Abstract
Background
Health equity can lead to disparities in cancer screening, treatment, and mortality. This systematic review aims to identify and describe interventions that used video or DVD formats to reduce health inequity in cancer screening and review the effectiveness of such interventions in increasing screening rates compared to usual care conditions.
Methods
We searched PubMed, Web of Science, Embase, and Cochrane databases for randomized control trials (RCTs) published until 18/01/2023 that compared intervention versus usual care control groups, with the percentage of cancer screening uptake during follow-up as an outcome. The risk of Bias was assessed with the Cochrane Collaboration tool.
Results
After screening 4201 abstracts, 192 full texts were assessed for eligibility and 18 were included that focused on colorectal (n = 9), cervical (n = 5), breast (n = 5), and prostate (n = 1) cancer screening. All were based in the USA except one and most focused on ethnicity/race, while some included low-income populations. Most of the video interventions used to increase cervical cancer screening reported positive results. Studies aimed at increasing mammography uptake were mostly effective only in specific groups of participants, such as low-income or less-educated African American women. Results for colorectal cancer screening were conflicting. Videos that were culturally tailored or used emotive format were generally more effective than information-only videos.
Conclusions
Video interventions to increase cancer screening among populations with low screening uptake show some positive effects, though results are mixed. Interventions that use individual and cultural tailoring of the educational material should be further developed and investigated outside of the USA.
Similar content being viewed by others
Introduction
The World Health Organization (WHO) defines health inequity as “systematic differences in the health status of different population groups” [https://www.who.int/news-room/facts-in-pictures/detail/healthinequities-and-their-causes]. Health inequity arises from many causes, including social, economic, environmental, and structural disparities that contribute to differences in health outcomes within and between societies. For many cancers, health inequity occurs at several levels, with differences observed in screening detection, diagnosis, treatment, and mortality. Screening at the public health and population level is an important strategy, especially for cervical, prostate, breast, and colorectal (CRC) cancers. For example, breast cancer mortality can be reduced with mammography screening [1] and CRC mortality through guaiac fecal occult blood testing (FOBT) or flexible sigmoidoscopy [2] screening techniques. A UK study reported that cervical cancer screening currently prevents 70% of cervical cancer deaths and estimated that 83% of such deaths could be prevented if everyone attended screening regularly [3].
Studies, mostly from the USA, have revealed lower cancer screening rates in certain racial and ethnic groups [4,5,6], immigrants [7], those with low-income or living in socio-economically deprived neighbourhoods [7, 8], and people living in rural areas [9]. The reasons behind differences in cancer screening uptake are complex and multifactorial. Sociodemographic and cultural norms [10, 11], as well as perceived susceptibility, benefits, and barriers, can all contribute to screening intention or completion [11]. Cancer stigma is significantly higher in men and in those from ethnic minority backgrounds and is associated with not being screened as recommended for cervical, breast, and colorectal cancer [12]. A review on cervical cancer screening identified numerous sociocultural factors influencing health-related beliefs and healthcare utilization among immigrant and ethnic minorities in the US [6] and the authors recommended that culturally relevant screening strategies should be developed to address growing health inequity [6]. Interventions that focus on social determinants of health to improve breast, cervical, and colorectal cancer screening appear to be cost-effective for underserved populations in the US because the increase in screening can lead to earlier diagnosis and treatment, better health outcomes, and improvements in quality-adjusted life-years [13]. Different interventions that focus on the barriers and motives underlying the lack of screening have been evaluated such as letters or alerts to remind people to attend a screening, using lay health workers or healthcare professionals to deliver group or individual health counselling and education, designing ethnically and culturally tailored print or video materials, providing financial incentives, and using interactive multimedia programs and decision aids [14,15,16,17,18,19,20,21,22,23,24,25,26,27]. Some trials have used video and DVDs to target groups with low cancer screening, to deliver information about the importance of screening, and different screening modalities and to address potential barriers to screening. These may be especially relevant now due to disruptions to routine screening services during the COVID-19 pandemic [28] as they have the potential to be delivered remotely. As results differ between studies, it will be useful to systematically evaluate the current evidence to provide an overview of how effective such interventions are for improving cancer screening, especially as they may be more cost-effective than some of the other more complex interventions.
Therefore, the objective of the current review is to describe interventions that used video or DVD formats to increase cancer screening in populations with low screening uptake and review the effectiveness of such interventions in increasing screening rates. Specifically, we focus on interventions that use videos or DVDs to deliver information with specific aims to i) assess whether participants who are shown video and DVD interventions aimed at increasing screening uptake have higher screening over follow-up than people receiving standard screening programs (usual care) and ii) compare different types of video delivery, for example, informative videos versus other types of video format (i.e., emotive videos that use a narrator who is a cancer survivor or culturally tailored storylines etc.).
Method
The review was reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) recommendations [29]. In this review, we include papers covering various types of health inequity, including those related to ethnicity and race, low income, and low educational status. Due to heterogeneity between studies, we did not include a meta-analysis.
Search Strategy and Selection Criteria
We searched four databases for articles published until 18/01/2023: 1) PubMed electronic database of the National Library of Medicine; 2) Web of Science; 3) Embase and; 4) Cochrane. Medical subject heading (MeSH) terms and free words referring to health equity and cancer screening were used as keywords. The PubMed search string is shown in Appendix 1.
