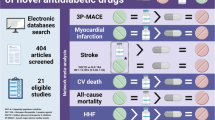
Abstract
Background
Absolute treatment benefits—expressed as numbers needed to treat—of the glucose lowering and cardiovascular drugs, glucagon-like peptide-1 (GLP-1) receptor agonists and sodium-glucose transporter 2 (SGLT2) inhibitors on renal outcomes remain uncertain. With the present meta-analysis of digitalized individual patient data, we aimed to display and compare numbers needed to treat of both drugs on a composite renal outcome.
Methods
From Kaplan–Meier plots of major cardiovascular outcome trials of GLP-1 receptor agonists and SGLT2 inhibitors vs. placebo, we digitalized individual patient time-to-event information on composite renal outcomes with WebPlotDigitizer 4.2; numbers needed to treat from individual cardiovascular outcome trials were estimated using parametric Weibull regression models and compared to original data. Random-effects meta-analysis generated meta-numbers needed to treat with 95% confidence intervals (CI).
Results
Twelve cardiovascular outcome trials (three for GLP-1 receptor agonists, nine for SGLT2 inhibitors) comprising 90,865 participants were included. Eight trials were conducted in primary type 2 diabetes populations, two in a primary heart failure and two in a primary chronic kidney disease population. Mean estimated glomerular filtration rate at baseline ranged between 37.3 and 85.3 ml/min/1.73 m2. Meta-analyses estimated meta-numbers needed to treat of 85 (95% CI 60; 145) for GLP-1 receptor agonists and 104 (95% CI 81; 147) for SGLT2 inhibitors for the composite renal outcome at the overall median follow-up time of 36 months.
Conclusion
The present meta-analysis of digitalized individual patient data revealed moderate and similar absolute treatment benefits of GLP-1 receptor agonists and SGLT2 inhibitors compared to placebo for a composite renal outcome.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes mellitus (T2DM), with prevalence increasing in many world regions, is a major global health issue [1, 2]. As a significant cause of cardiovascular disease and chronic kidney disease (CKD) [3, 4], T2DM is associated with a great burden of morbidity and mortality and subsequent high socio-economic impact [5, 6]. Thus, optimal treatment of T2DM and associated comorbidities is crucial to reduce the global burden of disease.
Updated T2DM treatment guidelines promote the use of sodium-glucose transporter 2 (SGLT2) inhibitors as well as glucagon-like peptide-1 (GLP-1) receptor agonists in subjects at high cardiovascular risk or with known cardiovascular disease [7, 8]. This recommendation derives from beneficial effects on diabetes-related cardiovascular as well as renal outcomes in major cardiovascular outcome trials in subjects with T2DM [9, 10]. Subsequently, these glucose-lowering drugs were shown to be effective also in populations without T2DM. As a result, SLGT2 inhibitors (empagliflozin and dapagliflozin) are now an integral part of first-line therapy in heart failure with reduced ejection fraction [11,12,13,14], and are the first drug class ever showing statistically significant reductions in major cardiovascular events in heart failure with preserved ejection fraction [15, 16]. GLP-1 receptor agonists (liraglutide and semaglutide) adopt an emerging role in specific treatment of obesity, showing sustained effects on weight loss in large scale trials [17].
For approval of antidiabetic therapy to treat T2DM, the U.S. Food and Drug Administration requires proof of non-inferiority on the hazard ratio (HR). Therefore, the majority of reports from cardiovascular outcome trials give only these relative effect estimates. Respective meta-analyses pooling data from these trials mostly report relative effects as well [10, 18]. In contrast, although it is recommended in guidelines, absolute treatment effects have rarely been reported in trials. Expression of absolute treatment effects by numbers needed to treat provides fundamental advantages in evaluating the cost/benefit ratio of a drug intervention. They help to clarify medical beneficial potential and allow evaluation of economic implications [19,20,21]. Since patient-level data from individual trials are not publicly available in the majority of cases, meta-analyses of absolute treatment effects for time-to-event outcomes cannot be performed. In order to incorporate absolute treatment effects on renal outcomes in a comprehensive meta-analysis, we applied a validated method of digitalization of time-to-event information obtained from publications of cardiovascular outcome trials investigating GLP-1 receptor agonists and SGLT2 inhibitors [22,23,24,25,26], as previously applied to cardiovascular and mortality outcomes [27, 28].
Methods
Study selection, outcome definition, data extraction and quality assessment
Eligible trials comparing SGLT2 inhibitors or GLP-1 receptor agonists to placebo were identified from the cardiovascular outcome trial summit reports by Schnell et al. [29,30,31,32,33,34,35,36], annual reflections on all major randomised controlled trials investigating cardiovascular outcomes in the field of diabetes and associated diseases. The most recent cardiovascular outcome trial summit report was published in March 2023. To identify relevant cardiovascular outcome trials outside of the regular cardiovascular outcome trial summit reports, we cross-checked a well known expert forum report on cardiovascular outcome trials in T2DM by Cefalu et al. [37]. However, no additional cardiovascular outcome trials were found. No protocol was pre-registered (e.g. in PROSPERO).
Full texts of cardiovascular outcome trial reports as well as supplementary information were searched for Kaplan–Meier plots depicting time-to-event information for a composite renal outcome. Cardiovascular outcome trials were excluded when no Kaplan–Meier plot for a composite renal outcome of SGLT2 inhibitors or GLP-1 receptor agonists vs. placebo were retrievable. Individual trial definitions of composite renal outcomes as reported served as the primary endpoint; details are provided in Table 1.
Digitalization of individual patient data from Kaplan–Meier plots was performed using two validated methods [24, 25] that were applied by our group in previous work [27, 28]: WebPlotDigitizer, Version 4.2 [22] and the R code of Guyot et al. [23].
