Abstract
Background:
With the popularity of laparoscopic cholecystectomy, common bile duct injury has been reported more frequently. There is no perfect method for repairing porcine biliary segmental defects.
Methods:
After the decellularization of human arterial blood vessels, the cells were cultured with GFP+ (carry green fluorescent protein) porcine bile duct epithelial cells. The growth and proliferation of porcine bile duct epithelial cells on the human acellular arterial matrix (HAAM) were observed by hematoxylin–eosin (HE) staining, electron microscopy, and immunofluorescence. Then, the recellularized human acellular arterial matrix (RHAAM) was used to repair biliary segmental defects in the pig. The feasibility of it was detected by magnetic resonance cholangiopancreatography, liver function and blood routine changes, HE staining, immunofluorescence, real-time quantitative PCR (RT-qPCR), and western blot.
Results:
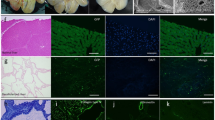
After 4 weeks (w) of co-culture of HAAM and GFP+ porcine bile duct epithelial cells, GFP+ porcine bile duct epithelial cells grew stably, proliferated, and fused on HAAM. Bile was successfully drained into the duodenum without bile leakage or biliary obstruction. Immunofluorescence detection showed that GFP-positive bile duct cells could still be detected after GFP-containing bile duct cells were implanted into the acellular arterial matrix for 8 w. The implanted bile duct cells can successfully resist bile invasion and protect the acellular arterial matrix until the newborn bile duct is formed.
Conclusion:
The RHAAM can be used to repair biliary segmental defects in pigs, which provides a new idea for the clinical treatment of common bile duct injury.










Similar content being viewed by others
References
Dolan JP, Diggs BS, Sheppard BC, Hunter JG. Ten-year trend in the national volume of bile duct injuries requiring operative repair. Surg Endosc. 2005;19:967–73.
Nilsson E. Incidence and nature of bile duct injuries following laparoscopic cholecystectomy: an audit of 5913 cases. Br J Surg. 1997;84:424.
Russell JC, Walsh SJ, Mattie AS, Lynch JT. Bile duct injuries, 1989–1993. A statewide experience. Connecticut laparoscopic cholecystectomy registry. Arch Surg. 1996;131:382–8.
Vecchio R, MacFadyen BV, Latteri S. Laparoscopic cholecystectomy: an analysis on 114,005 cases of United States series. Int Surg. 1998;83:215–9.
Mathisen O, Søreide O, Bergan A. Laparoscopic cholecystectomy: bile duct and vascular injuries: management and outcome. Scand J Gastroenterol. 2002;37:476–81.
Schmidt SC, Settmacher U, Langrehr JM, Neuhaus P. Management and outcome of patients with combined bile duct and hepatic arterial injuries after laparoscopic cholecystectomy. Surgery. 2004;135:613–8.
Flum DR, Cheadle A, Prela C, Dellinger EP, Chan L. Bile duct injury during cholecystectomy and survival in medicare beneficiaries. JAMA. 2003;290:2168–73.
Boerma D, Rauws EA, Keulemans YC, Bergman JJ, Obertop H, Huibregtse K, et al. Impaired quality of life 5 years after bile duct injury during laparoscopic cholecystectomy: a prospective analysis. Ann Surg. 2001;234:750–7.
Moore DE, Feurer ID, Holzman MD, Wudel LJ, Strickland C, Gorden DL, et al. Long-term detrimental effect of bile duct injury on health-related quality of life. Arch Surg. 2004;139:476–81.
Malik AA, Rather SA, Bari SU, Wani KA. Long-term results of choledochoduodenostomy in benign biliary obstruction. World J Gastrointest Surg. 2012;4:36–40.
Murray KF, Carithers RL Jr. AASLD practice guidelines: evaluation of the patient for liver transplantation. Hepatology. 2005;41(6):1407–32.
Perkins JD. Are we reporting the same thing? Liver Transpl. 2007;13:465–6.
Skaro AI, Jay CL, Baker TB, Wang E, Pasricha S, Lyuksemburg V, et al. The impact of ischemic cholangiopathy in liver transplantation using donors after cardiac death: the untold story. Surgery. 2009;146:543–52.
Enestvedt CK, Malik S, Reese PP, Maskin A, Yoo PS, Fayek SA, et al. Biliary complications adversely affect patient and graft survival after liver retransplantation. Liver Transpl. 2013;19:965–72.
Chan BP, Leong KW. Scaffolding in tissue engineering: general approaches and tissue-specific considerations. Eur Spine J. 2008;17:467–79.
Sampaziotis F, Justin AW, Tysoe OC, Sawiak S, Godfrey EM, Upponi SS, et al. Reconstruction of the mouse extrahepatic biliary tree using primary human extrahepatic cholangiocyte organoids. Nat Med. 2017;23:954–63.
Yannas IV. Emerging rules for inducing organ regeneration. Biomaterials. 2013;34:321–30.
Wagenseil JE, Mecham RP. Vascular extracellular matrix and arterial mechanics. Physiol Rev. 2009;89:957–89.
Shiojiri N, Sugiyama Y. Immunolocalization of extracellular matrix components and integrins during mouse liver development. Hepatology. 2004;40:346–55.
Baloch Z, Klapper J, Buchanan L, Schwartz M, Amenta PS. Ontogenesis of the murine hepatic extracellular matrix: an immunohistochemical study. Differentiation. 1992;51:209–18.
Hodde JP, Record RD, Liang HA, Badylak SF. Vascular endothelial growth factor in porcine-derived extracellular matrix. Endothelium. 2001;8:11–24.
Voytik-Harbin SL, Brightman AO, Kraine MR, Waisner B, Badylak SF. Identification of extractable growth factors from small intestinal submucosa. J Cell Biochem. 1997;67:478–91.
Acknowledgements
The authors thank Doc. Li Li (Department of hepatobiliary surgery, Ganmei Hospital affiliated to Kunming Medical University, Kunming, Yunnan, 650500, China) for the critical comment and discussion on this study.
Funding
The study was supported by National Natural Science Foundation of China (No. 81560089) and Yunnan Province Health Science and Technology Project (No.2014NS198).
Author information
Authors and Affiliations
Contributions
Wei Liu drafting the article, a substantial contribution to the conception and design of the study. Sheng-Ning Zhang, Zong-Qiang Hu, Shi-Ming Feng, Zhen-Hui Li, Shu-Feng Xiao, and Hong-Shu Wang performed the research and contribution to acquisition, interpretation, and analysis of data. Li Li revising the draft critically and final approval of the version to be published.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no financial conflicts of interest.
Ethical statement
The study protocol was approved by the institutional review board of Ganmei Hospital affiliated to Kunming Medical University. Informed consent was confirmed by the Ganmei Hospital affiliated to Kunming Medical University. The animal studies were performed after receiving approval of the Ethics Committee of Ganmei Hospital affiliated to Kunming Medical University (2015-01).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, W., Zhang, SN., Hu, ZQ. et al. Study of Recellularized Human Acellular Arterial Matrix Repairs Porcine Biliary Segmental Defects. Tissue Eng Regen Med 16, 653–665 (2019). https://doi.org/10.1007/s13770-019-00212-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13770-019-00212-z