Abstract
Background
Alkaline phosphatase has been found on neuronal membranes and plasma alkaline phosphatase (ALP) activity increases during brain injury and cerebrovascular diseases, suggesting that its levels may reflect the neuronal loss. It is known that ALP is higher in subjects affected by Alzheimer’s dementia and inversely correlated with cognitive functions. No study has investigated the relationship between ALP and cognitive functions in old-age subject with pre-clinical cognitive impairment.
Methods
This is a cross-sectional study with data gathered from the ReGAl 2.0 project (Rete Geriatrica Alzheimer-Geriatric Network on Alzheimer’s disease), a large Italian multicentric clinical-based study. A cohort of 209 old-age subjects healthy controls (HC), Subjective cognitive decline (SCD), and Mild Cognitive Impairment (MCI) was included in the study. Cognitive performances were assessed with a large neuropsychological battery. The same day, serum alkaline phosphatase activity was measured in all subjects.
Results
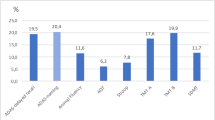
We found that the SCD group had significantly higher ALP levels as compared with HC (p = 0.001). Among all neuropsychological tests, in all population ALP levels negatively correlated with scores at attentional matrices (r = − 0.243, p = 0.002), Digit Span Forward (r = − 0.241, p = 0.003) and Letter Fluency Test (r = − 0.196, p = 0.044). Attentional Matrices (r = − 0.208, p = 0.014) and Letter Fluency Test (r = − 0.229, p = 0.019) remained significantly correlated with ALP even after controlling for gender. In the SCD group, only the Attentional Matrices significantly and negatively correlated with ALP (r = − 0.344 p = 0.035), while no significant correlations were found in HC or MCI.
Conclusions
Results indicate that serum alkaline phosphatase activity is increased in SCD and inversely correlates with cognitive functions. Further studies are needed to investigate the role of ALP in the progression to AD.


Similar content being viewed by others
References
Cheng Y-W, Chen T-F, Chiu M-J (2017) From mild cognitive impairment to subjective cognitive decline: conceptual and methodological evolution. Neuropsychiatr Dis Treat 13:491–498. https://doi.org/10.2147/NDT.S123428
Jessen F, Amariglio RE, van Boxtel M et al (2014) A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimer’s Dement 10:844–852. https://doi.org/10.1016/j.jalz.2014.01.001
Mendonça MD, Alves L, Bugalho P (2016) From Subjective Cognitive Complaints to Dementia. Am J Alzheimer’s Dis Other Demen 31:105–114. https://doi.org/10.1177/1533317515592331
Apostolova LG (2016) Alzheimer Disease. Continuum (Minneap Minn) 22:419–34. https://doi.org/10.1212/CON.0000000000000307
Fonta C, Négyessy L (2015) Tissue-nonspecific alkaline phosphatase (TNAP). Springer, Netherlands
Cacabelos R, Fernández-Novoa L, Corzo L et al (2004) Phenotypic profiles and functional genomics in Alzheimer’s disease and in dementia with a vascular component. Neurol Res 26:459–480. https://doi.org/10.1179/016164104225017677
Díaz-Hernández M, Gómez-Ramos A, Rubio A et al (2010) Tissue-nonspecific alkaline phosphatase promotes the neurotoxicity effect of extracellular tau. J Biol Chem 285:32539–32548. https://doi.org/10.1074/jbc.M110.145003
Kellett KA, Williams J, Vardy ER et al (2011) Plasma alkaline phosphatase is elevated in Alzheimer’s disease and inversely correlates with cognitive function. Int J Mol Epidemiol Genet 2:114–121
Vardy ERLC, Kellett KAB, Cocklin SL, Hooper NM (2012) Alkaline Phosphatase Is Increased in both Brain and Plasma in Alzheimer’s Disease. Neurodegener Dis 9:31–37. https://doi.org/10.1159/000329722
Bessi V, Mazzeo S, Padiglioni S et al (2018) From Subjective Cognitive Decline to Alzheimer’s Disease: The Predictive Role of Neuropsychological Assessment, Personality Traits, and Cognitive Reserve. A 7-Year Follow-Up Study. J Alzheimer’s Dis 63:1523–1535. https://doi.org/10.3233/JAD-171180
Boccardi V, Conestabile Della Staffa M, Baroni M et al (2017) Prevalence and Correlates of Behavioral Disorders in Old Age Subjects with Cognitive Impairment: Results from the ReGAl Project. J Alzheimers Dis 60:1275–1283. https://doi.org/10.3233/JAD-170494
Albert MS, DeKosky ST, Dickson D et al (2011) The diagnosis of mild cognitive impairment due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimer’s Dement 7:270–279. https://doi.org/10.1016/j.jalz.2011.03.008
Petersen RC (2004) Mild cognitive impairment as a diagnostic entity. J Intern Med 256:183–194. https://doi.org/10.1111/j.1365-2796.2004.01388.x
Folstein MF, Folstein SE, McHugh PR (1975) "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Hughes CP, Berg L, Danziger WL et al (1982) A new clinical scale for the staging of dementia. Br J Psychiatry 140:566–572
Mariani E, Monastero R, Ercolani S et al (2008) Influence of comorbidity and cognitive status on instrumental activities of daily living in amnestic mild cognitive impairment: results from the ReGAl project. Int J Geriatr Psychiatry 23:523–530. https://doi.org/10.1002/gps.1932
