Abstract
Background
Effective use of nontechnical skills (NTS) contributes to the provision of safe, quality care in the fast-paced, dynamic setting of the operating room (OR). Inter-professional education of NTS to OR team members can improve performance. Such training requires the accurate measurement of NTS in order to identify gaps in their utilization by OR teams. Although several instruments for measuring OR NTS exist in the literature, each tool tends to define specific NTS differently.
Aim
We aimed to determine commonalities in defined measurements among existing OR NTS tools.
Methods
We undertook a comprehensive literature review of assessment tools for OR NTS to determine the critical components common to these instruments. A PubMed search of the literature from May 2009 to May 2019 combined various combinations of keywords and Medical Subject Headings (MeSH) related to the following subjects: teamwork, teams, assessment, debriefing, surgery, operating room, nontechnical, communication. From this start, articles were selected describing specific instruments. Three reviewers then identified the common components measured among these assessment tools. Reviewers collated kin constructs within each instrument using frequency counts of similarly termed and conceptualized components.
Results
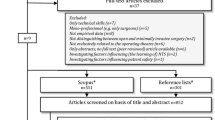
The initial PubMed search produced 119 articles of which 24 articles satisfied the inclusion criteria. Within these articles, 10 assessment tools evaluated OR NTS. Kin constructs were grouped into six NTS categories in the following decreasing frequency order: communication, situation awareness, teamwork, leadership, decision making, and task management/decision making (equal).
Conclusion
NTS OR assessment tools in the literature have a variety of kin constructs related to the specific measured components within the instruments. Such kin constructs contain thematic cohesion across six primary NTS groupings with some variation in scale and scope. Future plans include using this information to develop an easy-to-use assessment tool to assist with debriefing in the clinical environment.



Similar content being viewed by others
References
Hull L, Arora S, Kassab E, Kneebone R, Sevdalis N. Observational teamwork assessment for surgery: content validation and tool refinement. J Am Coll Surg. 2011;212(2):234–243.e1-5.
Mishra A, Catchpole K, McCulloch P. The Oxford NOTECHS System: reliability and validity of a tool for measuring teamwork behaviour in the operating theatre. Qual Saf Health Care. 2009;18(2):104–8.
Spanager L, Beier-Holgersen R, Dieckmann P, Konge L, Rosenberg J, Oestergaard D. Reliable assessment of general surgeons’ non-technical skills based on video-recordings of patient simulated scenarios. Am J Surg. 2013;206(5):810–7.
Mitchell L, Flin R, Yule S, Mitchell J, Coutts K, Youngson G. Development of a behavioural marker system for scrub practitioners’ non-technical skills (SPLINTS system). J Eval Clin Pract. 2013;19(2):317–23.
Gawande AA, Zinner MJ, Studdert DM, Brennan TA. Analysis of errors reported by surgeons at three teaching hospitals. Surgery. 2003;133(6):614–21.
McCulloch P, Mishra A, Handa A, Dale T, Hirst G, Catchpole K. The effects of aviation-style non-technical skills training on technical performance and outcome in the operating theatre. Qual Saf Health Care. 2009;18(2):109–15.
Phitayakorn R, Minehart R, Pian-Smith MC, et al. Practicality of intraoperative teamwork assessments. J Surg Res. 2014;190(1):22–8.
Fischer MM, Tubb CC, Brennan JA, Soderdahl DW, Johnson AE. Implementation of TeamSTEPPS at a Level-1 Military Trauma Center: The San Antonio Military Medical Center Experience. US Army Med Dep J. 2015:75–9.
Lyk-Jensen HT, Jepsen RM, Spanager L, Dieckmann P, Ostergaard D. Assessing Nurse Anaesthetists’ Non-Technical Skills in the operating room. Acta Anaesthesiol Scand. 2014;58(7):794–801.
Nicksa GA, Anderson C, Fidler R, Stewart L. Innovative approach using interprofessional simulation to educate surgical residents in technical and nontechnical skills in high-risk clinical scenarios. JAMA Surg. 2015;150(3):201–7.
Glarner CE, McDonald RJ, Smith AB, et al. Utilizing a novel tool for the comprehensive assessment of resident operative performance. J Surg Educ. 2013;70(6):813–20.
Sharma B, Mishra A, Aggarwal R, Grantcharov TP. Non-technical skills assessment in surgery. Surg Oncol. 2011;20(3):169–77.
Catchpole KR, Dale TJ, Hirst DG, Smith JP, Giddings TA. A multicenter trial of aviation-style training for surgical teams. J Patient Saf. 2010;6(3):180–6.
Rao R, Dumon KR, Neylan CJ, Morris JB, Riddle EW, Sensenig R, et al. Can simulated team tasks be used to improve nontechnical skills in the operating room? J Surg Educ. 2016;73(6):e42-7.
Dedy NJ, Fecso AB, Szasz P, Bonrath EM, Grantcharov TP. Implementation of an effective strategy for teaching nontechnical skills in the operating room: a single-blinded nonrandomized trial. Ann Surg. 2016;263(5):937–41.
Yule S, Parker SH, Wilkinson J, McKinley A, MacDonald J, Neill A, et al. Coaching non-technical skills improves surgical residents’ performance in a simulated operating room. J Surg Educ. 2015;72(6):1124–30.
