Abstract
Cardiovascular diseases (CVDs) remain a major health concern worldwide, where mesenchymal stem cells (MSCs) therapy gives great promise in their management through their regenerative and paracrine actions. In recent years, many studies have shifted from the use of transplanted stem cells to their secreted exosomes for the management of various CVDs and cardiovascular-related diseases including atherosclerosis, stroke, myocardial infarction, heart failure, peripheral arterial diseases, and pulmonary hypertension. In different models, MSC-derived exosomes have shown beneficial outcomes similar to cell therapy concerning regenerative and neovascular actions in addition to their anti-apoptotic, anti-remodeling, and anti-inflammatory actions. Compared with their parent cells, exosomes have also demonstrated several advantages, including lower immunogenicity and no risk of tumor formation. However, the maintenance of stability and efficacy of exosomes after in vivo transplantation is still a major concern in their clinical application. Recently, new approaches have been developed to enhance their efficacy and stability including their preconditioning before transplantation, use of genetically modified MSC-derived exosomes, or their utilization as a targeted drug delivery system. Herein, we summarized the use of MSC-derived exosomes as therapies in different CVDs in addition to recent advances for the enhancement of their efficacy in these conditions.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Mesenchymal stem cells (MSCs) are multipotent adult progenitor cells with differentiation and self-renewal capabilities. They could be isolated from various sources, including adipose tissues, umbilical cord blood, bone marrow (BM) [1, 2]. MSCs have been revealed as a promising candidate in different cardiovascular diseases (CVDs) [3,4,5]. The therapeutic potential of MSCs has been proposed to depend partly on their capacity to secrete extracellular vesicles (EVs) and other paracrine factors [6,7,8,9].
EVs consist mainly of exosomes, microvesicles, and apoptotic bodies. MSC-derived exosomes display biological functions similar to MSCs, contributing to tissue regeneration by enclosing and conveying various cytokines (e.g., interleukin (IL)-6 and IL-10) [10, 11], growth factors (e.g., transforming growth factor beta and hepatocyte growth factor (HGF)) [12, 13], signaling lipids [14], mRNAs (e.g., insulin-like growth factor 1 receptor (IGF-1R) [15], and regulatory miRNAs (e.g., miRNA-21 and miRNA-133b) [16, 17]. Exosomes have demonstrated several advantages over pure cell treatments, including lower immunogenicity and no risk of tumor formation [18].
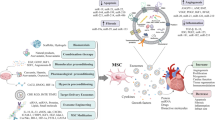
Recent studies have shown that MSC-derived exosomes could represent a novel therapeutic approach for the management of different CVDs and cardiovascular-related diseases (Fig. 1). Essentially, exosomes secreted by MSCs have revealed significant roles in cytoprotection, stimulation of angiogenesis, inhibition of cardiac fibroblast development, and modulation of macrophage infiltration in the infarcted region [19, 20].
Moreover, several preclinical studies have confirmed that MSC-derived exosomes reduced the infarct size, leading to the recovery of blood flow and improvement of post-myocardial infarction cardiac function [21,22,23]. Despite these significant benefits, the clinical application of exosomes reveals several limitations including the maintenance of efficacy and stability of exosomes over time after in vivo transplantation [24]. Thus, new approaches have been continuously developed to enhance their efficacy and stability including their preconditioning before transplantation, use of genetically modified MSC-derived exosomes, or their utilization as a targeted drug delivery system [25].
2 MSC-derived exosomes and their origin
Since their first successful transplantation in 1968 [26], cell therapies have been used as an alternative therapy in various diseases, particularly CVDs [27,28,29]. Stem cell-based therapies could repair the damaged cardiomyocytes and subsequently improve cardiac function in several preclinical and some clinical trials [30]. However, their clinical applications have limitations, including low survival and engraftment, immune rejection, and risk of tumorigenic potential [31].
Interestingly, stem cells can repair injured tissues via paracrine actions through their derived exosomes [32]. Exosomes are a homogenous population of EVs that originate from endosomes and are released by parent cells extracellularly. Exosomes are nanosized vesicles with a diameter of 30–100 nm; thus, they differ from other EVs that originate from the plasma membrane with a diameter of 100–1000 nm. Exosomes are novel mediators of cell-to-cell signaling and communication through the transfer of mRNA, regulatory miRNAs, cytokines, peptides, and signaling lipids leading to information transfer and coordinative function between cells [33].
Exosomes, as nanosized EVs, are distributed through a vast complex of body fluids, which represents a challenge in their isolation. Several types of exosome separation strategies have been reported till now, including ultrafiltration, ultra-speed centrifugation, charge neutralization-based polymer precipitation, immunoaffinity capture, size-exclusion chromatograph, and microfluidic techniques [34]. Despite being the standard technique for exosome separation because of its high processing capacity, ultra-speed centrifugation reveals lipoprotein contamination and high levels of protein aggregate in separated exosomes, which greatly affect their quantification and functional analysis using this technique [35]. Thus, tremendous efforts to explore the different physiochemical and biochemical properties of exosomes have been made to improve their separation.
Moreover, exosomes could be isolated from a cell culture medium by different methods to enhance their isolation outcome. Compared with the traditional isolation method using ultracentrifugation, the method based on tangential flow filtration increases the isolation yield of exosomes that originate from human umbilical cord MSCs (UCMSCs) 92.5 times [36]. The serum-depletion process has also yielded highly purified and clinically active exosomes from their cell culture medium [36]. By using a MSC surface marker (CD73), the purity of UCMSC-derived exosomes was reported to be enhanced 15.6 times using the process of depleting fetal bovine serum (FBS)-derived exosomes. Moreover, impurities resulting from FBS assessed by low-density lipoprotein-cholesterol levels were negligibly detected in the isolated exosomes. The angiogenic effects of highly purified UCMSC-derived exosomes were enhanced by approximately 71.4% in vitro using human coronary artery endothelial cells. Thus, the improvement of the purity and yield of MSC-derived exosomes affects their angiogenic and regenerative activities [36].
Exosomes could be regarded as mediators and biomarkers of various diseases including CVDs. The Osaka Acute Coronary Insufficiency Study revealed a positive correlation between the development of heart failure (HF) and levels of p53-responsive miRNAs inside EVs [37]. Levels of exosomal miRNA-9 and miRNA-124 could be used as promising biomarkers for the diagnosis of acute ischemic stroke, together with the serum IL-6 level, National Institutes of Health Stroke Scale (NIHSS) scores, and infarct sizes [38]. In addition, the exosomes isolated from monocrotaline-treated mice and patients with idiopathic pulmonary hypertension (PH) contained increased levels of miRNA-19b, miRNA-20a, miRNA-20b, and miRNA-145 [39]. Therefore, these exosomal miRNAs could be used for the diagnosis and prognosis of various CVDs. On the contrary, they could be used as therapies by acting as signaling agents that are capable of transferring specific peptides or miRNAs to target tissues or cells [40].
Surface markers such as CD9, CD63, and CD81 could characterize exosomes in addition to biogenesis-related specific marker proteins such as TSG101 and ALIX and heat-shock proteins (HSP60, HSP70, and HSP90). However, these markers are not exclusive to exosomes and could be revealed on other EVs [41]. Moreover, compared with their parents, exosomes could express different marker proteins. For example, the known endothelial marker CD144 is not present on exosomes derived from human umbilical vein endothelial cells (HUVECs) [40]. Moreover, the content of exosomes depends on the status of the parent cell [42]. The exosomes originated from chronic myelogenous leukemia were found to stimulate the release of IL-8 from BM stromal cells in addition to the enhancement of the progression of leukemia [43]. On the contrary, MSC-derived exosomes were found to alleviate symptoms in an experimental model of stroke by promoting angiogenesis, neurogenesis, and neurite remodeling [44].
Increasing evidence suggested that exosomes generated from stem cells exerted similar protective and reparative properties to their original cells. MSCs synthesize and secrete functional exosomes that are cholesterol-rich phospholipid vesicles, which afford direct protection of their RNA contents, specifically miRNAs against the action of RNase [45]. The therapeutic outcomes of exosomes and other EVs depend mainly on the delivery of peptides or non-coding RNAs, specifically miRNAs such as miRNA-21, miRNA-22, miRNA-24, and miRNA-29a, which have revealed cardioprotective roles in different diseases, along with other miRNAs [46,47,48,49,50].
3 MSC-derived exosomes as therapy in different CVDs
MSC therapy has been studied in various CVDs, where its beneficial effects depend most probably on the paracrine secretion of bioactive molecules such as small non-coding miRNA. MSC release vesicles of various sizes loaded with miRNAs primarily for cell-to-cell communication. Research has shown that MSC-derived exosomes could accumulate in the ischemic myocardial tissue and regulate cell proliferation, apoptosis, inflammation, and angiogenesis [51, 52]. Exosomes can be used as drug delivery systems by being loaded with the required miRNAs to the target organ of interest, such as the heart. Hence, exosome-based cell-free therapy could be assessed as an alternative to cell-based therapy [53]. Importantly, Wang et al. identified miRNAs in human endometrium-derived MSC (EnMSC)-derived exosomes, particularly miRNA-21, as potential mediators of cardioprotection provided by EnMSC therapy. Thus, exosomes derived from other adult stem cells could be a subject of great attention as an alternative to cell-based therapy for CVDs (Table 1) [54].
3.1 Atherosclerosis
Atherosclerosis is a chronic inflammatory disease of blood vessels that involves multiple processes such as lipid penetration, endothelial dysfunction, inflammatory response, and cell proliferation [55]. The development of atherosclerosis is initiated by endothelial dysfunction, where Zhang et al. [72] found that exosomes loaded with miRNA-155 promote atherosclerosis and induce endothelial injury. On the contrary, MSC-derived exosomes modulate the inflammatory response to atherosclerotic plaques, providing a potential way to prevent atherosclerosis [73]. MSC-derived exosomes also inhibited atherosclerosis in ApoE−/− mice by preventing macrophage infiltration in addition to the promotion of M2 macrophage polarization in atherosclerotic plaques [56]. MSC-secreted exosomal miRNAs, which have been reported to regulate macrophage function, include miRNA-21-5p [63], miRNA-146a [64], miRNA-30a [65], and let-7 [66]. Besides, BM-derived MSC (BM-MSC) exosomal miRNA-133 can downregulate macrophage surface cholesterol efflux-related genes such as ATP-binding cassette subfamily A number 1 and ATP-binding cassette subfamily G number 1, resulting in interrupted cholesterol efflux and inhibiting foam cell formation [74]. MSC-derived exosomes also reverse the polarization status of macrophages by decreasing miRNA-182 expression and inhibiting the inflammation process [75]. Additionally, MSC-derived exosomal miRNA-145 can inhibit atherosclerosis by targeting junction adhesion molecule A (JAM-A) [55].
