Abstract
Background
Nutrition guidance for athletes must consider a range of variables to effectively support individuals in meeting energy and nutrient needs. Resistance exercise is a widely adopted training method in athlete preparation and rehabilitation and therefore is one such variable that will influence nutrition guidance. Given its prominence, the capacity to meaningfully quantify resistance exercise energy expenditure will assist practitioners and researchers in providing nutrition guidance. However, the significant contribution of anaerobic metabolism makes quantifying energy expenditure of resistance exercise challenging.
Objective
The aim of this scoping review was to investigate the methods used to assess resistance exercise energy expenditure.
Methods
A literature search of Medline, SPORTDiscus, CINAHL and Web of Science identified studies that included an assessment of resistance exercise energy expenditure. Quality appraisal of included studies was performed using the Rosendal Scale.
Results
A total of 19,867 studies were identified, with 166 included after screening. Methods to assess energy expenditure included indirect calorimetry (n = 136), blood lactate analysis (n = 25), wearable monitors (n = 31) and metabolic equivalents (n = 4). Post-exercise energy expenditure was measured in 76 studies. The reported energy expenditure values varied widely between studies.
Conclusions
Indirect calorimetry is widely used to estimate energy expenditure. However, given its limitations in quantifying glycolytic contribution, indirect calorimetry during and immediately following exercise combined with measures of blood lactate are likely required to better quantify total energy expenditure. Due to the cumbersome equipment and technical expertise required, though, along with the physical restrictions the equipment places on participants performing particular resistance exercises, indirect calorimetry is likely impractical for use outside of the laboratory setting, where metabolic equivalents may be a more appropriate method.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Indirect calorimetry is used widely but is limited in quantifying the glycolytic cost of resistance exercise. |
Indirect calorimetry measures during and immediately following resistance exercise in combination with blood lactate measures before and after exercise may be the most valid means of estimating total energy expenditure of resistance exercise. Metabolic equivalents may be the easiest tool to implement in the field. |
Future research should aim to develop a more valid system to quantify the glycolytic contribution to resistance exercise and better understand how resistance exercise energy expenditure is currently estimated by practitioners in the field. |
1 Introduction
Resistance training can increase strength and power while reducing injury risk, and has been established as an essential auxiliary training tool in elite [1, 2], amateur [3], young [4], old [5], individual [6, 7] and team sport athletes [1, 2]. Furthermore, in sports such as bodybuilding, Olympic weightlifting, powerlifting and CrossFit, resistance exercise can be considered a primary mode of training [7,8,9,10]. Outside of a performance context, resistance exercise is used as an essential tool in athlete rehabilitation [11]. The often-periodised nature of competition preparation dictates variation in training characteristics based on the goals of each cycle. From a resistance exercise perspective, such variation would involve adjustments in training frequency (sessions per week), load (percentage of repetition maximum), volume (sets and repetitions) and movement velocity, amongst others. Such characteristics would therefore influence the overall workload experienced by the athlete, requiring a consideration of complementary facets of overall health and performance including nutrition.
The dietary requirements of athletes are primarily influenced by daily training load, but also impacted by other variables including health, injury status and environment [12, 13]. The variable nature of these factors within and across training phases and competition means sports dietitians must be dynamic with their nutrition support, providing customised direction around energy and nutrient requirements. Ultimately, energy intake requirements will be determined by the energy expended through resting metabolic rate and non-exercise activity energy expenditure, and, specifically in the context of the athlete, the hugely variable energy expenditure of exercise [14, 15]. As such, it is pertinent for sports dietitians to gather and assess athlete and training data to provide accurate guidance around dietary energy requirements for individual athletes. In particular, capturing estimates of exercise energy expenditure will support practitioners in providing this dietary energy guidance [12].
The reference method for quantifying total energy expenditure is direct calorimetry, but this is largely unavailable to researchers and practitioners [16]. Doubly labelled water, considered the reference measure for free living total energy expenditure, has been used to quantify the energy expenditure of various athlete cohorts [17,18,19,20]. However, this technique is limited in day-to-day practice due to costs and accessibility, while also failing to determine daily fluctuations in expenditure and lacking the capacity to quantify the energy expenditure of individual exercise sessions [15]. Physiological and metabolic complications that can result from imbalances in energy intake and the energy expenditure of exercise (low energy availability) include reductions in muscle protein synthesis and resting metabolic rate, as well as menstrual dysfunction, hormonal disruption and increased injury risk [21, 22]. Emerging evidence also suggests potential detrimental outcomes of acute imbalances between intake and expenditure within a day [23,24,25]. These physiological and metabolic complications demonstrate a clear justification for quantifying the energy expenditure of exercise [26]. As such, tools that allow this measurement are warranted. Given the prevalence of resistance exercise in athlete preparation, and by extension its contribution to exercise energy expenditure, the capacity to meaningfully quantify the energy expenditure of a resistance exercise session specifically will assist practitioners in providing energy requirement guidance. This will support athlete health and performance by optimising energy intake within and between days.
Indirect calorimetry is typically used to measure the energy cost of continuous, aerobic-based exercise. This technique relies on the subject achieving steady-state conditions and most of the energy being expended via aerobic energy pathways. Unlike aerobic exercise, though, resistance exercise depends on the significant contribution of anaerobic metabolism [27, 28]. Furthermore, the typically high-intensity, short-duration characteristics of a resistance exercise effort (i.e. a single set) means steady-state is not achieved [29]. As such, values of energy expenditure estimated through indirect calorimetry likely neglect a significant fraction of the energy cost of resistance exercise [29]. Depending on training variables, this anaerobic fraction may be over 40% of energy expenditure [30]. Attempts have been made to quantify the anaerobic contribution to resistance exercise energy expenditure. Blood lactate changes from pre- to post-exercise have been used to estimate the glycolytic energy cost [30, 31], with an energy equivalent used per unit increase in blood lactate concentration [32]. This method may be limited given that blood lactate is only an approximation of muscle blood lactate production. Indirect calorimetry during recovery periods between and immediately after exercise sets captures the energy supplied by the phosphagen system via measurement of the fast phase of excess oxygen uptake [33, 34]. Estimations of total energy expenditure have also been made on the basis of the Compendium of Physical Activities, with metabolic equivalent (MET) values of 3.5–6.0 used depending on the nature of the resistance exercise [35], while regression analyses have been performed to predict energy expenditure factoring in participant and training variables [36]. Both MET values and regression analyses are limited, though, by their dependence on indirect calorimetry to estimate energy expenditure, and resistance exercise MET values fail to account for disparity in energy expenditure depending on variability in muscle mass activation. Despite each of these methods being recognised, the range of techniques used to date suggests no accepted standard for quantifying the energy expenditure of resistance exercise. Further exploration of this field is therefore needed to establish recommendations for the accurate quantification of resistance exercise energy expenditure.
Factors within a resistance exercise session likely contribute to overall energy expenditure. The intensity of the exercise will influence the contribution of anaerobic systems to metabolic output [27], as will the proximity to failure, while movement velocity also influences energy expenditure [37]. Unlike continuous exercise, the high-intensity, intermittent nature of resistance exercise will result in significant energy expenditure during recovery periods (i.e. between sets and exercises) despite no external work being performed, largely attributed to the replenishment of high energy phosphates [28, 30]. The specific exercise itself also influences energy expenditure. Exercises activating larger amounts of muscle mass will inherently result in greater expenditure than those utilising smaller amounts of muscle mass, across a range of lifting intensities. For example, single sets of half squat and biceps curl performed to momentary failure at 80% one repetition maximum resulted in expenditures of 150.9 ± 20.9 and 35.8 ± 9.5 kJ/min, respectively [38]. The capacity to quantify total energy cost of a resistance exercise session will therefore require a system that considers these factors.
Given the prominent incorporation of resistance exercise in athlete programming, from both performance and rehabilitation perspectives, along with the importance of dietary guidance centred around individual energy and nutrient needs, accurately quantifying the energy cost of resistance exercise is warranted. Such a quantification would allow practitioners to better service athletes in meeting their dietary, health and performance goals. Researchers would also benefit through increasing the capacity to quantify the energy cost of training interventions, allowing a more accurate link between training variables and physiological outcomes. In addition, the capacity to quantify resistance exercise energy expenditure would also allow for a more accurate assessment of energy availability, given the critical role of quantifying energy expenditure of exercise. Therefore, the aim of this scoping review is to investigate the methods used to assess the energy expenditure of resistance exercise. This will support practitioners and researchers in estimating the energy cost of resistance exercise, and therefore enable more individual guidance around energy and nutrient needs.
2 Methods
Reporting of this scoping review follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) extension for scoping review guidelines. The protocol for this scoping review is registered at Open Science Framework (https://doi.org/10.17605/OSF.IO/PUZWB).
2.1 Eligibility Criteria
Experimental and observational study designs were eligible for inclusion. Review papers, abstracts and grey literature were not eligible. Studies not reported in English were excluded. Any study that included an assessment of the energy expenditure of resistance exercise was eligible for inclusion. This included single- and multi-set resistance exercise, circuit-based resistance exercise and exercise where body weight was used as resistance. Studies quantifying the energy expenditure of the usual training program of athletes, where the usual program included some form of resistance exercise, were also included, regardless of whether energy expenditure of the resistance training session itself was reported. No restrictions on participant age, sex, level of activity or health status were imposed.
2.2 Search Strategy
The systematic search to identify studies was conducted by one researcher (L.M.) from the earliest record until 8 January 2024. Databases searched included Medline via Ovid, SPORTDiscus via EBSCOHost, CINAHL via EBSCOHost, and Web of Science. The search used key words and controlled vocabulary in the following combination: (“resistance train*” OR “resistance exercise*” OR “progressive resistance” OR “Weightlift*” OR “weight lift*” OR “Bodybuild*” OR “body build*” OR “weight train*” OR “strength train*” OR “progressive train*” OR “athlet*”) and (“energy expend*” OR “metabol*” OR “calorimet*” OR “energy availab*”). The full electronic search strategy is presented in Supplementary Fig. 1.