Pena G, Altree M, Field J, Sainsbury D, Babidge W, Hewett P, et al. Nontechnical skills training for the operating room: A prospective study using simulation and didactic workshop. Surgery. 2015;158(1):300–9.
Beard JD, Marriott J, Purdie H, Crossley J. Assessing the surgical skills of trainees in the operating theatre: a prospective observational study of the methodology. Health Technol Assess. 2011;15(1):i–xxi 1-162.
Spanager L, Konge L, Dieckmann P, Beier-Holgersen R, Rosenberg J, Oestergaard D. Assessing trainee surgeons’ nontechnical skills: five cases are sufficient for reliable assessments. J Surg Educ. 2015;72(1):16–22.
Spanager L, Lyk-Jensen HT, Dieckmann P, Wettergren A, Rosenberg J, Ostergaard D. Customization of a tool to assess Danish surgeons non-technical skills in the operating room. Dan Med J. 2012;59(11):A4526.
Yule S, Paterson-Brown S, Maran N, Rowley D. Development of a rating system for surgeons’ non-technical skills. Med Educ. 2006;40:1098–104.
Nguyen N, Elliott JO, Watson WD, Dominguez E. Simulation improves nontechnical skills performance of residents during the perioperative and intraoperative phases of surgery. J Surg Educ. 2015;72(5):957–63.
Dedy NJ, Szasz P, Louridas M, Bonrath EM, Husslein H, Grantcharov TP. Objective structured assessment of nontechnical skills: Reliability of a global rating scale for the in-training assessment in the operating room. Surgery. 2015;157(6):1002–13.
Gardner AK, Russo MA, Jabbour II, Kosemund M, Scott DJ. Frame-of-reference training for simulation-based intraoperative communication assessment. Am J Surg. 2016;212(3):548–551.e2.
Undre S, Sevdalis N, Healey AN, Darzi S, Vincent CA. Teamwork in the operating theatre: cohesion or confusion? J Eval Clin Pract. 2006;12(2):182–9.
Boet S, Pigford AA, Fitzsimmons A, Reeves S, Triby E, Bould MD. Interprofessional team debriefings with or without an instructor after a simulated crisis scenario: An exploratory case study. J Interprof Care. 2016;30(6):717–25.
Kim J, Neilipovitz D, Cardinal P, Chiu M. A comparison of global rating scale and checklist scores in the validation of an evaluation tool to assess performance in the resuscitation of critically ill patients during simulated emergencies (abbreviated as "CRM simulator study IB"). Simul Healthc. 2009;4(1):6–16.
Kim J, Neilipovitz D, Cardinal P, Chiu M, Clinch J. A pilot study using high-fidelity simulation to formally evaluate performance in the resuscitation of critically ill patients: The University of Ottawa Critical Care Medicine, High-Fidelity Simulation, and Crisis Resource Management I Study. Crit Care Med. 2006;34(8):2167–74.
Flin R, Mitchell L, McLeod B. Non-technical skills of the scrub practitioner: the SPLINTS system. ORNAC J. 2014;32(3):33–8.
Rhee AJ, Valentin-Salgado Y, Eshak D, Feldman D, Kischak P, Reich DL, et al. Team training in the perioperative arena: a methodology for implementation and auditing behavior. Am J Med Qual. 2017;32(4):369–75.
Department of Defense Patient Safety Program, Agency for Healthcare Research and Quality (AHRQ). TeamSTEPPS 2.0 pocket guide: team strategies & tools to enhance performance and patient safety. 2013;AHRQ Pub. No. 14-0001-2 Replaces AHRQ Pub. No. 06-0020-2 Revised December 2013.
Salas E, Sims DE, Burke CS. Is there a big five in teamwork? Small Group Res. 2005;36:555–99.
Robertson ER, Hadi M, Morgan LJ, Pickering SP, Collins G, New S, et al. Oxford NOTECHS II: a modified theatre team non-technical skills scoring system. PLoS One. 2014;9(3):e9e0320.
Salas E. Saving Lives With Teamwork: Guidance From Team Science. http://www.vtoxford.org/meetings/AMQC/Handouts2014/Day1A_20_SalasCarrollUmoren_Fri_PRECONSavingLives.pdf. Accessed 15 Oct 2019.
Paige JT, Garbee DD, Kozmenko V, Yu Q, Kozmenko L, Yang T, et al. Getting a head start: high-fidelity, simulation-based operating room team training of interprofessional students. J Am Coll Surg. 2014;218(1):140–9.
Funding
This work was made possible through the generous support from a Medical Education Scholarship, Research, and Evaluation (MESRE) grant from the Southern Group on Educational Affairs (SGEA) of the Association of American Medical Colleges (AAMC) awarded in 2016.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval
N/A
Informed Consent
N/A
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Garbee, D.D., Bonanno, L.S., Rogers, C.L. et al. Comprehensive Literature Search to Identify Assessment Tools for Operating Room Nontechnical Skills to Determine Common Critical Components. Med.Sci.Educ. 31, 81–89 (2021). https://doi.org/10.1007/s40670-020-01117-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-020-01117-6