From original trial reports, HRs with 95% confidence intervals (CI) as well as trial and patient characteristics were extracted. Accuracy of data extractions was checked by one investigator and double checked by another investigator. Divergences were resolved by group discussion. Risk of bias was appraised by one reviewer of our group according to recommendations from the Cochrane Collaboration’s revised tool for risk of bias assessment in randomised trials [38].
Weibull model fit, estimates of absolute treatment effect, and numbers needed to treat notation
For estimation of survival functions and to achieve absolute risk differences of both treatment groups, parametric Weibull regression models were fitted for all trials separately [39]. For each individual trial, monthly probability differences (treatment–control) were estimated for being free of the analysed event from month 1 to the respective maximal observation time. To obtain estimates for monthly numbers needed to treat, these probability differences were inverted [40]. The number needed to treat is defined as the number of patients who need to be treated for a determined time interval to prevent one additional event in the treatment group in comparison to the placebo group. Hence, positive numbers needed to treat are indicative that the drug is beneficial. A neutral effect of a therapeutic intervention, corresponding to a HR of 1, is denoted by a value of infinity for the number needed to treat.
Assessment of model validity
For appraisal of the validity of extracted data, comparison of HRs from the original papers to estimated Weibull HRs was carried out by calculating intra-class correlation coefficients. Furthermore, we plotted the estimated Weibull survival curves along with Kaplan–Meier survival curves from the extracted data for graphical assessment of the fit of the Weibull models.
Meta-analysis
Random-effects inverse-variance meta-analysis for each single monthly time point was carried out separately to summarise numbers needed to treat overall as well as for the two drug classes; all trial data were included up to longest available follow-up. Primarily, all computations were performed on the probability difference scale. They were later transformed to the number needed to treat scale in order to display results in figures and graphs. For management and analysis of data, we used SAS (SAS Institute Inc., Cary, NC, USA), Version 9.4. All data will be made publicly available in an online repository after publication.
Results
Study selection
Original time-to-event information on a composite renal outcome was retrievable from Kaplan–Meier curves of 12 major cardiovascular outcome trials, which were included in the analysis: three trials investigated GLP-1 receptor agonists (AMPLITUDE-O [41], LEADER [42, 43], and REWIND [44, 45]), nine SGLT2 inhibitors (CANVAS [46], CREDENCE [47], DAPA-CKD [48], DECLARE-TIMI 58 [49], EMPA-KIDNEY [50], EMPA-REG [51, 52], EMPEROR-PRESERVED [15, 53], EMPEROR-REDUCED [12, 53], and VERTIS-CV [54]). For all digitized Kaplan–Meier plots, the number of patients at risk was reported. The EXSCEL trial reported results of exenatide on a composite renal outcome, however could not be included due to lack of Kaplan–Meier plots [55]. The SUSTAIN-6 trial was excluded because the extracted HRs were very far from the originally reported HR, suggesting methodological problems [56].
Study characteristics
Clinical characteristics of the cardiovascular outcome trials’ study populations are listed in Table 2. In total, time-to-event information from 90,865 patients were extracted and used for further analysis. Median follow-up time ranged from 13.0 to 63.6 months among included studies; overall median follow-up time was 35.8 months. All cardiovascular outcome trials featured high cardiovascular risk populations [57]. The majority of trials were conducted in subjects selected for T2DM, while EMPEROR-PRESERVED [15] and EMPEROR-REDUCED [12] primarily included individuals with heart failure. DAPA-CKD [48] and EMPA-KIDNEY [50] were conducted in a population of subjects with CKD as the major inclusion criterion.
Mean estimated glomerular filtration rate (eGFR) at baseline ranged from 37.3 to 85.3 ml/min/1.73 m2. Definitions of composite renal endpoints were heterogeneous among the analysed cardiovascular outcome trials. However, all definitions included a pre-specified increase in serum creatinine or decrease in eGFR and incident end-stage kidney disease or renal replacement therapy. With the exception of AMLPITUDE-O [41], REWIND [44, 45], EMPEROR-PRESERVED [15], and EMPEROR-REDUCED [12], renal death was included in all composite renal endpoints. Risk of bias among all studies was low (Supplementary Table 1).
Relative and absolute treatment effect estimates
A total of 6199 (6.8%) patients experienced a composite renal event. Information on relative effect measures is given in Table 3: Original, digitalized, and Weibull HRs with 95% CI; absolute treatment effect estimates are reported as numbers needed to treat at 12, 24, 36, and 48 months. In addition, Fig. 1 depicts a graphical display of monthly number needed to treat point estimates with 95% CI for both trial drugs.
Numbers needed to treat in individual trials. Time-dependent numbers needed to treat (NNTs) over trial follow-up time for individual trials with their pointwise 95% confidence intervals (yellow: GLP-1 receptor agonists, red: SGLT2 inhibitors), Estimates and confidence intervals are truncated from above at 100,000
Accuracy of data extraction was assessed by a scatterplot (Supplementary Fig. 1) that compares the HR as reported from the original trial to the Weibull HR from the extracted data. Comparison revealed excellent correspondence indicated by an intra-class correlation of 99.5% (95% CI 99.0%; 100%). Supplementary Fig. 2 shows Kaplan–Meier survival curve estimates for both treatment groups in each trial along with the estimated survival curves from the corresponding Weibull models.