References from the selected papers and from other relevant articles were also screened for potential studies. We used a PICOS to define relevant articles. Population included groups of people that are disproportionately affected by disparities, such as ethnic minorities and people with low income or educational levels. We focused only on cancers that are usually screened at the general population level as a public health strategy for everyone of a certain age (e.g., we did not include, for example, screening for lung cancer as it is not routinely done in people unless they are in high-risk groups such as heavy smokers etc.). Thus, we focused on CRC, breast, prostate, and cervical cancer. Intervention included any intervention to increase cancer screening uptake that used a video or DVD method to provide information to a specific group of people (low SES, ethnic minority groups etc.). Comparison was measured in two ways. First, we compared interventions versus usual care (i.e., usual screening invitation and process). Second, we compared different methods to deliver the information in the videos (for example, comparing culturally tailored videos to informative videos etc.). Outcome was a percentage of cancer screening uptake during follow-up (self-reported or medical record documentation of screening completion). Any type of screening was included, such as pap tests, HPV self-sampling test kits, mammographies, clinical breast exams, fecal immunochemical test (FIT), FOBT, flexible sigmoidoscopy, colonoscopy, etc.). Study design was limited exclusively to RCTs.
Study Selection and Data Extraction
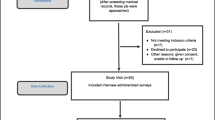
Two reviewers independently screened the titles and abstracts of the selected studies. Table 1 shows the exclusion criteria. The full texts of the articles selected by one or more of the reviewers were retrieved for evaluation. Two reviewers independently read the full texts and extracted the information from the selected studies. A third person reviewed the data extraction, and any disagreement was resolved through consensus. The numbers of abstracts screened, and studies assessed for eligibility, with reasons for exclusions at each stage, are presented in Fig. 1.
Data Extraction
Data extraction was conducted by one researcher and checked by another. Information was extracted on study design, number of participants (controls and intervention), participant demographics and baseline characteristics, type of cancer screening, type of intervention (including a description of the intervention), comparison group, and outcome (screening uptake). Data was recorded using RevMan.
Assessment of Risk of Bias
The Review Manager software and the Cochrane Risk of Bias Tool were used for a methodological quality assessment of the risk of bias of the included studies [30]. The following domains were evaluated: (1) selection bias: sequence generation, allocation concealment; (2) detection bias: blinding of outcome assessment; (3) attrition bias: incomplete outcome data; and (4) reporting bias: selective reporting. In the case of a low possibility of bias, the studies were categorized as “low risk”, in the case of a high possibility of bias — “high risk” and if the occurrence of risk of bias could not be indicated — “unclear risk”. An in-detail summary of the risk of bias assessment is included in Appendix 2 (Tables 1 to 16). Bias assessment was done independently by two authors and discussed to reach a consensus in case of disagreement.
Results
Search Results
Figure 1 presents the results of the search; 4201 papers were identified in the search after duplicates were removed. After screening the titles and abstracts, 193 were assessed for eligibility but 2 reports could not be retrieved. One additional publication was found during the reference list search, but the data were from 1991 and it was excluded, as it is likely that the data are not relevant to the current health equity field. We excluded 25 conference abstracts and 21 protocols. After reading the full text, 18 were included in the final review [23, 31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47].
Study Characteristics
The characteristics of the studies are shown in Tables 2–5. One study was conducted in New Zealand [32] and the remainder were from the USA. Most of the interventions were targeted to populations with either low socioeconomic status (low household income, high rates of unemployment, not covered by medical insurance) or to specific cultural or ethnic/racial populations in the USA, including Latino/Hispanic, Chinese women, and African American populations, as well as Maori and Pacific people in New Zealand. Although some studies had multiple outcomes, for example, change in health literacy or screening knowledge or beliefs, we only extracted data relevant to the aim of this review, namely screening completion. Follow-up times ranged from 4 weeks to 12 months, but most were 6 months.
Video Interventions
The studies used videos or DVDs to provide information to participants about cancer screening. A range of information was included such as general information about cancer risks, risk factors, and the importance of screening, and often they showed films of the screening process. In many cases, the studies compared different modalities of information delivery, for example, comparing factual videos to emotive ones (e.g., featuring a cancer survivor), or added cultural tailoring (e.g., designed to debunk culturally based beliefs about cancer or screening, or using language and narrators of the same race or ethnicity as participants etc.). One [49] used an interactive DVD with 36 combinations of messages that changed according to belief questions that the participants answered using arrows on the DVD remote. According to the PICOS and exclusion criteria, we tried to include only studies that had only used videos alone, but some combined the video with another method, such as a brochure. We excluded studies where the video was only one part of a much larger intervention with multiple components. The comparison conditions were mostly usual care/normal screening but some compared video alone with combinations of other intervention components, for example, there were four arms in the ACCION study [38, 39], one which used a “promotora” (lay health advisor from the Hispanic community), one which used only a video to deliver information, and one that included both video and promotora, compared to a no-intervention control.
Cervical Cancer Screening
Our search identified five studies on cervical cancer screening [40,41,42,43,44], as shown in Table 2. Calderon-Mora et al. [41] found no significant effect of their novella-style video on screening completion in Latina women compared to an information flipchart, but they did find an effect within women aged 51–65. Rivers et al. [42] demonstrated that the way that messages were delivered through video had an effect on screening rates but the effect differed on how they were worded. Although results did not reach statistical significance when pap tests were described as a detection behaviour, participants shown “loss-framed” messages (e.g., that emphasized negative aspects of what could happen if you do not get screening) had double the odds of completing screening than participants who watched gain-framed messages (e.g., “if you don’t get regular pap tests, you can’t detect cervical cancer early” versus “if you get regular pap tests, you can detect cervical cancer early”).
Byrd et al. [40] reported significantly higher self-reported cervical cancer screening in participants in the video-only arm of their study compared to controls but, interestingly, the screening rates did not differ in the video arm compared to a more complex intervention arm that included training by a promotora in conjunction with the instructional video. In contrast, a study on Chinese women in North America [43] found that an intervention containing an education-entertainment video, a motivational pamphlet, an educational brochure, and a fact sheet, increased screening completion (25–39%) compared to usual care (15%) but when the materials were delivered with an outreach worker who provided tailored counselling screening rates were significantly higher (39%) than when participants received the material by post (25%). Similarly, Thompson et al. [48] reported the same results in Latina women, though the Spanish language video was not statistically significantly better at increasing screening rates than usual care, there was only an effect when the video was present in combination with a home-based educational session led by a trained promotora. After a reference list search, we also identified a study from the UK of potential interest [50] on Asian women, but it was not included as it was published in 1991 and the results are unlikely to be relevant to the current field.