3.2 Myocardial infarction (MI)
MI is a detrimental outcome of transient or persistent occlusion of coronary arteries with subsequent necrosis of the myocardium and loss of cardiomyocytes [76]. MSC transplantation into the infarcted region could improve cardiac function, a feature that could be enhanced by MSC modification through the upregulation of miRNA-1 that promotes MSC survival and their differentiation into cardiomyocytes [77]. As a compensatory ischemic signaling, exosomes released by the injured cardiomyocytes can transfer peptides and miRNAs to distant organs such as the BM. Moreover, exosomes from progenitor cells derived from the BM are delivered again to ischemic or injured tissues to allow their repair and regeneration [78].
Interestingly, under ischemic conditions, MSC-derived exosomes are loaded with elevated miRNA-22 levels in the injured cardiomyocytes to prevent apoptosis by targeting Mecp2 [79]. These exosomes also preserve ATP levels, reduce oxidative stress in addition to the induction of phosphatidylinositol 3-kinase/protein kinase B (Akt) signaling, and thus enhance the viability of the myocardium and prevent adverse outcomes of remodeling after ischemia/reperfusion injury [80]. Under the influence of miRNA-182, MSC-derived exosomes could also alter the macrophage polarization status from M1 to M2 and thus prevent myocardial ischemia/reperfusion injury [75]. MSC-derived exosomes also enhanced regional blood flow recovery in the injured heart through the promotion of angiogenesis [23] besides the attenuation of the induced inflammatory status [60]. Moreover, human MSC-derived exosomes enhanced cardiac contractility and calcium-handling gene expression in human-engineered cardiac tissue in vitro, highlighting their beneficial effects on cardiac contractility [81].
Exosomes isolated from Akt-overexpressing human UCMSCs have shown improvement of cardiac regeneration and promotion of angiogenesis through the activation of platelet-derived growth factor D [82]. Furthermore, the ability of exosomes obtained from mouse BM-MSCs to repair infarcted myocardium was enhanced after exposure to hypoxia, which was attributed to miRNA-210 and neutral sphingomyelinase 2 activities [83]. Notably, the combined delivery of exosomes and BM-MSCs in a sequential manner effectively reduced the scar size and restored heart functions after acute MI (AMI) in rats compared with those treated with exosomes or MSCs alone [59]. Therefore, MSC-derived exosomes could be an effective therapy for the management of AMI.
3.3 HF
Mortality and morbidity are still major concerns in patients with HF despite the significant advances in its prevention and therapies [58]. In HF, the heart cannot pump the required blood to meet the body’s needs. Adverse remodeling following MI is one of the important factors that contribute to HF development. Endothelial dysfunction, imbalanced angiogenesis, and inflammation also critically contributed to the progression of HF [84].
Cardiomyocyte-derived exosomes of healthy volunteers significantly promoted the proliferation and reduced the apoptosis of neonatal rat cardiomyocytes in vitro, whereas exosomes from patients with HF produced the opposite outcomes, which may be secondary to decreased exosomal miRNA-21-5p that activates phosphatase and tensin homolog and downregulates Akt phosphorylation in cardiomyocytes [85]. Matsumoto et al. proposed that exosome-derived miRNAs can be used as a prognostic tool for HF in patients with AMI and elevated levels of p53-responsive miRNAs (34a, 192, and 194)18 days after AMI among patients experiencing HF within 1 year [37]. Exosome-associated p53-responsive miRNAs may also predict left ventricular remodeling after AMI [37]. Similarly, compared with healthy volunteers, patients with HF show elevated levels of miRNA-21and miRNA-92 [86] and reduced levels of miRNA-425 and miRNA-744in serum exosomes [87]. Notably, all these miRNAs are usually positively correlated with fibrosis and thus could be used for the diagnosis of hypertrophic heart diseases in addition to being possible targets to prevent their progression to HF [88].
Importantly, a previous study demonstrated that genetic loss of Alix, an important factor for exosome biogenesis, markedly diminished the in vivo production of exosomes by MSCs, affecting their therapeutic outcomes in a HF model and implicating their importance in mediating actions of MSCs [63]. On the contrary, some factors such as adiponectin were found to stimulate biogenesis and secretion of exosomes by MSCs, thereby enhancing their therapeutic efficacy in HF [63]. Ju et al. also reported that cardiac MSC-derived exosomes improved cardiac functions by enhancing capillary density and cardiomyocyte proliferation in a mouse AMI model [89]. Through their enhanced antifibrotic activity, MSCs overexpressing adrenomedullin can further enhance heart functions in rats with HF [90]. Moreover, exosomes secreted by human embryonic stem cell-derived cardiovascular progenitors demonstrated comparable cardioprotective potential to their parent cells in an experimental model of post-infarction HF [91].
3.4 Peripheral arterial diseases (PADs)
PADs are diseases affecting peripheral arteries and thus blood flow to the limbs [92]. This may cause claudication symptoms and affect patients’ quality of life [93]. PAD is likely to be an indication of atherosclerosis, affects blood flow in arteries, and lessens blood supply to legs and, sometimes, to arms [92]. Recent evidence has indicated the success of stem cell-derived exosome application in the management of PAD by promoting angiogenesis [94, 95].
Exosomes from induced pluripotent stem cells-derived MSCs endorsed angiogenesis after injection into the ischemic limbs of mice [96]. EVs isolated from BM-MSCs were also found to enhance the formation of blood vessels in the ischemic limb in vivo by enriching them with vascular endothelial growth factor (VEGF) protein and miRNA-210-3p that upregulated VEGFR1 and VEGFR2 expressions in endothelial cells [97, 98]. In addition, Du et al. boosted the angiogenic potential of MSC-derived exosomes with a nitric oxide-releasing polymer in hind limb ischemia in a murine model where higher levels of VEGF and miRNA-126 cargo promoted angiogenesis [99]. Furthermore, CD34+ cells release exosomes that transfer miRNA-126-3p into their target cells to downregulate the expression of Sprouty-related EVH1 domain containing 1 and upregulate the genes that promote angiogenesis [100].
3.5 Stroke
As one of the well-known fatal diseases, mortality and long-term disability prevail in ischemic stroke [101]. In ischemic stroke, blood vessel occlusion leads to brain ischemia with subsequent neuronal damage [102]. MSCs have shown great potential in the treatment of ischemic stroke through the release of biomolecules that induce angiogenesis [103], anti-apoptosis [104], and immunomodulation [105]. However, the difficulty to deliver MSCs limits their clinical application in ischemic stroke after intravenous administration because of the large diameters of MSCs (15–40 μm) where they are mostly captured by pulmonary capillaries, in addition topoor survival in inflammatory and hypoxic conditions of ischemic lesions [106]. The limitations of MSC therapy could be overcome by MSC-derived exosomes, as the pulmonary capillaries can permit nanosized exosomes, avoiding their accumulation in the lungs following systemic administration [107].
MSC-derived exosomes have been evaluated as therapies for the management of ischemic stroke [66, 108] where MSC-derived exosomes reveal more or less similar outcomes to those of MSCs. In an experimental model of transient middle cerebral artery occlusion, intravenous administration of MSC-derived exosomes stimulated the recovery of neuronal function through the induction of neurogenesis and neurite outgrowth and remodeling[44]. Other studies have revealed that MSC-derived exosomes exhibit nearly similar angiogenic, immunomodulatory, and neuroprotective potentials to MSCs [109, 110]. Interestingly, the efficacy of exosomes was enhanced by the glucose and oxygen deprivation of their treated MSCs, which could be related to the upregulation of some functional proteins in the derived exosomes [111, 112]. Excitingly, MSC-derived exosomes enhanced motor function recovery in a stroke model in primates [113]. These derived exosomes not only act by reducing neuroinflammation and shifting of the microglia into restorative functions [114], but by hampering injury-related hyperexcitability and restoring excitatory–inhibitory balance [115].
3.6 PH
PH is a complicated pathological condition that is associated with the remodeling of pulmonary vessels, hypertrophy of the right ventricle, and subsequently its failure [116, 117]. No fully effective therapies are available for the management of vascular remodeling in PH. Exosomes isolated experimentally from monocrotaline-treated mice or clinically from patients with idiopathic pulmonary arterial hypertension showed upregulated levels of some miRNAs, such as miRNA-19b, miRNA-20a, miRNA-20b, and miRNA-145. On the contrary, MSC-derived exosomes were enriched with antiproliferative and anti-inflammatory miRNAs, namely, miRNA-34a, miRNA-122, miRNA-124, and miRNA-127. These assessments highlight the significant role of miRNAs in the prognosis or prevention of this disease [39]. Interestingly, the administration of exosomes from the conditioned media of BM-MSCs was demonstrated to reverse hypoxia-induced pulmonary fibrosis, leading to the full improvement of PH and right ventricular hypertrophy, whereas exosome-depleted media did not affect hypoxia-induced PH [68, 118]. Additionally, repeated administrations of MSC-derived exosomes were more effective than single administration in the reversal of semaxinib/hypoxia-induced PH in a rat model [119].
Several studies have shown that intravenous delivery of MSC-derived exosomes can inhibit PH vascular remodeling in different ways [39, 68, 119]. MSC-derived exosomes could alleviate PH through the reversal of pulmonary vascular remodeling and inhibition of its associated hyperproliferative pathways, including signal transducer and activator of transcription 3 (STAT3)-mediated signaling [68]. MSC-derived exosomes could also inhibit the proliferation of pulmonary arterial smooth muscle cells and apoptosis of hypoxia-induced pulmonary arterial endothelial cells through the upregulation of the expression of wnt5a and regulation of the RhoA and GSK3β/β-catenin signaling pathway [67]. MSC-derived exosomes attenuated PH in an experimental model of bronchopulmonary dysplasia through VEGF signaling with increased expression of VEGF/VEGFR2 [71]. Furthermore, MSC-derived exosomes may be enriched with protective miRNAs such as miRNA-483 [120] and miR-21-5p [121]. The overexpression of miR-483 in endothelial cells inhibits inflammatory and fibrogenic responses and leads to ameliorated PH phenotypes in rats [120]. MSC-derived exosomes alleviate ischemia/reperfusion injury in mouse lung by transporting anti-apoptotic miR-21-5p [121]. Importantly, intravenous administration of MSC-derived exosomes was found to upregulate miRNA-204 expression in the lungs, with the attenuation of the increased right ventricular systolic pressure in an experimental model of hypoxia-induced PH [68].