2.3 Selection of Studies and Data Extraction
After the search was conducted and duplicates removed, manuscripts were screened by title and abstract by one researcher (L.M.). Full texts of all potentially eligible texts were independently screened by two researchers (L.M. and L.W.). Disagreements were resolved by discussion between screening authors. If a resolution could not be achieved, a third author (G.S.) made the final decision. All screening steps were conducted using Covidence systematic review software (Veritas Health Innovation, Melbourne, Australia).
A standardised Microsoft Excel spreadsheet (Microsoft Corporation, Redmond, WA, USA) was used for data extraction. All publications were extracted by L.M. Duplicate extraction was divided between L.W., G.D., K.P., J.W. and G.S. Extracted data included study characteristics (author, publication year, country and design), participant characteristics (sample size, age, sex and training status), resistance training details (exercises, sets, repetitions, load, rest and movement velocity), and outcome measures (energy expenditure assessment technique, energy expenditure values and post-exercise energy expenditure). A computer program (WebPlotDigitizer, Version 4.6) was used to calculate the mean and standard deviation of data reported in figures [39]. Final data extraction was crosschecked by L.M.
2.4 Assessment of Reporting Quality
Although assessment of methodological quality is not required for scoping reviews, researchers deemed it appropriate for the overview of literature on the topic. The methodological quality of all included publications was assessed using the Rosendal Scale [40]. This scale assesses several factors associated with the minimisation of bias in areas such as participant selection, performance and data analysis. The scale is a combination of items from the Jadad scoring system [41], the Physiotherapy Evidence Database (PEDro) scale [42], and the Delphi List [43], in addition to recommendations contained in the CONSORT statement [44]. Scoring of each publication was determined by dividing the number of ‘yes’ responses by the number of relevant items, with excellent methodological quality indicated by a score of ≥ 60%. Each publication was scored by two researchers (L.M. and L.W.), with discrepancies resolved by discussion.
2.5 Data Synthesis
A narrative approach to data synthesis was used. Characteristics of resistance exercise performed within included studies were categorised (single-exercise, multi-exercise, circuit training and group exercise). The technique used to estimate resistance exercise energy expenditure in each study was described, with studies grouped together on the basis of the assessment technique utilised. Due to variability in how energy expenditure was reported, the energy expenditure value within included studies was synthesised and presented as ranges. Tables and figures are used to summarise findings.
3 Results
3.1 Study Selection and Characteristics
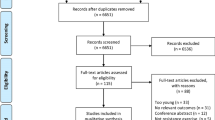
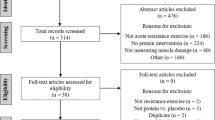
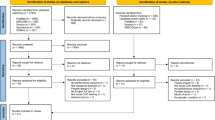
The initial search yielded 24,725 citations. Following the removal of duplicates (n = 4858) and assessment of full text for eligibility (n = 391), a total of 166 articles met inclusion criteria [1, 14, 25, 27, 28, 30, 31, 33, 34, 36,37,38, 45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123,124,125,126,127,128,129,130,131,132,133,134,135,136,137,138,139,140,141,142,143,144,145,146,147,148,149,150,151,152,153,154,155,156,157,158,159,160,161,162,163,164,165,166,167,168,169,170,171,172,173,174,175,176,177,178,179,180,181,182,183,184,185,186,187,188,189,190,191,192,193,194,195,196,197,198]. Figure 1 outlines the flow of study identification. A total of 14 studies were published before 2000, 32 studies were published between 2000 and 2009, 89 studies were published between 2010 and 2019 and 31 studies were published between 2020 and 2023. By design, studies were cross-over studies (n = 84), cross-sectional studies (n = 39), repeated measures studies (n = 19), randomised controlled trials (n = 16), longitudinal observational studies (n = 4), single-group intervention studies (n = 2), a non-randomised controlled trial (n = 1) and a retrospective study (n = 1). Studies were conducted in the USA (n = 83), Europe (n = 34), South America (n = 18), Canada (n = 8), Australia (n = 6), Japan (n = 5), the UK (n = 6), New Zealand (n = 4), India (n = 1), and Singapore (n = 1).
The sample size of the studies ranged from 2 to 417. The mean age of participants ranged from 12.9 to 73.1 years. Six studies did not report mean participant age; however, two of these reported the age range of participants. Studies recruited trained participants (n = 99), recreationally active participants (n = 21), untrained participants (n = 23), clinical participants (n = 9) and a combination of trained and untrained participants (n = 4). Participant training status was not described in 10 studies.
3.2 Resistance Training Characteristics
Details of the resistance training conducted in the included studies are presented in Supplementary Table 1. Of the 166 included studies, 42 used a single-exercise resistance training session, 60 used a multi-exercise resistance training session, 31 used a circuit training session, 5 measured group exercise classes, 2 studies used both single- and multi-exercise resistance training sessions and 26 studies had participants perform their usual resistance training program but did not describe the details of these programs.
3.3 Energy Expenditure Assessment
The methods used to assess energy expenditure of resistance training are presented in Supplementary Table 1 and Fig. 2. Indirect calorimetry (n = 136) was the predominant method used to assess energy expenditure in included studies, along with blood lactate (n = 25) and wearable monitors (n = 13). Other methods reported were metabolic equivalents (MET) via the Compendium of Physical Activities (n = 4), a standard energy cost of resistance exercise per minute (n = 3), and an individual rating of perceived exertion–energy expenditure regression equation (n = 1).
Methods of energy expenditure assessment reported in included studies. RER, respiratory exchange ratio; La−, lactate; MET, metabolic equivalents; EE, energy expenditure; RPE, rating of perceived exertion. aStudies used a separate energy equivalent value for inter-set and inter-exercise rest periods to that used during exercise periods. bStudies included a measure of energy expenditure in the period following resistance training. cO2 deficit purported to capture both the glycolytic and phosphagen systems
3.3.1 Indirect Calorimetry
In total, 136 studies utilised indirect calorimetry to measure the energy expenditure of resistance exercise. These studies collected expired gas for either a portion or the entire duration of the resistance training. Whole room indirect calorimetry was used in 3 of 136 studies [94, 124, 125], with the remaining studies using either a metabolic cart (n = 131) or Douglas bags (n = 2). Most (n = 99) of the 136 studies defined how energy expenditure was calculated from indirect calorimetry. This calculation was based on a set energy equivalent per litre of oxygen (for example, 21.1 kJ/L O2; n = 58), an equation based on volume of oxygen (VO2) and volume of carbon dioxide (VCO2; for example, the Weir equation [199]; n = 21), an energy equivalent based on the respiratory exchange ratio (n = 17) or stoichiometric values (n = 3). The remaining 37 studies did not describe how energy expenditure was calculated from indirect calorimetry. A separate energy equivalent per litre of oxygen during inter-set and inter-exercise rest periods to that during the exercise period was used in seven studies.
3.3.2 Glycolytic Energy Expenditure
The glycolytic contribution to energy expenditure was estimated in 26 studies [27, 28, 30, 31, 33, 34, 37, 38, 47, 52, 99, 105, 107, 108, 117, 119, 121, 122, 141, 150, 154, 160, 168, 173, 174, 197]. Each of these studies included glycolytic measures in addition to indirect calorimetry measures. Blood lactate was measured in 25 of the 26 studies, with the change in blood lactate concentration (peak-rest [La−]) converted to an oxygen equivalent (3 mL O2/kg body mass/mmol [La−]), with energy expenditure calculated from this oxygen volume. One study used the accumulated oxygen deficit to quantify combined anaerobic energy expenditure [38].
3.3.3 Wearable Monitors
Wearable monitors were used in 31 studies to estimate energy expenditure of resistance exercise. This included 18 studies that measured total activity energy expenditure of athletes performing their usual training program that included resistance training. Monitors used were the Sensewear armband (n = 10) [1, 46, 51, 53, 71, 79, 80, 109, 157, 185], chest-mounted heart rate monitor (n = 5) [98, 117, 155, 156, 177], accelerometer (n = 5; wrist-mounted, n = 3; hip-mounted, n = 1; or waist-mounted, n = 1) [140, 147, 162, 163, 192], combination heart rate and accelerometer (n = 7; chest-mounted, n = 5; wrist- and chest-mounted, n = 1; or wrist-mounted, n = 1) [115, 129, 165, 167, 186, 190] and multiple wearable sensors (n = 4; wrist- and chest-mounted, n = 2; wrist-mounted, n = 1; and wrist-, hip- and waist-mounted, n = 1) [25, 57, 96, 131, 196]. Five of these studies were attempting to validate wearable monitors for measurement of energy expenditure against indirect calorimetry [51, 57, 96, 131, 157].
3.3.4 Post-exercise Energy Expenditure
Energy expenditure was measured in the period immediately post-exercise in 76 studies. Indirect calorimetry was used in each of these studies to assess post-exercise energy expenditure. Measurements continued for a pre-specified time frame (n = 57), ranging from 3 to 180 min, or until VO2 returned to a pre-determined value (n = 15) based on pre-exercise resting energy expenditure measurements or a defined O2 consumption (range: 4–5 ml O2/kg/min). In addition, resting metabolic rate was compared with pre-exercise metabolic rate at one or more of 12, 24, 36, 48, and 72 h after resistance training in four studies [45, 91, 101, 118].
3.4 Resistance Training Energy Expenditure
Energy expenditure was reported as both an absolute expenditure (total kJ) and as a rate of expenditure (kJ/min). Energy expenditure values reported varied widely between studies. Absolute values ranged from 6–1575 kJ for single-exercise studies, 38–2957 kJ for multi-exercise studies, 235–1822 kJ for circuit exercise studies, and 1050–1402 kJ for group exercise studies. Relative expenditure values ranged from 8–151 kJ/min for single-exercise studies, 6–62 kJ/min for multi-exercise studies, 11–55 kJ/min for circuit exercise studies, and 4–6 kJ/min for group exercise studies. Reporting standard also varied, with studies reporting expenditure values as exercise alone, exercise plus inter-set rest, and exercise plus inter-set rest plus post-exercise recovery expenditure. Only a small number of studies (n = 34) accounted for resting metabolic rate within the reported energy expenditure values.
3.5 Assessment of Reporting Quality
Results of the quality assessment are presented in Supplementary Table 2. Average Rosendal score was 66.7 ± 15.1%, with 118 of 166 studies achieving a score rated as excellent (≥ 60%).