Prostate Cancer Screening
There was only one study on prostate cancer screening [45] (Table 3), which used an intervention consisting of a 25-min videotape focusing on a middle-aged African American man as he discusses prostate cancer screening with his friends, family, and doctor. Participants in the intervention group did not have higher odds of prostate screening completion than controls.
Breast Cancer Screening
We identified five studies that examined breast cancer screening as an outcome (Table 4). One [31] reported a small but not significant effect of a videotape on increasing mammography screening. Champion et al. [49] utilized an interactive DVD containing both video and other visual presentations to deliver tailored messages to participants. African American women with incomes below $75,000 who were in the interactive DVD group completed significantly more mammograms than women in usual care over follow-up. Similar results were reported by Gathirua-Mwangi et al. [46] in their study on African American women; for women with low incomes (≤ $30,000) a tailored narrative DVD intervention increased the odds of mammography five times compared to usual care, but no effect was seen in women with higher income levels. Kreuter et al. [23] also reported different success rates of their intervention depending on the characteristics of the patient. Specifically, in women with lower education (< 12 years) a narrative video format (with personal stories from African American breast cancer survivors) improved mammography completion compared to an informative, factual video narrated by an African American woman, but no effects were seen in women with higher educational levels (more than 12 years). In a trial on Chinese American immigrants [47] assessed acculturation, which was dichotomized according to English language ability and years of US residency. The culturally targeted video significantly increased mammography screening among low-acculturated women compared to the control condition (fact sheet).
Colorectal Cancer (CRC) Screening
Nine studies reported findings from RCTS on CRC screening [31,32,33,34,35,36,37,38,39] (Table 5), of which two [38, 39] had data from the same trial. Several studies reported no effect of their interventions. In Davis et al.’s (14) study on low literacy, low-income, ethnically diverse communities, multicomponent, targeted, low-literacy materials were not found to be significantly different or more effective in increasing FIT uptake compared with the nontargeted materials. They instead suggested that the provision of a FIT test plus education may provide a key driver to improve CRC screening. Fernández et al. (15) evaluated a small media intervention consisting of a flipchart and DVD about CRC and screening compared to a tailored interactive multimedia intervention and usual care control. Neither of the two interventions increased screening uptake compared to controls. Gwede et al.’s (13) “LCARES” intervention featuring a Spanish language, low-literacy, culturally targeted photonovella booklet and DVD did not increase screening uptake compared to a standard Spanish-language booklet. Colonoscopy completion was also not significantly higher in Hoffman et al.’s (12) decision-aid video in an African American population. However, it did increase patients´ knowledge and reduced their decisional conflict. The only study outside of the US evaluated an intervention in Maori and Pacific people in New Zealand [32]. The DVD providing culturally tailored information on bowel cancer and FOBT included a famous Māori rugby player, who delivered key program messages aimed at improving knowledge and reducing barriers, including the ease and cleanliness of the test, and key features of invitation and program participation. The DVD also featured two well-known local Māori elders presenting a narrative description of their program participation experience. Surprisingly, FOBT screening was significantly lower in the intervention (13.6%) versus usual care controls (25.9%). However, spoiled kit rates were significantly higher among those who were not sent the DVD (33.1% versus 12.4% in Māori and 42.1% versus 21.9% in Pacific).
The other studies, however, did report some positive results. Aragones et al. [51] found higher CRC screening in Latino immigrants at three-month follow-up using an educational video in Spanish on a portable personal digital video display device accompanied by a brochure with key information for the patient, and a patient-delivered paper-based reminder for their physician, compared to a usual care control. Of note, the intervention’s success may have been due to the fact that it targeted both physicians (through a patient-delivered paper-based reminder for their physician) and patients. Cameron et al. [33] reported significantly higher screening at both three and six months in their intervention versus usual care control. The intervention was a mailing consisting of a personalized reminder letter from the physician, an educational brochure, and a DVD about colorectal cancer and colorectal cancer screening. Lairson et al.[38] and Shokar et al.[39] reported data from the same trial, the ACCION program: a community-wide service and research program designed to educate and facilitate colorectal cancer screening compliance among a low-income, uninsured Hispanic population. Interventions included a video-only arm, a promotora-only arm, and a video-plus promotora arm. The screening was higher in participants who only viewed the video compared to controls (78% vs 10.1%).
Risk of Bias
Random sequence generation (selection bias): Seven studies had a low risk of bias. The authors described in detail a random component of the sequence-generation process. Eight studies were assessed as having an unclear risk of bias, as no information about the randomization process was provided. One study had a high risk of bias because the investigators described a non-random component in the sequence generation process.
Allocation concealment (selection bias): Two studies were judged at low risk of bias, as the allocation methods used were appropriate. Two studies had a high risk of bias because investigators enrolling participants could possibly foresee assignments. Twelve studies were assessed with an unclear risk of bias as they contained no information about allocation concealment procedures.
Blinding of participants and personnel (performance bias): In four studies unlikely that the blinding could have been broken, so the risk of bias was judged as low. Ten studies were assessed with a high risk, due to lack of blinding or incomplete blinding. Two studies were judged with an unclear risk, due to lack of information about blinding of participants and providers.
Blinding of outcome assessment (detection bias): In three studies the outcome assessment was blinded, so the risk of bias was judged as low. Eight studies were assessed with a high risk, as the outcome assessment was not blinded. Five studies were judged with an unclear risk, due to lack of information about blinding of outcome assessor.
Incomplete outcome data (attrition bias): Ten studies were assessed with a low risk of bias because no missing data were found, or the purpose of participants’ exclusion was properly argued. No studies had a high risk of bias related to the number of drop-outs due to missing primary outcome data. Six studies were judged with an unclear risk, due to lack of information about a reason for missing data.
