Abstract
Background
The modalities and contributions to drug safety of patient adverse drug reaction reporting systems in 50 countries have been reviewed and analysed.
Methods
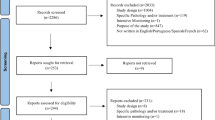
The means made available by National Health Competent Authorities (NCAs) for patients to report drug side effects were compared through literature review and questionnaire.
Results
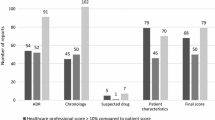
Among the 50 countries included in this study, we found that direct patient reporting systems exist in 44 countries and represent 9 % of total reports, the rest coming from healthcare professionals. Australia was the first, in 1964, and the United States has the system in which patients are the most involved. A total of 27 countries have a patient-specific reporting form, and 31 countries provide a form to complete online. In order to help patients, four countries constrain the description of the reaction and 12 constrain the choice of drug on the reporting form. Most of the surveyed countries request the patient’s medical history (30 countries) and concomitant therapies (41 countries). The total number of fields per form ranges from 6 to 59, with a mean of 36 items.
Conclusions
Most of the surveyed countries have implemented a patient adverse drug reaction reporting system. From this study, it seems that an online reporting form increases the rate of reporting. Currently, many different forms exist worldwide; these should be harmonized by considering the strengths and weaknesses of all existing forms. But above all, to increase the number of reports, each country should promote NCA-initiated adverse drug reactions reporting systems.




Similar content being viewed by others
References
REGULATION (EU) No 1235/2010 OF THE EUROPEAN PARLIAMENT AND OF THE COUNCIL of 15 December 2010 amending, as regards pharmacovigilance of medicinal products for human use, Regulation (EC) No 726/2004 laying down Community procedures for the authorisation and supervision of medicinal products for human and veterinary use and establishing a European Medicines Agency, and Regulation (EC) No 1394/2007 on advanced therapy medicinal products; 2010. http://ec.europa.eu/health/files/eudralex/vol-1/reg_2010_1235/reg_2010_1235_en.pdf. Accessed 21 Oct 2013.
DIRECTIVE 2010/84/EU OF THE EUROPEAN PARLIAMENT AND OF THE COUNCIL of 15 December 2010 amending, as regards pharmacovigilance, Directive 2001/83/EC on the Community code relating to medicinal products for human use; 2010. http://eur-lex.europa.eu/LexUriServ/LexUriServ.do?uri=OJ:L:2010:348:0074:0099:EN:PDF. Accessed 21 Oct 2013.
Directive 2001/83/EC of the European Parliament and of the Council of 6 November 2001 on the community code relating to medicinal products for human use—article 107a. Official Journal L. 2004;311:67–128.
World Health Organization website. http://apps.who.int/medicinedocs/fr/d/Jh1465e/4.html. Accessed 20 Sept 2013.
Egberts TC, Smulders M, de Koning FH, Meyboom RH, Leufkens HG. Can adverse drug reactions be detected earlier? A comparison of reports by patients and professionals. BMJ. 1996;313(7056):530–1.
De Langen J, Van Hunsel F, Passier A, De Jong-Van den Berg L, Van Grootheest K. Adverse drug reaction reporting by patients in the Netherlands: three years of experience. Drug Saf. 2008;31(6):515–24.
Blenkinsopp A, Wilkie P, Wang M, Routledge PA. Patient reporting of suspected adverse drug reactions: a review of published literature and international experience. Br J Clin Pharmacol. 2007;63(2):148–56.
Herxheimer A, Crombag R, Alves TL. Direct patient reporting of adverse drug reactions: a fifteen-country survey and literature review. Health Action International Europe; 2010. http://www.haiweb.org/10052010/10_May_2010_Report_Direct_Patient_Reporting_of_ADRs.pdf. Accessed 20 Jun 2013.
Cumber SL, Heffer SJ, Gandhi S, Avery AJ. The Yellow Card Scheme: experience of patient reporting of adverse drug reactions 5 years since launch. Pharmacoepidemiol Drug Saf. 2010;19:S321.
Van Hunsel F, Härmark L, Pal S, Olsson S, Van Grotheest K. Experiences with adverse drug reaction reporting by patients: an 11-country survey. Drug Saf. 2012;35(1):45–60.
Basch E. The missing voice of patients in drug-safety reporting. N Engl J Med. 2010;362(10):865–9.