4 Discussion
This study aimed to review the methods used to assess resistance exercise energy expenditure. A total of 166 studies were included in the review, with the majority utilising indirect calorimetry to estimate energy expenditure. A smaller proportion of studies complemented indirect calorimetry by using methods to estimate the glycolytic contribution to energy expenditure. Wearable sensors were also utilised in included studies, many of which examined athletes performing their usual resistance training program as a component of a broader assessment of energy expenditure and quantifying energy availability. A range of resistance exercise sessions were examined in studies, including single and multi-exercise sessions, low and high intensity sessions, circuit training, and group exercise classes. Given the variability of metabolic characteristics of this range of exercises, the choice of method to quantify energy expenditure requires consideration of these characteristics. Although the majority of studies employed indirect calorimetry, there are limitations to this method pertinent to its application in resistance exercise.
4.1 Indirect Calorimetry
Of the 166 studies included in this scoping review, 136 used indirect calorimetry to estimate energy expenditure. Although a valid method to measure the aerobic metabolic output during steady state exercise, indirect calorimetry is unable to quantify the glycolytic contribution to energy expenditure [168]. Resistance exercise is typically characterised by short duration, high intensity efforts. Loads of 80% of one repetition maximum or more are recommended for increasing muscular strength [200]. Exercises programmed to increase muscular power may vary in relative load, but movement velocity is emphasised [201]. Finally, while muscle hypertrophy can be achieved at a range of lifting intensities, proximity to failure is likely required [202]. This emphasis on high intensity, high velocity, fatigue-inducing exercise requires a significant anaerobic contribution to metabolic output. Therefore, to accurately quantify the energy expenditure of such exercise, employment of a system that can capture the anaerobic component accurately is necessary. Although indirect calorimetry is capable of accounting for the energy expended by the phosphagen system through the fast phase of oxygen uptake immediately after exercise [32], it is limited in measuring the anaerobic glycolytic component of expenditure. As such, indirect calorimetry alone is likely to underestimate the total energy expenditure of resistance exercise [203].
4.2 Glycolytic Energy Expenditure
Given the limitations of indirect calorimetry for quantifying total expenditure, it is likely a requirement of any resistance exercise measure to include a method of gauging the glycolytic contribution to energy expenditure. Twenty-six of the reviewed studies used a measure of glycolytic energy expenditure in addition to indirect calorimetry. Specifically, blood lactate accumulation during the resistance exercise was measured to quantify glycolytic energy expenditure. The importance of including a measure of the glycolytic expenditure is reinforced when examining the contributions of aerobic and glycolytic systems during resistance exercise. For example, single sets of bench press performed to failure at 70% 1 repetition maximum showed a glycolytic expenditure of 26.5 ± 4.4 kJ and an aerobic expenditure of 4.9 ± 2.0 kJ. Similar differences in contribution were reported in loads ranging from 37 to 90% 1 repetition maximum [28]. Similarly, across two sets of bench press performed to failure at 70%, 80% or 90% 1 repetition maximum, the glycolytic pathway contributed a greater proportion of total energy expenditure compared to the aerobic pathway (32.9 ± 8.6 vs 14.2 ± 6.0 kJ, 33.1 ± 9.7 vs 8.9 ± 2.8 kJ, 21.5 ± 5.7 vs 6.2 ± 2.2 kJ, respectively) [27]. Sets of submaximal resistance exercise terminated prior to failure also showed significant contributions from glycolytic energy expenditure, albeit less than the aerobic contribution [47, 105]. In addition to these measures of glycolytic energy expenditure, previous studies have shown significant reductions in muscle glycogen content following resistance training, particularly in type II glycolytic muscle fibres, indicating a heavy reliance on glycolysis [204,205,206,207]. Clearly there is merit in including a measure of glycolytic expenditure when quantifying the energy cost of resistance exercise. Program design factors such as intensity and proximity to failure will likely influence the magnitude of the anaerobic system contribution to overall energy expenditure.
The accumulation of blood lactate, indicative of a positive balance between lactate production and clearance, represents an overall energy turnover greater than the rate of oxygen consumption. An energy equivalent value has been determined for each unit increase in blood lactate, established as 3 mL O2/kg body mass/mmol lactate, allowing the calculation of the glycolytic contribution to total expenditure [32]. Blood lactate accumulation can be measured using the difference in lactate pre- to post-exercise. A challenge though in the resistance exercise context is the intermittent effort, whereby relatively long duration rest intervals are typically interspersed amongst short duration sets. Because of this, measuring the change in blood lactate between each set may provide further insight into anaerobic expenditure than the pre- and post-exercise difference alone. This serves to highlight the nuanced approach required to quantify resistance exercise energy expenditure, where consideration of training specific characteristics is necessary. A degree of pragmatism is also necessary; although further insight may be gained from inter-set measures, the intrusive nature of blood lactate measurement needs to be recognised, particularly outside the laboratory setting. For this reason, a lactate monitoring system akin to continuous glucose monitoring may provide additional insight. The use of blood lactate measures is not itself without limitations though. One such limitation is that blood lactate concentration at best provides only an approximate description of muscle lactate levels and glycolytic ATP resynthesis [203]. Further research elucidating a more valid measure of glycolytic energy expenditure is therefore required. The influence of muscle fibre composition of athletes on glycolytic energy expenditure during resistance exercise also warrants investigation based on the differing metabolic capacities of muscle fibre types [208].
4.3 Wearable Monitors
Wearable monitors were utilised in 31 included studies, with the Sensewear armband the most frequently used (n = 10). Of these 28 studies, 18 estimated total energy expenditure of participants conducting their usual training routine that included resistance exercise. While accessibility and ease of application make wearable technologies an attractive tool for monitoring energy expenditure, such tools have shown limited capacity to provide an accurate quantification of resistance exercise expenditure [57]. Five included studies attempted to validate wearable devices against indirect calorimetry [51, 57, 96, 131, 157]. Resistance exercise protocols included body weight exercises, circuit resistance exercise, and traditional resistance exercise. The devices used included wrist-, chest-, waist-, hip-, and arm-worn, such as the Sensewear armband. Overall findings varied, but four of the five studies found either poor correlation or significant differences in absolute energy expenditure values between monitors and indirect calorimetry [51, 57, 96, 131]. Monitors were found to both under- and overestimate energy expenditure values against indirect calorimetry, with mean absolute percentage errors ranging markedly (15.1–57.0%) [51, 57, 96, 131], and similar marked variance in correlations (r = 0.02–0.74) [57, 96, 131]. One study found the Sensewear armband Mini and BodyMedia FIT had very large correlations with indirect calorimetry (r = 0.77–0.78) and a trivial to small percent mean change from indirect calorimetry during traditional resistance training [157]. It is notable though that none of these validation studies included a measure of glycolytic expenditure with indirect calorimetry, meaning the criterion measures used in these studies may themselves be limited. In addition, the location of devices on the body may influence validity, with suggestions that arm-worn devices may have limited capacity to capture lower extremity exercise and vice versa [157]. Given the limited validity currently available for wearable devices in a resistance training context, the use of such devices should proceed with caution when quantifying energy expenditure, particularly with commercially available devices which show significant variability [131].
4.4 Post-exercise Energy Expenditure
Resistance exercise consistently demonstrates an elevation in energy expenditure beyond the acute exercise period. This is evidenced by an increased heart rate and VO2 relative to pre-exercise for at least 30 min after the cessation of lifting [55, 149, 151, 161]. Four of the reviewed studies included a measure of metabolic rate at one or more of 12, 24, 36, 48, and 72 h after resistance exercise. Results in these studies varied, with metabolic rate remaining elevated for up to 12–72 h [101, 118], although these longer-term elevations are likely trivial, and in part attributable to exercise-induced muscle damage [209] along with measurement noise [210]. Contrary to this is the acute elevation in VO2 and energy expenditure immediately following a resistance exercise effort relative to pre-exercise. The VO2 measured in the first minute following an exercise set has been observed to increase beyond values measured during the set [151]. This increase in VO2 in the minutes following a resistance effort is considered the fast phase of oxygen kinetics and accounts for the energy expenditure of the phosphagen system. The absolute contribution of this measure may be equivalent to, if not greater than, the contribution from either aerobic metabolism or glycolytic metabolism during the exercise set [27, 31]. Acknowledging the dependence on anaerobic energy systems during resistance exercise and the observable metabolic output immediately following a resistance exercise effort related to the phosphagen system, it appears pertinent to include measures of post-exercise oxygen consumption in any calorimetric estimation of resistance exercise energy expenditure. These measures should include rest periods between sets and the recovery period following the final set. It is suggested that recovery measures continue until VO2 returns to 5 mL/kg/min (a typical standing oxygen uptake) [28].
4.5 Metabolic Equivalents
An underutilised approach to estimating energy expenditure in the reviewed studies was the use of MET values. Four studies quantified the energy expenditure of resistance exercise using MET [14, 68, 132, 194]. Each study assessed total energy expenditure of participants during their regular training and competition routines, which included resistance exercise. Resistance exercise was assigned a MET value according to the Compendium of Physical Activities [35], from which energy expenditure was calculated. A strength of the MET system is its simplicity of application in estimating energy expenditure. No equipment is necessary, with users assigning an appropriate value based on training characteristics before undertaking basic calculations to convert MET into an energy expenditure. For this reason, its use is appealing for practitioners in the field. A challenge, though, in the resistance training context is selecting an appropriate MET value to assign. The most recent iteration of the Compendium provides MET values of 3.5, 5.0 and 6.0 for resistance exercises on the basis of the type and intensity of training, derived from published literature [35]. Previous research has measured MET values during resistance exercise and compared these with the Compendium of Physical Activities. Depending on population and training characteristics, measured values range between 3.0 and 8.0 MET, with the higher values observed in circuit style training characterised by high repetitions with minimal rest periods [144, 145, 183, 211]. Similar variability was identified in the energy expenditure measured in studies included in the current review, suggesting a range of equivalent MET values. The almost twofold difference between highest and lowest MET values from the Compendium of Physical Activities, and the large variability in energy expenditure values of reviewed studies, highlights the importance of clearly defining resistance exercise and considering the amount of muscle mass activated during exercise when using the MET system. In addition to the challenge of selecting the most relevant MET value, this system may also underestimate energy expenditure of resistance exercise on the basis of how the values have been derived. The MET values are obtained from measurements of the oxygen cost of the activity, thus neglecting the meaningful contribution to expenditure from glycolysis. Furthermore, Compendium instructions recommend applying the MET value to the active exercise period and excluding periods of rest between sets [35]. This process would likely then miss the substantial energy expenditure associated with the phosphagen system. At minimum though, the MET system may be applied in the field to provide an estimate of approximate energy expenditure. Consideration should also be given to the health status of the individual. A modified MET value may be more suitable for athletes presenting with anomalies relating to muscle activation, including some paralympic athletes, given that the resistance exercise MET value for wheelchair users is 2.2 [212].
