Abstract
Background and Objectives
MHAA4549A, a human anti-influenza immunoglobulin (Ig) G1 monoclonal antibody, is being developed to treat patients hospitalized for influenza A infection. This study examined the pharmacokinetics (PKs) of MHAA4549A in a phase IIa, randomized, double-blind, dose-ranging trial in healthy volunteers challenged with influenza A virus.
Methods
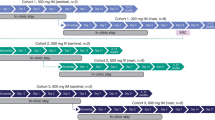
Serum PK data were collected from 60 subjects in three single-dose groups (400, 1200, or 3600 mg) who received MHAA4549A intravenously 24–36 h after inoculation with the influenza A virus. Nasopharyngeal swab MHAA4549A concentration data were collected on days 1–8, and all subjects, including the placebo group, received 75 mg oseltamivir twice daily from days 7 to 11. Plasma samples were collected 4 h postdose on day 8 for oseltamivir and its active metabolite oseltamivir carboxylate (OC) (all subjects, n = 100), including subjects treated with oseltamivir alone and placebo. Noncompartmental analysis was performed for both nasal and serum PKs.
Results
MHAA4549A showed dose-proportional serum PKs with a long terminal half-life (approximately 21.9–24.6 days) and slow clearance (approximately 152–240 mL/day); however, nasopharyngeal swab PKs were not dose proportional. No differences in mean plasma concentrations of oseltamivir and OC at 4 h postdose on day 8 were observed between the MHAA4549A treatment and placebo groups. No subjects who received MHAA4549A developed anti-drug antibodies.
Conclusion
MHAA4549A serum PKs were consistent with that of a human IgG1antibody without known endogenous targets. MHAA4549A showed nonlinear PKs in nasopharyngeal swab samples, which will guide future dose selection to achieve the high drug concentrations needed at the site of action for efficacy. These data demonstrate no PK interactions between MHAA4549A and oseltamivir, and support flat dosing.
Trial Registration
ClinicalTrials.gov identifier, NCT01980966.



Similar content being viewed by others
References
World Health Organization. Influenza (Seasonal). Geneva: World Health Organization; 2014. http://www.who.int/mediacentre/factsheets/fs211/en/. Accessed 9 Oct 2016.
Matias G, Taylor R, Haguinet F, Schuck-Paim C, Lustig R, Shinde V. Estimates of mortality attributable to influenza and RSV in the United States during 1997-2009 by influenza type or subtype, age, cause of death, and risk status. Influ Other Respir Viruses. 2014;8:507–15.
Snacken R, Quinten C, Devaux I, Plata F, Broberg E, Zucs P, et al. Surveillance of hospitalised severe cases of influenza A(H1N1)pdm09 and related fatalities in nine EU countries in 2010-2011. Influ Other Respir Viruses. 2012;6:e93–6.
Finkelman BS, Viboud C, Koelle K, Ferrari MJ, Bharti N, Grenfell BT. Global patterns in seasonal activity of influenza A/H3N2, A/H1N1, and B from 1997 to 2005: viral coexistence and latitudinal gradients. PLoS One. 2007;2:e1296.
Osterholm MT, Kelley NS, Sommer A, Belongia EA. Efficacy and effectiveness of influenza vaccines: a systematic review and meta-analysis. Lancet Infect Dis. 2012;12(1):36–44.
Wang Z, Tobler S, Roayaei J, Eick A. Live attenuated or inactivated influenza vaccines and medical encounters for respiratory illnesses among US military personnel. JAMA. 2009;301(9):945–53.
Tisa V, Barberis I, Faccio V, Paganino C, Trucchi C, Martini M, et al. Quadrivalent influenza vaccine: a new opportunity to reduce the influenza burden. J Prev Med Hyg. 2016;57:E28–33.
Grohskopf LA, Sokolow LZ, Broder KR, Olsen SJ, Karron RA, Jernigan DB, et al. Prevention and control of seasonal influenza with vaccines. MMWR Recomm Rep. 2016;65:1–54.
Neu KE, Henry Dunand CJ, Wilson PC. Heads, stalks and everything else: how can antibodies eradicate influenza as a human disease? Curr Opin Immunol. 2016;42:48–55.
Gerdil C. The annual production cycle for influenza vaccine. Vaccine. 2003;21:1776–9.
Nachbagauer R, Krammer F. Universal influenza virus vaccines and therapeutic antibodies. Clin Microbiol Infect. 2017;23(4):222–8.
de Jong JC, Beyer WE, Palache AM, Rimmelzwaan GF, Osterhaus AD. Mismatch between the 1997/1998 influenza vaccine and the major epidemic A(H3N2) virus strain as the cause of an inadequate vaccine-induced antibody response to this strain in the elderly. J Med Virol. 2000;61:94–9.
Tricco AC, Chit A, Soobiah C, Hallett D, Meier G, Chen MH, et al. Comparing influenza vaccine efficacy against mismatched and matched strains: a systematic review and meta-analysis. BMC Med. 2013;11:153.