Meta-analysis of absolute treatment effects
Figure 2a shows treatment efficacy of GLP1 receptor agonists and SGLT2 inhibitors for the prevention of a single composite renal outcome on the number needed to treat scale: Estimated meta-numbers needed to treat were 85 (95% CI 60; 145) for GLP-1 receptor agonists and 104 (95% CI 81; 147) for SGLT2 inhibitors at the overall median follow-up time of 36 months. When pooling numbers needed to treat across both treatments, we found a meta-number needed to treat to prevent a single composite renal outcome of 65 (95% CI 51; 91) at a follow-up of 48 months (Fig. 2b).
Meta-Analysis of numbers needed to treat. Random-effects inverse-variance meta-analysis of numbers needed to treat (Meta-NNTs, with 95% CI) over trial follow-up time. a Data were pooled from trials according to GLP-1 receptor agonists (yellow) or SGLT2 inhibitors (red) study drugs. b data were pooled from all trials, regardless of the tested study drug. Estimates and confidence intervals are truncated from above at 100,000 (a) and 10,000, respectively
Discussion
In the present work, we performed a comprehensive meta-analysis of digitalized individual patient data from major cardiovascular outcome trials to assess absolute treatment effects (measured as numbers needed to treat) of GLP-1 receptor agonists and SGLT2 inhibitors on a composite renal outcome. For both drug classes, we observed a similar moderate absolute treatment efficacy when compared to placebo.
To improve cardiovascular outcomes, current guidelines encourage the use of GLP-1 receptor agonists and SGLT2 inhibitors in subjects with T2DM as well as SGLT2 inhibitors for the treatment of heart failure with the highest level of recommendation (Class I) [7, 58]. In subjects with T2DM and mild or moderate CKD, treatment with GLP-1 receptor agonists or SGLT2 inhibitors should be initiated, if therapy additional to metformin is required [58].
The majority of cardiovascular outcome trials on GLP-1 receptor agonists and SGLT2 inhibitors report treatment effects as relative measures (hazard, odds, or risk ratios), however, these ignore the baseline risk of the population when used as the main measure of efficacy. Higher baseline risk of a population is associated with higher absolute risk reductions, which can be achieved by an intervention, e.g. a drug treatment. Hence, guidelines for reporting randomised trials recommend providing information on relative and absolute effect measures, since absolute effect measures provide fundamental advantages for assessment of treatment efficacy and cost/benefit calculations [59]. They also facilitate comparative analyses with other drug classes and help patients to appraise expected benefits.
The quality of all cardiovascular outcome trials included in this analysis was high. These were well-conducted international randomised controlled trials published in high-impact journals with low risk of bias (Supplementary Table 1) [38]. Although inclusion criteria and target populations differed, cardiovascular risk in patients of all trials was high: populations featured either high proportions of cardiovascular disease, long-term T2DM or heart failure [12, 15, 41, 42, 44, 46,47,48,49,50,51, 54]. Average renal function was impaired in all populations, however, mean baseline eGFR notably differed from substantial CKD (< 60 mL/min/1.73 m2 in CREDENCE [47], DAPA-CKD [48], and EMPA-KIDNEY [50] to only mild renal impairment (60 to 89 mL/min/1.73 m2) in the other cardiovascular outcome trials [12, 15, 41, 42, 44, 46, 49, 51, 54]. Subjects with a lower eGFR are at higher risk for progression of kidney disease, indicating a baseline heterogeneity of renal risk in the analysed populations [60]. This emphasises the importance of looking at relative as well as absolute treatment effects. Relative treatment effects (HRs) for a composite renal outcome were comparable in CANVAS (0.60) [46], CREDENCE (0.66) [47], and DAPA-CKD (0.56) [48], but differed markedly on the number needed to treat scale: The 3-year meta-number needed to treat in CANVAS was 110, but 25 in CREDENCE; the 2-year meta-number needed to treat was 192 in CANVAS, but 23 in DAPA-CKD—indicating a substantially higher absolute efficacy in higher-risk patient populations.
Compared to the efficacy of SGLT2 inhibitors on hospitalisation for heart failure in DAPA-HF [11, 27] (2-year meta-number needed to treat of 21) and EMPEROR-REDUCED [12, 27] (2-year meta-number needed to treat of 15), the present analysis revealed only moderate absolute beneficial treatment effects of GLP-1 receptor agonists (36-month meta-number needed to treat of 85) and SGLT2 inhibitors (36-month meta-number needed to treat of 104) for a composite renal outcome. Whereas SGLT2 inhibitors are preferable over GLP-1 receptor agonists in heart failure with or without T2DM due to results from specific heart failure trials and current guideline recommendations, our analysis could not identify a greater advantage for either drug class regarding composite renal outcomes. However, appraisal of clinical relevance of a drug class in different populations based on comparing treatment efficacy for different outcomes is difficult and should not guide clinical decisions.
Type 2 diabetes mellitus is the leading cause of CKD [60]. It is associated with high morbidity/mortality burden and health expenditures [61]. There has been discussion about optimal selection of clinically relevant endpoints in trials to assess kidney-specific drug efficacy [62, 63]. Incident end-stage kidney disease or need for renal replacement therapy is without doubt a very serious clinical condition. Treatment of patients with end-stage kidney disease or renal transplantation is complex, logistically challenging, and causes substantial health expenditures [64,65,66,67]. Among cardiovascular outcome trials in T2DM, incident end-stage kidney disease is rare with event proportions of less than one percent, which generates the need to evaluate a composite outcome for renal drug efficacy in trials with reasonable sample size and duration of follow-up [68]. A decline of kidney function to a non-end-stage extent (measured as increase in serum creatinine or decline in eGFR) is the additional outcome that was included in all of the composite endpoints of cardiovascular outcome trials in the present analysis. However, definitions ranged from sustained ≥ 30% decline in eGFR (REWIND [44]) to doubling of serum creatinine [43, 46, 47, 52, 54], which approximates a 57% decline in eGFR and is a long-established kidney outcome, which is highly predictive of end-stage kidney disease (Table 1) [69]. The threshold of ≥ 40% eGFR decline, as applied in five cardiovascular outcome trials of the present analysis [12, 15, 41, 49, 50], was a reliable predictor of end-stage kidney disease or the traditional doubling of serum creatinine (HR ~ 20 over a median follow-up of two years) [70], whereas the association of a threshold of ≥ 30% serum creatinine increase was less strong (HR ~ 9). Hence, despite heterogeneity among composite renal outcome definitions, we assume all singular composite endpoint definitions include clinically meaningful outcomes suitable to assess kidney-specific treatment benefits in clinical trials (Table 1).