4 Enhancement of the therapeutic effects of MSC-derived exosomes
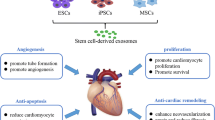
MSC-derived exosomes have been revealed as future candidates for cell-free therapy that could be used in the management of various diseases. However, a major challenge of their clinical application includes the maintenance of their efficacy and stability over time after their systemic transplantation [122]. As the characteristics of exosomes vary depending on the status of MSCs from which they are derived, exposure of MSCs to different external stimuli such as preconditioning with cytokines, hypoxia, and chemicals has enhanced the immunomodulatory and regenerative effects of their derived exosomes [123]. Moreover, genetic and cell surface modification of MSC-derived exosomes can modulate their therapeutic efficacy [124]. Different mechanisms could be used to improve functions of MSC-derived exosomes (Fig. 2).
4.1 Preconditioning strategies
4.1.1 Increasing exosome production using different culture conditions
Although MSC-derived exosomes represent a promising candidate for cardiac regeneration and repair, their low level of production from routine culture conditions limits their therapeutic efficacy. Alterations of the characteristics of MSC-derived exosomes and their components are caused by the use of different culture conditions. For example, the culture of MSCs with the serum from the blood of mice with middle cerebral artery occlusion afforded more neuroprotection than that obtained from culture of MSCs with normal serum due to the remarkably upregulated expression of miRNA-20a in the released exosomes [125].
Importantly, exosomes from different microenvironments may have a focus on a specified cell type. For instance, neuron-derived EVs preferentially target cells in the nervous system [126]. However, further evaluation is needed to determine whether co-culturing of MSCs with the required cell type (e.g.,cardiomyocytes) can improve the efficacy of the released exosomes to target the same cell type. The production of MSC-derived exosomes could be also increased using 3D culture techniques. For example, the use of a 3D porous scaffold structure instead of 2D surfaces in plastic plates enhances the production MSC-derived exosomes and their therapeutic efficacy [127]. Microcarriers and bioreactors could be used for MSC expansions on large scale and thus increasing the amounts of their released exosomes [128]. Additionally, the use of osmotic stress such as vesiculation buffers containing chloride salts can enhance the production of EVs from targeted cells [129]. The usage of 1- to 2-μm pore polymer filters was found to improve the production of exosomes by extruding cells [130]. Furthermore, the amount of EVs produced can be enhanced by their treatment with cytochalasin B [131]. Similarly, MSC-derived exosomes treated with cytochalasin B have the same angiogenic potential to their parent MSCs [132].
4.1.2 Hypoxic preconditioning of MSCs
Hypoxic or ischemic preconditioning is a widely accepted approach for priming MSCs and MSC-derived exosomes. Several studies have demonstrated that exosomes from hypoxia-primed MSCs promote higher angiogenic potential relative to exosomes from MSCs cultured undernormoxic conditions [133, 134]. Salomon et al. reported that exosomes from hypoxia-primed placental MSCs increased the migration and angiogenic tube formation of placental microvascular endothelial cells [135]. In addition, hypoxia-primed MSCs produced exosomes that attenuated inflammation and elevated fat survival after grafting [136] with upregulated levels of angiopoietin-1, epidermal growth factor (EGF), and fibroblast growth factor proteins [134]. Vesicles produced by hypoxia-conditioned MSCs also induced protein kinase A signaling, vascular endothelial growth factor expression, and thus their angiogenic potential in vitro [137].
MSCs are enriched with miRNAs, which may promote cardiomyocyte survival during hypoxia [138]. Ischemic preconditioning induces BM-MSC survival by upregulating miRNA-210 expression, which targets caspase-8-associated protein [139]. Hypoxic preconditioning of BM-MSC exosomes could also inhibit cardiomyocyte apoptosis after AMI by upregulating miRNA-24 [140]. In addition, exosomes with overexpressed hypoxia-inducible factor 1-alpha were associated with elevated levels of proangiogenic factors that promoted neovessel development and prevented fibrosis in a rat model of MI [141]. The actions of exosomes from hypoxia-primed MSCs could be related to the transferred miRNA-210, which improves the angiogenic and anti-apoptotic functions of HUVECs, resulting in enhanced vascularization and survival rate [142]. These preconditioned exosomes also directly suppress GSK3β expression through miRNA-26a, resulting in the observed cardioprotective effects after MI [143].
4.1.3 Pharmacological preconditioning of MSCs
Preconditioning of MSCs with pharmacological agents may be considered an effective approach to enhance their efficacy. All these preconditioning techniques prevented apoptosis of transplanted MSCs in vivo and led to the improvement of their function [144, 145]. In general, these effects could be due to their enhanced angiogenic and antifibrotic potential. Preconditioning with several pharmacological agents [144,145,146] revealed a link between the enhanced effects and the increased levels of VEGF, fibroblast growth factor-2, or HGF and Akt signaling pathway activation. After their preconditioning with Buyang Huanwu decoction, MSC-derived EVs were demonstrated to increase VEGF levels and thus prevent brain injury in a rat model of cerebral ischemia [147]. Atorvastatin was found to enhance the immunomodulatory potential of MSCs by preventing inflammatory cell infiltration and thus the levels of pro-inflammatory cytokines via a C-X-C chemokine receptor type 4 (CXCR-4)-dependent mechanism. These effects would reduce the infarct size and improve functional recovery in a rat model of stroke [148]. Thus, paracrine actions of MSCs and their therapeutic outcomes are affected by their surrounding microenvironment even with minor changes in the culture conditions or changes associated with injured tissue microenviroment [149], and this would ultimately affect the actions of their derived exosomes.
4.1.4 Biomolecular or chemical preconditioning of MSCs
Biomolecules such as growth factors or others (i.e., angiotensin-II, EGF, glial cell line-derived neurotrophic factor, IGF-1, and stromal-derived factor 1 (SDF-1) and tumor necrosis factor α) were revealed to enhance the paracrine functions of MSCs and their regenerative capacity. Preconditioning of MSCs with interferon-gamma (IFN-γ) stimulates the IFN-primed MSCs to produce exosomes that are enriched with anti-inflammatory proteins, neuroprotective proteins, and anti-inflammatory RNAs [132, 150, 151].
Other biomolecules have been evaluated as preconditioning agents where exosomes derived from thrombin-primed MSCs revealed the improvement of proliferation, migration, and tube formation by HUVECs in vitro and in severe neonatal ischemic encephalopathy in vivo [152]. Interestingly, preconditioning of MSCs with traditional Chinese medicine that is used in the management of acute coronary syndrome improved the function of derived exosomes through the downregulation of the expression of the H3K27 demethylase UTX and hence the enhancement of cardiomyocyte proliferation [153]. Exosomes from NO-preconditioned MSCs also increasedthe levels of VEGF and miRNA-126, which could be proposed as a novel mechanism contributing to the increased angiogenic capacity of these exosomes [99]. In addition, chitosan hydrogel could enhance the retention and stability of exosomes and augment their therapeutic and angiogenic effects in a model of hind limb ischemia [122].
4.2 Genetically modified MSC-derived exosomes
The use of genetically modified MSCs is another approach to enhance the efficacy of exosomes by the knockdown or overexpression of certain RNAs. For instance, transfecting MSCs with a recombinant adenovirus with the Akt gene would upregulate the levels of platelet-derived growth factor D (PDGF-D) produced in their derived exosomes [82] and thus enhance their angiogenic, regenerative, and reparative potential.
Exosomes from GATA-4-overexpressing MSCs were demonstrated to improve cardiac function by decreasing apoptosis and increasing the number of newly formed blood vessels in a mouse model of MI [154]. MSCs with overexpressed GATA-4 are enriched with anti-apoptotic miRNA-19a, which induces the extracellular signal-regulated kinase (ERK) and Akt signaling pathways [138]. Likewise, MSCs with overexpressed CXCR4 were shown to release exosomes with enhanced tube formation by HUVECs and significant cardioprotective effects through the activation of Akt signaling in a rat model of MI [155]. In another study, MSCs overexpressing Akt released exosomes with enhanced angiogenic functions in vitro and improved regenerative potential in vivo by activating PDGF-D in a rat model of acute MI [82]. Exosomes derived from MSCs with overexpressed indoleamine 2,3-dioxygenase were found to increase the Tregs/CD8 + T-cell ratio and hence inhibited the production of pro-inflammatory cytokines and enhanced the immune tolerance in a rat model of cardiac allografts [156]. Furthermore, exosomes derived from MSCs with overexpressed SDF-1were shown to enhance cardiac repair through the inhibition of apoptosis and promotion of endothelial microvessel regeneration in a mouse model of MI [157].
Similarly, the overexpression of miRNAs in MSCs can enhance the efficacy of exosomes. MSCs overexpressing miRNA-133 produced exosomes that decreased inflammation and fibrosis in a rat model of AMI [158]. MSCs with overexpressed miRNA-146 and miRNA-93-5p also released exosomes that inhibited myocardial damage in a rat model of MI. These exosomes also inhibited in vitro the inflammatory cytokine expression and autophagy in hypoxic H9c2 cells [159]. Similarly, MSCs with overexpressed miRNA-126 released exosomes that promoted microvascular generation and suppressed the expression of hypoxia-induced inflammation factors in vitro in addition to the inhibition of cardiac inflammation and fibrosis in vivo [160]. Thus, genetically modified MSC-derived exosomes could be an effective way to enhance their efficacy in regenerative medicine.