Kandel R, Hartshorn KL. Prophylaxis and treatment of influenza virus infection. BioDrugs. 2001;15:303–23.
Kohno S, Kida H, Mizuguchi M. Shimada J; S-021812 Clinical Study Group. Efficacy and safety of intravenous peramivir for treatment of seasonal influenza virus infection. Antimicrob Agents Chemother. 2010;54:4568–74.
Monto AS, Moult AB, Sharp SJ. Effect of zanamivir on duration and resolution of influenza symptoms. Clin Ther. 2000;22:1294–305.
Monto AS, Fleming DM, Henry D, de Groot R, Makela M, Klein T, et al. Efficacy and safety of the neuraminidase inhibitor zanamivir in the treatment of influenza A and B virus infections. J Infect Dis. 1999;180:254–61.
Nicholson KG, Aoki FY, Osterhaus AD, Trottier S, Carewicz O, Mercier CH, et al. Efficacy and safety of oseltamivir in treatment of acute influenza: a randomised controlled trial. Neuraminidase inhibitor flu treatment investigator group. Lancet. 2000;355:1845–50.
Aoki FY, Macleod MD, Paggiaro P, Carewicz O, El Sawy A, Wat C, IMPACT Study Group, et al. Early administration of oral oseltamivir increases the benefits of influenza treatment. J Antimicrob Chemother. 2003;51:123–9.
Nakamura G, Chai N, Park S, Chiang N, Lin Z, Chiu H, et al. An in vivo human-plasmablast enrichment technique allows rapid identification of therapeutic influenza A antibodies. Cell Host Microbe. 2013;14:93–103.
Kamen L, Kho E, Lin YL, Chung S. Anti-influenza antibody MHAA4549A induces ADCC in influenza-infected cells. Presented at the Keystone Symposium on Molecular and Cellular Biology: Antibodies as Drugs (X2). Whistler; 2016 (6–10 March 2016).
Lim JJ, Deng R, Derby MA, Larouche R, Horn P, Anderson M, et al. Two phase 1, randomized, double-blind, placebo-controlled, single ascending-dose studies to investigate the safety, tolerability, and pharmacokinetics of an anti-influenza a monoclonal antibody, MHAA4549A, in healthy volunteers. Antimicrob Agents Chemother. 2016;60:5437–44.
McBride JM, Rosenberger C, Tavel JA, Deng R, Derby MA, Burgess T, et al. Clinical safety and efficacy of MHAA4549A, a novel monoclonal antibodyfor the treatment of severe influenza a: results of a randomized, double-blind, placebo controlled clinical trial [poster No. 20161]. Presented at the Keystone Symposium on Molecular and Cellular Biology: Viral Immunity. Breckenridge; 2015 (11–16 Jan 2015).
Hayden FG, Treanor JJ, Fritz RS, Lobo M, Betts RF, Miller M, et al. Use of the oral neuraminidase inhibitor oseltamivir in experimental human influenza: randomized controlled trials for prevention and treatment. JAMA. 1999;282:1240–6.
Rayner CR, Chanu P, Gieschke R, Boak LM, Jonsson EN. Population pharmacokinetics of oseltamivir when coadministered with probenecid. J Clin Pharmacol. 2008;48:935–47.
Kamal MA, Van Wart SA, Rayner CR, Subramoney V, Reynolds DK, Bulik CC, et al. Population pharmacokinetics of oseltamivir: pediatrics through geriatrics. Antimicrob Agents Chemother. 2013;57:3470–7.
Monto AS, Ceglarek JP, Hayner NS. Liver function abnormalities in the course of a type A (H1N1) influenza outbreak: relation to Reye’s syndrome. Am J Epidemiol. 1981;114:750–9.
Polakos NK, Cornejo JC, Murray DA, Wright KO, Treanor JJ, Crispe IN, et al. Kupffer cell-dependent hepatitis occurs during influenza infection. Am J Pathol. 2006;168:1169–78.
Yingying C. Abnormal liver chemistry in patients with influenza A H1N1. Liver Int. 2011;31:902.
Dirks NL, Meibohm B. Population pharmacokinetics of therapeutic monoclonal antibodies. Clin Pharmacokinet. 2010;49:633–59.
Gupta P, Kamath AV, Park S, Chiu H, Lutman J, Maia M, et al. Preclinical pharmacokinetics of MHAA4549A, a human monoclonal antibody to influenza A virus, and the prediction of its efficacious clinical dose for the treatment of patients hospitalized with influenza A. MAbs. 2016;8:991–7.
Darouiche R, Perkins B, Musher D, Hamill R, Tsai S. Levels of rifampin and ciprofloxacin in nasal secretions: correlation with MIC90 and eradication of nasopharyngeal carriage of bacteria. J Infect Dis. 1990;162:1124–7.
Shelton MJ, Lovern M, Ng-Cashin J, Jones L, Gould E, Gauvin J, et al. Zanamivir pharmacokinetics and pulmonary penetration into epithelial lining fluid following intravenous or oral inhaled administration to healthy adult subjects. Antimicrob Agents Chemother. 2011;55:5178–84.