Renal pathogenesis includes inflammatory, humoral, metabolic and oxidative stress factors as well as macro- and microvascular disease [71]. Together with blood pressure reduction [72], intensive glycaemic control showed beneficial effects on diabetic kidney disease [73]. Metformin, the long-term first choice for treating people with T2DM has a 10-year number needed to treat of ~ 10–20 for major cardiovascular or diabetes-related endpoints [74, 75]. Due to consistent treatment effects of GLP-1 receptor agonists and SGLT2 inhibitors on major adverse cardiovascular events, and of SGLT2 inhibitors on renal endpoints with and without concomitant metformin use [76, 77], recent concepts have promoted the use of GLP1-receptor agonists and SGLT2 inhibitors in subjects with T2DM and CKD regardless of metformin administration [78]. However, the nephroprotective potential of GLP-1 receptor agonists and SGLT2 inhibitors is not limited to improved glycaemic control. Several indirect (e.g. blood pressure in SGLT2 inhibitors, weight loss in GLP-1 receptor agonists) and direct effects on the kidney have been reported (e.g. improvement of intrarenal haemodynamics or prevention of ischaemic and oxidative damage in SGLT2 inhibitors) [79, 80]. Positive results of DAPA-CKD [48] and EMPA-Kidney [50], the two large scale randomised controlled trials of SGLT2 inhibitors in subjects with pre-existing impaired renal function as the primary inclusion criterion, encourage the use of SGLT2 inhibitors in individuals with kidney disease regardless of coexisting T2DM. Similar trials of GLP-1 receptor agonists are currently not available. However, according to our results, they may represent an important area of future research.
In addition to previous analyses of other outcomes, this study now shows meta-analysed absolute effects of these drug classes regarding number needed to treat for a composite renal outcome. Ludwig et al. reported numbers needed to treat for major adverse cardiovascular events [40] and Davies et al. analysed a primary composite outcome and all‐cause mortality [81]. Our group previously analysed the trials´ primary outcomes, all-cause and cardiovascular mortality, as well as hospitalisation for heart failure [27, 28]. Although other groups used different digitalization tools and statistical methods, results for the analysed outcomes were comparable, which demonstrates that the method of digitalization of individual patient data to assess absolute treatment effects is valid and reliable, especially for cardiovascular outcome trials.
Due to our prespecified selection criteria, no systematic literature review was conducted. Trial selection for our meta-analysis relied on a shared definition of cardiovascular outcome trials as reported in the annual cardiovascular outcome trial summit reports [29,30,31,32,33,34,35] and thus the most important studies in the field were included; however, we cannot rule out that smaller non-cardiovascular outcome trial studies with renal outcomes may have been overlooked. The exclusion of trials (e.g. EXSCEL) due to lack of Kaplan–Meier plots may also have introduced bias. Differences in characteristics and design of included cardiovascular outcome trials introduce heterogeneity, a general limitation of meta-analyses requiring a cautious interpretation of results. Within the present work, heterogeneity derives from differences in baseline kidney function, heterogeneous baseline risk for the analysed outcome as well as differences in definitions of the outcomes among individual trials, all of which may introduce bias. However, we believe all composite renal outcome definitions among the included cardiovascular outcome trials to be clinically meaningful and suitable to assess drug efficacy.
Additionally, computations within the present work rely on digitalized individual patient outcomes and fitted Weibull models not including original patient data, which introduces risk of differences between original and extracted event counts (Supplementary Table 2) and does not allow appropriate interaction analyses. Therefore, no further insight into associations of patient characteristics with outcomes other than the analysed composite outcome can be obtained. The inability to perform subgroup analyses prevents the identification of effect modifiers. However, lack of access to individualised patient data renders the method of data digitalization unavoidable to perform the present analysis of absolute treatment effects. Sensitivity analyses, in the form of assessment of the Weibull curves (direct origin of estimated number needed to treat) fit, show excellent alignment to extracted data (Supplementary Fig. 2), which strongly indicates the validity of the applied methods.
Conclusions
The present meta-analysis of digitalized individual patient data revealed moderate and similar absolute treatment benefits of GLP-1 receptor agonists and SGLT2 inhibitors compared to placebo for a composite renal outcome.
Data availability
All data will be made publicly available in an online repository after publication.
