Abstract
Background
As research becomes an increasingly important component of medical education, there is greater emphasis on incorporating programmatic enhancements to the research experience. This study builds a logic model to summarize research program inputs, outputs, and outcomes from research-oriented medical schools across the country, providing a framework that institutions can use to design and improve their medical student research training programs.
Methods
Between November 2021 and February 2022, we administered a survey assessing institutional characteristics, research offerings, curriculum, funding, and student scholarly products to the medical schools ranked 1–50 in research in 2021 by US News and World Report. Results were compiled in the form of a logic model.
Results
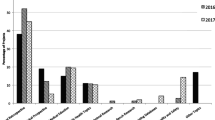
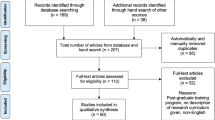
Thirty-seven institutions (72.5%) responded. Common program inputs included personnel such as at least one funded program director (97.3%), while funding for medical student research activities was highly variable (8–72%). There was much less funding for faculty research mentors (2.7%), advisors (18.9%), and teaching faculty (29.7%). Common outputs included a medical student research office or program (97.3%), formal research curricula (83.8%), and services and programs such as research day (91.9%). The most common outcomes tracked were publications (48.6%), presentations/posters (43.2%), student participation (29.7%), and completion of a research requirement (29.7%).
Conclusions
Common themes in medical student research training programs may be conceptualized with a logic model that schools can use to develop, evaluate, and iteratively improve their programs. Institutions should consider their desired program outcomes prior to designing inputs (e.g., funding, personnel) and outputs (e.g., curriculum, training).

Similar content being viewed by others
References
2023 GQ all schools summary report. Association of American Medical Colleges; 2023. Accessed on 30 Dec 2023 https://www.aamc.org/data-reports/students-residents/report/graduation-questionnaire-gq.
2022 GQ all schools summary report. Association of American Medical Colleges; 2022. Accessed on 30 Dec 2023 https://www.aamc.org/data-reports/students-residents/report/graduation-questionnaire-gq.
Liaison Committee on Medical Education. Functions and structure of a medical school 2023–24. Association of American Medical Colleges and American Medical Association; 2022. Accessed 7 Aug 2023 https://lcme.org/publications/.
Toci GR, Elsner JA, Bigelow BF, Bryant BR, LaPorte DM. Medical student research productivity: which variables are associated with matching to a highly ranked orthopaedic residency program? J Surg Educ. 2021;78(2):512–8. https://doi.org/10.1016/j.jsurg.2020.08.024.
Daus K, McEchron M. The impact of medical student research as a discussion topic during the residency interview process. BMC Med Educ. 2021;21(1):556. https://doi.org/10.1186/s12909-021-02989-x.
United States Medical Licensing Examination. USMLE Step 1 transition to pass/fail only score reporting. Federation of State Medical Boards (FSMB) and National Board of Medical Examiners (NBME); 2021. Accessed on 7 Aug 2023 https://www.usmle.org/usmle-step-1-transition-passfail-only-score-reporting.
Raborn LN, Janis JE. Current views on the new United States Medical Licensing Examination Step 1 pass/fail format: a review of the literature. J Surg Res. 2022;274:31–45. https://doi.org/10.1016/j.jss.2022.01.002.
Cluver J, Book S, Brady K, Back S, Thornley N. Engaging medical students in research: reaching out to the next generation of physician-scientists. Acad Psychiatry. 2014;38(3):345–9. https://doi.org/10.1007/s40596-014-0097-8.
Chang Y, Ramnanan CJ. A review of literature on medical students and scholarly research: experiences, attitudes, and outcomes. Acad Med. 2015;90(8):1162–73. https://doi.org/10.1097/acm.0000000000000702.
Cornett M, Palermo C, Wallace MJ, Diug B, Ward B. A realist review of scholarly experiences in medical education. Med Educ. 2021;55(2):159–66. https://doi.org/10.1111/medu.14362.
Karani R, Ognibene FP, Fallar R, Gliatto P. Medical students’ experiences with authorship in biomedical research: a national survey. Acad Med. 2013;88(3):364–8. https://doi.org/10.1097/ACM.0b013e31827fc6ae.
Funston G, Piper RJ, Connell C, Foden P, Young AM, O’Neill P. Medical student perceptions of research and research-orientated careers: an international questionnaire study. Med Teach. 2016;38(10):1041–8. https://doi.org/10.3109/0142159x.2016.1150981.