Selective reporting (reporting bias): Six studies were judged with a low risk of bias because the study protocol was registered with the study’s pre-specified outcomes. Study protocol was not available for ten studies and, thus, they were judged with a high risk. Detailed risk of bias in the included studies is shown in Fig. 2, whereas the overall quality of included studies can be observed in Fig. 3.
Discussion
Main Findings
Our systematic review identified twenty studies that assessed video interventions aimed to increase cancer screening in ethnic and racial minority groups, and populations with low income. For cervical cancer screening, most of the video interventions reported positive results. Studies aimed at increasing mammography uptake generally were only effective in specific groups of participants, such as low-income or less-educated African American women. Studies on CRC screening reported conflicting results, with half finding significant effects on screening uptake and the rest reporting no difference in screening between intervention and control participants. Of note, except for one study, all were based in the USA; thus, the current scientific evidence cannot be generalized to other countries.
Differences in Intervention Effects According to the Characteristics of the Participant
Overall, the results of video-based interventions had varying effects in terms of improving screening uptake compared to usual care conditions. Generally, interventions that included culturally and ethically tailored videos were more effective. Importantly, the effects of some interventions differed according to the characteristics of the individual. Champion et al.[49] and Gathirua-Mwangi et al.[46] reported significant effects on mammography screening of their tailored DVD interventions only in low-income African American women, but not in those with higher incomes. Similarly, Kreuter et al. [23] reported effects only in African American women with lower education. Latina women age 51–65 years were the only age group to have a significant difference in screening uptake for cervical cancer in a novella-style video intervention [41]. Wang et al. [7] also only found significant effects of a culturally targeted versus generic video only among low-acculturated Chinese American women, whereas the two videos did not lead to different screening uptake in high-acculturated women. They discussed that recently immigrated women and ones with limited English language abilities find it challenging to assimilate to the US cultural environment and face challenges such as access to care. Their culturally targeted video included an all-Chinese cast and many Chinese cultural features that may have helped low-acculturated women find it easier to relate to the video and, thus, their level of involvement increases. These results are promising, as they suggest that tailoring the content to the target audience may create effective strategies to help specific medically underserved populations. A meta-analysis concluded that mammography attendance is generally lower among immigrant and minority women compared to other women (46.2% vs 55.0%; odds ratio = 0.64) [52] and lack of knowledge is thought to be a key barrier to attending breast screening in Black, Asian and Minority Ethnic (BAME) women [53] but designing studies of barriers around race and ethnicity is not always appropriate because other demographic factors may play a role [54]. Gathirua-Mwangi et al. [46] reported that the low-income participants in their study paid significantly more attention to the DVD than higher-income women and, thus, their intervention may have been more successful in this group because the increased attention could maximize their learning. They further hypothesized that the narrative format of the DVD may also have played a role. Champion et al. [49] described that their DVD better impacted lower-income participants because the majority of female actors in the film were cast as women with lower incomes but also postulated that the reduced effect of the intervention in higher-income women may be due to DVDs being less engaging format for health education in this group than the internet, for example.
The Potential use of Video in Media and Social Media Campaigns
In the current review, we included RCTs that focused on videos and DVDs as education and training tools to increase knowledge and improve health literacy compared to usual care. However, these studies were conducted in rigorously controlled research conditions, and it may be of interest to see how they can be applied in more realistic settings. Specifically, they may have more far-reaching effects if used within a large media education campaign. In the “REACHing Vietnamese American Women: A Community Model for Promoting Cervical Cancer Screening (REACH)” study [55] used a media education campaign and a lay health worker outreach program to increase Vietnamese American women’s cervical cancer awareness, knowledge, and screening. They used Vietnamese-language television channels to broadcast television ads, along with radio and newspaper ads and concluded that media education campaigns can increase Vietnamese women’s awareness of the importance of pap tests, although it was higher when the intervention was combined with a lay health worker, the media campaign alone did increase pap test uptake. Due to the increasing use of social media, and its potential usage in delivering health education, it may be of interest to assess ways of adapting video interventions for use in social media, though this field is still relatively new. A review of social media and mHealth technologies for cancer screening found only four studies with social media interventions [56]. Some of the benefits of using social media for health communication include increased interactions with others and more available, shared, and tailored information, as well as peer/social/emotional support [57]. Further, adapting videos to social media platforms may be an important way of targeting hard-to-reach populations. For example, the use of social media and videos were recommended communication channels for breast cancer educational messages for young African American women in a study using informant interviews [57]. These women face health inequities that place them at greater risk for mortality from breast cancer [58]. Another study reported that a large proportion of medically underserved women are overdue for cervical cancer screening, but they regularly use social media and are willing to participate in social media-driven interventions [50].
Advantages of Video and DVD Interventions for Screening Promotion
There are several advantages to delivering health inequity interventions via video and DVD. First, delivery can be modified according to the characteristics of the individual, for example in different languages or with differing material according to age or health literacy levels. Second, they might be cost-effective in terms of reaching large amounts of people. Cost-effectiveness was not investigated here, as it was not the primary aim of our review, although it is of great relevance. Gathirua-Mwangi et al.´s [46] article reported that the DVD arm of their study was three times less expensive than a telephone intervention. In the ACCION program Lairson et al. [38] reported that, when delivered to a group, their video was the most cost-effective CRC screening promotion intervention, compared to other study arms that included a promotora. A further advantage of video and DVD interventions is that they have the potential to be delivered remotely, for example, several trials mailed DVDs and videos to participants [33, 47, 49]. This is of growing importance due to the COVID-19 pandemic, when worldwide screening rates for breast, colon, and cervical cancer were lower [28], and health inequities may be increased; for example, there was a lower likelihood of returning for breast cancer screening after COVID-19-related closures for people in higher poverty areas, those without health insurance, people who need an interpreter, and those with longer travel times [59]. Delivering interventions to promote cancer screening remotely can help to target specific groups during periods when public health restrictions are tightened and there are changes to routine medical services and a reduction in face-to-face health promotion programs.