References
WHO. The top 10 causes of death online2020 [Available from: https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death
Sun H, Saeedi P, Karuranga S et al (2022) IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract 183:109119. https://doi.org/10.1016/j.diabres.2021.109119. (Published Online First: 2021/12/10)
Sarwar N, Gao P, Seshasai SR et al (2010) Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet 375(9733):2215–2222. https://doi.org/10.1016/s0140-6736(10)60484-9. (Published Online First:2010/07/09)
Tuttle KR, Mauer MG, Narva AS (2012) KDOQI clinical practice guideline for diabetes and CKD: 2012 update. Am J Kidney Dis 60(5):850–86. https://doi.org/10.1053/j.ajkd.2012.07.005. (Published Online First: 2012/10/17)
Safiri S, Karamzad N, Kaufman JS et al (2022) Prevalence, deaths and disability-adjusted-life-years (DALYs) due to type 2 diabetes and its attributable risk factors in 204 countries and territories, 1990–2019: results from the global burden of disease study 2019. Front Endocrinol (Lausanne) 13:838027. https://doi.org/10.3389/fendo.2022.838027. (Published Online First:2022/03/15)
Seuring T, Archangelidi O, Suhrcke M (2015) The economic costs of type 2 diabetes: a global systematic review. Pharmacoeconomics 33(8):811–831. https://doi.org/10.1007/s40273-015-0268-9. (Published Online First: 2015/03/20)
Cosentino F, Grant PJ, Aboyans V et al (2020) 2019 ESC guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD. Eur Heart J 41(2):255–323. https://doi.org/10.1093/eurheartj/ehz486. (Published Online First:2019/09/10)
Disease C, Management R (2021) Standards of medical care in diabetes-2021. Diabetes Care 44(Suppl 1):S125–S150. https://doi.org/10.2337/dc21-S010. (Published Online First: 2020/12/11)
Sattar N, Lee MMY, Kristensen SL et al (2021) Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of randomised trials. Lancet Diabetes Endocrinol 9(10):653–662. https://doi.org/10.1016/s2213-8587(21)00203-5. (Published Online First: 2021/08/24)
Zelniker TA, Wiviott SD, Raz I et al (2019) SGLT2 inhibitors for primary and secondary prevention of cardiovascular and renal outcomes in type 2 diabetes: a systematic review and meta-analysis of cardiovascular outcome trials. Lancet 393(10166):31–39. https://doi.org/10.1016/s0140-6736(18)32590-x. (Published Online First: 2018/11/15)
McMurray JJV, Solomon SD, Inzucchi SE et al (2019) Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med 381(21):1995–2008. https://doi.org/10.1056/NEJMoa1911303. (Published Online First: 2019/09/20)
Packer M, Anker SD, Butler J et al (2020) Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med 383(15):1413–1424. https://doi.org/10.1056/NEJMoa2022190. (Published Online First: 2020/09/01)
McDonagh TA, Metra M, Adamo M et al (2021) 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 42(36):3599–3726. https://doi.org/10.1093/eurheartj/ehab368. (Published Online First: 2021/08/28)
Heidenreich PA, Bozkurt B, Aguilar D et al (2022) 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol 79(17):e263–e421. https://doi.org/10.1016/j.jacc.2021.12.012. (Published Online First: 2022/04/06)
Anker SD, Butler J, Filippatos G et al (2021) Empagliflozin in heart failure with a preserved ejection fraction. N Engl J Med 385(16):1451–1461. https://doi.org/10.1056/NEJMoa2107038. (Published Online First: 2021/08/28)
Solomon SD, McMurray JJV, Claggett B et al (2022) Dapagliflozin in heart failure with mildly reduced or preserved ejection fraction. N Engl J Med 387(12):1089–1098. https://doi.org/10.1056/NEJMoa2206286. (Published Online First: 2022/08/27)
Xie Z, Yang S, Deng W et al (2022) Efficacy and safety of liraglutide and semaglutide on weight loss in people with obesity or overweight: a systematic review. Clin Epidemiol 14:1463–1476. https://doi.org/10.2147/clep.S391819. (Published Online First: 2022/12/14)
Kristensen SL, Rørth R, Jhund PS et al (2019) Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of cardiovascular outcome trials. Lancet Diabetes Endocrinol 7(10):776–785. https://doi.org/10.1016/s2213-8587(19)30249-9. (Published Online First: 2019/08/20)
Schulz KF, Altman DG, Moher D (2010) CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ 340:c332. https://doi.org/10.1136/bmj.c332. (Published Online First: 2010/03/25)
Guyatt GH, Oxman AD, Santesso N et al (2013) GRADE guidelines: 12. Preparing summary of findings tables-binary outcomes. J Clin Epidemiol 66(2):158–72. https://doi.org/10.1016/j.jclinepi.2012.01.012. (Published Online First: 2012/05/23)
Sciences TAoM (2017) Sources of evidence for assessing the safety, efficacy and effectiveness of medicines: the Academy of Medical Sciences. https://acmedsci.ac.uk/file-download/86466482. Accessed 10 Jan 2024
Rohatgi A (2019) WebPlotDigitizer: Ankit Rohatgi. https://automeris.io/WebPlotDigitizer/releases. Accessed 10 Jan 2024
Guyot P, Ades AE, Ouwens MJ et al (2012) Enhanced secondary analysis of survival data: reconstructing the data from published Kaplan-Meier survival curves. BMC Med Res Methodol 12:9. https://doi.org/10.1186/1471-2288-12-9. (Published Online First: 2012/02/03)
Drevon D, Fursa SR, Malcolm AL (2017) Intercoder reliability and validity of webplotdigitizer in extracting graphed data. Behav Modif 41(2):323–339. https://doi.org/10.1177/0145445516673998. (Published Online First: 2016/10/21)