5 Use of exosomes as targeted drug delivery systems
Exosomes exhibit unique characteristics that make them an ideal vehicle for drug delivery. Their existence in all biological fluids increases their tolerance in the body when used as drug delivery vehicles [161]. Exosomes could be also loaded with specific drugs or biomolecules for the development of specific therapeutic outcomes. Therapeutic loading of exosomes could be performed with the required agents before or after being isolated from biological fluids [162]. Pasucci et al. revealed that paclitaxel (PTX)-loaded MSC-derived exosomes isolated after the incubation of PTX with MSCs exhibited anti-tumor activity [163]. Another feature that supports the use of exosomes as vehicles for drug delivery includes their ability to cross the blood–brain barrier [164] and produce their therapeutic effect [165, 166]. The intravenous administration of exosomes conjugated with RGDyK can target the ischemic lesion in a model of middle cerebral artery occlusion in mice. Furthermore, the loading of these exosomes with curcumin suppressed inflammation and apoptosis in the ischemic region [66]. All these factors make exosomes an ideal vehicle for drug delivery in various diseases including CVDs.
Importantly, the systemic administration of exogenous exosomes for therapeutic purposes is technically challenging and subjected to macrophage-mediated phagocytosis in the liver where the vast majority of exosomes accumulate, leading to the rapid decrease in their circulation levels after intravenous administration [167,168,169]. This implies the need to generate higher doses of exosomes to meet the clinical requirements, which is usually limited by the number of cellular sources available for secreting sufficient amounts of exosomes [170].
Modifying the surface of exosomes using different pre-and post-isolation methods could be useful to control their pharmacokinetics by elevating their circulating half-life, increasing their bioavailability to target tissues, and improving their therapeutic efficacy [170]. For example, coating their surface using PEGylation method prevents them from being aggregated or subjected to phagocytosis, prolonging their half-life and enhancing their blood circulation time sixfold in comparison to unmodified exosomes [170, 171]. Several labeling methods such as bioluminescence emitted from luciferase could be used to evaluate the pharmacokinetics of exosomes and their biodistribution [172]. However, all structural modifications of exosomes should be tested for their safety and efficacy in well-designed in vivo models.
Recent evidence showed that, unlike other vectors that have been used for gene delivery, exosomes could be used to carry different contents including miRNAs to adjacent or distant targeted cells [173, 174] to mediate the crosstalk among cell types and provide reliable way to overcome the inefficient and nonspecific delivery [175, 176]. The challenge is how to effectively load these exosomes with required biomaterials without affecting their structure or ability to interact with target cells. Electroporation is a commonly applied technique that has been used to add anti-inflammatory compounds to exosomes from macrophages with a loading efficacy of approximately 20% and was successfully evaluated by reducing inflammation in acute peritonitis and atherosclerosis development [177]. Transfection techniques also have been used to load exosomes with the desired cargo, such as miRNAsor proteins. Recent findings have revealed that exosomes loaded with syndecan-1 ameliorated pulmonary edema through the reduction of pro-inflammatory cytokines (IL-1β, tumor necrosis factor-α, and IL-6) [178]. Additionally, exosomes loaded with miR-21-5p, a miRNA that is downregulated in HF, exhibited good regenerative potential in MI unlike that derived from cardiac stromal cells in patients with HF [85]. Therefore, exosomes could be used as potential vectors of required biomolecules, which could fundamentally change the current therapeutic management of CVDs in the future.
6 Limitations and future challenges
The use of stem cell-derived exosomes has many advantages compared with the transplantation of parent stem cells, where the induction of IFN-γ can increase the risk of immune rejection following the MSC transplantation [179]. On the contrary, the derived exosomes revealed low immunogenicity and negligible risk of tumor development [180]. MSC-derived exosomes are more easy and stable to store than MSCs [57] in addition to their relatively lower cost production [181]. Exosomes show no obvious adverse reactions, such as fever and allergic or hemolytic reactions [182]. Additionally, exosomes can produce stronger therapeutic effects, as they can cross capillaries without plugging because they are much smaller than their parent cells [183]. Repeated administrations of BM-MSC-derived exosomes did not show any harmful immune reactions or toxicity in mice as evaluated by immunotyping of various tissues and histological examinations [128, 184]. Thus, exosomes could be more efficacious than their parent cells after systemic administration by the recapitulation of the beneficial effects of their parent cells and overcoming their limitations [52].
Despite these significant advantages, the application of exosomes has several limitations [24] including inconvenient and time-wasting procedure used for extraction using the classic high-speed centrifugation in addition to the limitation of the amount of exosomes produced. Besides, several harmful and unwanted components could be present in the exosomes, which should be modified and removed. Furthermore, only few exosomes reach the target area after systemic administration, which could greatly restrict their efficiency [168]. Thus, several challenges should be addressed to harness the full therapeutic potential of exosomes.
Several considerations should be evaluated before the clinical applications of exosomes. First, more accurate isolation methods should be adopted other than that based on their size, as different vesicle sizes may reflect only different components in the isolated exosomes. For example, their isolation may depend on the epitopes expressed by the donor cell. Additionally, MSC-derived exosomes may be contaminated by exosomes of various cell types, as they are usually isolated from blood or culture media. Thus, extracting the exosomes from multivesicular endosomes before being released may help get purified exosomes and overcome the problem of contamination. It is also important to understand the mechanism of exosome dynamic secretion and their uptake at the tissue level in addition to the establishment of a well-defined method for single-exosome analysis rather than the whole-exosome population. Finally, recent evidence demonstrates that MSC-derived exosomes may exhibit different therapeutic outcomes according to the variations of their components in different microenvironments. For instance, MSCs may release exosomes that exhibit immunomodulatory actions after MI in the pro-inflammatory phase and then exosomes that exert pro-angiogenic actions in the reparative and regenerative phases [52]. Taken together, continuous attempts are required to understand the exact mechanisms of the therapeutic actions of exosomes and hence the possibility of their modification or enhancement. More studies are also needed to evaluate the best route of administration of exosomes, their optimal dose, and their pharmacokinetics and biodistribution inside the body. Importantly, the engineered exosomes should be tested for their efficacy, immunogenicity, and safety in general [183,184,185].
7 Conclusion
CVDs are a major cause of death worldwide; thus, continuous efforts have beenmade to search for novel therapeutic strategies to trigger the repair and regeneration of injured tissues. In experimental studies, exosomes have emerged over the past decade as an alternative to cell-based therapy in various CVDs with promising and beneficial outcomes concerning neovascular, anti-apoptotic, anti-remodeling, and anti-inflammatory actions. Exosomes could be used both as biomarkers or mediators of various diseases in addition to their management by targeting injured areas with specific peptides or miRNAs or other factors. Despite continuous efforts to enhance the isolation and production yield of MSC-derived exosomes and efficacy and stability over time after in vivo transplantation, more investigations and approaches are required to overcome the limitations of their use before their clinical application.
References
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage potential of adult human mesenchymal stem cells. Science. 1999;284:143–7.
Caplan AI. Mesenchymal stem cells. J Orthop Res. 1991;9:641–50.
Orlic D, Kajstura J, Chimenti S, Jakoniuk I, Anderson SM, Li B, et al. Bone marrow cells regenerate infarcted myocardium. Nature. 2001;410:701–5.
Berry MF, Engler AJ, Woo YJ, Pirolli TJ, Bish LT, Jayasankar V, et al. Mesenchymal stem cell injection after myocardial infarction improves myocardial compliance. Am J Physiol Heart Circ Physiol. 2006;290:H2196–203.
Li L, Zhang S, Zhang Y, Yu B, Xu Y, Guan Z. Paracrine action mediate the antifibrotic effect of transplanted mesenchymal stem cells in a rat model of global heart failure. Mol Biol Rep. 2009;36:725–31.
Katsuda T, Kosaka N, Takeshita F, Ochiya T. The therapeutic potential of mesenchymal stem cell-derived extracellular vesicles. Proteomics. 2013;13:1637–53.
Caplan AI, Dennis JE. Mesenchymal stem cells as trophic mediators. J Cell Biochem. 2006;98:1076–84.
Timmers L, Lim SK, Arslan F, Armstrong JS, Hoefer IE, Doevendans PA, et al. Reduction of myocardial infarct size by human mesenchymal stem cell conditioned medium. Stem Cell Res. 2008;1:129–37.
Lai RC, Arslan F, Lee MM, Sze NS, Choo A, Chen TS, et al. Exosome secreted by MSC reduces myocardial ischemia/reperfusion injury. Stem Cell Res. 2010;4:214–22.
Burrello J, Monticone S, Gai C, Gomez Y, Kholia S, Camussi G. Stem cell-derived extracellular vesicles and immune-modulation. Front Cell Dev Biol. 2016;4:83.
Lai RC, Tan SS, Teh BJ, Sze SK, Arslan F, De Kleijn DP, et al. Proteolytic potential of the MSC exosome proteome: implications for an exosome-mediated delivery of therapeutic proteasome. Int J Proteomics. 2012;2012:971907.
Luo Y, Wang Y, Poynter JA, Manukyan MC, Herrmann JL, Abarbanell AM, et al. Pretreating mesenchymal stem cells with interleukin-1β and transforming growth factor-β synergistically increases vascular endothelial growth factor production and improves mesenchymal stem cell–mediated myocardial protection after acute ischemia. Surgery. 2012;151:353–63.
Hoang DH, Nguyen TD, Nguyen HP, Nguyen XH, Do PTX, Dang VD, et al. Differential wound healing capacity of mesenchymal stem cell-derived exosomes originated from bone marrow, adipose tissue and umbilical cord under serum-and xeno-free condition. Front Mol Biosci. 2020;7:119.
Deng H, Sun C, Sun Y, Li H, Yang L, Wu D, et al. Lipid, protein, and microRNA composition within mesenchymal stem cell-derived exosomes. Cell Reprogram. 2018;20:178–86.
Tomasoni S, Longaretti L, Rota C, Morigi M, Conti S, Gotti E, et al. Transfer of growth factor receptor mRNA via exosomes unravels the regenerative effect of mesenchymal stem cells. Stem Cells Dev. 2013;22:772–80.
Shao L, Zhang Y, Lan B, Wang J, Zhang Z, Zhang L, et al. MiRNA-sequence indicates that mesenchymal stem cells and exosomes have similar mechanism to enhance cardiac repair. Biomed Res Int. 2017;2017:4150705.
