ITRI, Taiwan, Blazer Foundation (Rockford), UICOM, Rockford.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest to declare.
Informed Consent
All authors agreed and given consent.
Research Involving Human Participants and/or Animals
This research does not involve human and animal participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Morris, D., Mamidi, S.K., Kamat, S. et al. Mechanical, Electrochemical and Biological Behavior of 3D Printed-Porous Titanium for Biomedical Applications. J Bio Tribo Corros 7, 39 (2021). https://doi.org/10.1007/s40735-020-00457-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40735-020-00457-5