Moeyaert M, Maggin D, Verkuilen J (2016) Reliability, validity, and usability of data extraction programs for single-case research designs. Behav Modif 40(6):874–900. https://doi.org/10.1177/0145445516645763. (Published Online First: 2016/04/30)
Saluja R, Cheng S, Delos Santos KA et al (2019) Estimating hazard ratios from published Kaplan-Meier survival curves: a methods validation study. Res Synth Methods 10(3):465–475. https://doi.org/10.1002/jrsm.1362. (Published Online First: 2019/05/28)
Wolff G, Lin Y, Akbulut C et al (2022) Meta-analysed numbers needed to treat of novel antidiabetic drugs for cardiovascular outcomes. ESC Heart Fail. https://doi.org/10.1002/ehf2.14213. (Published Online First: 2022/11/08)
Kuss O, Akbulut C, Schlesinger S et al (2022) Absolute treatment effects for the primary outcome and all-cause mortality in the cardiovascular outcome trials of new antidiabetic drugs: a meta-analysis of digitalized individual patient data. Acta Diabetol 59(10):1349–1359. https://doi.org/10.1007/s00592-022-01917-9. (Published Online First: 2022/07/26)
Schnell O, Standl E, Catrinoiu D et al (2016) Report from the 1st cardiovascular outcome trial (CVOT) summit of the diabetes & cardiovascular disease (D&CVD) EASD study group. Cardiovasc Diabetol 15:33. https://doi.org/10.1186/s12933-016-0357-x. (Published Online First: 2016/02/20)
Schnell O, Standl E, Catrinoiu D et al (2017) Report from the 2nd cardiovascular outcome trial (CVOT) summit of the diabetes and cardiovascular disease (D&CVD) EASD study group. Cardiovasc Diabetol 16(1):35. https://doi.org/10.1186/s12933-017-0508-8. (Published Online First: 2017/03/13)
Schnell O, Standl E, Catrinoiu D et al (2018) Report from the 3rd cardiovascular outcome trial (CVOT) summit of the diabetes & cardiovascular disease (D&CVD) EASD study group. Cardiovasc Diabetol 17(1):30. https://doi.org/10.1186/s12933-018-0667-2. (Published Online First: 2018/02/21)
Schnell O, Standl E, Catrinoiu D et al (2019) Report from the 4th cardiovascular outcome trial (CVOT) summit of the diabetes & cardiovascular disease (D&CVD) EASD study group. Cardiovasc Diabetol 18(1):30. https://doi.org/10.1186/s12933-019-0822-4. (Published Online First: 2019/03/13)
Schnell O, Standl E, Cos X et al (2020) Report from the 5th cardiovascular outcome trial (CVOT) summit. Cardiovasc Diabetol 19(1):47. https://doi.org/10.1186/s12933-020-01022-7. (Published Online First: 2020/04/19)
Schnell O, Cos X, Cosentino F et al (2021) Report from the CVOT Summit 2020: new cardiovascular and renal outcomes. Cardiovasc Diabetol 20(1):75. https://doi.org/10.1186/s12933-021-01254-1. (Published Online First: 2021/04/02)
Schnell O, Battelino T, Bergenstal R et al (2022) Report from the CVOT summit 2021: new cardiovascular, renal, and glycemic outcomes. Cardiovasc Diabetol 21(1):50. https://doi.org/10.1186/s12933-022-01481-0. (Published Online First: 2022/04/10)
Schnell O, Battelino T, Bergenstal R et al (2023) CVOT Summit 2022 Report: new cardiovascular, kidney, and glycemic outcomes. Cardiovasc Diabetol 22(1):59. https://doi.org/10.1186/s12933-023-01788-6. (Published Online First: 2023/03/18)
Cefalu WT, Kaul S, Gerstein HC et al (2018) Cardiovascular outcomes trials in type 2 diabetes: where do we go from here? Reflections from a diabetes care editors’ expert forum. Diabetes Care 41(1):14–31. https://doi.org/10.2337/dci17-0057. (Published Online First: 2017/12/22)
Sterne JAC, Savović J, Page MJ et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898. https://doi.org/10.1136/bmj.l4898. (Published Online First: 2019/08/30)
Collett D (2015) Modelling survival data in medical research, 3rd edn. Chapman and Hall/CRC
Ludwig L, Darmon P, Guerci B (2020) Computing and interpreting the number needed to treat for cardiovascular outcomes trials: perspective on GLP-1 RA and SGLT-2i therapies. Cardiovasc Diabetol 19(1):65. https://doi.org/10.1186/s12933-020-01034-3. (Published Online First: 2020/05/15)
Gerstein HC, Sattar N, Rosenstock J et al (2021) Cardiovascular and renal outcomes with efpeglenatide in type 2 diabetes. N Engl J Med 385(10):896–907. https://doi.org/10.1056/NEJMoa2108269. (Published Online First: 2021/07/03)
Marso SP, Daniels GH, Brown-Frandsen K et al (2016) Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med 375(4):311–322. https://doi.org/10.1056/NEJMoa1603827. (Published Online First: 2016/06/14)
Mann JFE, Ørsted DD, Brown-Frandsen K et al (2017) Liraglutide and renal outcomes in type 2 diabetes. N Engl J Med 377(9):839–848. https://doi.org/10.1056/NEJMoa1616011. (Published Online First: 2017/08/31)
Gerstein HC, Colhoun HM, Dagenais GR et al (2019) Dulaglutide and cardiovascular outcomes in type 2 diabetes (REWIND): a double-blind, randomised placebo-controlled trial. Lancet 394(10193):121–130. https://doi.org/10.1016/s0140-6736(19)31149-3. (Published Online First: 2019/06/14)
Gerstein HC, Colhoun HM, Dagenais GR et al (2019) Dulaglutide and renal outcomes in type 2 diabetes: an exploratory analysis of the REWIND randomised, placebo-controlled trial. Lancet 394(10193):131–138. https://doi.org/10.1016/s0140-6736(19)31150-x. (Published Online First: 2019/06/14)
Neal B, Perkovic V, Mahaffey KW et al (2017) Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 377(7):644–657. https://doi.org/10.1056/NEJMoa1611925. (Published Online First: 2017/06/13)