Xin H, Li Y, Buller B, Katakowski M, Zhang Y, Wang X, et al. Exosome-mediated transfer of miR-133b from multipotent mesenchymal stromal cells to neural cells contributes to neurite outgrowth. Stem Cells. 2012;30:1556–64.
Wei W, Ao Q, Wang X, Cao Y, Liu Y, Zheng SG, et al. Mesenchymal stem cell-derived exosomes: a promising biological tool in nanomedicine. Front Pharmacol. 2021;11:1954.
Khan M, Nickoloff E, Abramova T, Johnson J, Verma SK, Krishnamurthy P, et al. Embryonic stem cell–derived exosomes promote endogenous repair mechanisms and enhance cardiac function following myocardial infarction. Circ Res. 2015;117:52–64.
Rosca AM, Moustafa Abou Rayia D, Tutuianu R. Emerging role of stem cells-derived exosomes as valuable tools for cardiovascular therapy. Curr Stem Cell Res Ther. 2017;12:134–8.
Zhang Z, Yang J, Yan W, Li Y, Shen Z, Asahara T. Pretreatment of cardiac stem cells with exosomes derived from mesenchymal stem cells enhances myocardial repair. J Am Heart Assoc. 2016;5:e002856.
Cervio E, Barile L, Moccetti T, Vassalli G. Exosomes for intramyocardial intercellular communication. Stem Cells Int. 2015;2015:482171.
Bian S, Zhang L, Duan L, Wang X, Min Y, Yu H. Extracellular vesicles derived from human bone marrow mesenchymal stem cells promote angiogenesis in a rat myocardial infarction model. J Mol Med. 2014;92:387–97.
Wiklander OP, Nordin JZ, O’Loughlin A, Gustafsson Y, Corso G, Mäger I, et al. Extracellular vesicle in vivo biodistribution is determined by cell source, route of administration and targeting. J Extracell Vesicles. 2015;4:26316.
Lee BC, Kang KS. Functional enhancement strategies for immunomodulation of mesenchymal stem cells and their therapeutic application. Stem Cell Res Ther. 2020;11:397.
Bach F, Albertini R, Joo P, Anderson J, Bortin M. Bone-marrow transplantation in a patient with the Wiskott-Aldrich syndrome. Lancet. 1968;2:1364–6.
Dimmeler S, Burchfield J, Zeiher AM. Cell-based therapy of myocardial infarction. Arterioscler Thromb Vasc Biol. 2008;28:208–16.
du Pré BC, Doevendans PA, van Laake LW. Stem cells for cardiac repair: an introduction. J Geriatr Cardiol. 2013;10:186.
Yu H, Lu K, Zhu J, Wang J. Stem cell therapy for ischemic heart diseases. Br Med Bull. 2017;121:135–54.
Sanganalmath SK, Bolli R. Cell therapy for heart failure: a comprehensive overview of experimental and clinical studies, current challenges, and future directions. Circ Res. 2013;113:810–34.
Gu E, Chen W-Y, Gu J, Burridge P, Wu JC. Molecular imaging of stem cells: tracking survival, biodistribution, tumorigenicity, and immunogenicity. Theranostics. 2012;2:335–45.
Gnecchi M, Zhang Z, Ni A, Dzau VJ. Paracrine mechanisms in adult stem cell signaling and therapy. Circ Res. 2008;103:1204–19.
Corrado C, Raimondo S, Chiesi A, Ciccia F, De Leo G, Alessandro R. Exosomes as intercellular signaling organelles involved in health and disease: basic science and clinical applications. Int J Mol Sci. 2013;14:5338–66.
Yang D, Zhang W, Zhang H, Zhang F, Chen L, Ma L, et al. Progress, opportunity, and perspective on exosome isolation-efforts for efficient exosome-based theranostics. Theranostics. 2020;10:3684–707.
Li P, Kaslan M, Lee SH, Yao J, Gao Z. Progress in exosome isolation techniques. Theranostics. 2017;7:789–804.
Kim JY, Rhim WK, Yoo YI, Kim DS, Ko KW, Heo Y, et al. Defined MSC exosome with high yield and purity to improve regenerative activity. J Tissue Eng. 2021;12:20417314211008624.
Matsumoto S, Sakata Y, Suna S, Nakatani D, Usami M, Hara M, et al. Circulating p53-responsive microRNAs are predictive indicators of heart failure after acute myocardial infarction. Circ Res. 2013;113:322–6.
Ji Q, Ji Y, Peng J, Zhou X, Chen X, Zhao H, et al. Increased brain-specific MiR-9 and MiR-124 in the serum exosomes of acute ischemic stroke patients. PLoS One. 2016;11:e0163645.
Aliotta JM, Pereira M, Wen S, Dooner MS, Del Tatto M, Papa E, et al. Exosomes induce and reverse monocrotaline-induced pulmonary hypertension in mice. Cardiovasc Res. 2016;110:319–30.
Lawson C, Vicencio JM, Yellon DM, Davidson SM. Microvesicles and exosomes: new players in metabolic and cardiovascular disease. J Endocrinol. 2016;228:R57–71.
Théry C, Ostrowski M, Segura E. Membrane vesicles as conveyors of immune responses. Nat Rev Immunol. 2009;9:581–93.
de Jong OG, Verhaar MC, Chen Y, Vader P, Gremmels H, Posthuma G, et al. Cellular stress conditions are reflected in the protein and RNA content of endothelial cell-derived exosomes. J Extracell Vesicles. 2012;1:18396.
Corrado C, Raimondo S, Saieva L, Flugy AM, De Leo G, Alessandro R. Exosome-mediated crosstalk between chronic myelogenous leukemia cells and human bone marrow stromal cells triggers an interleukin 8-dependent survival of leukemia cells. Cancer Lett. 2014;348:71–6.
Xin H, Li Y, Cui Y, Yang JJ, Zhang ZG, Chopp M. Systemic administration of exosomes released from mesenchymal stromal cells promote functional recovery and neurovascular plasticity after stroke in rats. J Cereb Blood Flow Metab. 2013;33:1711–5.
Joo HS, Suh JH, Lee HJ, Bang ES, Lee JM. Current knowledge and future perspectives on mesenchymal stem cell-derived exosomes as a new therapeutic agent. Int J Mol Sci. 2020;21:727.
de Abreu RC, Fernandes H, da Costa Martins PA, Sahoo S, Emanueli C, Ferreira L. Native and bioengineered extracellular vesicles for cardiovascular therapeutics. Nat Rev Cardiol. 2020;17:685–97.
Wang Y, Zhang L, Li Y, Chen L, Wang X, Guo W, et al. Exosomes/microvesicles from induced pluripotent stem cells deliver cardioprotective miRNAs and prevent cardiomyocyte apoptosis in the ischemic myocardium. Int J Cardiol. 2015;192:61–9.
Ribeiro-Rodrigues TM, Laundos TL, Pereira-Carvalho R, Batista-Almeida D, Pereira R, Coelho-Santos V, et al. Exosomes secreted by cardiomyocytes subjected to ischaemia promote cardiac angiogenesis. Cardiovasc Res. 2017;113:1338–50.
Gollmann-Tepeköylü C, Pölzl L, Graber M, Hirsch J, Nägele F, Lobenwein D, et al. miR-19a-3p containing exosomes improve function of ischaemic myocardium upon shock wave therapy. Cardiovasc Res. 2020;116:1226–36.
Minghua W, Zhijian G, Chahua H, Qiang L, Minxuan X, Weifang Z, et al. Plasma exosomes induced by remote ischaemic preconditioning attenuate myocardial ischaemia/reperfusion injury by transferring miR-24. Cell Death Dis. 2018;9:320.
Nasser MI, Masood M, Adlat S, Gang D, Zhu S, Li G, et al. Mesenchymal stem cell-derived exosome microRNA as therapy for cardiac ischemic injury. Biomed Pharmacother. 2021;143:112118.
Sun SJ, Wei R, Li F, Liao SY, Tse HF. Mesenchymal stromal cell-derived exosomes in cardiac regeneration and repair. Stem Cell Reports. 2021;16:1662–73.
Haider KH, Aramini B. Mircrining the injured heart with stem cell-derived exosomes: an emerging strategy of cell-free therapy. Stem Cell Res Ther. 2020;11:23.
Adamiak M, Sahoo S. Exosomes in myocardial repair: advances and challenges in the development of next-generation therapeutics. Mol Ther. 2018;26:1635–43.
Yang W, Yin R, Zhu X, Yang S, Wang J, Zhou Z, et al. Mesenchymal stem-cell-derived exosomal miR-145 inhibits atherosclerosis by targeting JAM-A. Mol Ther Nucleic Acids. 2021;23:119–31.
Li J, Xue H, Li T, Chu X, Xin D, Xiong Y, et al. Exosomes derived from mesenchymal stem cells attenuate the progression of atherosclerosis in ApoE−/-mice via miR-let7 mediated infiltration and polarization of M2 macrophage. Biochem Biophys Res Commun. 2019;510:565–72.
Ma J, Chen L, Zhu X, Li Q, Hu L, Li H. Mesenchymal stem cell-derived exosomal miR-21a-5p promotes M2 macrophage polarization and reduces macrophage infiltration to attenuate atherosclerosis. Acta Biochim Biophys Sin. 2021;53:1227–36.
Zou L, Ma X, Lin S, Wu B, Chen Y, Peng C. Bone marrow mesenchymal stem cell-derived exosomes protect against myocardial infarction by promoting autophagy. Exp Ther Med. 2019;18:2574–82.
Huang P, Wang L, Li Q, Xu J, Xu J, Xiong Y, et al. Combinatorial treatment of acute myocardial infarction using stem cells and their derived exosomes resulted in improved heart performance. Stem Cell Res Ther. 2019;10:300.
Teng X, Chen L, Chen W, Yang J, Yang Z, Shen Z. Mesenchymal stem cell-derived exosomes improve the microenvironment of infarcted myocardium contributing to angiogenesis and anti-inflammation. Cell Physiol Biochem. 2015;37:2415–24.
Huang P, Wang L, Li Q, Tian X, Xu J, Xu J, et al. Atorvastatin enhances the therapeutic efficacy of mesenchymal stem cells-derived exosomes in acute myocardial infarction via up-regulating long non-coding RNA H19. Cardiovasc Res. 2020;116:353–67.