4.6 Limitations
This scoping review has limitations which should be considered. Many studies did not define how energy expenditure was calculated from expired gas analysis, and few studies reported the reproducibility of energy expenditure measures. The variability in units used to report energy expenditure (absolute expenditure and rate of expenditure) limited the capacity to report the values identified in reviewed studies. The energy expenditure of resistance exercise may vary on the basis of training age and training goals. Due to the inconsistencies in energy expenditure reporting, the influence of these variables was unable to be examined.
5 Conclusion
The capacity to quantify the energy expenditure of resistance exercise would allow researchers and practitioners to better address the energy and nutrient needs of athletes. Most included studies in this scoping review used indirect calorimetry to estimate energy expenditure during resistance exercise. This technique captures the aerobic energy expenditure, with oxygen uptake measured in the minutes immediately following exercise also estimating the energy expenditure of the phosphagen system. A small number of studies included blood lactate analysis before and after exercise to account for the glycolytic contribution to expenditure. Wearable monitors and the MET system were also used to estimate energy expenditure in a small number of studies.
Based on these findings, it is suggested that laboratory measures of resistance exercise energy expenditure utilise blood lactate analysis to capture the glycolytic system in addition to indirect calorimetry measured during and in the minutes immediately following exercise to account for the aerobic and phosphagen systems. Measures of energy expenditure in the field will likely rely largely on estimations. The MET system may be viable despite having limitations, whereas wearable monitors should be used with caution based on current validity measures. The use of multiple devices, capturing both upper and lower body as well as variable sensor inputs, may provide more valid estimates of resistance exercise energy expenditure. Additional evidence is required to validate such a method.
There are several questions future research could investigate. Identifying other means to quantify the glycolytic contribution to expenditure beyond change in blood lactate would be valuable. Investigating the influence of muscle fibre composition on glycolytic energy expenditure would also be of value based on differences in substrate utilisation between fibre types. Developing a compendium of resistance exercises and their approximate energy expenditure values may assist practitioners. Currently, there is a paucity of literature examining energy expenditure in paralympic athletes. Future research in this population is warranted to confirm transferability of the measurement techniques identified in this review. Finally, understanding the methods currently used by practitioners in the field to estimate energy expenditure of resistance exercise would support the findings of the present scoping review.
References
Bradley WJ, Cavanagh B, Douglas W, Donovan TF, Twist C, Morton JP, et al. Energy intake and expenditure assessed “in-season” in an elite European rugby union squad. Eur J Sport Sci EJSS. 2015;15(6):469–79.
Bradley WJ, Cavanagh BP, Douglas W, Donovan TF, Morton JP, Close GL. Quantification of training load, energy intake, and physiological adaptations during a rugby preseason: a case study from an elite European Rugby Union Squad. J Strength Cond Res. 2015;29(2):534–44.
García-Pinillos F, Lago-Fuentes C, Jaén-Carrillo D, Bujalance-Moreno P, Latorre-Román P, Roche-Seruendo LE, et al. Strength training habits in amateur endurance runners in Spain: influence of athletic level. Int J Environ Res Public Health. 2020;17(21).
Lloyd RS, Oliver JL. The youth physical development model: a new approach to long-term athletic development. Strength Cond J. 2012;34(3):61–72.
Del Vecchio L, Reaburn P. Mixed methods strength training for the masters athlete a review. J Austral Strength Cond. 2013;21(4).
Reid M, Schneiker K. Strength and conditioning in tennis: current research and practice. J Sci Med Sport. 2008;11(3):248–56.
Mitchell L, Slater G, Hackett D, Johnson N, O’Connor H. Physiological implications of preparing for a natural male bodybuilding competition. Eur J Sport Sci. 2018;18(5):619–29.
Swinton PA, Lloyd R, Agouris I, Stewart A. Contemporary training practices in elite British powerlifters: survey results from an international competition. J Strength Cond Res. 2009;23(2):380–4.
Hackett DA, Johnson NA, Chow CM. Training practices and ergogenic aids used by male bodybuilders. J Strength Cond Res. 2013;27(6):1609–17.
Claudino JG, Gabbett TJ, Bourgeois F, Souza HS, Miranda RC, Mezêncio B, et al. CrossFit overview: systematic review and meta-analysis. Sports Med Open. 2018;4(1):11.
Maestroni L, Read P, Bishop C, Turner A. Strength and power training in rehabilitation: underpinning principles and practical strategies to return athletes to high performance. Sports Med. 2020;50(2):239–52.
Thomas DT, Erdman KA, Burke LM. American College of Sports Medicine Joint Position Statement. Nutrition and athletic performance. Med Sci Sports Exerc. 2016;48(3):543–68.
Tipton KD. Nutritional support for exercise-induced injuries. Sports Med. 2015;45(1):93–104.
Taylor HL, Garabello G, Pugh J, Morton J, Langan-Evans C, Louis J, et al. Patterns of energy availability of free-living athletes display day-to-day variability that is not reflected in laboratory-based protocols: insights from elite male road cyclists. J Sports Sci. 2022;40(16):1849–56.
Westerterp KR. Doubly labelled water assessment of energy expenditure: principle, practice, and promise. Eur J Appl Physiol. 2017;117(7):1277–85.
Kenny GP, Notley SR, Gagnon D. Direct calorimetry: a brief historical review of its use in the study of human metabolism and thermoregulation. Eur J Appl Physiol. 2017;117(9):1765–85.
Morehen JC, Bradley WJ, Clarke J, Twist C, Hambly C, Speakman JR, et al. The assessment of total energy expenditure during a 14-day in-season period of professional rugby league players using the doubly labelled water method. Int J Sport Nutr Exerc Metab. 2016;26(5):464–72.
Anderson L, Orme P, Naughton RJ, Close GL, Milsom J, Rydings D, et al. Energy intake and expenditure of professional soccer players of the English Premier League: evidence of carbohydrate periodization. Int J Sport Nutr Exerc Metab. 2017;27(3):228–38.
Sagayama H, Hamaguchi G, Toguchi M, Ichikawa M, Yamada Y, Ebine N, et al. Energy requirement assessment in Japanese table tennis players using the doubly labeled water method. Int J Sport Nutr Exerc Metab. 2017;27(5):421–8.
Jesus F, Sousa M, Nunes CL, Francisco R, Rocha P, Minderico CS, et al. Energy availability over one athletic season: an observational study among athletes from different sports. Int J Sport Nutr Exerc Metab. 2022;32(6):479–90.
Logue D, Madigan SM, Delahunt E, Heinen M, Mc Donnell SJ, Corish CA. Low energy availability in athletes: a review of prevalence, dietary patterns, physiological health, and sports performance. Sports Med. 2018;48(1):73–96.
Oxfeldt M, Phillips SM, Andersen OE, Johansen FT, Bangshaab M, Risikesan J, et al. Low energy availability reduces myofibrillar and sarcoplasmic muscle protein synthesis in trained females. J Physiol. 2023;601(16):3481–97.
Fahrenholtz IL, Sjödin A, Benardot D, Tornberg ÅB, Skouby S, Faber J, et al. Within-day energy deficiency and reproductive function in female endurance athletes. Scand J Med Sci Sports. 2018;28(3):1139–46.
Torstveit MK, Fahrenholtz I, Stenqvist TB, ystein Sylta Ø, Melin A. Within-day energy deficiency and metabolic perturbation in male endurance athletes. Int J Sport Nutr Exerc Metab. 2018;28(4):419.
Lundstrom EA, De Souza MJ, Canil HN, Williams NI. Sex differences and indications of metabolic compensation in within-day energy balance in elite Division 1 swimmers. Appl Physiol Nutr Metab. 2023;48(1):74–87.
Ackerman KE, Rogers MA, Heikura HA, Burke LM, Stellingwerff T, Hackney AC, et al. Methodology for studying relative energy deficiency in sport (REDs): a narrative review by a subgroup of the International Olympic Committee (IOC) consensus on REDs. Br J Sports Med. 2023;57(17):1136.
Scott CB, Leary MP, Tenbraak AJ. Energy expenditure characteristics of weight lifting: 2 sets to fatigue. Appl Physiol Nutr Metab. 2011;36(1):115–20.
Scott CB, Leighton BH, Ahearn KJ, McManus JJ. Aerobic, anaerobic, and excess postexercise oxygen consumption energy expenditure of muscular endurance and strength: 1-set of bench press to muscular fatigue. J Strength Cond Res. 2011;25(4):903–8.
Scott CB, Reis VM. Steady state models provide an invalid estimate of intermittent resistance-exercise energy costs. Eur J Hum Mov. 2014;33:70–8.
Scott CB, Croteau A, Ravlo T. Energy expenditure before, during, and after the bench press. J Strength Cond Res. 2009;23(2):611–8.
Scott CB. The effect of time-under-tension and weight lifting cadence on aerobic, anaerobic, and recovery energy expenditures: 3 submaximal sets. Appl Physiol Nutr Metab. 2012;37(2):252–6.
di Prampero PE, Ferretti G. The energetics of anaerobic muscle metabolism: a reappraisal of older and recent concepts. Respir Physiol. 1999;118(2):103–15.
Freitas MC, Cholewa JM, Gerosa-Neto J, Goncalves DC, Caperuto EC, Lira FS, et al. A single dose of oral ATP supplementation improves performance and physiological response during lower body resistance exercise in recreational resistance-trained males. J Strength Cond Res. 2019;33(12):3345–52.
Brunelli DT, Finardi EAR, Bonfante ILP, Gaspari AF, Sardeli AV, Souza TMF, et al. Acute low- compared to high-load resistance training to failure results in greater energy expenditure during exercise in healthy young men. PLoS ONE [Electronic Resource]. 2019;14(11): e0224801.
Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr, Tudor-Locke C, et al. 2011 Compendium of Physical Activities: a second update of codes and MET values. Med Sci Sports Exerc. 2011;43(8):1575–81.
Lytle JR, Kravits DM, Martin SE, Green JS, Crouse SF, Lambert BS. Predicting energy expenditure of an acute resistance exercise bout in men and women. Med Sci Sports Exerc. 2019;51(7):1532–7.
Mazzetti S, Douglass M, Yocum A, Harber M. Effect of explosive versus slow contractions and exercise intensity on energy expenditure. Med Sci Sports Exerc. 2007;39(8):1291–301.
Reis VM, Garrido ND, Vianna J, Sousa AC, Alves JV, Marques MC. Energy cost of isolated resistance exercises across low- to high-intensities. PLoS ONE [Electronic Resource]. 2017;12(7): e0181311.
Rohatgi A. WebPlotDigitizer. 4.6 ed. Pacifica, California, USA; 2022.
van Rosendal SP, Osborne MA, Fassett RG, Coombes JS. Guidelines for glycerol use in hyperhydration and rehydration associated with exercise. Sports Med. 2010;40(2):113–29.
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJM, Gavaghan DJ, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17(1):1–12.
Maher CG, Moseley AM, Sherrington C, Elkins MR, Herbert RD. A description of the trials, reviews, and practice guidelines indexed in the PEDro database. Phys Ther. 2008;88(9):1068–77.
Verhagen AP, de Vet HCW, de Bie RA, Kessels AGH, Boers M, Bouter LM, et al. The Delphi list: a criteria list for quality assessment of randomized clinical trials for conducting systematic reviews developed by Delphi consensus. J Clin Epidemiol. 1998;51(12):1235–41.
Schulz KF, Altman DG, Moher D. CONSORT 2010 Statement: updated guidelines for reporting parallel group randomized trials. Ann Intern Med. 2010;152(11):726–32.
Abboud GJ, Greer BK, Campbell SC, Panton LB. Effects of load-volume on EPOC after acute bouts of resistance training in resistance-trained men. J Strength Cond Res. 2013;27(7):1936–41.
Aerenhouts D, Zinzen E, Clarys P. Energy expenditure and habitual physical activities in adolescent sprint athletes. J Sports Sci Med. 2011;10(2):362–8.
Aniceto RR, Ritti-Dias RM, Scott CB, Martins de Lima FF, Pessôa dos Prazeres TM, do Prado WL. Acute effects of different weight training methods on energy expenditure in trained men. Revista Brasileira de Medicina do Esporte. 2013;19(3):181–5.
Anthierens A, Olivier N, Thevenon A, Mucci P. Trunk muscle aerobic metabolism responses in endurance athletes, combat athletes and untrained men. Int J Sports Med. 2019;40(7):434–9.
Barreto AC, Maior AS, Menezes P, Willardson JM, Silva J, Reis VR, et al. Effect of different resistance exercise repetition velocities on excess post-exercise oxygen consumption and energetic expenditure. Int Sportmed J. 2010;11(1):235–43.
Beckham SG, Earnest CP. Metabolic cost of free weight circuit weight training. J Sports Med Phys Fit. 2000;40(2):118–25.
Benito P, Neiva C, González-Quijano P, Cupeiro R, Morencos E, Peinado A. Validation of the SenseWear armband in circuit resistance training with different loads. Eur J Appl Physiol. 2012;112(8):3155–9.
Benito PJ, Alvarez-Sanchez M, Diaz V, Morencos E, Peinado AB, Cupeiro R, et al. Cardiovascular fitness and energy expenditure response during a combined aerobic and circuit weight training protocol. PLoS ONE [Electronic Resource]. 2016;11(11): e0164349.
Berthiaume MP, Lalande-Gauthier M, Chrone S, Karelis AD. Energy expenditure during the group exercise course Bodypump in young healthy individuals. J Sports Med Phys Fit. 2015;55(6):563–8.
Bertucci WM, Arfaoui A, Duc S, Letellier T, Brikci A. Effect of whole body vibration in energy expenditure and perceived exertion during intense squat exercise. Acta Bioeng Biomech. 2015;17(1):87–93.
Binzen CA, Swan PD, Manore MM. Postexercise oxygen consumption and substrate use after resistance exercise in women. Med Sci Sports Exerc. 2001;33(6):932–8.
Bloomer RJ. Energy cost of moderate-duration resistance and aerobic exercise. J Strength Cond Res. 2005;19(4):878–82.
Boudreaux BD, Hebert EP, Hollander DB, Williams BM, Cormier CL, Naquin MR, et al. Validity of wearable activity monitors during cycling and resistance exercise. Med Sci Sports Exerc. 2018;50(3):624–33.
Brentano MA, Umpierre D, Porto Santos L, Lopes AL, Martins Kruel LF. Supersets do not change energy expenditure during strength training sessions in physically active individuals. J Exerc Sci Fit. 2016;14(2):41–6.
Brewer CB, Booher BM, Lawton N. Comparison of acute energy expenditure and rating of perceived exertion in equivalent bouts of circuit training and treadmill running. J Strength Cond Res. 2021;35(3):680–7.
Brisebois MF, Biggerstaff KD, Nichols DL. Cardiorespiratory responses to acute bouts of high-intensity functional training and traditional exercise in physically active adults. J Sports Med Phys Fit. 2022;62(2):199–206.
Cadieux S, McNeil J, Lapierre MP, Riou ME, Doucet E. Resistance and aerobic exercises do not affect post-exercise energy compensation in normal weight men and women. Physiol Behav. 2014;130:113–9.
Caruso JF, Borgsmiller JA, Riner RD, Mason ML, Lutz BR, Nelson CC. Net energy expenditure of gravity-independent high-speed resistive exercise done by women. Aviat Space Environ Med. 2012;83(2):111–7.
Caruso JF, Hamill JL, Yamauchi M, Hernanadez DA, Cho M, Nelson NM, et al. Net caloric cost and electromyographic responses to seated leg presses performed against inertial resistance. Isokinet Exerc Sci. 2006;14(1):15–23.
Caruso JF, Hernandez DA. Net caloric cost of a 3-set flywheel ergometer resistance exercise paradigm. J Strength Cond Res. 2002;16(4):567–72.
Caruso JF, Hernandez DA, Saito K, Cho M, Nelson NM. Inclusion of eccentric actions on net caloric cost resulting from isoinertial resistance exercise. J Strength Cond Res. 2003;17(3):549–55.
Caruso JF, Herron JC, Hernandez DA, Porter A, Schweickert T, Manning TF. Metabolic responses to the seated calf press exercise performed against inertial resistance. Aviat Space Environ Med. 2005;76(11):1019–23.
Chatzinikolaou A, Fatouros I, Petridou A, Jamurtas A, Avloniti A, Douroudos I, et al. Adipose tissue lipolysis is upregulated in lean and obese men during acute resistance exercise. Diabetes Care. 2008;31(7):1397–9.
Cherian KS, Sainoji A, Nagalla B, Yagnambhatt VR. Energy balance coexists with disproportionate macronutrient consumption across pretraining, during training, and posttraining among Indian junior soccer players. Pediatr Exerc Sci. 2018;30(4):506–15.
Correa CS, Teixeira BC, Cobos RC, Macedo RC, Kruger RL, Carteri RB, et al. High-volume resistance training reduces postprandial lipaemia in postmenopausal women. J Sports Sci. 2015;33(18):1890–901.
Correa CS, Teixeira BC, Macedo RC, Bittencourt A, Kruger RL, Gross JS, et al. Resistance exercise at variable volume does not reduce postprandial lipemia in postmenopausal women. Age. 2014;36(2):869–79.
Costello N, Deighton K, Cummins C, Whitehead S, Preston T, Jones B. Isolated & combined wearable technology underestimate the total energy expenditure of professional young rugby league players; a doubly labelled water validation study. J Strength Cond Res. 2019;27:27.
Crommett AD, Kinzey SJ. Excess postexercise oxygen consumption following acute aerobic and resistance exercise in women who are lean or obese. J Strength Cond Res. 2004;18(3):410–5.
Cunha FA, Gomes GSM, Carvalho J, da Silva NSL. Concurrent exercise circuit protocol performed in public fitness facilities meets the American College of Sports Medicine guidelines for energy cost and metabolic intensity among older adults in Rio de Janeiro City. Appl Physiol Nutr Metab. 2019;44(5):477–84.
Da Silva ME, Fernandez JM, Castillo E, Nunez VM, Vaamonde DM, Poblador MS, et al. Influence of vibration training on energy expenditure in active men. J Strength Cond Res. 2007;21(2):470–5.
Danoff PL, Danoff JV. Energy cost and heart rate response to static and dynamic leg exercise. Arch Phys Med Rehabil. 1982;63(3):130–4.
De Looze MP, Toussaint HM, Commissaris DA, Jans MP, Sargeant AJ. Relationships between energy expenditure and positive and negative mechanical work in repetitive lifting and lowering. J Appl Physiol. 1994;77(1):420–6.
DeGroot DW, Quinn TJ, Kertzer R, Vroman NB, Olney WB. Circuit weight training in cardiac patients: determining optimal workloads for safety and energy expenditure. J Cardiopulm Rehabil. 1998;18(2):145–52.
Dos Santos TR, Billinger SA, Midgley AW, Michalski AC, Costa VAB, Fonseca GF, et al. Appetite and energy intake following a bout of circuit resistance training in chronic hemiparetic stroke patients: a preliminary randomized controlled trial. Top Stroke Rehabil. 2022:1–14.
Drenowatz C, Grieve GL, DeMello MM. Change in energy expenditure and physical activity in response to aerobic and resistance exercise programs. Springerplus. 2015;4:798.
Drenowatz C, Hand GA, Shook RP, Jakicic JM, Hebert JR, Burgess S, et al. The association between different types of exercise and energy expenditure in young nonoverweight and overweight adults. Appl Physiol Nutr Metab. 2015;40(3):211–7.
Dudley GA, Tesch PA, Harris RT, Golden CL, Buchanan P. Influence of eccentric actions on the metabolic cost of resistance exercise. Aviat Space Environ Med. 1991;62(7):678–82.