Strengths and Limitations
The strength of the current study is the systematic, comprehensive literature search with thorough study selection and quality assessment. However, some limitations should be noted. We only found one study outside of the US and, thus, it may be difficult to generalize any findings to other settings, especially as the US has no universal healthcare coverage and has specific health inequity challenges associated with this. We also only reported studies in the literature that focused on cultural, ethnic, or economic inequity. It may be of interest to conduct a future systematic review specifically on interventions that target other groups that face cancer screening inequity such as incarcerated women [60] or LGBTQ persons [61]. It is also worth discussing that we only included RCTs that had a video-only intervention arm, as we wanted to focus on how tailoring the delivery may affect screening behaviour. Videos are often used in conjunction with other health promotion components such as group or individual health education and counselling, such as Byrd et al.‘s [40] study, which did not find differences in cervical cancer screening in participants in the video-only arm of their study compared to a more complex intervention arm that included training by a promotora, the instructional video, and a flip chart. Similar results were also reported for FIT uptake in a USA study [62]. So et al. [63] used an interesting approach that involved targeting older South Asian adults together with one of their younger family members in Hong Kong, which included culturally and linguistically relevant video clip, but this was used in conjunction with other components such as an instructor-led health presentation and health information booklet [63]. Although it was successful in increasing FIT screening uptake, it was not possible to isolate the effect of the video component as the intervention had multiple components. Further, we only included studies that had screening completion as an outcome, although there are studies that look instead at other related outcomes such as knowledge and attitudes regarding screening or intention to participate in screening in the future. For example, a study in the Netherlands reported that a culturally sensitive educational video targeting Turkish and Moroccan women resulted in more positive screening attitudes compared to the normal information brochure [64] but such studies were not included as we aimed to focus on concrete screening behaviours. Finally, it is important to consider that these trials include small, specific groups of people, and it is not clear whether they can actually lead to improvements in health equity from a larger perspective. These interventions need to be viewed from a broader standpoint that considers the wealth of changes needed to achieve a meaningful shift in equity, from a Health in All Policies approach that requires action from multiple sectors.
Future Research
It will be of interest to identify effective intervention strategies within European settings and other countries worldwide to assess differences in screening barriers and uptake between countries and whether these need different interventions and modalities to target them. Studies that can adapt already existing video-based interventions to other groups with high health inequity may also be relevant. More research is needed on specific subgroups, for example, young minority women, who face health inequities that place them at greater risk for mortality from breast cancer [58]. As discussed above, the cost-effectiveness of interventions is important, and all future trials should include a measurement of cost in addition to screening completion as an outcome. It is worth noting that culturally tailored video interventions have also been shown to increase illness knowledge in specific groups of people with cancer; for example, a pilot study in Amazonian women in treatment for cervical cancer reported increased knowledge about their illness. Thus, it will be of interest to extend studies on specific groups such as these to examine whether video interventions can be adapted also for the purpose of increasing screening uptake.
Conclusions
In conclusion, although results are mixed, video interventions to promote screening for breast, cervical, and colorectal cancer in this field have some positive results, especially if they are tailored. During and after the COVID-19 pandemic, further testing and development of effective intervention strategies that can be delivered remotely, such as videos, may provide relevant health promotion strategies that can help to reduce health inequities in cancer screening.
References
Nelson HD, Fu R, Cantor A, Pappas M, Daeges M, Humphrey L. Effectiveness of Breast Cancer Screening: Systematic Review and Meta-analysis to Update the 2009 U.S. Preventive Services Task Force Recommendation. Ann Intern Med. 2016;164(4):244–55. https://doi.org/10.7326/m15-0969.
Fitzpatrick-Lewis D, Ali MU, Warren R, Kenny M, Sherifali D, Raina P. Screening for Colorectal Cancer: A Systematic Review and Meta-Analysis. Clin Colorectal Cancer. 2016;15(4):298–313. https://doi.org/10.1016/j.clcc.2016.03.003.
Landy R, Pesola F, Castañón A, Sasieni P. Impact of cervical screening on cervical cancer mortality: estimation using stage-specific results from a nested case-control study. Br J Cancer. 2016;115(9):1140–6. https://doi.org/10.1038/bjc.2016.290.
Jun J, Nan X. Determinants of Cancer Screening Disparities Among Asian Americans: A Systematic Review of Public Health Surveys. J Cancer Educ. 2018;33(4):757–68. https://doi.org/10.1007/s13187-017-1211-x.
Consedine NS, Tuck NL, Ragin CR, Spencer BA. Beyond the black box: a systematic review of breast, prostate, colorectal, and cervical screening among native and immigrant African-descent Caribbean populations. J Immigr Minor Health. 2015;17(3):905–24. https://doi.org/10.1007/s10903-014-9991-0.
Johnson CE, Mues KE, Mayne SL, Kiblawi AN. Cervical cancer screening among immigrants and ethnic minorities: a systematic review using the Health Belief Model. J Low Genit Tract Dis. 2008;12(3):232–41. https://doi.org/10.1097/LGT.0b013e31815d8d88.
Mottram R, Knerr WL, Gallacher D, Fraser H, Al-Khudairy L, Ayorinde A, et al. Factors associated with attendance at screening for breast cancer: a systematic review and meta-analysis. BMJ Open. 2021;11(11):e046660. https://doi.org/10.1136/bmjopen-2020-046660.
Smith D, Thomson K, Bambra C, Todd A. The breast cancer paradox: A systematic review of the association between area-level deprivation and breast cancer screening uptake in Europe. Cancer Epidemiol. 2019;60:77–85. https://doi.org/10.1016/j.canep.2019.03.008.