Morse R, Brooks E, Hines K, Lara-Agudelo D. Methodology: 2023–2024 best medical schools rankings. U.S. News & World Report; 2023. Accessed on 7 Aug 2023 https://www.usnews.com/education/best-graduate-schools/articles/medical-schools-methodology.
Hatry HP, van Houten T, Plantz M, Taylor M. Measuring program outcomes: a practical approach. United Way of America; 1996.
Armstrong EG, Barsion SJ. Using an outcomes-logic-model approach to evaluate a faculty development program for medical educators. Acad Med. 2006;81(5):438–88. https://doi.org/10.1097/01.Acm.0000222259.62890.71.
Giuliani M, Gillan C, Wong O, et al. Evaluation of high-fidelity simulation training in radiation oncology using an outcomes logic model. Radiat Oncol. 2014;9:189. https://doi.org/10.1186/1748-717x-9-189.
Hayes H, Parchman ML, Howard R. A logic model framework for evaluation and planning in a primary care practice-based research network (PBRN). J Am Board Fam Med. 2011;24(5):576–82. https://doi.org/10.3122/jabfm.2011.05.110043.
Möller R, Wallberg A, Shoshan M. Faculty perceptions of factors that indicate successful educational outcomes of medical students’ research projects: a focus group study. BMC Med Educ. 2021;21(1):519. https://doi.org/10.1186/s12909-021-02954-8.
Bierer SB, Chen HC. How to measure success: the impact of scholarly concentrations on students–a literature review. Acad Med. 2010;85(3):438–52. https://doi.org/10.1097/ACM.0b013e3181cccbd4.
Ngaage LM, Elegbede A, McGlone KL, et al. Integrated plastic surgery match: trends in research productivity of successful candidates. Plast Reconstr Surg. 2020;146(1):193–201. https://doi.org/10.1097/prs.0000000000006928.
Kistka HM, Nayeri A, Wang L, Dow J, Chandrasekhar R, Chambless LB. Publication misrepresentation among neurosurgery residency applicants: an increasing problem. J Neurosurg. 2016;124(1):193–8. https://doi.org/10.3171/2014.12.Jns141990.
Rodriguez-Unda NA, Webster ND, Verheyden CN. Trends in academic “ghost publications” in plastic surgery residency applications: a 3-year study. Plast Reconstr Surg Glob Open. 2020;8(1):e2617. https://doi.org/10.1097/gox.0000000000002617.
Collins FS, Tabak LA. Policy: NIH plans to enhance reproducibility. Nature. 2014;505(7485):612–3. https://doi.org/10.1038/505612a.
Breining G. Addressing the research replication crisis. USA: Association of American Medical Colleges; 2017. Accessed on 7 Aug 2023. https://www.aamc.org/news-insights/addressing-research-replication-crisis.
A Barrios-Anderson, E Wu, DD Liu. A survey study examining the motivations, concerns, and perspectives of medical students engaging in neurosurgical research. Surg Neurol Int. 2021;12:490. https://doi.org/10.25259/sni_742_2021.
Mehta K, Sinno S, Thanik V, Weichman K, Janis JE, Patel A. Matching into integrated plastic surgery: the value of research fellowships. Plast Reconstr Surg. 2019;143(2):640–5. https://doi.org/10.1097/prs.0000000000005212.
Cotter EJ, Polce EM, Lee E, et al. Incidence of research gap years in orthopaedic residency applicants: the new standard? J Am Acad Orthop Surg Glob Res Rev. 2021;5(11). https://doi.org/10.5435/JAAOSGlobal-D-21-00247.
Swash M, Lees AJ. Medical conferences: value for money? J Neurol Neurosurg Psychiatry. 2019;90(4):483–4. https://doi.org/10.1136/jnnp-2018-319248.
Ellingson MK, Shi X, Skydel JJ, et al. Publishing at any cost: a cross-sectional study of the amount that medical researchers spend on open access publishing each year. BMJ Open. 2021;11(2):e047107. https://doi.org/10.1136/bmjopen-2020-047107.
Acknowledgements
The authors would like to acknowledge Robert Fallar, PhD, Associate Dean of Assessment and Evaluation and Associate Professor (Medical Education), Icahn School of Medicine at Mount Sinai, for assistance with survey development.
Funding
The authors report there is no funding associated with the work featured in this article
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Feldman, N., Swartz, T.H., Karani, R. et al. An Evidence-Based Framework for Medical Student Research Training. Med.Sci.Educ. 34, 421–428 (2024). https://doi.org/10.1007/s40670-024-02001-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-024-02001-3