Yesavage JA, Sheikh JI (1986) 9/Geriatric Depression Scale (GDS). Clin Gerontol 5:165–173. https://doi.org/10.1300/J018v05n01_09
Katz S, Ab F, Rw M, Al Et (1963) Studies Of Illness In The Aged. The Index Of Adl: A Standardized Measure Of Biological And Psychosocial Function. JAMA 185:914–919
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9:179–186
Neuropsychological assessment, 4th ed. - PsycNET. https://psycnet.apa.org/record/2004-16637-000. Accessed 2 Apr 2020
Kessels RP, van den Berg E, Ruis C, Brands AM (2008) The Backward Span of the Corsi Block-Tapping Task and Its Association with the WAIS-III Digit Span. Assessment 15:426–434. https://doi.org/10.1177/1073191108315611
Horner MD, Teichner G, Kortte KB, Harvey RT (2002) Construct validity of the Babcock Story Recall Test. Appl Neuropsychol 9:114–116. https://doi.org/10.1207/S15324826AN0902_7
Carlesimo GA, Caltagirone C, Gainotti G et al (1996) The mental deterioration battery: Normative data, diagnostic reliability and qualitative analyses of cognitive impairment. Eur Neurol 36:378–384. https://doi.org/10.1159/000117297
Négyessy L, Xiao J, Kántor O et al (2011) Layer-specific activity of tissue non-specific alkaline phosphatase in the human neocortex. Neuroscience 172:406–418. https://doi.org/10.1016/j.neuroscience.2010.10.049
Street SE, Kramer NJ, Walsh PL et al (2013) Tissue-nonspecific alkaline phosphatase acts redundantly with PAP and NT5E to generate adenosine in the dorsal spinal cord. J Neurosci 33:11314–11322. https://doi.org/10.1523/Jneurosci.0133-13.2013
Mazzeo S, Padiglioni S, Bagnoli S et al (2019) The dual role of cognitive reserve in subjective cognitive decline and mild cognitive impairment: a 7-year follow-up study. J Neurol 266:487–497. https://doi.org/10.1007/s00415-018-9164-5
Stewart R, Godin O, Crivello F et al (2011) Longitudinal neuroimaging correlates of subjective memory impairment: 4-year prospective community study. Br J Psychiatry 198:199–205. https://doi.org/10.1192/bjp.bp.110.078683
Derouesné C, Dealberto MJ, Boyer P et al (1993) Empirical evaluation of the ‘Cognitive Difficulties Scale’ for assessment of memory complaints in general practice: A study of 1628 cognitively normal subjects aged 45–75 years. Int J Geriatr Psychiatry 8:599–607. https://doi.org/10.1002/gps.930080712
Yamashita M, Sasaki M, Mii K et al (1989) Measurement of Serum Alkaline Phosphatase Isozyme I in Brain-damaged Patients. Neurol Med Chir (Tokyo) 29:995–998. https://doi.org/10.2176/nmc.29.995
Silveri MC, Reali G, Jenner C, Puopolo M (2007) Attention and Memory in the Preclinical Stage of Dementia. J Geriatr Psychiatry Neurol 20:67–75. https://doi.org/10.1177/0891988706297469
Acknowledgements
ReGAl 2.0 study group: Carlo Alberto Defanti, Cosimo Dentizzi, Antonio Gambardella, Daniela Mari, Fiammetta Monacelli, Fabio Monzani, Enrico Mossello, Graziano Onder, Giovanni Scala. Coordinating center: Institute of Gerontology and Geriatrics, Santa Maria della Misericordia Hospital, Department of Medicine, University of Perugia, Italy (Patrizia Mecocci, Virginia Boccardi). Collecting centers: Carlo Alberto Defanti (Fondazione Europea Ricerca Biomedica FERB, Centro Alzheimer, Ospedale Briolini, Gazzaniga, Bergamo, Italy); Cosimo Dentizzi (Centro Diurno Alzheimer, Centro Alzheimer ASREM Campobasso, Italy); Antonio Gambardella (Department of Medical, Surgical, Neurological, Metabolic and Aging Sciences, University of Campania "Luigi Vanvitelli", Napoli, Italy); Daniela Mari (Geriatric Unit, Fondazione IRCCS Ca' Granda Ospedale Maggiore Policlinico, Milano, Italy); Fiammetta Monacelli (Geriatrics Clinic, Department of Internal Medicine and Medical Specialties DIMI, University of Genova, Genova, Italy); Fabio Monzani (Geriatrics Unit, Department of Clinical and Experimental Medicine, University of Pisa, Pisa, Italy); Enrico Mossello (Department of Experimental and Clinical Medicine, Research Unit of Medicine of Aging, University of Firenze, Firenze Italy); Graziano Onder (Centro di Medicina dell'Invecchiamento, Department of Geriatrics, Università Cattolica del Sacro Cuore di Roma and IRCCS Fondazione Policlinico "A. Gemelli", Roma, Italy); Giovanni Scala (Poliambulatorio ASL Roma 2, Roma, Italy). Webmaster: Arcangelo Biancardi.
Funding
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The study is carried in accordance with the 1964 Helsinki Declaration and its later amendments and with the ethical standards of the institutional ethics committee, and was approved by the ethics committee of the University of Perugia, Perugia, Italy.
Informed consent
All subjects provided written informed consent to participate in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Boccardi, V., Bubba, V., Murasecco, I. et al. Serum alkaline phosphatase is elevated and inversely correlated with cognitive functions in subjective cognitive decline: results from the ReGAl 2.0 project. Aging Clin Exp Res 33, 603–609 (2021). https://doi.org/10.1007/s40520-020-01572-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-020-01572-6