Wang H, Roy S, Kim J, Farazi PA, Siahpush M, Su D. Barriers of colorectal cancer screening in rural USA: a systematic review. Rural Remote Health. 2019;19(3):5181. https://doi.org/10.22605/rrh5181.
Rogers CR, Mitchell JA, Franta GJ, Foster MJ, Shires D. Masculinity, Racism, Social Support, and Colorectal Cancer Screening Uptake Among African American Men: A Systematic Review. Am J Mens Health. 2017;11(5):1486–500. https://doi.org/10.1177/1557988315611227.
Lau J, Lim TZ, Jianlin Wong G, Tan KK. The health belief model and colorectal cancer screening in the general population: A systematic review. Prev Med Rep. 2020;20:101223. https://doi.org/10.1016/j.pmedr.2020.101223.
Vrinten C, Gallagher A, Waller J, Marlow LAV. Cancer stigma and cancer screening attendance: a population based survey in England. BMC Cancer. 2019;19(1):566. https://doi.org/10.1186/s12885-019-5787-x.
Mohan G, Chattopadhyay S. Cost-effectiveness of Leveraging Social Determinants of Health to Improve Breast, Cervical, and Colorectal Cancer Screening: A Systematic Review. JAMA Oncol. 2020;6(9):1434–44. https://doi.org/10.1001/jamaoncol.2020.1460.
Mehta SJ, Oyalowo A, Reitz C, Dean O, McAuliffe T, Asch DA, et al. Text messaging and lottery incentive to improve colorectal cancer screening outreach at a community health center: A randomized controlled trial. Preventive Medicine Reports. 2020;19:101114. https://doi.org/10.1016/j.pmedr.2020.101114.
Mehta SJ, Pepe RS, Gabler NB, Kanneganti M, Reitz C, Saia C, et al. Effect of Financial Incentives on Patient Use of Mailed Colorectal Cancer Screening Tests: A Randomized Clinical Trial. JAMA Netw Open. 2019;2(3):e191156. https://doi.org/10.1001/jamanetworkopen.2019.1156.
Mehta SJ, Reitz C, Niewood T, Volpp KG, Asch DA. Effect of Behavioral Economic Incentives for Colorectal Cancer Screening in a Randomized Trial. Clin Gastroenterol Hepatol. 2021;19(8):1635-41.e1. https://doi.org/10.1016/j.cgh.2020.06.047.
Coronado GD, Beresford SAA, McLerran D, Jimenez R, Patrick DL, Ornelas I, et al. Multilevel Intervention Raises Latina Participation in Mammography Screening: Findings from (sic)Fortaleza Latina! Cancer Epidemiol Biomark Prev. 2016;25(4):584–92. https://doi.org/10.1158/1055-9965.Epi-15-1246.
Ahmed NU, Haber G, Semenya KA, Hargreaves MK. Randomized controlled trial of mammography intervention in insured very low-income women. Cancer Epidemiol Biomark Prev. 2010;19(7):1790–8. https://doi.org/10.1158/1055-9965.EPI-10-0141.
Sadler GR, Beerman PR, Lee K, Hung J, Nguyen H, Cho J, et al. Promoting Breast Cancer Screening Among Asian American Women: the Asian Grocery Store-Based Cancer Education Program. J Cancer Educ. 2012;27(4):612–7. https://doi.org/10.1007/s13187-012-0419-z.
West DS, Greene P, Pulley L, Kratt P, Gore S, Weiss H, et al. Stepped-care, community clinic interventions to promote mammography use among low-income rural African American women. Health Educ Behav. 2004;31(4 Suppl):29s–44s. https://doi.org/10.1177/1090198104266033.
Cuaresma CF, Sy AU, Nguyen TT, Ho RCS, Gildengorin GL, Tsoh JY, et al. Results of a lay health education intervention to increase colorectal cancer screening among Filipino Americans: A cluster randomized controlled trial. Cancer. 2018;124:1535–42. https://doi.org/10.1002/cncr.31116.
Horne HN, Phelan DF, Pollack CE, Markakis D, Wenzel J, Ahmed S, et al. Effect of patient navigation on colorectal cancer screening in a community-based randomized controlled trial of urban African American adults. Cancer Causes Control. 2015;26:239–46. https://doi.org/10.1007/s10552-014-0505-0.
Kreuter MW, Holmes K, Alcaraz K, Kalesan B, Rath S, Richert M, et al. Comparing narrative and informational videos to increase mammography in low-income African American women. Patient Educ Couns. 2010;81(SUPPL. 1):S6–14. https://doi.org/10.1016/j.pec.2010.09.008.
Murphy ST, Frank LB, Chatterjee JS, Moran MB, Zhao N, Amezola de Herrera P, et al. Comparing the Relative Efficacy of Narrative vs Nonnarrative Health Messages in Reducing Health Disparities Using a Randomized Trial. Am J Public Health. 2015;105(10):2117–23. https://doi.org/10.2105/ajph.2014.302332.
Gabel P, Edwards A, Kirkegaard P, Larsen MB, Andersen B. The LEAD trial-The effectiveness of a decision aid on decision making among citizens with lower educational attainment who have not participated in FIT-based colorectal cancer screening in Denmark: A randomised controlled trial. Patient Educ Couns. 2020;103(2):359–68. https://doi.org/10.1016/j.pec.2019.08.029.
Lee EE, Brecht ML, Park H, Lee J, Oh KM. Web-Based Study for Improving Mammography Among Korean American Women. J Cancer Educ. 2017;32(2):257–63. https://doi.org/10.1007/s13187-015-0920-2.
Rawl SM, Skinner CS, Perkins SM, Springston J, Wang HL, Russell KM, et al. Computer-delivered tailored intervention improves colon cancer screening knowledge and health beliefs of African-Americans. Health Educ Res. 2012;27(5):868–85. https://doi.org/10.1093/her/cys094.
