Abstract
Background
Integrated surgical residency programs and early specialization tracts have increased, with proposed benefits including shorter training time and increased exposure. Drawbacks include a loss of breadth and the need for earlier trainee career decisions. We sought to assess the rate of changing specialty interests over the course of general surgery residency, and what, if any, factors influenced that decision.
Methods
An 11-question, web-based survey was sent to alumni (2009–2019) of a single academic general surgery residency training program. It queried demographics and experiences during medical school and residency, whether specialty interest changed, and if so, what factors influenced that decision.
Results
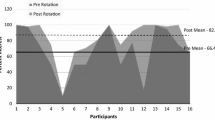
The survey was emailed to 53 alumni and completed by 59% (n = 31). The majority were male (n = 24, 77%) and Caucasian (n = 26, 84%). All 31 respondents went on to fellowship training. Three individuals (10%) did not declare a specialty interest when applying to residency. Of the 28 who declared an interest, the majority (n = 17, 61%) changed their interest over the course of residency and ultimately applied to fellowship in a different field. Amongst these, only six (25%) had previous exposure in medical school to the field they ultimately went in to. All who changed specialties (n = 17) reported an impactful clinical rotation influencing their decision.
Conclusions
Nearly two-thirds of general surgery residents at a single academic institution changed their specialty interest over the course of residency. Our findings suggest that while integrated programs may provide benefits, many medical students are not being exposed to these potential fields.

Similar content being viewed by others
Data Availability
Available to review
References
Borman KR, Vick LR, Biester TW, Mitchell ME. Changing demographics of residents choosing fellowships: longterm data from the American Board of Surgery. J Am Coll Surg. 2008;206:782–8; discussion 788-789. https://doi.org/10.1016/j.jamcollsurg.2007.12.012.
Stitzenberg KB, Sheldon GF. Progressive specialization within general surgery: adding to the complexity of workforce planning. J Am Coll Surg. 2005;201:925–32. https://doi.org/10.1016/j.jamcollsurg.2005.06.253.
Longo WE, Sumpio B, Duffy A, et al. Early specialization in surgery: the new frontier. Yale J Biol Med. 2008;81:187–91.
Craft JA, Craft TP. Rising medical education debt a mounting concern. Graduates also face less favorable repayment terms, shortage of training positions. Mo Med. 2012;109:266–70.
Jauhar S. From all walks of life--nontraditional medical students and the future of medicine. N Engl J Med. 2008;359:224–7. https://doi.org/10.1056/NEJMp0802264.
Campbell ST, Dave DR. Two sides to every story: early specialization in medical education. Med Sci Educ. 2018;28:243–6. https://doi.org/10.1007/s40670-017-0489-y.
Grant SB, Dixon JL, Glass NE, Sakran JV. Early surgical subspecialization: a new paradigm? Part I Bull Am Coll Surg. 2013;98:38–42.
The American Board of Surgery. Training & certification. Flexible rotations. http://www.absurgery.org/default.jsp?policyflexrotations. Accessed 1 May 2020.
Ferguson C. The arguments against fellowship training and early specialization in general surgery. Arch Surg. 2003;138:915–6.
Schmidt LE, Cooper CA, Guo WA. Factors influencing US medical students’ decision to pursue surgery. J Surg Res. 2016;203:64–74. https://doi.org/10.1016/j.jss.2016.03.054.
Berman L, Rosenthal MS, Curry LA, et al. Attracting surgical clerks to surgical careers: role models, mentoring, and engagement in the operating room. J Am Coll Surg. 2008;207:793–800, 800.e1–2. https://doi.org/10.1016/j.jamcollsurg.2008.08.003.
Chen H, Hardacre JM, Martin C, Lillemoe KD. Do medical school surgical rotations influence subspecialty choice? J Surg Res. 2001;97:172–8. https://doi.org/10.1006/jsre.2001.6135.