Perkovic V, Jardine MJ, Neal B et al (2019) Canagliflozin and renal outcomes in type 2 diabetes and nephropathy. N Engl J Med 380(24):2295–2306. https://doi.org/10.1056/NEJMoa1811744. (Published Online First:2019/04/17)
Heerspink HJL, Stefánsson BV, Correa-Rotter R et al (2020) Dapagliflozin in patients with chronic kidney disease. N Engl J Med 383(15):1436–1446. https://doi.org/10.1056/NEJMoa2024816. (Published Online First: 2020/09/25)
Wiviott SD, Raz I, Bonaca MP et al (2019) Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med 380(4):347–357. https://doi.org/10.1056/NEJMoa1812389. (Published Online First: 2018/11/13)
Herrington WG, Staplin N, Wanner C et al (2023) Empagliflozin in patients with chronic kidney disease. N Engl J Med 388(2):117–127. https://doi.org/10.1056/NEJMoa2204233. (Published Online First: 2022/11/05)
Zinman B, Wanner C, Lachin JM et al (2015) Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 373(22):2117–2128. https://doi.org/10.1056/NEJMoa1504720. (Published Online First: 2015/09/18)
Wanner C, Inzucchi SE, Lachin JM et al (2016) Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med 375(4):323–334. https://doi.org/10.1056/NEJMoa1515920. (Published Online First: 2016/06/15)
Packer M, Butler J, Zannad F et al (2021) Empagliflozin and major renal outcomes in heart failure. N Engl J Med 385(16):1531–1533. https://doi.org/10.1056/NEJMc2112411. (Published Online First: 2021/08/28)
Cannon CP, Pratley R, Dagogo-Jack S et al (2020) Cardiovascular outcomes with ertugliflozin in type 2 diabetes. N Engl J Med 383(15):1425–1435. https://doi.org/10.1056/NEJMoa2004967. (Published Online First: 2020/09/24)
Holman RR, Bethel MA, Mentz RJ et al (2017) Effects of once-weekly exenatide on cardiovascular outcomes in type 2 diabetes. N Engl J Med 377(13):1228–1239. https://doi.org/10.1056/NEJMoa1612917. (Published Online First: 2017/09/15)
Marso SP, Bain SC, Consoli A et al (2016) Semaglutide and cardiovascular outcomes in patients with type 2 diabetes. N Engl J Med 375(19):1834–1844. https://doi.org/10.1056/NEJMoa1607141. (Published Online First: 2016/09/17)
Visseren FLJ, Mach F, Smulders YM et al (2021) 2021 ESC guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J 42(34):3227–3337. https://doi.org/10.1093/eurheartj/ehab484. (Published Online First:2021/08/31)
American Diabetes Association Group (2021) 9. Pharmacologic approaches to glycemic treatment: standards of medical care in diabetes-2021. Diabetes Care 44(Suppl 1):111–24. https://doi.org/10.2337/dc21-S009. (Published Online First: 2020/12/11)
Moher D, Hopewell S, Schulz KF et al (2010) CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. BMJ 340:c869. https://doi.org/10.1136/bmj.c869. (Published Online First: 2010/03/25)
KDIGO. Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO (2012) clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl 2013(3):1–150
Mullins CD, Pantalone KM, Betts KA et al (2022) CKD progression and economic burden in individuals with CKD associated with type 2 diabetes. Kidney Med 4(11):100532. https://doi.org/10.1016/j.xkme.2022.100532. (Published Online First: 2022/11/08)
Perkovic V, Koitka-Weber A, Cooper ME et al (2020) Choice of endpoint in kidney outcome trials: considerations from the EMPA-REG OUTCOME® trial. Nephrol Dial Transplant 35(12):2103–2111. https://doi.org/10.1093/ndt/gfz179. (Published Online First: 2019/09/10)
Inker LA, Grams ME, Guðmundsdóttir H et al (2022) Clinical trial considerations in developing treatments for early stages of common, chronic kidney diseases: a scientific workshop cosponsored by the national kidney foundation and the US food and drug administration. Am J Kidney Dis 80(4):513–526. https://doi.org/10.1053/j.ajkd.2022.03.011. (Published Online First: 2022/08/16)
System USRD (2018) 2018 USRDS annual data report: epidemiology of kidney disease in the United States. https://www.niddk.nih.gov/about-niddk/strategic-plans-reports/usrds/prior-data-reports. Accessed 10 Jan 2024
Levin A, Tonelli M, Bonventre J et al (2017) Global kidney health 2017 and beyond: a roadmap for closing gaps in care, research, and policy. Lancet 390(10105):1888–1917. https://doi.org/10.1016/s0140-6736(17)30788-2. (Published Online First: 2017/04/25)
Yang F, Liao M, Wang P et al (2021) The cost-effectiveness of kidney replacement therapy modalities: a systematic review of full economic evaluations. Appl Health Econ Health Policy 19(2):163–180. https://doi.org/10.1007/s40258-020-00614-4. (Published Online First: 2020/10/14)
Sundström J, Bodegard J, Bollmann A et al (2022) Prevalence, outcomes, and cost of chronic kidney disease in a contemporary population of 2·4 million patients from 11 countries: the CaReMe CKD study. Lancet Reg Health Eur 20:100438. https://doi.org/10.1016/j.lanepe.2022.100438. (Published Online First:2022/09/13)
Williams DM, Nawaz A, Evans M (2020) Renal outcomes in type 2 diabetes: a review of cardiovascular and renal outcome trials. Diabetes Ther 11(2):369–386. https://doi.org/10.1007/s13300-019-00747-3. (Published Online First: 2019/12/22)
Lambers Heerspink HJ, Perkovic V, de Zeeuw D (2011) Is doubling of serum creatinine a valid clinical ‘hard’ endpoint in clinical nephrology trials? Nephron Clin Pract 119(3):c195-9. https://doi.org/10.1159/000327614. (Discussion c99 Published Online First: 2011/08/13)