Peng Y, Zhao JL, Peng ZY, Xu WF, Yu GL. Exosomal miR-25-3p from mesenchymal stem cells alleviates myocardial infarction by targeting pro-apoptotic proteins and EZH2. Cell Death Dis. 2020;11:317.
Nakamura Y, Kita S, Tanaka Y, Fukuda S, Obata Y, Okita T, et al. Adiponectin stimulates exosome release to enhance mesenchymal stem-cell-driven therapy of heart failure in mice. Mol Ther. 2020;28:2203–19.
Gong M, Yu B, Wang J, Wang Y, Liu M, Paul C, et al. Mesenchymal stem cells release exosomes that transfer miRNAs to endothelial cells and promote angiogenesis. Oncotarget. 2017;8:45200–12.
Xue C, Shen Y, Li X, Li B, Zhao S, Gu J, et al. Exosomes derived from hypoxia-treated human adipose mesenchymal stem cells enhance angiogenesis through the PKA signaling pathway. Stem Cells Dev. 2018;27:456–65.
Tian T, Zhang HX, He CP, Fan S, Zhu YL, Qi C, et al. Surface functionalized exosomes as targeted drug delivery vehicles for cerebral ischemia therapy. Biomaterials. 2018;150:137–49.
Zhang S, Liu X, Ge LL, Li K, Sun Y, Wang F, et al. Mesenchymal stromal cell-derived exosomes improve pulmonary hypertension through inhibition of pulmonary vascular remodeling. Respir Res. 2020;21:71.
Lee C, Mitsialis SA, Aslam M, Vitali SH, Vergadi E, Konstantinou G, et al. Exosomes mediate the cytoprotective action of mesenchymal stromal cells on hypoxia-induced pulmonary hypertension. Circulation. 2012;126:2601–11.
Willis GR, Fernandez-Gonzalez A, Anastas J, Vitali SH, Liu X, Ericsson M, et al. Mesenchymal stromal cell exosomes ameliorate experimental bronchopulmonary dysplasia and restore lung function through macrophage immunomodulation. Am J Respir Crit Care Med. 2018;197:104–16.
Ge L, Jiang W, Zhang S, Wang J, Xin Q, Sun C, et al. Mesenchymal stromal cell-derived exosomes attenuate experimental pulmonary arterial hypertension. Curr Pharm Biotechnol. 2021;22:1654–62.
Braun RK, Chetty C, Balasubramaniam V, Centanni R, Haraldsdottir K, Hematti P, et al. Intraperitoneal injection of MSC-derived exosomes prevent experimental bronchopulmonary dysplasia. Biochem Biophys Res Commun. 2018;503:2653–8.
Zheng B, Yin WN, Suzuki T, Zhang XH, Zhang Y, Song Ll, et al. Exosome-mediated miR-155 transfer from smooth muscle cells to endothelial cells induces endothelial injury and promotes atherosclerosis. Mol Ther. 2017;25:1279–94.
Liu J, Wu J, Li L, Li T, Wang J. The role of exosomal non-coding RNAs in coronary artery disease. Front Pharmacol. 2020;11:603104.
Lin Y, Zhu W, Chen X. The involving progress of MSCs based therapy in atherosclerosis. Stem Cell Res Ther. 2020;11:216.
Zhao J, Li X, Hu J, Chen F, Qiao S, Sun X, et al. Mesenchymal stromal cell-derived exosomes attenuate myocardial ischaemia-reperfusion injury through miR-182-regulated macrophage polarization. Cardiovasc Res. 2019;115:1205–16.
Feld S, Kjellgren O, Smalling RW. Aggressive interventional treatment of acute myocardial infarction. Cardiology. 1995;86:365–73.
Huang F, Li ML, Fang ZF, Hu XQ, Liu QM, Liu ZJ, et al. Overexpression of MicroRNA-1 improves the efficacy of mesenchymal stem cell transplantation after myocardial infarction. Cardiology. 2013;125:18–30.
Sahoo S, Losordo DW. Exosomes and cardiac repair after myocardial infarction. Circ Res. 2014;114:333–44.
Feng Y, Huang W, Wani M, Yu X, Ashraf M. Ischemic preconditioning potentiates the protective effect of stem cells through secretion of exosomes by targeting Mecp2 via miR-22. PLoS One. 2014;9:e88685.
Arslan F, Lai RC, Smeets MB, Akeroyd L, Choo A, Aguor EN, et al. Mesenchymal stem cell-derived exosomes increase ATP levels, decrease oxidative stress and activate PI3K/Akt pathway to enhance myocardial viability and prevent adverse remodeling after myocardial ischemia/reperfusion injury. Stem Cell Res. 2013;10:301–12.
Mayourian J, Cashman TJ, Ceholski DK, Johnson BV, Sachs D, Kaji DA, et al. Experimental and computational insight into human mesenchymal stem cell paracrine signaling and heterocellular coupling effects on cardiac contractility and arrhythmogenicity. Circ Res. 2017;121:411–23.
Ma J, Zhao Y, Sun L, Sun X, Zhao X, Sun X, et al. Exosomes derived from AKt-modified human umbilical cord mesenchymal stem cells improve cardiac regeneration and promote angiogenesis via activating platelet-derived growth factor D. Stem Cells Transl Med. 2017;6:51–9.
Zhu J, Lu K, Zhang N, Zhao Y, Ma Q, Shen J, et al. Myocardial reparative functions of exosomes from mesenchymal stem cells are enhanced by hypoxia treatment of the cells via transferring microRNA-210 in an nSMase2-dependent way. Artif Cells Nanomed Biotechnol. 2018;46:1659–70.
Sun HJ, Wu ZY, Nie XW, Bian JS. Role of endothelial dysfunction in cardiovascular diseases: the link between inflammation and hydrogen sulfide. Front Pharmacol. 2020;10:1568.
Qiao L, Hu S, Liu S, Zhang H, Ma H, Huang K, et al. microRNA-21-5p dysregulation in exosomes derived from heart failure patients impairs regenerative potential. J Clin Invest. 2019;129:2237–50.
Goren Y, Kushnir M, Zafrir B, Tabak S, Lewis BS, Amir O. Serum levels of microRNAs in patients with heart failure. Eur J Heart Fail. 2012;14:147–54.
Wang L, Liu J, Xu B, Liu YL, Liu Z. Reduced exosome miR-425 and miR-744 in the plasma represents the progression of fibrosis and heart failure. Kaohsiung J Med Sci. 2018;34:626–33.
Ye W, Tang X, Yang Z, Liu C, Zhang X, Jin J, et al. Plasma-derived exosomes contribute to inflammation via the TLR9-NF-κB pathway in chronic heart failure patients. Mol Immunol. 2017;87:114–21.
Ju C, Shen Y, Ma G, Liu Y, Cai J, Kim IM, et al. Transplantation of cardiac mesenchymal stem cell-derived exosomes promotes repair in ischemic myocardium. J Cardiovasc Transl Res. 2018;11:420–8.
Li LL, Peng C, Zhang M, Liu Y, Li H, Chen H, et al. Mesenchymal stem cells overexpressing adrenomedullin improve heart function through antifibrotic action in rats experiencing heart failure. Mol Med Rep. 2018;17:1437–44.
Kervadec A, Bellamy V, El Harane N, Arakélian L, Vanneaux V, Cacciapuoti I, et al. Cardiovascular progenitor–derived extracellular vesicles recapitulate the beneficial effects of their parent cells in the treatment of chronic heart failure. J Heart Lung Transplant. 2016;35:795–807.
Kullo IJ, Rooke TW. Peripheral artery disease. N Engl J Med. 2016;374:861–71.
Chen JC, Koo M, Hwang JH. Risks of peripheral arterial occlusive disease in patients with obstructive sleep apnoea: a population-based case–control study. Clin Otolaryngol. 2015;40:437–42.
Babaei M, Rezaie J. Application of stem cell-derived exosomes in ischemic diseases: opportunity and limitations. J Transl Med. 2021;19:196.
Li X, Jiang C, Zhao J. Human endothelial progenitor cells-derived exosomes accelerate cutaneous wound healing in diabetic rats by promoting endothelial function. J Diabetes Complicat. 2016;30:986–92.
Hu GW, Li Q, Niu X, Hu B, Liu J, Zhou SM, et al. Exosomes secreted by human-induced pluripotent stem cell-derived mesenchymal stem cells attenuate limb ischemia by promoting angiogenesis in mice. Stem Cell Res Ther. 2015;6:10.
Gangadaran P, Rajendran RL, Lee HW, Kalimuthu S, Hong CM, Jeong SY, et al. Extracellular vesicles from mesenchymal stem cells activates VEGF receptors and accelerates recovery of hindlimb ischemia. J Control Release. 2017;264:112–26.
Liu F, Lou YL, Wu J, Ruan QF, Xie A, Guo F, et al. Upregulation of microRNA-210 regulates renal angiogenesis mediated by activation of VEGF signaling pathway under ischemia/perfusion injury in vivo and in vitro. Kidney Blood Press Res. 2012;35:182–91.
Du W, Zhang K, Zhang S, Wang R, Nie Y, Tao H, et al. Enhanced proangiogenic potential of mesenchymal stem cell-derived exosomes stimulated by a nitric oxide releasing polymer. Biomaterials. 2017;133:70–81.
Mathiyalagan P, Liang Y, Kim D, Misener S, Thorne T, Kamide CE, et al. Angiogenic mechanisms of human CD34+ stem cell exosomes in the repair of ischemic hindlimb. Circ Res. 2017;120:1466–76.
Chen L, Zhang G, Khan AA, Guo X, Gu Y. Clinical efficacy and meta-analysis of stem cell therapies for patients with brain ischemia. Stem Cells Int. 2016;2016:6129579.
Moustafa RR, Baron JC. Pathophysiology of ischaemic stroke: insights from imaging, and implications for therapy and drug discovery. Br J Pharmacol. 2008;153:S44–54.
Zhang T, Lee YW, Rui YF, Cheng TY, Jiang XH, Li G. Bone marrow-derived mesenchymal stem cells promote angiogenesis and growth of breast and prostate tumors. Stem Cell Res Ther. 2013;4:70.
Gu Y, Zhang Y, Bi Y, Liu J, Tan B, Gong M, et al. Mesenchymal stem cells suppress neuronal apoptosis and decrease IL-10 release via the TLR2/NFκB pathway in rats with hypoxic-ischemic brain damage. Mol Brain. 2015;8:65.
