Abstract
Objective
Recent evidences suggested that hypertension was associated with changes in gut microbiota composition. As intervention with probiotics might be considered as one of the approaches for modulating gut microbiota, the objective of the present study was to systematically review the meta-analyses of controlled trials (CTs) to elucidate the effects of probiotics on blood pressure.
Methods
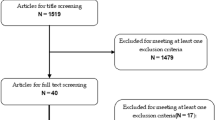
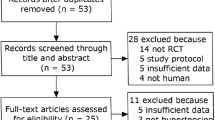
We searched PubMed, Web of Science, and Cochrane Library databases until November 2019 to explore all the meta-analyses conducted on the CTs assessing the efficacy of probiotics in the management of blood pressure (BP). Meta-analyses performed on in vitro, animal or observational studies were excluded from the study. References of the included studies were also screened to obtain further eligible publications.
Results
From the 111 records which were identified during the literature search, 5 meta-analyses met the selection criteria. Total sample size was 2703 subjects (1009 subjects with type 2 diabetes mellitus (T2DM)), aged 12–75 years from both sexes. Results of meta-analyses have been shown a moderate effect of probiotics on BP in hypertensive adults with/without T2DM; from 3.10 to 5.04 mmHg for systolic blood pressure (SBP) and from 0.39 to 3.84 mmHg for diastolic blood pressure (DBP) after 3–24 weeks consumption. These effects were greater in adults with BP ≥ 130/85, by dairy products, by Asian fermented products with multiple species and higher dose of probiotics (≥ 1011 colony forming units (CFU)).
Conclusion
It seems probiotic foods and supplements which were contained high dose multiple species of probiotic bacteria could be more effective in BP control.

Similar content being viewed by others
Availability of data
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
Abbreviations
- HTN:
-
Hypertension
- SBP:
-
Systolic blood pressure
- DALYs:
-
Disability-adjusted life-years
- SCFAs:
-
Short chain fatty acids
- RCTs:
-
Randomized clinical trials
- PRISMA:
-
Preferred Reporting Items for Systematic reviews and Meta-Analyses
- CTs:
-
Controlled trials
- AMSTAR:
-
Multiple Systematic Reviews’
- T2DM:
-
Type 2 diabetes
- MetS:
-
Metabolic syndrome
- DBP:
-
Diastolic blood pressure
- CFU:
-
Colony forming units
- ACE:
-
Angiotensin-converting enzyme
- NO:
-
Nitric oxide
References
Forouzanfar MH, Liu P, Roth GA, Ng M, Biryukov S, Marczak L, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990–2015. JAMA. 2017;317(2):165–82.
Qin J, Li R, Raes J, Arumugam M, Burgdorf KS, Manichanh C, et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature. 2010;464(7285):59–65.
Quigley EMM. Gut bacteria in health and disease. Gastroenterol Hepatol (N Y). 2013;9(9):560–9.
Yang T, Santisteban MM, Rodriguez V, Li E, Ahmari N, Carvajal JM, et al. Gut dysbiosis is linked to hypertension. Hypertension. 2015;65(6):1331–40.
Pluznick JL (2017) Microbial short-chain fatty acids and blood pressure regulation. Curr Hypertens Rep 19(4):25. https://doi.org/10.1007/s11906-017-0722-5
Yan Q, Gu Y, Li X, Yang W, Jia L, Chen C, et al. Alterations of the gut microbiome in hypertension. Front Cell Infect Microbiol 2017;7(381). https://doi.org/10.3389/fcimb.2017.00381.
Gibson GR, Hutkins R, Sanders ME, Prescott SL, Reimer RA, Salminen SJ, et al. Expert consensus document: The International Scientific Association for Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of prebiotics. Nat Rev Gastroenterol Hepatol. 2017;14(8):491–502.
Moro-García MA, Alonso-Arias R, Baltadjieva M, Benítez CF, Barrial MAF, Ruisánchez ED, et al. Oral supplementation with Lactobacillus delbrueckii subsp. bulgaricus 8481 enhances systemic immunity in elderly subjects. Age. 2013;35(4):1311–26.