Lambers Heerspink HJ, Tighiouart H, Sang Y et al (2014) GFR decline and subsequent risk of established kidney outcomes: a meta-analysis of 37 randomized controlled trials. Am J Kidney Dis 64(6):860–866. https://doi.org/10.1053/j.ajkd.2014.08.018. (Published Online First: 2014/12/03)
Thomas MC, Brownlee M, Susztak K et al (2015) Diabetic kidney disease. Nat Rev Dis Primers 1:15018. https://doi.org/10.1038/nrdp.2015.18. (Published Online First: 2015/01/01)
Emdin CA, Rahimi K, Neal B et al (2015) Blood pressure lowering in type 2 diabetes: a systematic review and meta-analysis. JAMA 313(6):603–615. https://doi.org/10.1001/jama.2014.18574. (Published Online First: 2015/02/11)
Coca SG, Ismail-Beigi F, Haq N et al (2012) Role of intensive glucose control in development of renal end points in type 2 diabetes mellitus: systematic review and meta-analysis intensive glucose control in type 2 diabetes. Arch Intern Med 172(10):761–769. https://doi.org/10.1001/archinternmed.2011.2230. (Published Online First: 2012/05/29)
Gerstein HC (1999) Metformin reduced diabetes-related end points and all-cause mortality in overweight patients with type 2 diabetes. ACP J Club 130(1):3. https://doi.org/10.7326/ACPJC-1999-130-1-003
UK Prospective Diabetes Study (UKPDS) Group (1998) Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet 352(9131):854–65 (Published Online First: 1998/09/22)
Tsapas A, Karagiannis T, Avgerinos I et al (2021) GLP-1 receptor agonists for cardiovascular outcomes with and without metformin. A systematic review and meta-analysis of cardiovascular outcomes trials. Diabetes Res Clin Pract 177:108921–88. https://doi.org/10.1016/j.diabres.2021.108921. (Published Online First: 2021/06/19)
Neuen BL, Arnott C, Perkovic V et al (2021) Sodium-glucose co-transporter-2 inhibitors with and without metformin: a meta-analysis of cardiovascular, kidney and mortality outcomes. Diabetes Obes Metab 23(2):382–390. https://doi.org/10.1111/dom.14226. (Published Online First: 2020/10/13)
Davies MJ, Aroda VR, Collins BS et al (2022) Management of hyperglycemia in type 2 diabetes, 2022. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 45(11):2753–86. https://doi.org/10.2337/dci22-0034. (Published Online First: 2022/09/24)
Lee MMY, Petrie MC, McMurray JJV et al (2020) How do SGLT2 (sodium-glucose cotransporter 2) inhibitors and GLP-1 (glucagon-like peptide-1) receptor agonists reduce cardiovascular outcomes?: completed and ongoing mechanistic trials. Arterioscler Thromb Vasc Biol 40(3):506–522. https://doi.org/10.1161/atvbaha.119.311904. (Published Online First: 2020/01/31)
Scheen AJ (2019) Effects of glucose-lowering agents on surrogate endpoints and hard clinical renal outcomes in patients with type 2 diabetes. Diabetes Metab 45(2):110–121. https://doi.org/10.1016/j.diabet.2018.10.003. (Published Online First:2018/11/28)
Davies MJ, Kloecker DE, Webb DR et al (2020) Number needed to treat in cardiovascular outcome trials of glucagon-like peptide-1 receptor agonists: a systematic review with temporal analysis. Diabetes Obes Metab 22(9):1670–1677. https://doi.org/10.1111/dom.14066. (Published Online First:2020/05/07)
Funding
Open Access funding enabled and organized by Projekt DEAL. All authors declare: No external or third-party funding was received for the submitted work.
Author information
Authors and Affiliations
Contributions
Research idea and study design: MB, GW, OK; data acquisition: MB, CP, CA; data analysis/interpretation: MB, CP, KGV, RW, CJ, CA, SS, GW, OK; statistical analysis: CA, OK; supervision or mentorship: MK, MR, GW. All authors were involved in drafting the work or revising it critically for important intellectual content, gave final approval of the version submitted, and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare: No direct or indirect funding was received by any industry party for the present work; no financial relationships with any organisations that might have an interest in the submitted work in the previous three years; no other relationships or activities that could appear to have influenced the submitted work. MB received congress travel expenses from Daiichi Sankyo and personal fees from Amgen, Sanofi-Aventis and Novartis. MR reports personal fees from Allergan, Astra-Zeneca, Bristol-Myers-Squibb, Eli Lilly, Fishawack Group, Gilead Sciences, Intercept Pharma, Inventiva, Novartis, Novo Nordisk, Pfizer, Prosciento, Sanofi US, and Target RWE and investigator-initiated research support from Boehringer-Ingelheim, Nutricia/Danone, and Sanofi-Aventis. SS received honoraria for lectures from Novo Nordisk. GW received congress travel expenses from Abbott. OK reports honoraria for biostatistical education and consulting from Berlin-Chemie.
Ethical approval
Not applicable.
Human and animal rights
In the present meta-analysis, no primary patient or animal data were analysed for the submitted work. However, all individual trials included report ethics approval warranting human rights.
Informed consent
Written informed consent obtained from trial participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Brockmeyer, M., Parco, C., Vargas, K.G. et al. Absolute treatment effects of novel antidiabetic drugs on a composite renal outcome: meta-analysis of digitalized individual patient data. J Nephrol 37, 309–321 (2024). https://doi.org/10.1007/s40620-023-01858-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-023-01858-8