Egger T, Flueck JL. Energy availability in male and female elite wheelchair athletes over seven consecutive training days. Nutrients. 2020;12(11):25.
Falcone PH, Chih-Yin TAI, Carson LR, Joy JM, Mosman MM, McCann TR, et al. Caloric expenditure of aerobic, resistance, or combined high-intensity interval training using a hydraulic resistance system in healthy men. J Strength Cond Res. 2015;29(3):779–85.
Farinatti PT, Castinheiras Neto AG. The effect of between-set rest intervals on the oxygen uptake during and after resistance exercise sessions performed with large- and small-muscle mass. J Strength Cond Res. 2011;25(11):3181–90.
Farinatti PT, Simao R, Monteiro WD, Fleck SJ. Influence of exercise order on oxygen uptake during strength training in young women. J Strength Cond Res. 2009;23(3):1037–44.
Fatouros IG, Tournis S, Leontsini D, Jamurtas AZ, Sxina M, Thomakos P, et al. Leptin and adiponectin responses in overweight inactive elderly following resistance training and detraining are intensity related. J Clin Endocrinol Metab. 2005;90(11):5970–7.
Ferrari R, Alberton C, Pinto S, Cadore E, Pinto R, Kruel LF. Oxygen consumption during concurrent training: influence of intra-session exercise sequence and aerobic exercise modality. Biol Sport. 2018;35(3):247–52.
Garnacho-Castano MV, Albesa-Albiol L, Serra-Paya N, Gomis Bataller M, Feliu-Ruano R, Guirao Cano L, et al. The slow component of oxygen uptake and efficiency in resistance exercises: a comparison with endurance exercises. Front Physiol. 2019;10:357.
Garnacho-Castano MV, Albesa-Albiol L, Serra-Paya N, Gomis Bataller M, Pleguezuelos Cobo E, Guirao Cano L, et al. Oxygen uptake slow component and the efficiency of resistance exercises. J Strength Cond Res. 2021;35(4):1014–22.
Greer BK, O’Brien J, Hornbuckle LM, Panton LB. EPOC comparison between resistance training and high-intensity interval training in aerobically fit women. Int J Exerc Sci. 2021;14(2):1027–35.
Greer BK, Sirithienthad P, Moffatt RJ, Marcello RT, Panton LB. EPOC comparison between isocaloric bouts of steady-state aerobic, intermittent aerobic, and resistance training. Res Q Exerc Sport. 2015;86(2):190–5.
Gremeaux V, Drigny J, Nigam A, Juneau M, Guilbeault V, Latour E, et al. Long-term lifestyle intervention with optimized high-intensity interval training improves body composition, cardiometabolic risk, and exercise parameters in patients with abdominal obesity. Am J Phys Med Rehabil. 2012;91(11):941–50.
Guiraud T, Labrunee M, Pillard F, Granger R, Bousquet M, Richard L, et al. Whole-body strength training using a Huber Motion Lab in coronary heart disease patients: safety, tolerance, fuel selection, and energy expenditure aspects and optimization. Am J Phys Med Rehabil. 2015;94(5):385–94.
Gutierrez J, Gribok A, Rumpler W, Chandran A, DiPietro L. A single bout of resistance exercise does not promote excess postexercise energy expenditure in untrained young men with a family history of diabetes. Int J Sport Nutr Exerc Metab. 2015;25(1):20–6.
Haddock BL, Wilkin LD. Resistance training volume and post exercise energy expenditure. Int J Sports Med. 2006;27(2):143–8.
Hajj-Boutros G, Landry-Duval MA, Comtois AS, Gouspillou G, Karelis AD. Wrist-worn devices for the measurement of heart rate and energy expenditure: s validation study for the Apple Watch 6, Polar Vantage V and Fitbit Sense. Eur J Sport Sci. 2022:1–13.
Haltom RW, Kraemer RR, Sloan RA, Hebert EP, Frank K, Tryniecki JL. Circuit weight training and its effects on excess postexercise oxygen consumption. Med Sci Sports Exerc. 1999;31(11):1613–8.
Harris N, Kilding A, Sethi S, Merien F, Gottschall J. A comparison of the acute physiological responses to BODYPUMP (TM) versus iso-caloric and iso-time steady state cycling. J Sci Med Sport. 2018;21(10):1085–9.
Harris NK, Dulson DK, Logan GRM, Warbrick IB, Merien FLR, Lubans DR. Acute responses to resistance and high-intensity interval training in early adolescents. J Strength Cond Res. 2017;31(5):1177–86.
Harris NK, Woulfe CJ, Wood MR, Dulson DK, Gluchowski AK, Keogh JB. Acute physiological responses to strongman training compared to traditional strength training. J Strength Cond Res. 2016;30(5):1397–408.
Heden T, Lox C, Rose P, Reid S, Kirk EP. One-set resistance training elevates energy expenditure for 72 h similar to three sets. Eur J Appl Physiol. 2011;111(3):477–84.
Hu J, Browne JD, Arnold MT, Robinson A, Heacock MF, Ku R, et al. Physiological and metabolic requirements, and user-perceived exertion of immersive virtual reality exergaming incorporating an adaptive cable resistance system: an exploratory study. Games Health J. 2021;10(5):361–9.
Hulsey CR, Soto DT, Koch AJ, Mayhew JL. Comparison of kettlebell swings and treadmill running at equivalent rating of perceived exertion values. J Strength Cond Res. 2012;26(5):1203–7.
Hunter GR, Bickel CS, Fisher G, Neumeier WH, McCarthy JP. Combined aerobic and strength training and energy expenditure in older women. Med Sci Sports Exerc. 2013;45(7):1386–93.
Hunter GR, Seelhorst D, Snyder S. Comparison of metabolic and heart rate responses to super slow vs. traditional resistance training. J Strength Cond Res. 2003;17(1):76–81.
Jacobs PL, Mahoney ET, Nash MS, Green BA. Circuit resistance training in persons with complete paraplegia. J Rehabil Res Dev. 2002;39(1):21–8.
Jarvinen L, Lundin Petersdotter S, Chaillou T. High-intensity resistance exercise is not as effective as traditional high-intensity interval exercise for increasing the cardiorespiratory response and energy expenditure in recreationally active subjects. Eur J Appl Physiol. 2022;122(2):459–74.
Joao GA, Almeida GPL, Tavares LD, Kalva-Filho CA, Carvas Junior N, Pontes FL, et al. Acute behavior of oxygen consumption, lactate concentrations, and energy expenditure during resistance training: comparisons among three intensities. Front Sports Act Living. 2021;3: 797604.
Jun Liang O, Brownlee IA. Energy expenditure, availability, and dietary intake assessment in competitive female dragon boat athletes. Sports (2075–4663). 2017;5(2):45.
Kalb JS, Hunter GR. Weight training economy as a function of intensity of the squat and overhead press exercise. J Sports Med Phys Fit. 1991;31(2):154–60.
Katch FI, Freedson PS, Jones CA. Evaluation of acute cardiorespiratory responses to hydraulic resistance exercise. Med Sci Sports Exerc. 1985;17(1):168–73.
Keim NL, Canty DJ, Barbieri TF, Wu MM. Effect of exercise and dietary restraint on energy intake of reduced-obese women. Appetite. 1996;26(1):55–70.
Kelleher AR, Hackney KJ, Fairchild TJ, Keslacy S, Ploutz-Snyder LL. The metabolic costs of reciprocal supersets vs. traditional resistance exercise in young recreationally active adults. J Strength Cond Res. 2010;24(4):1043–51.
Kemmler W, Von Stengel S, Schwarz J, Mayhew JL. Effect of whole-body electromyostimulation on energy expenditure during exercise. J Strength Cond Res. 2012;26(1):240–5.
Kinnunen H, Hakkinen K, Schumann M, Karavirta L, Westerterp KR, Kyrolainen H. Training-induced changes in daily energy expenditure: methodological evaluation using wrist-worn accelerometer, heart rate monitor, and doubly labeled water technique. PLoS ONE [Electronic Resource]. 2019;14(7): e0219563.
Koerhuis CL, van der Heide FM, Hof AL. Energy consumption in static muscle contraction. Eur J Appl Physiol. 2003;88(6):588–92.
Lyristakis P, Ball N, McKune AJ. Reliability of methods to measure energy expenditure during and after resistance exercise. Appl Physiol Nutr Metab. 2019;44(12):1276–82.
Magkos F, Tsekouras YE, Prentzas KI, Basioukas KN, Matsama SG, Yanni AE, et al. Acute exercise-induced changes in basal VLDL-triglyceride kinetics leading to hypotriglyceridemia manifest more readily after resistance than endurance exercise. J Appl Physiol. 2008;105(4):1228–36.
Magosso RF, da Silva Junior AJ, Neto AP, Neto JC, Baldissera V. Energy expenditure during multiple sets of leg press and bench press. J Exerc Physiol Online. 2013;16(5):57–62.
Marzolini S, McIlroy W, Oh P, Brooks D. Can individuals participating in cardiac rehabilitation achieve recommended exercise training levels following stroke? J Cardiopulm Rehabil Prev. 2012;32(3):127–34.
Mazzetti S, Wolff C, Yocum A, Reidy P, Douglass M, Cochran M. Effect of maximal and slow versus recreational muscle contractions on energy expenditure in trained and untrained men. J Sports Med Phys Fit. 2011;51(3):381–92.
Mazzetti SA, Wolff C, Collins B, Kolankowski MT, Wilkerson B, Overstreet M, et al. Influence of differences in exercise-intensity and kilograms/set on energy expenditure during and after maximally explosive resistance exercise. Int J Exerc Sci. 2011;4(4):273–82.
McMillan DW, Maher JL, Jacobs KA, Mendez AJ, Nash MS, Bilzon JLJ. Effects of exercise mode on postprandial metabolism in humans with chronic paraplegia. Med Sci Sports Exerc. 2021;53(7):1495–504.
Melanson EL, Sharp TA, Seagle HM, Donahoo WT, Grunwald GK, Peters JC, et al. Resistance and aerobic exercise have similar effects on 24-h nutrient oxidation. Med Sci Sports Exerc. 2002;34(11):1793–800.
Melanson EL, Sharp TA, Seagle HM, Donahoo WT, Grunwald GK, Peters JC, et al. Twenty-four-hour metabolic responses to resistance exercise in women. J Strength Cond Res. 2005;19(1):61–6.