Zhang R, Liu Y, Yan K, Chen L, Chen X-R, Li P, et al. Anti-inflammatory and immunomodulatory mechanisms of mesenchymal stem cell transplantation in experimental traumatic brain injury. J Neuroinflammation. 2013;10:106.
Eggenhofer E, Luk F, Dahlke MH, Hoogduijn MJ. The life and fate of mesenchymal stem cells. Front Immunol. 2014;5:148.
Smyth T, Kullberg M, Malik N, Smith-Jones P, Graner MW, Anchordoquy TJ. Biodistribution and delivery efficiency of unmodified tumor-derived exosomes. J Control Release. 2015;199:145–55.
Manuel GE, Johnson T, Liu D. Therapeutic angiogenesis of exosomes for ischemic stroke. Int J Physiol Pathophysiol Pharmacol. 2017;9:188–91.
Hu B, Chen S, Zou M, He Z, Shao S, Liu B. Effect of extracellular vesicles on neural functional recovery and immunologic suppression after rat cerebral apoplexy. Cell Physiol Biochem. 2016;40:155–62.
Doeppner TR, Herz J, Görgens A, Schlechter J, Ludwig AK, Radtke S, et al. Extracellular vesicles improve post-stroke neuroregeneration and prevent postischemic immunosuppression. Stem Cells Transl Med. 2015;4:1131–43.
Lee JY, Kim E, Choi SM, Kim DW, Kim KP, Lee I, et al. Microvesicles from brain-extract—treated mesenchymal stem cells improve neurological functions in a rat model of ischemic stroke. Sci Rep. 2016;6:33038.
Nalamolu KR, Venkatesh I, Mohandass A, Klopfenstein JD, Pinson DM, Wang DZ, et al. Exosomes secreted by the cocultures of normal and oxygen–glucose-deprived stem cells improve post-stroke outcome. Neuromol Med. 2019;21:529–39.
Liu W, Bai X, Zhang A, Huang J, Xu S, Zhang J. Role of exosomes in central nervous system diseases. Front Mol Neurosci. 2019;12:240.
Go V, Bowley BG, Pessina MA, Zhang ZG, Chopp M, Finklestein SP, et al. Extracellular vesicles from mesenchymal stem cells reduce microglial-mediated neuroinflammation after cortical injury in aged Rhesus monkeys. Geroscience. 2020;42:1–17.
Medalla M, Chang W, Calderazzo SM, Go V, Tsolias A, Goodliffe JW, et al. Treatment with mesenchymal-derived extracellular vesicles reduces injury-related pathology in pyramidal neurons of monkey perilesional ventral premotor cortex. J Neurosci. 2020;40:3385–407.
Li L, Wei C, Kim IK, Janssen-Heininger Y, Gupta S. Inhibition of nuclear factor-κB in the lungs prevents monocrotaline-induced pulmonary hypertension in mice. Hypertension. 2014;63:1260–9.
Hurst LA, Dunmore BJ, Long L, Crosby A, Al-Lamki R, Deighton J, et al. TNFα drives pulmonary arterial hypertension by suppressing the BMP type-II receptor and altering NOTCH signalling. Nat Commun. 2017;8:14079.
Hansmann G, Fernandez-Gonzalez A, Aslam M, Vitali SH, Martin T, Mitsialis SA, et al. Mesenchymal stem cell-mediated reversal of bronchopulmonary dysplasia and associated pulmonary hypertension. Pulm Circ. 2012;2:170–81.
Hogan SE, Rodriguez Salazar MP, Cheadle J, Glenn R, Medrano C, Petersen TH, et al. Mesenchymal stromal cell-derived exosomes improve mitochondrial health in pulmonary arterial hypertension. Am J Physiol Lung Cell Mol Physiol. 2019;316:L723–37.
Zhang J, He Y, Yan X, Chen S, He M, Lei Y, et al. Micro RNA-483 amelioration of experimental pulmonary hypertension. EMBO Mol Med. 2020;12:e11303.
Wei Li J, Wei L, Han Z, Chen Z. Mesenchymal stromal cells-derived exosomes alleviate ischemia/reperfusion injury in mouse lung by transporting anti-apoptotic miR-21–5p. Eur J Pharmacol. 2019;852:68–76.
Zhang K, Zhao X, Chen X, Wei Y, Du W, Wang Y, et al. Enhanced therapeutic effects of mesenchymal stem cell-derived exosomes with an injectable hydrogel for hindlimb ischemia treatment. ACS Appl Mater Interfaces. 2018;10:30081–91.
Noronha NC, Mizukami A, Caliári-Oliveira C, Cominal JG, Rocha JLM, Covas DT, et al. Priming approaches to improve the efficacy of mesenchymal stromal cell-based therapies. Stem Cell Res Ther. 2019;10:131.
Park JS, Suryaprakash S, Lao YH, Leong KW. Engineering mesenchymal stem cells for regenerative medicine and drug delivery. Methods. 2015;84:3–16.
Kim EH, Kim DH, Kim HR, Kim SY, Kim HH, Bang OY. Stroke serum priming modulates characteristics of mesenchymal stromal cells by controlling the expression miRNA-20a. Cell Transplant. 2016;25:1489–99.
Pegtel D, Peferoen L, Amor S. Extracellular vesicles as modulators of cell-to-cell communication in the healthy and diseased brain. Philos Trans R Soc Lond B Biol Sci. 2014;369:20130516.
Phan J, Kumar P, Hao D, Gao K, Farmer D, Wang A. Engineering mesenchymal stem cells to improve their exosome efficacy and yield for cell-free therapy. J Extracell Vesicles. 2018;7:1522236.
Mendt M, Kamerkar S, Sugimoto H, McAndrews KM, Wu CC, Gagea M, et al. Generation and testing of clinical-grade exosomes for pancreatic cancer. JCI Insight. 2018;3:e99263.
Del Piccolo N, Placone J, He L, Agudelo SC, Hristova K. Production of plasma membrane vesicles with chloride salts and their utility as a cell membrane mimetic for biophysical characterization of membrane protein interactions. Anal Chem. 2012;84:8650–5.
Wu H, Oliver AE, Ngassam VN, Yee CK, Parikh AN, Yeh Y. Preparation, characterization, and surface immobilization of native vesicles obtained by mechanical extrusion of mammalian cells. Integr Biol. 2012;4:685–92.
Pick H, Schmid EL, Tairi AP, Ilegems E, Hovius R, Vogel H. Investigating cellular signaling reactions in single attoliter vesicles. J Am Chem Soc. 2005;127:2908–12.
Gomzikova MO, Zhuravleva MN, Vorobev VV, Salafutdinov II, Laikov AV, Kletukhina SK, et al. Angiogenic activity of cytochalasin B-induced membrane vesicles of human mesenchymal stem cells. Cells. 2020;9:95.
Zhang HC, Liu XB, Huang S, Bi XY, Wang HX, Xie LX, et al. Microvesicles derived from human umbilical cord mesenchymal stem cells stimulated by hypoxia promote angiogenesis both in vitro and in vivo. Stem Cells Dev. 2012;21:3289–97.
Han Y, Ren J, Bai Y, Pei X, Han Y. Exosomes from hypoxia-treated human adipose-derived mesenchymal stem cells enhance angiogenesis through VEGF/VEGF-R. Int J Biochem Cell Biol. 2019;109:59–68.
Salomon C, Ryan J, Sobrevia L, Kobayashi M, Ashman K, Mitchell M, et al. Exosomal signaling during hypoxia mediates microvascular endothelial cell migration and vasculogenesis. PLoS One. 2013;8:e68451.
Han YD, Bai Y, Yan XL, Ren J, Zeng Q, Li XD, et al. Co-transplantation of exosomes derived from hypoxia-preconditioned adipose mesenchymal stem cells promotes neovascularization and graft survival in fat grafting. Biochem Biophys Res Commun. 2018;497:305–12.
Almeria C, Weiss R, Roy M, Tripisciano C, Kasper C, Weber V, et al. Hypoxia conditioned mesenchymal stem cell-derived extracellular vesicles induce increased vascular tube formation in vitro. Front Bioeng Biotechnol. 2019;7:292.
Yu B, Kim HW, Gong M, Wang J, Millard RW, Wang Y, et al. Exosomes secreted from GATA-4 overexpressing mesenchymal stem cells serve as a reservoir of anti-apoptotic microRNAs for cardioprotection. Int J Cardiol. 2015;182:349–60.
Kim HW, Haider HK, Jiang S, Ashraf M. Ischemic preconditioning augments survival of stem cells via miR-210 expression by targeting caspase-8-associated protein 2. J Biol Chem. 2009;284:33161–8.
Zhang C, Shao K, Liu C, Li C, Yu B. Hypoxic preconditioning BMSCs-exosomes inhibit cardiomyocyte apoptosis after acute myocardial infarction by upregulating microRNA-24. Eur Rev Med Pharmacol Sci. 2019;23:6691–9.
Sun J, Shen H, Shao L, Teng X, Chen Y, Liu X, et al. HIF-1α overexpression in mesenchymal stem cell-derived exosomes mediates cardioprotection in myocardial infarction by enhanced angiogenesis. Stem Cell Res Ther. 2020;11:373.
Zhu LP, Tian T, Wang JY, He JN, Chen T, Pan M, et al. Hypoxia-elicited mesenchymal stem cell-derived exosomes facilitates cardiac repair through miR-125b-mediated prevention of cell death in myocardial infarction. Theranostics. 2018;8:6163-77.
Park H, Park H, Mun D, Kang J, Kim H, Kim M, et al. Extracellular vesicles derived from hypoxic human mesenchymal stem cells attenuate GSK3β expression via miRNA-26a in an ischemia-reperfusion injury model. Yonsei Med J. 2018;59:736–45.
Cui X, Wang H, Guo H, Wang C, Ao H, Liu X, et al. Transplantation of mesenchymal stem cells preconditioned with diazoxide, a mitochondrial ATP-sensitive potassium channel opener, promotes repair of myocardial infarction in rats. Tohoku J Exp Med. 2010;220:139–47.