Haggerty KA, Beaty CA, George TJ, et al. Increased exposure improves recruitment: early results of a program designed to attract medical students into surgical careers. Ann Thorac Surg. 2014;97:2111–4; discussion 2114. https://doi.org/10.1016/j.athoracsur.2014.02.029.
Patel MS, Mowlds DS, Khalsa B, et al. Early intervention to promote medical student interest in surgery and the surgical subspecialties. J Surg Educ. 2013;70:81–6. https://doi.org/10.1016/j.jsurg.2012.09.001.
2019 report on residents executive summary. In: Assoc. Am. Med. Coll. https://www.aamc.org/data-reports/students-residents/interactive-data/report-residents/2019/executive-summary. Accessed 9 Apr 2020.
Khoushhal Z, Hussain MA, Greco E, et al. Prevalence and causes of attrition among surgical residents: a systematic review and meta-analysis. JAMA Surg. 2017;152:265–72. https://doi.org/10.1001/jamasurg.2016.4086.
Chen H, Reddy RM, Palmer SW, et al. Attrition rates in integrated vascular and cardiothoracic surgery residency and fellowship programs. J Vasc Surg. 2019;69:236–41. https://doi.org/10.1016/j.jvs.2018.07.074.
Lynch G, Nieto K, Puthenveettil S, et al. Attrition rates in neurosurgery residency: analysis of 1361 consecutive residents matched from 1990 to 1999. J Neurosurg. 2015;122:240–9. https://doi.org/10.3171/2014.10.JNS132436.
Prager JD, Myer CM, Myer CM. Attrition in otolaryngology residency. Otolaryngol--Head Neck Surg. 2011;145:753–4. https://doi.org/10.1177/0194599811414495.
Walker JL, Janssen H, Hubbard D. Gender differences in attrition from orthopaedic surgery residency. J Am Med Womens Assoc 1972. 1993;48:182–4 193.
Yang MK, Meyerson JM, Pearson GD. Resident attrition in plastic surgery: a national survey of plastic surgery program directors. Ann Plast Surg. 2018;81:360–3. https://doi.org/10.1097/SAP.0000000000001526.
Jones TL, Baxter MAJ, Khanduja V. A quick guide to survey research. Ann R Coll Surg Engl. 2013;95:5–7. https://doi.org/10.1308/003588413X13511609956372.
Robertson CM, Klingensmith ME, Coopersmith CM. Prevalence and cost of full-time research fellowships during general surgery residency: a national survey. Ann Surg. 2009;249:155–61. https://doi.org/10.1097/SLA.0b013e3181929216.
ACGME residents and fellows by sex and specialty, 2017. In: AAMC. https://www.aamc.org/data-reports/workforce/interactive-data/acgme-residents-and-fellows-sex-and-specialty-2017. Accessed 22 Sep 2020.
Wong RL, Sullivan MC, Yeo HL, et al. Race and surgical residency: results from a national survey of 4339 US general surgery residents. Ann Surg. 2013;257:782–7. https://doi.org/10.1097/SLA.0b013e318269d2d0.
Code Availability
Available to review
Author information
Authors and Affiliations
Contributions
K Giuliano—formation of study question, study design, survey design and distribution, data analysis, data interpretation, manuscript preparation; E Etchill—study design, survey design, data interpretation, manuscript preparation; S DeBrito—formation of study question, study design, data interpretation, manuscript preparation; B Sacks—formation of study question, study design, survey design, data interpretation, manuscript preparation.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethics Approval
This study was approved by the Johns Hopkins Institutional Review Board.
Consent to Participate
Completion of the survey served as the study participants’ informed consent (and was stated as such in the survey).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
Survey distributed to Hopkins General Surgery residency alumni. (PDF 87 kb)
Rights and permissions
About this article
Cite this article
Giuliano, K., Etchill, E., DiBrito, S. et al. What Kind of Surgeon Will You Be? An Analysis of Specialty Interest Changes Over the Course of General Surgery Residency. Med.Sci.Educ. 30, 1599–1604 (2020). https://doi.org/10.1007/s40670-020-01110-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-020-01110-z