Melby C, Scholl C, Edwards G, Bullough R. Effect of acute resistance exercise on postexercise energy expenditure and resting metabolic rate. J Appl Physiol. 1993;75(4):1847–53.
Monteiro AG, Alveno DA, Prado M, Monteiro GA, Ugrinowitsch C, Aoki MS, et al. Acute physiological responses to different circuit training protocols. J Sports Med Phys Fit. 2008;48(4):438–42.
Mookerjee S, Welikonich MJ, Ratamess NA. Comparison of energy expenditure during single-set vs. multiple-set resistance exercise. J Strength Cond Res. 2016;30(5):1447–52.
Moon JM, Zabriskie HA, Harty PS, Currier BS, Blumkaitis JC, Stecker RA, et al. Comparison of energy expenditure observed between scheduled activities in collegiate team-sport female athletes. Sports. 2021;9(4):02.
Morgan B, Woodruff SJ, Tiidus PM. Aerobic energy expenditure during recreational weight training in females and males. J Sports Sci Med. 2003;2(3):117–22.
Morris CE, Wessel PA, Tinius RA, Schafer MA, Maples JM. Validity of activity trackers in estimating energy expenditure during high-intensity functional training. Res Q Exerc Sport. 2019;90(3):377–84.
Moss SL, Randell RK, Burgess D, Ridley S, ÓCairealláin C, Allison R, et al. Assessment of energy availability and associated risk factors in professional female soccer players. Eur J Sport Sci. 2021;21(6):861–70.
Mukaimoto T, Ohno M. Effects of circuit low-intensity resistance exercise with slow movement on oxygen consumption during and after exercise. J Sports Sci. 2012;30(1):79–90.
Munch GW, Rosenmeier JB, Petersen M, Rinnov AR, Iepsen UW, Pedersen BK, et al. Comparative effectiveness of low-volume time-efficient resistance training versus endurance training in patients with heart failure. J Cardiopulm Rehabil Prev. 2018;38(3):175–81.
Nakagata T, Yamada Y, Naito H. Energy expenditure, recovery oxygen consumption, and substrate oxidation during and after body weight resistance exercise with slow movement compared to treadmill walking. Physiol Int. 2018;105(4):371–85.
Nakagata T, Yamada Y, Naito H. Metabolic equivalents of body weight resistance exercise with slow movement in older adults using indirect calorimetry. Appl Physiol Nutr Metab. 2019;44(11):1254–7.
Nakagata T, Yamada Y, Naito H. Estimating energy cost of body weight resistance exercise using a multistage exercise test. J Strength Cond Res. 2022;36(5):1290–6.
Nunez TP, Amorim FT, Beltz NM, Mermier CM, Moriarty TA, Nava RC, et al. Metabolic effects of two high-intensity circuit training protocols: does sequence matter? J Exerc Sci Fit. 2020;18(1):14–20.
Ortego AR, Dantzler DK, Zaloudek A, Tanner J, Khan T, Panwar R, et al. Effects of gender on physiological responses to strenuous circuit resistance exercise and recovery. J Strength Cond Res. 2009;23(3):932–8.
Paduan Joaquim D, Ridel Juzwiak C, Winckler C. Do paralympic track and field athletes have low energy availability?/Os atletas do atletismo paralímpico tem baixa energia disponível? Braz J Kineanthr Hum Perform. 2018;20(1):71–81.
Pafili ZK, Bogdanis GC, Maridaki M. Cardiorespiratory characteristics and cholesterol responses to a single session of heavy leg press exercise. J Sports Sci Med. 2010;9(4):580–6.
Parmar P, Perry R, Martin J, Vickers S, Baptista R, Edwards R, et al. Net energy costs from resistive exercise done on flywheel-based hardware. Isokinet Exerc Sci. 2015;23(4):221–7.
Petitt DS, Arngrimsson SA, Cureton KJ. Effect of resistance exercise on postprandial lipemia. J Appl Physiol. 2003;94(2):694–700.
Phillips WT, Ziuraitis JR. Energy cost of the ACSM single-set resistance training protocol. J Strength Cond Res. 2003;17(2):350–5.
Phillips WT, Ziuraitis JR. Energy cost of single-set resistance training in older adults. J Strength Cond Res. 2004;18(3):606–9.
Quintero AP, Bonilla-Vargas KJ, Correa-Bautista JE, Dominguez-Sanchez MA, Triana-Reina HR, Velasco-Orjuela GP, et al. Acute effect of three different exercise training modalities on executive function in overweight inactive men: a secondary analysis of the BrainFit study. Physiol Behav. 2018;197:22–8.
Rangan VV, Willis LH, Slentz CA, Bateman LA, Shields AT, Houmard JA, et al. Effects of an 8-month exercise training program on off-exercise physical activity. Med Sci Sports Exerc. 2011;43(9):1744–51.
Ratamess NA, Bush JA, Kang J, Kraemer WJ, Stohs SJ, Nocera VG, et al. The effects of supplementation with p-synephrine alone and in combination with caffeine on metabolic, lipolytic, and cardiovascular responses during resistance exercise. J Am Coll Nutr. 2016;35(8):657–69.
Ratamess NA, Falvo MJ, Mangine GT, Hoffman JR, Faigenbaum AD, Kang J. The effect of rest interval length on metabolic responses to the bench press exercise. Eur J Appl Physiol. 2007;100(1):1–17.
Ratamess NA, Kang J, Kuper JD, O’Grady EA, Ellis NL, Vought IT, et al. Acute cardiorespiratory and metabolic effects of a sandbag resistance exercise protocol. J Strength Cond Res. 2018;32(6):1491–502.
Ratamess NA, Rosenberg JG, Kang J, Sundberg S, Izer KA, Levowsky J, et al. Acute oxygen uptake and resistance exercise performance using different rest interval lengths: the influence of maximal aerobic capacity and exercise sequence. J Strength Cond Res. 2014;28(7):1875–88.
Ratamess NA, Rosenberg JG, Klei S, Dougherty BM, Kang J, Smith CR, et al. Comparison of the acute metabolic responses to traditional resistance, body-weight, and battling rope exercises. J Strength Cond Res. 2015;29(1):47–57.
Rawson ES, Walsh TM. Estimation of resistance exercise energy expenditure using accelerometry. Med Sci Sports Exerc. 2010;42(3):622–8.
Realzola RA, Mang ZA, Millender DJ, Beam JR, Bellovary BN, Wells AD, et al. Metabolic profile of reciprocal supersets in young, recreationally active women and men. J Strength Cond Res. 2021;27:27.
Reed J, De Souza MJ, Williams N. Changes in energy availability across the season in Division I female soccer players. J Sports Sci. 2013;31(3):314–24.
Reed JL, De Souza MJ, Kindler JM, Williams NI. Nutritional practices associated with low energy availability in Division I female soccer players. J Sports Sci. 2014;32(16):1499–509.
Reeve MD, Pumpa KL, Ball N. Accuracy of the SenseWear Armband Mini and the BodyMedia FIT in resistance training. J Sci Med Sport. 2014;17(6):630–4.
Reis VM, Vianna JM, Barbosa TM, Garrido N, Vilaca Alves J, Carneiro AL, et al. Are wearable heart rate measurements accurate to estimate aerobic energy cost during low-intensity resistance exercise? PLoS One [Electronic Resource]. 2019;14(8): e0221284.
Robergs RA, Gordon T, Reynolds J, Walker TB. Energy expenditure during bench press and squat exercises. J Strength Cond Res. 2007;21(1):123–30.
Roberson KB, Jacobs KA, White MJ, Signorile JF. Loads and movement speed affect energy expenditure during circuit resistance exercise. Appl Physiol Nutr Metab. 2017;42(6):637–46.
Rustaden AM, Gjestvang C, Bo K, Haakstad LAH, Paulsen G. Similar energy expenditure during bodypump and heavy load resistance exercise in overweight women. Front Physiol. 2020;11:570.
Salagaras BS, Mackenzie-Shalders KL, Nelson MJ, Fraysse F, Wycherley TP, Slater GJ, et al. Comparisons of daily energy intake vs. expenditure using the GeneActiv Accelerometer in elite Australian football athletes. J Strength Cond Res. 2021;35(5):1273–8.
Salagaras BS, Mackenzie-Shalders KL, Slater GJ, McLellan C, Coffey VG. Increased carbohydrate availability effects energy and nutrient periodisation of professional male athletes from the Australian Football League. Appl Physiol Nutr Metab. 2021;46(12):1510–6.
Santa-Clara H, Melo X, Willi R, Pinto R, Santos V, Almeida JP, et al. Energy expenditure during an exercise training session for cardiac patients. Appl Physiol Nutr Metab. 2018;43(3):292–8.
Santos DA, Silva AM, Matias CN, Magalhaes JP, Fields DA, Minderico CS, et al. Validity of a combined heart rate and motion sensor for the measurement of free-living energy expenditure in very active individuals. J Sci Med Sport. 2014;17(4):387–93.
Sarafian D, Schutz Y, Montani J-P, Dulloo AG, Miles-Chan JL. Sex difference in substrate oxidation during low-intensity isometric exercise in young adults. Appl Physiol Nutr Metab. 2016;41(9):977–84.
Schaal K, VanLoan MD, Hausswirth C, Casazza GA. Decreased energy availability during training overload is associated with non-functional overreaching and suppressed ovarian function in female runners. Appl Physiol Nutr Metab. 2021;46(10):1179–88.
Scott CB. Contribution of blood lactate to the energy expenditure of weight training. J Strength Cond Res. 2006;20(2):404–11.
Scott JM, Hackney K, Downs M, Guined J, Ploutz-Snyder R, Fiedler J, et al. The metabolic cost of an integrated exercise program performed during 14 days of bed rest. Aviat Space Environ Med. 2014;85(6):612–7.
Seliger V, Dolejs L, Karas V. A dynamometric comparison of maximum eccentric, concentric, and isometric contractions using EMG and energy expenditure measurements. Eur J Appl Physiol Occup Physiol. 1980;45(2–3):235–44.
Seliger V, Dolejs L, Karas V, Pachlopnikova I. Adaptation of trained athletes’ energy expediture to repeated concentric and eccentric muscle contractions. Int Z Angew Physiol. 1968;26(3):227–34.