Van Hunsel F, Talsma A, Van Puijenbroek E, De Jong-Van den Berg L, Van Grootheest K. The proportion of patient reports of suspected ADRs to signal detection in the Netherlands: case–control study. Pharmacoepidemiol Drug Saf. 2011;20(3):286–91.
Hazell L, Cornelius V, Shakir S, Avery AJ. Patient reporting of adverse drug reactions in the UK: potential signals generated by patients compared to healthcare professionals [poster abstract no. 227]. Pharmacoepidemiol Drug Saf. 2010;19(Suppl. 1):S97–8.
Hazell L, Cornelius V, Hannaford P, Shakir S, Avery AJ. How do patients contribute to signal detection? Drug Saf. 2013;36(3):199–206.
White RW, Tatonetti NP, Shah NH, Altman RB, Horvitz E. Web-scale pharmacovigilance: listening to signals from the crowd. J Am Med Inform Assoc. 2013;20(3):404–8.
Banerjee AK, Okun S, Edwards IR, Wicks P, Smith M, Mayall S, Flamion B, Cleland C, Basch E. Patient-reported outcome measures in safety event reporting—PROSPER consortium guidance. Drug Saf. 2013;36:1129–49.
Van Hunsel F, Van der Welle C, Passier A, Van Puijenbroek E, Van Grootheest K. Motives for reporting adverse drug reactions by patient-reporters in the Netherlands. Eur J Clin Pharmacol. 2010;66(11):1143–50.
Van Hunsel F, Ten Berge EA, Borgsteede SD, Van Grootheest K. What motivates patients to report an adverse drug reaction? Ann Pharmacother. 2010;44(5):936–7.
Anderson C, Krska J, Murphy E, Avery A. The importance of direct patient reporting of suspected adverse drug reactions: a patient perspective. Br J Clin Pharmacol. 2011;72(5):806–22.
http://www.who-umc.org/DynPage.aspx?id=98080&mn1=7347&mn2=7252&mn3=7322&mn4=7324. Accessed 20 Mar 2014.
Hoffmann E, Fouretier A, Vergne C, Bertram D. Pharmacovigilance regulatory requirements in Latin America. Pharm Med. 2012;26:1–12.
Isah AO, Pal SN, Olsson S, Dodoo A, Bencheikh RS. Specific features of medicines safety and pharmacovigilance in Africa. Ther Adv Drug Saf. 2012;3(1):25–34.
http://apps.who.int/medicinedocs/pdf/s4893e/s4893e.pdf. Accessed 20 Mar 2014.
The Erice declaration: the critical role of communication in drug safety. Hugman B Drug Saf. 2006;29(1):91–3.
Avery AJ, Anderson C, Bond CM, et al. Evaluation of patient reporting of adverse drug reactions to the UK ‘Yellow Card Scheme’: literature review, descriptive and qualitative analyses, and questionnaire surveys. Health Technol Assess. 2011;15(20):1–234, iii–iv.
Robertson J, Newby DA. Low awareness of adverse drug reaction reporting systems: a consumer survey. Med J Aust. 2013;199(10):684–6.
Irish Medicines Board. Tract “Medicines and side effects”. http://www.imb.ie/images/uploaded/documents/SideEffects.pdf. Accessed 3 Nov 2013.
9th Call for Proposals 2013—Innovative Medicines Initiative—IMI/DORA_2013-03180. http://www.imi.europa.eu. Accessed 29 Oct 2013.
Singh A, Bhatt P. Comparative evaluation of adverse drug reaction reporting forms for introduction of a spontaneous generic ADR form. J Pharmacol Pharmacother. 2012;3(3):228–32.
Olsson S, Pal SN, Stergachis A, Couper M. Pharmacovigilance activities in 55 low- and middle-income countries: a questionnaire-based analysis. Drug Saf. 2010;33(8):689–703.
Chiahemen T. Interview: how NAFDAC checkmates adverse drug reaction with PRASCOR—Mrs. Osakwe. National Accord Newspaper; 2013.
Funding and conflicts of interest
No sources of funding were used to assist in the preparation of this study. Florence Margraff and Delphine Bertram have no conflicts of interest that are directly relevant to the content of this study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Margraff, F., Bertram, D. Adverse Drug Reaction Reporting by Patients: An Overview of Fifty Countries. Drug Saf 37, 409–419 (2014). https://doi.org/10.1007/s40264-014-0162-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-014-0162-y