Mayo M, Potugari B, Bzeih R, Scheidel C, Carrera C, Shellenberger RA. Cancer Screening During the COVID-19 Pandemic: A Systematic Review and Meta-analysis. Mayo Clin Proc Innov Qual Outcomes. 2021;5(6):1109–17. https://doi.org/10.1016/j.mayocpiqo.2021.10.003.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Bmj. 2021;372:n71. https://doi.org/10.1136/bmj.n71.
Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. Bmj. 2011;343:d5928. https://doi.org/10.1136/bmj.d5928.
Avis NE, Smith KW, Link CL, Goldman MB. Increasing mammography screening among women over age 50 with a videotape intervention. Prev Med. 2004;39(3):498–506. https://doi.org/10.1016/j.ypmed.2004.05.024.
Bartholomew K, Zhou L, Crengle S, Buswell E, Buckley A, Sandiford P. A targeted promotional DVD fails to improve Māori and Pacific participation rates in the New Zealand bowel screening pilot: results from a pseudo-randomised controlled trial. BMC Public Health. 2019;19(1):1245. https://doi.org/10.1186/s12889-019-7582-7.
Cameron KA, Persell SD, Brown T, Thompson J, Baker DW. Patient outreach to promote colorectal cancer screening among patients with an expired order for colonoscopy: a randomized controlled trial. Arch Intern Med. 2011;171(7):642–6. https://doi.org/10.1001/archinternmed.2010.468.
Davis TC, Berkel HJ, Arnold CL, Nandy I, Jackson RH, Murphy PW. Intervention to increase mammography utilization in a public hospital. J Gen Intern Med. 1998;13(4):230–3. https://doi.org/10.1046/j.1525-1497.1998.00072.x.
Fernández ME, Savas LS, Carmack CC, Chan W, Lairson DR, Byrd TL, et al. A randomized controlled trial of two interventions to increase colorectal cancer screening among Hispanics on the Texas-Mexico border. Cancer Causes Control. 2015;26(1):1–10. https://doi.org/10.1007/s10552-014-0472-5.
Gwede CK, Sutton SK, Chavarria EA, Gutierrez L, Abdulla R, Christy SM, et al. A culturally and linguistically salient pilot intervention to promote colorectal cancer screening among Latinos receiving care in a Federally Qualified Health Center. Health Educ Res. 2019;34(3):310–20. https://doi.org/10.1093/her/cyz010.
Hoffman AS, Lowenstein LM, Kamath GR, Housten AJ, Leal VB, Linder SK, et al. An entertainment-education colorectal cancer screening decision aid for African American patients: A randomized controlled trial. Cancer. 2017;123(8):1401–8. https://doi.org/10.1002/cncr.30489.
Lairson DR, Kim J, Byrd T, Salaiz R, Shokar NK. Cost-Effectiveness of Community Interventions for Colorectal Cancer Screening: Low-Income Hispanic Population. Health Promot Pract. 2018;19(6):863–72. https://doi.org/10.1177/1524839917750815.
Shokar NK, Byrd T, Salaiz R, Flores S, Chaparro M, Calderon-Mora J, et al. Against colorectal cancer in our neighborhoods (ACCION): A comprehensive community-wide colorectal cancer screening intervention for the uninsured in a predominantly Hispanic community. Prev Med. 2016;91:273–80. https://doi.org/10.1016/j.ypmed.2016.08.039.
Byrd TL, Wilson KM, Smith JL, Coronado G, Vernon SW, Fernandez-Esquer ME, et al. AMIGAS: a multicity, multicomponent cervical cancer prevention trial among Mexican American women. Cancer. 2013;119(7):1365–72. https://doi.org/10.1002/cncr.27926.
Calderón-Mora J, Alomari A, Shokar N (2022) Comparison of Narrative Video and Flipchart Presentation to Promote Cervical Cancer Screening Among Latinas Along the Border. Health Educ Behav 10901981221074918. https://doi.org/10.1177/10901981221074918.
Rivers SE, Salovey P, Pizarro DA, Pizarro J, Schneider TR. Message framing and pap test utilization among women attending a community health clinic. J Health Psychol. 2005;10(1):65–77. https://doi.org/10.1177/1359105305048556.
Taylor VM, Hislop TG, Jackson JC, Tu SP, Yasui Y, Schwartz SM, et al. A randomized controlled trial of interventions to promote cervical cancer screening among Chinese women in North America. J Natl Cancer Inst. 2002;94(9):670–7. https://doi.org/10.1093/jnci/94.9.670.
Thompson B, Carosso EA, Jhingan E, Wang L, Holte SE, Byrd TL, et al. Results of a randomized controlled trial to increase cervical cancer screening among rural Latinas. Cancer. 2017;123(4):666–74. https://doi.org/10.1002/cncr.30399.
Taylor KL, Davis JL 3rd, Turner RO, Johnson L, Schwartz MD, Kerner JF, et al. Educating African American men about the prostate cancer screening dilemma: a randomized intervention. Cancer Epidemiol Biomarkers Prev. 2006;15(11):2179–88. https://doi.org/10.1158/1055-9965.Epi-05-0417.
Gathirua-Mwangi WG, Monahan PO, Stump T, Rawl SM, Skinner CS, Champion VL. Mammography Adherence in African-American Women: Results of a Randomized Controlled Trial. Ann Behav Med. 2016;50(1):70–8. https://doi.org/10.1007/s12160-015-9733-0.
Wang JH, Schwartz MD, Brown RL, Maxwell AE, Lee MM, Adams IF, et al. Results of a randomized controlled trial testing the efficacy of a culturally targeted and a generic video on mammography screening among chinese-american immigrants. Cancer Epidemiol Biomarkers Prev. 2012;21(11):1923–32. https://doi.org/10.1158/1055-9965.Epi-12-0821.
Champion VL, Rawl SM, Bourff SA, Champion KM, Smith LG, Buchanan AH, et al. Randomized trial of DVD, telephone, and usual care for increasing mammography adherence. J Health Psychol. 2016;21(6):916–26. https://doi.org/10.1177/1359105314542817.