Shannon KA, Shannon RM, Clore JN, Gennings C, Warren BJ, Potteiger JA. Resistance exercise and postprandial lipemia: the dose effect of differing volumes of acute resistance exercise bouts. Metabolism. 2005;54(6):756–63.
Stec MJ, Rawson ES. Estimation of resistance exercise energy expenditure using triaxial accelerometry. J Strength Cond Res. 2012;26(5):1413–22.
Steele J, Butler A, Comerford Z, Dyer J, Lloyd N, Ward J, et al. Similar acute physiological responses from effort and duration matched leg press and recumbent cycling tasks. PeerJ. 2018;6: e4403.
Thornton MK, Potteiger JA. Effects of resistance exercise bouts of different intensities but equal work on EPOC. Med Sci Sports Exerc. 2002;34(4):715–22.
Thornton MK, Rossi SJ, McMillan JL. Comparison of two different resistance training intensities on excess post-exercise oxygen consumption in African American women who are overweight. J Strength Cond Res. 2011;25(2):489–96.
Tornberg AB, Melin A, Koivula FM, Johansson A, Skouby S, Faber J, et al. Reduced neuromuscular performance in amenorrheic elite endurance athletes. Med Sci Sports Exerc. 2017;49(12):2478–85.
Trexler ET, Keith DS, Lucero AA, Stoner L, Schwartz TA, Persky AM, et al. Effects of citrulline malate and beetroot juice supplementation on energy metabolism and blood flow during submaximal resistance exercise. J Diet Suppl. 2020;17(6):698–717.
Trexler ET, Keith DS, Schwartz TA, Ryan ED, Stoner L, Persky AM, et al. Effects of citrulline malate and beetroot juice supplementation on blood flow, energy metabolism, and performance during maximum effort leg extension exercise. J Strength Cond Res. 2019;33(9):2321–9.
van Etten LM, Westerterp KR, Verstappen FT, Boon BJ, Saris WH. Effect of an 18-wk weight-training program on energy expenditure and physical activity. J Appl Physiol. 1997;82(1):298–304.
van Etten LM, Westerterp KR, Verstappen TJ. Daily variation in energy expenditure during weight-training versus continuous arm cranking and cycling. Int J Sports Med. 1996;17(7):497–503.
Vandenbrink DN, Petrella NJ, Neufeld EV, Dolezal BA, Maclennan DP. Metabolic responses to a loaded movement training workout. J Sports Med Phys Fit. 2018;58(1–2):35–42.
Vezina JW, Der Ananian CA, Campbell KD, Meckes N, Ainsworth BE. An examination of the differences between two methods of estimating energy expenditure in resistance training activities. J Strength Cond Res. 2014;28(4):1026–31.
Vincent HK, Percival S, Creasy R, Alexis D, Seay AN, Laura Ann Z, et al. acute effects of enhanced eccentric and concentric resistance exercise on metabolism and inflammation. J Novel Physiother. 2014;4(2).
Walker EJ, McAinch AJ, Sweeting A, Aughey RJ. Inertial sensors to estimate the energy expenditure of team-sport athletes. J Sci Med Sport. 2016;19(2):177–81.
Wickham JB, Mullen NJ, Whyte DG, Cannon J. Comparison of energy expenditure and heart rate responses between three commercial group fitness classes. J Sci Med Sport. 2017;20(7):667–71.
Williams BM, Kraemer RR. Comparison of cardiorespiratory and metabolic responses in kettlebell high-intensity interval training versus sprint interval cycling. J Strength Cond Res. 2015;29(12):3317–25.
Wilmore JH, Parr RB, Ward P, Vodak PA, Barstow TJ, Pipes TV, et al. Energy cost of circuit weight training. Med Sci Sports. 1978;10(2):75–8.
Yoshida A, Ishikawa-Takata K, Tanaka S, Suzuki N, Nakae S, Murata H, et al. Validity of combination use of activity record and accelerometry to measure free-living total energy expenditure in female endurance runners. J Strength Cond Res. 2019;33(11):2962–70.
Zanders BR, Currier BS, Harty PS, Zabriskie HA, Smith CR, Stecker RA, et al. Changes in energy expenditure, dietary intake, and energy availability across an entire collegiate women’s basketball season. J Strength Cond Res. 2021;35(3):804–10.
Zotou E, Magkos F, Koutsari C, Fragopoulou E, Nomikos T, Sidossis LS, et al. Acute resistance exercise attenuates fasting and postprandial triglyceridemia in women by reducing triglyceride concentrations in triglyceride-rich lipoproteins. Eur J Appl Physiol. 2010;110(4):869–74.
Curtis C, Arjomandkhah N, Cooke C, Ranchordas MK, Russell M. Estimated energy expenditures and energy intakes of international female rugby sevens players in five days of a training camp and competition preparation. Nutrients. 2023.
del-cuerpo i, Jerez-Mayorga D, Chirosa-Ríos LJ, Morenas-Aguilar MD, Mariscal-Arcas M, López-Moro A, et al. Males have a higher energy expenditure than females during squat training. Nutrients. 2023.
McGuire A, Warrington G, Doyle L. Prevalence of low energy availability and associations with seasonal changes in salivary hormones and IgA in elite male Gaelic footballers. Eur J Nutr. 2023;62(4):1809–20.
Michalski AC, de Freitas FG, Midgley AW, Billinger SA, Costa VAB, dos Santos TR, et al. Can mixed circuit training elicit the recommended exercise intensity and energy expenditure in people after stroke? Top Stroke Rehabil. 2023;30(8):751–67.
Scheffer JH, Dunshea-Mooij CAE, Armstrong S, MacManus C, Kilding AE. Prevalence of low energy availability in 25 New Zealand elite female rowers—a cross sectional study. J Sci Med Sport. 2023;26(12):640–5.
Smith LE, Van Guilder GP, Dalleck LC, Harris NK. The effects of a single session of high intensity functional training on energy expenditure, VO(2), and blood lactate. J Sports Sci Med. 2022;21(4):545–54.
Traversa C, Nyman DLE, Spriet LL. Dietary intake over a 7-day training and game period in female varsity Rugby Union Players. Nutrients. 2022.
Weir JBV. New methods for calculating metabolic rate with special reference to protein metabolism. J Physiol. 1949;109(1–2):1–9.
Rhea MR, Alvar BA, Burkett LN, Ball SD. A meta-analysis to determine the dose response for strength development. Med Sci Sports Exerc. 2003;35(3):456–64.
Cormie P, McGuigan MR, Newton RU. Developing maximal neuromuscular power. Sports Med. 2011;41(2):125–46.
Schoenfeld BJ, Fisher J, Grgic J, Haun C, Helms ER, Phillips S, et al. Resistance training recommendations to maximize muscle hypertrophy in an athletic population: position stand of the IUSCA. Int J Strength Cond. 2021;1(1).
Scott CB. Contribution of anaerobic energy expenditure to whole body thermogenesis. Nutr Metab (Lond). 2005;2(1):14.
Tesch PA, Colliander EB, Kaiser P. Muscle metabolism during intense, heavy-resistance exercise. Eur J Appl Physiol Occup Physiol. 1986;55(4):362–6.
Tesch PA, Ploutz-Snyder LL, Ystrom L, Castro MJ, Dudley GA. Skeletal muscle glycogen loss evoked by resistance exercise. J Strength Cond Res. 1998;12(2):67–73.
Koopman R, Manders RJF, Jonkers RAM, Hul GBJ, Kuipers H, van Loon LJC. Intramyocellular lipid and glycogen content are reduced following resistance exercise in untrained healthy males. Eur J Appl Physiol. 2006;96(5):525–34.
Hokken R, Laugesen S, Aagaard P, Suetta C, Frandsen U, Ørtenblad N, et al. Subcellular localization- and fibre type-dependent utilization of muscle glycogen during heavy resistance exercise in elite power and Olympic weightlifters. Acta Physiol. 2021;231(2): e13561.
Schiaffino S, Reggiani C. Fiber types in mammalian skeletal muscles. Physiol Rev. 2011;91(4):1447–531.
Burt DG, Lamb K, Nicholas C, Twist C. Effects of exercise-induced muscle damage on resting metabolic rate, sub-maximal running and post-exercise oxygen consumption. Eur J Sport Sci. 2014;14(4):337–44.
Murgatroyd PR, Davies HL, Prentice AM. Intra-individual variability and measurement noise in estimates of energy expenditure by whole body indirect calorimetry. Br J Nutr. 1987;58(3):347–56.
Zanuso S, Bergamin M, Jimenez A, Pugliese G, D’Errico V, Nicolucci A, et al. Determination of metabolic equivalents during low- and high-intensity resistance exercise in healthy young subjects and patients with type 2 diabetes. Biol Sport. 2016;33(1):77–82.
Conger SA, Bassett DR. A compendium of energy costs of physical activities for individuals who use manual wheelchairs. Adapt Phys Act Q. 2011;28(4):310–25.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
At no point was funding received by any of the authors for the writing of this manuscript. The publishing of this article open access has been made possible through the Australian Catholic University Read and Publish Agreement.
Conflict of interest
Lachlan Mitchell, Luke Wilson, Grant Duthie, Kate Pumpa, Jonathon Weakley, Christopher Scott and Gary Slater declare that they have no conflicts of interest relevant to the content of this review.
Author contributions
The search strategy was developed by L.M., G.D. and G.S. L.M. conducted the search. L.M. and L.W. screened and selected studies. Data extraction was performed by L.M., L.W., G.D., K.P., J.W. and G.S. Data interpretation was performed by L.M., G.D., K.P., C.S. and G.S. L.M. and L.W. conducted the quality appraisal of studies. L.M., G.D., K.P., C.S. and G.S. contributed to the writing of the manuscript. All authors reviewed, refined and approved the final version of the manuscript.
Availability of data and material
All data and material in this manuscript are from peer-reviewed publications.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mitchell, L., Wilson, L., Duthie, G. et al. Methods to Assess Energy Expenditure of Resistance Exercise: A Systematic Scoping Review. Sports Med (2024). https://doi.org/10.1007/s40279-024-02047-8
Accepted:
Published:
DOI: https://doi.org/10.1007/s40279-024-02047-8