Wollacott AM, Boni MF, Szretter KJ, Sloan SE, Yousofshahi M, Viswanathan K, et al. Safety and upper respiratory pharmacokinetics of the hemagglutinin stalk-binding antibody VIS410 support treatment and prophylaxis based on population modeling of seasonal influenza A outbreaks. EBioMedicine. 2016;5:147–55.
Adawi A, Bisignano C, Genovese T, Filocamo A, Khouri-Assi C, Neville A, et al. In vitro and in vivo properties of a fully human IgG1 monoclonal antibody that combats multidrug resistant Pseudomonas aeruginosa. Int J Mol Med. 2012;30:455–64.
Ye L, Zeng R, Bai Y, Roopenian DC, Zhu X. Efficient mucosal vaccination mediated by the neonatal Fc receptor. Nat Biotechnol. 2011;29:158–63.
Patel K, Kirkpatrick C, Stroh M, Smith P, Deng R. Population pharmacokinetic/pharmacodynamic (PK/PD) modeling of MHAA4549A, an anti-influenza A monoclonal antibody in healthy subjects challenged with influenza A virus [poster no.A-053]. In: Presented at the 55th Interscience Conference on Antimicrobial Agents and Chemotherapy (ICAAC) Annual Meeting. San Diego; 2015. http://www.abstractsonline.com/Plan/ViewAbstract.aspx?sKey=066fe91c-1dff-48d2-a97e-9d682ce3a71c&cKey=e5865157-b5ac-4d2a-b813-d30a149af1e5&mKey=7a574a80-eab1-4b50-b343-4695df14907e. Accessed 1 Oct 2016 (17–21 Sep 2015).
Lee N, Ison MG. Diagnosis, management and outcomes of adults hospitalized with influenza. Antiviral Ther. 2012;17:143–57.
Deng R, Jin F, Prabhu S, Iyer S. Monoclonal antibodies: what are the pharmacokinetic and pharmacodynamic considerations for drug development? Expert Opin Drug Metab Toxicol. 2012;8:141–60.
Olofsson SK, Cars O. Optimizing drug exposure to minimize selection of antibiotic resistance. Clin Infect Dis. 2007;45(suppl 2):S129–36.
Chai N, Swem LR, Reichelt M, Chen-Harris H, Luis E, Park S, et al. Two escape mechanisms of influenza A virus to a broadly neutralizing stalk-binding antibody. PLoS Pathog. 2016;12:e1005702.
Girish S, Martin SW, Peterson MC, Zhang LK, Zhao H, Balthasar J, et al. AAPS workshop report: strategies to address therapeutic protein-drug interactions during clinical development. AAPS J. 2011;13:405–16.
US FDA. Guidance for Industry. Influenza: developing drugs for treatment and/or prophylaxis; 2011. http://www.fda.gov/downloads/drugs/guidancecomplianceregulatoryinformation/guidances/ucm091219.pdf. Accessed 30 Sep 2016.
Bai S, Jorga K, Xin Y, Jin D, Zheng Y, Damico-Beyer LA, et al. A guide to rational dosing of monoclonal antibodies. Clin Pharmacokinet. 2012;51:119–35.
Wang DD, Zhang S, Zhao H, Men AY, Parivar K. Fixed dosing versus body size-based dosing of monoclonal antibodies in adult clinical trials. J Clin Pharmacol. 2009;49:1012–24.
Zhang S, Shi R, Li C, Parivar K, Wang DD. Fixed dosing versus body size-based dosing of therapeutic peptides and proteins in adults. J Clin Pharmacol. 2012;52:18–28.
Lobo ED, Hansen RJ, Balthasar JP. Antibody pharmacokinetics and pharmacodynamics. J Pharm Sci. 2004;93:2645–68.
Davies BE. Pharmacokinetics of oseltamivir: an oral antiviral for the treatment and prophylaxis of influenza in diverse populations. J Antimicrob Chemother. 2010;65(suppl 2):ii5–10.
He G, Massarella J, Ward P. Clinical pharmacokinetics of the prodrug oseltamivir and its active metabolite Ro 64-0802. Clin Pharmacokinet. 1999;37:471–84.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Michael A. Derby is a former employee of, and Rong Deng, Ai Ping Lee, Mauricio Maia, Jeremy J. Lim, Tracy Burgess, Priscilla Horn, Elizabeth Newton, Jorge A. Tavel, and William D. Hanley are current employees of Genentech, Inc., a subsidiary of the Roche Group. All authors own Roche stock.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
This study was funded by Genentech, Inc. Anshin BioSolutions and Deborah Solymar (Genentech, Inc.) provided assistance with manuscript editing and writing and were funded by Genentech, Inc.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Deng, R., Lee, A.P., Maia, M. et al. Pharmacokinetics of MHAA4549A, an Anti-Influenza A Monoclonal Antibody, in Healthy Subjects Challenged with Influenza A Virus in a Phase IIa Randomized Trial. Clin Pharmacokinet 57, 367–377 (2018). https://doi.org/10.1007/s40262-017-0564-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-017-0564-y