Liu J, Zhu P, Song P, Xiong W, Chen H, Peng W, et al. Pretreatment of adipose derived stem cells with curcumin facilitates myocardial recovery via antiapoptosis and angiogenesis. Stem Cells Int. 2015;2015:638153.
Yao Y, Zhang F, Wang L, Zhang G, Wang Z, Chen J, et al. Lipopolysaccharide preconditioning enhances the efficacy of mesenchymal stem cells transplantation in a rat model of acute myocardial infarction. J Biomed Sci. 2009;16:74.
Yang J, Gao F, Zhang Y, Liu Y, Zhang DB, Decoction BH. enhances angiogenic effect of mesenchymal stem cell by upregulating VEGF expression after focal cerebral ischemia. J Mol Neurosci. 2015;56:898–906.
Tsai LK, Wang Z, Munasinghe J, Leng Y, Leeds P, Chuang DM. Mesenchymal stem cells primed with valproate and lithium robustly migrate to infarcted regions and facilitate recovery in a stroke model. Stroke. 2011;42:2932–9.
Madrigal M, Rao KS, Riordan NH. A review of therapeutic effects of mesenchymal stem cell secretions and induction of secretory modification by different culture methods. J Transl Med. 2014;12:260.
Domenis R, Cifù A, Quaglia S, Pistis C, Moretti M, Vicario A, et al. Pro inflammatory stimuli enhance the immunosuppressive functions of adipose mesenchymal stem cells-derived exosomes. Sci Rep. 2018;8:13325.
Harting MT, Srivastava AK, Zhaorigetu S, Bair H, Prabhakara KS, Toledano Furman NE, et al. Inflammation-stimulated mesenchymal stromal cell-derived extracellular vesicles attenuate inflammation. Stem Cells. 2018;36:79–90.
Kim YE, Sung SI, Chang YS, Ahn SY, Sung DK, Park WS. Thrombin preconditioning enhances therapeutic efficacy of human Wharton’s Jelly-derived mesenchymal stem cells in severe neonatal hypoxic ischemic encephalopathy. Int J Mol Sci. 2019;20:2477.
Ruan XF, Li YJ, Ju CW, Shen Y, Lei W, Chen C, et al. Exosomes from Suxiao Jiuxin pill-treated cardiac mesenchymal stem cells decrease H3K27 demethylase UTX expression in mouse cardiomyocytes in vitro. Acta Pharmacol Sin. 2018;39:579–86.
Li H, Zuo S, He Z, Yang Y, Pasha Z, Wang Y, et al. Paracrine factors released by GATA-4 overexpressed mesenchymal stem cells increase angiogenesis and cell survival. Am J Physiol Heart Circ Physiol. 2010;299:H1772–81.
Kang K, Ma R, Cai W, Huang W, Paul C, Liang J, et al. Exosomes secreted from CXCR4 overexpressing mesenchymal stem cells promote cardioprotection via Akt signaling pathway following myocardial infarction. Stem Cells Int. 2015;2015:659890.
He JG, Xie QL, Li BB, Zhou L, Yan D. Exosomes derived from IDO1-overexpressing rat bone marrow mesenchymal stem cells promote immunotolerance of cardiac allografts. Cell Transplant. 2018;27:1657–83.
Gong XH, Liu H, Wang SJ, Liang SW, Wang GG. Exosomes derived from SDF1-overexpressing mesenchymal stem cells inhibit ischemic myocardial cell apoptosis and promote cardiac endothelial microvascular regeneration in mice with myocardial infarction. J Cell Physiol. 2019;234:13878–93.
Chen Y, Zhao Y, Chen W, Xie L, Zhao Z-A, Yang J, et al. MicroRNA-133 overexpression promotes the therapeutic efficacy of mesenchymal stem cells on acute myocardial infarction. Stem Cell Res Ther. 2017;8:268.
Liu J, Jiang M, Deng S, Lu J, Huang H, Zhang Y, et al. miR-93-5p-containing exosomes treatment attenuates acute myocardial infarction-induced myocardial damage. Mol Ther Nucleic Acids. 2018;11:103–15.
Luo Q, Guo D, Liu G, Chen G, Hang M, Jin M. Exosomes from MiR-126-overexpressing adscs are therapeutic in relieving acute myocardial ischaemic injury. Cell Physiol Biochem. 2017;44:2105–16.
Lai RC, Yeo RW, Tan KH, Lim SK. Exosomes for drug delivery—a novel application for the mesenchymal stem cell. Biotechnol Adv. 2013;31:543–51.
Vader P, Mol EA, Pasterkamp G, Schiffelers RM. Extracellular vesicles for drug delivery. Adv Drug Deliv Rev. 2016;106:148–56.
Pascucci L, Coccè V, Bonomi A, Ami D, Ceccarelli P, Ciusani E, et al. Paclitaxel is incorporated by mesenchymal stromal cells and released in exosomes that inhibit in vitro tumor growth: a new approach for drug delivery. J Control Release. 2014;192:262–70.
Sun D, Zhuang X, Zhang S, Deng Z-B, Grizzle W, Miller D, et al. Exosomes are endogenous nanoparticles that can deliver biological information between cells. Adv Drug Deliv Rev. 2013;65:342–7.
Alvarez-Erviti L, Seow Y, Yin H, Betts C, Lakhal S, Wood MJ. Delivery of siRNA to the mouse brain by systemic injection of targeted exosomes. Nat Biotechnol. 2011;29:341–5.
Morales-Prieto DM, Stojiljkovic M, Diezel C, Streicher P-E, Röstel F, Lindner J, et al. Peripheral blood exosomes pass blood-brain-barrier and induce glial cell activation. bioRxiv. 2018. https://doi.org/10.1101/471409.
Morishita M, Takahashi Y, Nishikawa M, Takakura Y. Pharmacokinetics of exosomes—an important factor for elucidating the biological roles of exosomes and for the development of exosome-based therapeutics. J Pharm Sci. 2017;106:2265–9.
Takahashi Y, Nishikawa M, Shinotsuka H, Matsui Y, Ohara S, Imai T, et al. Visualization and in vivo tracking of the exosomes of murine melanoma B16-BL6 cells in mice after intravenous injection. J Biotechnol. 2013;165:77–84.
Imai T, Takahashi Y, Nishikawa M, Kato K, Morishita M, Yamashita T, et al. Macrophage-dependent clearance of systemically administered B16BL6-derived exosomes from the blood circulation in mice. J Extracell Vesicles. 2015;4:26238.
Parada N, Romero-Trujillo A, Georges N, Alcayaga-Miranda F. Camouflage strategies for therapeutic exosomes evasion from phagocytosis. J Adv Res. 2021;31:61–74.
Suk JS, Xu Q, Kim N, Hanes J, Ensign LM. PEGylation as a strategy for improving nanoparticle-based drug and gene delivery. Adv Drug Deliv Rev. 2016;99:28–51.
Badr CE, Tannous BA. Bioluminescence imaging: progress and applications. Trends Biotechnol. 2011;29:624–33.
Maheshwari R, Tekade M, Gondaliya P, Kalia K, D’Emanuele A, Tekade RK. Recent advances in exosome-based nanovehicles as RNA interference therapeutic carriers. Nanomedicine. 2017;12:2653–75.
Neves KB, Rios FJ, Sevilla‐Montero J, Montezano AC, Touyz RM. Exosomes and the cardiovascular system: role in cardiovascular health and disease. J Physiol. 2022. https://doi.org/10.1113/JP282054.
Mittelbrunn M, Gutiérrez-Vázquez C, Villarroya-Beltri C, González S, Sánchez-Cabo F, González M, et al. Unidirectional transfer of microRNA-loaded exosomes from T cells to antigen-presenting cells. Nat Commun. 2011;2:282.
Mathiyalagan P, Sahoo S. Exosomes-based gene therapy for MicroRNA delivery. Methods Mol Biol. 2017;1521:139–52.
Wu G, Zhang J, Zhao Q, Zhuang W, Ding J, Zhang C, et al. Molecularly engineered macrophage-derived exosomes with inflammation tropism and intrinsic heme biosynthesis for atherosclerosis treatment. Angew Chem Int Ed Engl. 2020;59:4068–74.
Zhang X, Lu A, Li Z, Sun J, Dai D, Qian L. Exosomes secreted by endothelial progenitor cells improve the bioactivity of pulmonary microvascular endothelial cells exposed to hyperoxia in vitro. Ann Transl Med. 2019;7:254.
Sun YQ, Zhang Y, Li X, Deng MX, Gao WX, Yao Y, et al. Insensitivity of human iPS cells-derived mesenchymal stem cells to interferon-γ-induced HLA expression potentiates repair efficiency of hind limb ischemia in immune humanized NOD Scid gamma mice. Stem Cells. 2015;33:3452–67.
Sun L, Xu R, Sun X, Duan Y, Han Y, Zhao Y, et al. Safety evaluation of exosomes derived from human umbilical cord mesenchymal stromal cell. Cytotherapy. 2016;18:413–22.
Lener T, Gimona M, Aigner L, Börger V, Buzas E, Camussi G, et al. Applying extracellular vesicles based therapeutics in clinical trials–an ISEV position paper. J Extracell Vesicles. 2015;4:30087.
Zhang Y, Mignone J, MacLellan WR. Cardiac regeneration and stem cells. Physiol Rev. 2015;95:1189–204.
Jayaraman S, Gnanasampanthapandian D, Rajasingh J, Palaniyandi K. Stem cell-derived exosomes potential therapeutic roles in cardiovascular diseases. Front Cardiovasc Med. 2021;8:723236.
Nikfarjam S, Rezaie J, Zolbanin NM, Jafari R. Mesenchymal stem cell derived-exosomes: a modern approach in translational medicine. J Transl Med. 2020;18:449.
Park DJ, Seo YJ. Engineering of extracellular vesicles based on payload changes for tissue regeneration. Tissue Eng Regen Med. 2021;18:485–97.
Acknowledgements
All of the persons contributed to the manuscript were placed as author in the manuscript.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical statement
There are no animal experiments carried out for this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ahmed, L., Al-Massri, K. New Approaches for Enhancement of the Efficacy of Mesenchymal Stem Cell-Derived Exosomes in Cardiovascular Diseases. Tissue Eng Regen Med 19, 1129–1146 (2022). https://doi.org/10.1007/s13770-022-00469-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13770-022-00469-x