Asare M, Lanning BA, Isada S, Rose T, Mamudu HM. Feasibility of Utilizing Social Media to Promote HPV Self-Collected Sampling among Medically Underserved Women in a Rural Southern City in the United States (U.S.). Int J Environ Res Public Health. 2021;18(20):10820. https://doi.org/10.3390/ijerph182010820.
Jerant A, Kravitz RL, Sohler N, Fiscella K, Romero RL, Parnes B, et al. Sociopsychological tailoring to address colorectal cancer screening disparities: a randomized controlled trial. Ann Fam Med. 2014;12(3):204–14. https://doi.org/10.1370/afm.1623.
Aragones A, Schwartz MD, Shah NR, Gany FM. A randomized controlled trial of a multilevel intervention to increase colorectal cancer screening among Latino immigrants in a primary care facility. J Gen Intern Med. 2010;25(6):564–7. https://doi.org/10.1007/s11606-010-1266-4.
Bhargava S, Moen K, Qureshi SA, Hofvind S. Mammographic screening attendance among immigrant and minority women: a systematic review and meta-analysis. Acta Radiol. 2018;59(11):1285–91. https://doi.org/10.1177/0284185118758132.
Baird J, Yogeswaran G, Oni G, Wilson EE. What can be done to encourage women from Black, Asian and minority ethnic backgrounds to attend breast screening? A qualitative synthesis of barriers and facilitators. Public Health. 2021;190:152–9. https://doi.org/10.1016/j.puhe.2020.10.013.
Miller BC, Bowers JM, Payne JB, Moyer A. Barriers to mammography screening among racial and ethnic minority women. Soc Sci Med. 2019;239:112494. https://doi.org/10.1016/j.socscimed.2019.112494.
Lam TK, McPhee SJ, Mock J, Wong C, Doan HT, Nguyen T, et al. Encouraging Vietnamese-American women to obtain Pap tests through lay health worker outreach and media education. J Gen Intern Med. 2003;18(7):516–24. https://doi.org/10.1046/j.1525-1497.2003.21043.x.
Ruco A, Dossa F, Tinmouth J, Llovet D, Jacobson J, Kishibe T, et al. Social Media and mHealth Technology for Cancer Screening: Systematic Review and Meta-analysis. J Med Internet Res. 2021;23(7):e26759. https://doi.org/10.2196/26759.
Huq MR, Woodard N, Okwara L, McCarthy S, Knott CL. Recommendations for breast cancer education for African American women below screening age. Health Educ Res. 2022;36(5):530–40. https://doi.org/10.1093/her/cyab033.
Kidd AD, Colbert AM, Jatoi I. Mammography: review of the controversy, health disparities, and impact on young african american women. Clin J Oncol Nurs. 2015;19(3):E52–8. https://doi.org/10.1188/15.Cjon.E52-e58.
Miller MM, Meneveau MO, Rochman CM, Schroen AT, Lattimore CM, Gaspard PA, et al. Impact of the COVID-19 pandemic on breast cancer screening volumes and patient screening behaviors. Breast Cancer Res Treat. 2021;189(1):237–46. https://doi.org/10.1007/s10549-021-06252-1.
Kelly PJ, Allison M, Ramaswamy M. Cervical cancer screening among incarcerated women. PLoS One. 2018;13(6):e0199220. https://doi.org/10.1371/journal.pone.0199220.
Ceres M, Quinn GP, Loscalzo M, Rice D. Cancer Screening Considerations and Cancer Screening Uptake for Lesbian, Gay, Bisexual, and Transgender Persons. Semin Oncol Nurs. 2018;34(1):37–51. https://doi.org/10.1016/j.soncn.2017.12.001.
Christy SM, Sutton SK, Abdulla R, Boxtha C, Gonzalez P, Cousin L, et al. A multilevel, low literacy dual language intervention to promote colorectal cancer screening in community clinics in Florida: A randomized controlled trial. Prev Med. 2022;158:107021. https://doi.org/10.1016/j.ypmed.2022.107021.
So WKW, Chan DNS, Law BMH, Choi KC, Krishnasamy M, Chan CWH. Effect of a family-based multimedia intervention on the uptake of faecal immunohistochemical test among South Asian older adults: A cluster-randomised controlled trial. Int J Nurs Stud. 2022;132:104254. https://doi.org/10.1016/j.ijnurstu.2022.104254.
Hamdiui N, Stein ML, van Steenbergen J, Crutzen R, Bouman M, Khan A, et al. Evaluation of a Web-Based Culturally Sensitive Educational Video to Facilitate Informed Cervical Cancer Screening Decisions Among Turkish- and Moroccan-Dutch Women Aged 30 to 60 Years: Randomized Intervention Study. J Med Internet Res. 2022;24(10):e35962. https://doi.org/10.2196/35962.
Funding
The writing of this paper was commercially funded by Viatris in the form of a payment for professional scientific writing services to Oliba, Rome, Italy. No products or services of Viatris have been discussed or promoted within this manuscript.
Author information
Authors and Affiliations
Contributions
ARP, MS, JMV, SD, SW, and JvV defined the objectives of the paper. JvV and ARP conducted the literature search and data extraction. All authors interpreted the results of the studies within the context of the aims. ARP and JvV prepared the draft. All authors critically revised the article and approved the final version.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent to Publish
Not applicable.
Competing Interests
ARP, SD, SW and JvV are employees of Viatris. MS and JMV have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix 1
Table
Appendix 2
Risk of bias tables—characteristics of included studies.
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Table
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Richardson-Parry, A., Silva, M., Valderas, J.M. et al. Video Interventions for Reducing Health Inequity in Cancer Screening Programmes: a Systematic Review. J. Racial and Ethnic Health Disparities (2023). https://doi.org/10.1007/s40615-023-01749-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40615-023-01749-5