Tong X, Dong J, Wu Z, Li W, Qin L. Dairy consumption and risk of type 2 diabetes mellitus: a meta-analysis of cohort studies. Eur J Clin Nutr. 2011;65(9):1027. https://doi.org/10.1038/ejcn.2011.62
Dalmeijer GW, Struijk EA, Van Der Schouw YT, Soedamah-Muthu SS, Verschuren WM, Boer JM, et al. Dairy intake and coronary heart disease or stroke—a population-based cohort study. Int J Cardiol. 2013;167(3):925–9.
Dong JY, Szeto IM, Makinen K, Gao Q, Wang J, Qin LQ, Zhao Y. Effect of probiotic fermented milk on blood pressure: a meta-analysis of randomized controlled trials. Br J Nutr. 2013;110(7):1188–94. https://doi.org/10.1017/S0007114513001712.
Khalesi S, Sun J, Buys N, Jayasinghe R. Effect of probiotics on blood pressure: a systematic review and meta-analysis of randomized, controlled trials. Hypertension. 2014;64(4):897–903. https://doi.org/10.1161/HYPERTENSIONAHA.114.03469.
He J, Zhang F, Han Y. Effect of probiotics on lipid profiles and blood pressure in patients with type 2 diabetes: a meta-analysis of RCTs. Med (Baltim). 2017;96(51):e9166. https://doi.org/10.1097/MD.0000000000009166.
Hendijani F, Akbari V. Probiotic supplementation for management of cardiovascular risk factors in adults with type II diabetes: a systematic review and meta-analysis. Clin Nutr. 2018;37(2):532–41. https://doi.org/10.1016/j.clnu.2017.02.015.
Dong Y, Xu M, Chen L, Bhochhibhoya A. Probiotic foods and supplements interventions for metabolic syndromes: a systematic review and meta-analysis of recent clinical trials. Ann Nutr Metab. 2019;74(3):224–41. https://doi.org/10.1159/000499028.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4(1):1. https://doi.org/10.1186/2046-4053-4-1.
Shea BJ, Grimshaw JM, Wells GA, Boers M, Andersson N, Hamel C, et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol. 2007;7(1):10.
Jose PA, Raj D. Gut microbiota in hypertension. Curr Opin Nephrol Hypertens. 2015;24(5):403–9. https://doi.org/10.1097/MNH.0000000000000149.
Noce A, Marrone G, Daniele FD, Ottaviani E, Jones G, Bernini R, Romani A, Rovella V. Impact of gut microbiota composition on onset and progression of chronic non-communicable diseases. Nutrients. 2019;11:1073. https://doi.org/10.3390/nu11051073.
Upadrasta A, Madempudi RS. Probiotics and blood pressure: current insights. Integr Blood Press Control. 2016;9:33–42. https://doi.org/10.2147/IBPC.S73246.
Sircana A, Michieli FD, Parente R, Framarin L, Leone N, Berrutti M, Paschetta E, Bongiovanni D, Musso G. Gut microbiota, hypertension and chronic kidney disease: recent advances. Pharmacol Res. 2019;144:390–408.
Schiffrin EJ, Thomas DR, Kumar VB, Brown C, Hager C, Van’t Hof MA, Morley JE, Guigoz Y. Systemic inflammatory markers in older persons: the effect of oral nutritional supplementation with prebiotics. J Nutr Health Aging. 2007;11(6):475–9.
Daliri EBM, Lee BH, Oh DH. Current perspectives on antihypertensive probiotics. Probiotics Antimicrob Proteins. 2017;9:91–101.
Tanida M, Yamano T, Maeda K, Okumura N, Fukushima Y, Nagai K. Effects of intraduodenal injection of Lactobacillus johnsonii La1 on renal sympathetic nerve activity and blood pressure in urethane-anesthetized rats. Neurosci Lett. 2005;389:109–14.
Gomez-Guzman M, Toral M, Romero M, Jimenez R, Galindo P, Sanchez M, Zarzuelo MJ, Olivares M, Galvez J, Duarte J. Antihypertensive effects of probiotics Lactobacillus strains in spontaneously hypertensive rats. Mol Nutr Food Res. 2015;59:2326–36.
Toral M, Gómez-Guzmán M, Jiménez R, Romero M, Sánchez M, Utrilla MP, et al. The probiotic Lactobacillus coryniformis CECT5711 reduces the vascular pro-oxidant and proinflammatory status in obese mice. Clin Sci (Lond). 2014;127:33–45.
Parnell JA, Reimer RA. Prebiotic fibres dose-dependently increase satiety hormones and alter Bacteroidetes and Firmicutes in lean and obese JCR: LA-cp rats. Br J Nutr. 2012;107(4):601–13.
Xu J, Ahren IL, Prykhodko O, Olsson C, Ahrne S, Molin G. Intake of Blueberry fermented by Lactobacillus plantarum affects the gut microbiota of L-NAME treated rats. Evid Based Complement Altern Med. 2013;2013:809128
Ahren IL, Xu J, Onning G, Olsson C, Ahrne S, Molin G. Antihypertensive activity of blueberries fermented by Lactobacillus plantarum DSM 15313 and effects on the gut microbiota in healthy rats. Clin Nutr. 2015;34:719–26.
Jauhiainen T, Vapaatalo H, Poussa T, Kyronpalo S, Rasmussen M, Korpela R. Lactobacillus helveticus fermented milk lowers blood pressure in hypertensive subjects in 24-h ambulatory blood pressure measurement. Am J Hypertens. 2005;18:1600–5.
Koppe L, Mafra D, Fouque D. Probiotics and chronic kidney disease. Kidney Int. 2015;88:958–66.
Blood Pressure Lowering Treatment Trialists’ Collaboration; Ninomiya T, Perkovic V, Turnbull F, Neal B, Barzi F, Cass A, Baigent C, Chalmers J, Li N, et al. Blood pressure lowering and major cardiovascular events in people with and without chronic kidney disease: Meta-analysis of randomised controlled trials. BMJ 2013; 347: f5680.
Aoyagi Y, Park S, Matsubar S, Honda Y, Amamoto R, Kushiro A, Miyazaki K, Shephard RJ. Habitual intake of fermented milk products containing Lactobacillus casei strain Shirota and a reduced risk of hypertension in older people. Benef Microbes. 2017;8:23–9.
Yap WB, Ahmad FM, Lim YC, Zainalabidin S. Lactobacillus casei strain C1 attenuates vascular changes in spontaneously hypertensive rats. Korean J Physiol Pharmacol. 2016;20:621–8.
Ardeshirlarijani E, Tabatabaei-Malazy O, Mohseni S, Qorbani M, Larijani B, Baradar Jalili R. Effect of probiotics supplementation on glucose and oxidative stress in type 2 diabetes mellitus: a meta-analysis of randomized trials. DARU J Pharm Sci. 2019;27:827. https://doi.org/10.1007/s40199-019-00302-2.
Mikelsaar M, Zilmer M. Lactobacillus fermentum ME-3- an antimicrobial and antioxidative probiotic. Microb Ecol Health Dis. 2009;21(1):1–27.
Kang Y, Zhang X, Cai Y, et al. Gut microbiota and metabolic disease: from pathogenesis to new therapeutic strategies. Rev Med Microbiol. 2016;27:141–52.
Ejtahed HS, Angoorani P, Soroush AR, Atlasi R, Hasani-Ranjbar S, Mortazavian AM, et al. Probiotics supplementation for the obesity management; A systematic review of animal studies and clinical trials. Journal of Functional Foods. 2019;52:228–42.
Funding
This study was funded by the Endocrinology and Metabolism Research Institute, Tehran University of Medical Sciences, Tehran, Iran.
Author information
Authors and Affiliations
Contributions
HSE and OTM designed the study and drafted the manuscript. EA helped to write of final draft of the manuscript, revision and re-analysis. ZHT helped in data extraction. SHR, ARS and BL helped in quality assessment and interpretation of data. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Consent for publication
Not applicable.
Ethics approval and consent to participate
Not applicable.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 13 kb)
Rights and permissions
About this article
Cite this article
Ejtahed, HS., Ardeshirlarijani, E., Tabatabaei-Malazy, O. et al. Effect of probiotic foods and supplements on blood pressure: a systematic review of meta-analyses studies of controlled trials. J Diabetes Metab Disord 19, 617–623 (2020). https://doi.org/10.1007/s40200-020-00525-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-020-00525-0